Why You Might Have Swelling With Depression
Swelling with depression often comes from fluid retention, medication side effects, or heart/kidney strain. Targeted labs available at Quest—no referral needed.
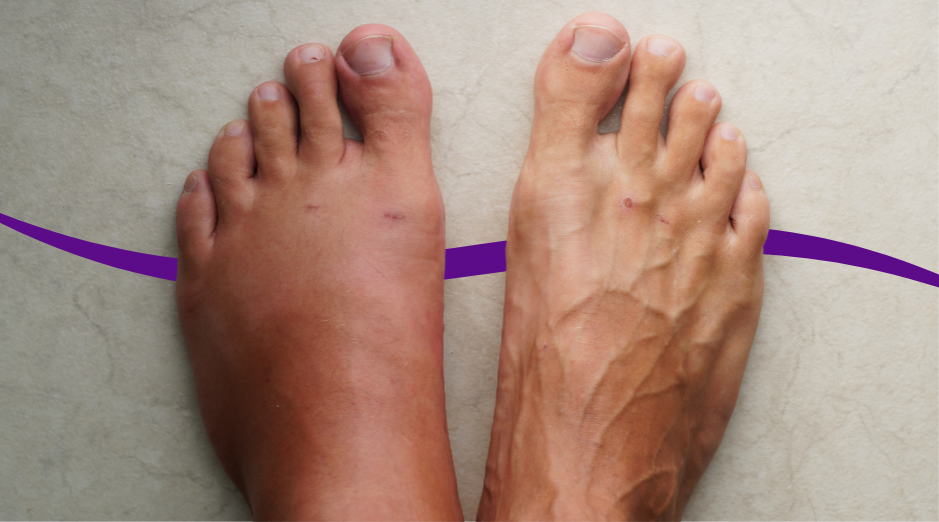
Swelling with depression usually comes from one of three buckets: your body holding onto salt and water because you are less active or sleeping poorly, a medication side effect (especially some antidepressants or blood pressure meds), or an underlying heart, kidney, liver, or thyroid problem that is also affecting your mood. The pattern of swelling and a few targeted blood tests can help sort out which one fits you. This combo is frustrating because it feels like your body is “betraying” you on two fronts at once. The good news is that swelling (also called fluid buildup [edema]) often follows rules: where it shows up, when it’s worse, and whether it pits when you press it can all point toward a cause. If you want help thinking through your specific pattern, PocketMD can walk you through the red flags and next steps, and Vitals Vault labs can help you check the most common medical contributors without a referral.
Why swelling can show up with depression
Less movement, more fluid pooling
When depression makes you sit or lie down more, gravity has more time to pull fluid into your feet, ankles, and lower legs. Your calf muscles normally act like a pump, so when they are “offline,” you can end the day with tight socks, puffy ankles, and shoes that suddenly feel small. A simple clue is timing: swelling that is worse at night and better after a night in bed often points to pooling rather than a dangerous organ problem.
Antidepressant-related water retention
Some antidepressants can cause swelling by changing how your blood vessels relax and how your kidneys handle salt and water, and a few can also trigger low sodium (hyponatremia) that makes you feel foggy or weak. You might notice new puffiness in your hands, face, or ankles within days to weeks of starting or increasing a dose. Do not stop your medication abruptly, but do message your prescriber promptly if the timing lines up, especially if you also feel dizzy, confused, or unusually tired.
Heart strain causing leg swelling
If your heart is not pumping strongly enough, pressure backs up in the veins and fluid leaks into tissues, which often shows up as swelling in both legs and ankles. This can overlap with depression because low energy and poor sleep can be symptoms of heart failure too, not just mood. Swelling that comes with shortness of breath when lying flat, waking up gasping, or rapid weight gain over a few days deserves urgent evaluation.
Kidney problems and protein loss
Your kidneys control fluid balance, and they also keep protein in your bloodstream where it belongs. When kidney filters are inflamed or leaky, you can lose protein in urine, which lowers the “pull” that keeps fluid inside blood vessels and leads to swelling that can be dramatic around the eyes in the morning. If you are noticing foamy urine, higher blood pressure, or swelling that is not improving overnight, it is worth checking kidney markers and urine protein soon.
Low thyroid slowing fluid clearance
An underactive thyroid (hypothyroidism) can cause a slower metabolism, constipation, weight gain, and a puffy look, and it can also worsen low mood. The swelling is often more “doughy” than pitting, and you may also feel cold, dry-skinned, or unusually slowed down. Because thyroid shifts are treatable, checking a thyroid-stimulating hormone test is one of the most practical first steps when swelling and depression travel together.
What actually helps with swelling (and when to get help)
Use the 10-second press test
Press your thumb firmly into the swollen area for 10 seconds and then release. If it leaves a dent that slowly fills back in, that “pitting” pattern often points to fluid pooling, salt retention, or heart/kidney causes rather than simple inflammation from an injury. Take a quick photo of the dent and the location, because showing the pattern to a clinician can speed up the right workup.
Do a daily ankle-and-weight check
Swelling is easier to track with numbers than with memory, especially when you are already mentally exhausted. Weigh yourself each morning after you pee, and measure around one ankle at the same spot with a string or tape. A gain of about 2–3 pounds in 24 hours or 5 pounds in a week suggests true fluid buildup, and it is a reason to contact your clinician rather than just “waiting it out.”
Try a 7-day sodium reset
If your swelling is from salt and water retention, you can often feel a difference within a week when you cut back on packaged and restaurant foods. Focus on cooking a few simple meals at home and choosing “no salt added” options, because the hidden sodium is usually the problem, not the salt shaker. If your rings fit better and your socks stop leaving deep marks, you have learned something useful about your personal driver.
Elevate and compress the right way
For leg and ankle swelling, elevation works best when your feet are above the level of your heart, not just on an ottoman. Graduated compression socks can help keep fluid from collecting during the day, but they should feel snug, not painful or numb. If one leg is much more swollen than the other, skip compression until you have been checked, because a clot needs to be ruled out first.
Review meds and supplements on purpose
Swelling is a known side effect of several common meds, including some antidepressants, calcium channel blockers for blood pressure, NSAID pain relievers, and steroid bursts. The fix is often a dose change, a switch, or adding a safer strategy for the original problem, but you need a deliberate review to connect the dots. Bring a list with start dates and dose changes, because that timeline is often more revealing than any single symptom description.
Useful biomarkers to discuss with your clinician
Creatinine
Creatinine is a waste product of muscle metabolism that is filtered by the kidneys and serves as the primary marker of kidney function. In functional medicine, creatinine levels reflect not only kidney health but also muscle mass and protein metabolism. Elevated creatinine indicates reduced kidney filtration capacity, while very low levels may indicate muscle wasting or poor protein intake. Creatinine is used to calculate eGFR and helps assess long-term kidney health and detoxification capacity. Creatinine measu…
Learn moreSodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreUrine Protein
Proteinuria is a key marker of kidney disease and damage. It indicates glomerular or tubular dysfunction. Persistent proteinuria is associated with progressive kidney disease, cardiovascular disease, and increased mortality. Early detection allows intervention to slow progression. Urine protein testing detects the presence of protein, primarily albumin, in urine. Normal urine contains minimal protein; elevated levels indicate kidney damage or disease.
Learn moreLab testing
Check kidney function, thyroid, and protein levels at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
If your swelling is mostly in your ankles, take a photo in the morning and again at night for three days. That day-to-night swing is a strong clue that gravity and inactivity are playing a big role.
Check whether the swelling is truly symmetric. One noticeably larger calf, new warmth, or tenderness on one side is not a “depression symptom,” and it is a reason to get checked the same day for a clot.
If you suspect a medication link, write down the exact start date and any dose changes, then compare it to when swelling began. That timeline often makes the answer obvious to your prescriber.
Do a quick “sock test” at the same time daily by looking at how deep the elastic marks are and how long they last. It sounds simple, but it is a surprisingly consistent way to track fluid retention when your mood makes detailed tracking hard.
When you elevate your legs, set a 20-minute timer and aim for feet above heart level. If you do this after dinner for a week and nothing changes at all, it is a hint you should look harder for a medical driver.
Frequently Asked Questions
Can depression itself cause swelling and water retention?
Depression can indirectly lead to swelling because you may move less, sleep worse, and eat more packaged salty foods, which makes fluid pool in your legs and ankles. That kind of swelling is often worse at the end of the day and improves overnight. If swelling is new, persistent, or spreading to your face or belly, it is worth checking basics like a CMP, albumin, and TSH.
Which antidepressants are most likely to cause swelling?
Swelling has been reported with several antidepressants, including SSRIs and SNRIs, and it can also happen when antidepressants contribute to low sodium (hyponatremia). The most important clue is timing: swelling that starts within days to weeks of a new medication or dose increase deserves a message to your prescriber. Ask whether checking sodium on a CMP makes sense for you, especially if you also feel foggy or weak.
When is swelling an emergency?
Get urgent care if swelling comes with trouble breathing, chest pain, coughing up pink froth, fainting, or a rapid weight gain of several pounds over a couple of days. Also treat one-sided leg swelling with warmth or pain as urgent because a blood clot is possible. If you are unsure, it is safer to be evaluated than to wait and hope.
Why are my ankles swollen but my face looks puffy too?
Ankles often swell from gravity, but facial puffiness can point toward a whole-body fluid balance issue, such as low thyroid or low blood protein (albumin) from kidney or liver problems. Morning puffiness around the eyes is a classic pattern when protein is being lost in urine. A CMP plus albumin and a thyroid test (TSH) is a practical starting point to narrow this down.
What labs should I ask for if I have swelling and low mood?
A focused starting set is a CMP to look at kidney function and sodium, albumin to check whether low protein is letting fluid leak into tissues, and TSH to screen for hypothyroidism that can mimic or worsen depression. These three do not diagnose everything, but they catch several common, treatable contributors. If results are abnormal or symptoms are escalating, bring the numbers to a clinician and ask what the next confirmatory step should be.
What the research says
2013 ACCF/AHA guideline for the management of heart failure (swelling and fluid overload red flags)
European Society of Cardiology guideline update on heart failure (practical approach to edema and congestion)
American Thyroid Association guidelines for treating hypothyroidism (symptoms, testing, and treatment targets)