Why You Swell More When You’re Stressed
Swelling under stress often comes from fluid retention hormones, higher salt cravings, or inflammation flares. Targeted labs available—no referral needed.
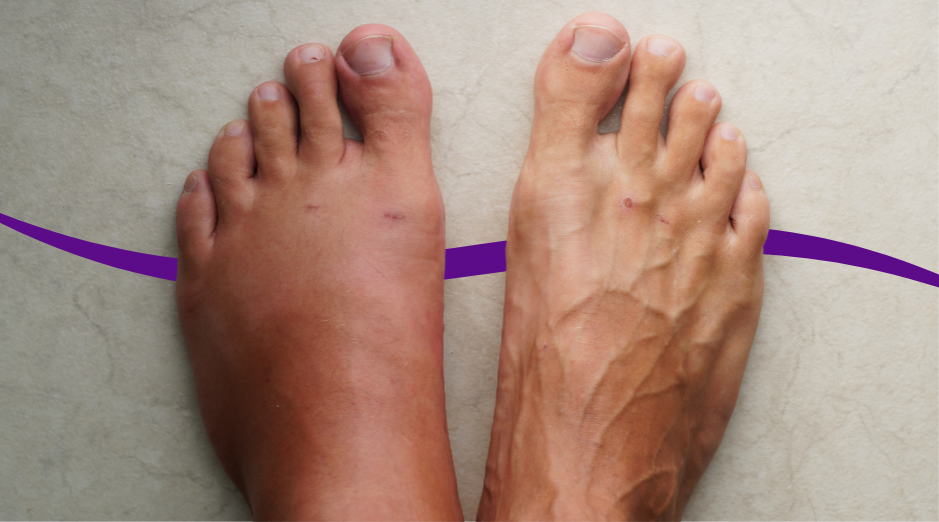
Swelling under stress is usually your body holding onto extra fluid because stress hormones push your kidneys to retain salt and water, your habits shift toward salty foods, or an underlying condition flares when you’re run down. It can show up as puffy eyelids, tight rings, or ankles that leave sock marks by evening. Basic labs can help you tell the difference between “stress-related water weight” and swelling that points to kidney, heart, liver, or thyroid issues. Stress-related swelling is common because stress changes more than your mood. It changes your hormones, your sleep, your inflammation level, and even how much you move during the day, and all of those affect where fluid sits in your tissues. The tricky part is that swelling can be harmless one week and a warning sign the next, so it helps to have a simple way to triage it. If you want help sorting your pattern and deciding what to test or when to get seen, PocketMD and targeted labs through Vitals Vault can be useful tools.
Why you swell more when you’re stressed
Stress hormones make you retain fluid
When you’re under pressure, your body turns up hormones like cortisol and aldosterone that help you “hold on” to salt and water. That can make your fingers feel tight, your face look puffier in the morning, or your ankles swell by the end of the day. A useful clue is timing: if swelling tracks with stressful weeks and improves after a couple of calmer days, fluid retention is a strong suspect.
Salt cravings and convenience foods
Stress often changes what you eat, and salty packaged foods pull water into your bloodstream and tissues. You may notice swelling after restaurant meals, late-night snacking, or travel days when you’re grabbing whatever is easy. Try a two-day experiment: keep sodium lower and cook simply, and see whether rings and shoes fit better by day two.
Less movement means pooling in legs
When you sit for long stretches, your calf muscles stop acting like a pump that pushes blood and fluid back up toward your heart. Fluid then settles in your lower legs, which is why you might see sock lines or ankle puffiness after a desk day or a long drive. If your swelling improves noticeably after a brisk 10–15 minute walk or leg elevation, gravity and immobility are likely part of the story.
Inflammation flare from stress
Stress can amplify inflammation, which makes tiny blood vessels leakier and lets fluid move into surrounding tissue. This can feel like “puffiness with tenderness,” and it often comes with achy joints, headaches, or a general sense that your body is on edge. The takeaway is to look for a trigger-and-flare pattern, because reducing the flare (sleep recovery, treating allergies, calming an autoimmune condition) often reduces the swelling too.
A hidden medical cause shows up
Sometimes stress is not the cause, but the spotlight: you notice swelling because you’re paying attention, or because stress worsens an underlying problem like kidney disease, heart failure, liver disease, or low thyroid. Red flags include swelling in just one leg with pain, sudden shortness of breath, chest pain, or swelling that is rapidly worsening over hours to a day. If any of those are happening, it’s worth urgent evaluation rather than trying to “stress-manage” your way out of it.
What actually helps with stress swelling
Do a 48-hour sodium reset
For two days, aim for mostly home-prepared food and avoid the obvious high-salt sources like takeout, deli meats, and salty snacks. This is not about perfection; it is a quick diagnostic tool to see how salt-sensitive your swelling is. If your swelling drops noticeably within 24–48 hours, you’ve learned something actionable you can repeat during stressful weeks.
Use legs-up and calf pumps
If your swelling is in your ankles or calves, elevate your legs above heart level for 15–20 minutes and do slow ankle circles or calf squeezes while you’re up there. That combination helps fluid move out of the lower legs instead of just shifting around. If you work at a desk, repeating this once mid-day can prevent the “evening ballooning” effect.
Try compression the right way
Graduated compression socks can reduce lower-leg swelling when sitting or standing is the main driver, but they work best when you put them on in the morning before swelling builds. Start with a comfortable, moderate level (often 15–20 mmHg) unless your clinician has told you otherwise. If compression makes pain worse, or one leg is much more swollen than the other, skip the experiment and get checked.
Protect sleep to calm hormones
Poor sleep makes cortisol run higher and makes you more salt-hungry the next day, which is a perfect recipe for puffiness. Pick one sleep anchor you can actually keep during stressful periods, such as a consistent wake time or a 30-minute “lights down” routine. When your sleep stabilizes, swelling that is stress-hormone driven often becomes less dramatic.
Get targeted testing if it persists
If swelling lasts more than two weeks, keeps returning, or is paired with fatigue, foamy urine, or shortness of breath, it is time to look under the hood. A few focused labs can quickly separate kidney protein loss, low blood protein, and thyroid-related fluid retention from simple lifestyle-related edema. Once you know which bucket you’re in, your next step becomes much clearer.
Useful biomarkers to discuss with your clinician
Sodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreCortisol, Total
Cortisol is the primary stress hormone that regulates metabolism, immune function, and blood pressure. In functional medicine, cortisol assessment is crucial for understanding stress response and its impact on overall health. Chronic elevation suppresses testosterone production and immune function, while low cortisol indicates adrenal insufficiency. Optimal cortisol rhythm supports energy, mood stability, and hormone balance. Cortisol orchestrates the body's stress response and daily energy rhythms. Balanced cor…
Learn moreHs Crp
High-sensitivity C-reactive protein (hs-CRP) is a key marker of systemic inflammation and cardiovascular risk. In functional medicine, we recognize hs-CRP as one of the most important predictors of heart disease, stroke, and metabolic dysfunction. Levels above 1.0 mg/L indicate increased inflammation that may be driven by poor diet, chronic infections, autoimmune conditions, or metabolic syndrome. Optimal levels below 0.5 mg/L are associated with the lowest cardiovascular risk and overall inflammatory burden. hs…
Learn moreLab testing
Get kidney function, albumin, and thyroid checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a “ring and sock test” for one week: check whether rings feel tighter in the morning and whether sock marks are deeper at night, and write down what your day looked like. Patterns show up fast, and they are more useful than guessing.
If your swelling is mostly in your legs, set a timer for every 60–90 minutes and do two minutes of calf raises or a brisk hallway walk. It sounds small, but it directly counters gravity-driven pooling.
If you wake up with a puffy face, try sleeping with your head slightly elevated for three nights and avoid late salty foods. Morning facial swelling is often a “fluid redistribution” problem, and this simple change can be surprisingly telling.
Take one clear photo of the swollen area at the same time each day for 5–7 days. It gives you an objective baseline, and it helps a clinician take you seriously if you do need to be evaluated.
When you try a fix, change only one variable at a time for 48 hours (for example, sodium reduction without adding new supplements). You will learn what actually moves the needle for your body instead of chasing ten things at once.
Frequently Asked Questions
Can stress really cause swelling and water retention?
Yes. Stress hormones can increase salt and water retention and can also change your behavior in ways that add fluid, like eating saltier foods or sitting more. The key is that stress-related swelling usually fluctuates and improves with sleep recovery, lower sodium, and more movement. If swelling is persistent or worsening, checking a CMP, albumin, and TSH is a practical next step.
Why are my ankles swollen after a stressful day at work?
A stressful workday often means more sitting and fewer muscle contractions in your calves, so fluid pools in your lower legs by evening. It can also mean a saltier lunch, which makes your body hold onto more water. Try a 15–20 minute legs-up break plus a short walk, and see if the swelling decreases within an hour.
Is puffy face in the morning from stress or something else?
Stress can contribute through poor sleep and saltier evening eating, which shifts fluid toward your face overnight. But persistent morning puffiness can also happen with low thyroid or low blood protein, which is why TSH and serum albumin are useful tests when it keeps happening. If you also notice foamy urine or new high blood pressure, get checked sooner rather than later.
When is swelling an emergency?
Get urgent care if you have sudden shortness of breath, chest pain, fainting, or swelling that comes on quickly with one leg being much more swollen and painful than the other. Those patterns can signal heart or lung strain or a blood clot, and waiting it out is not worth the risk. If you are unsure, err on the side of being seen the same day.
What labs should I ask for if swelling keeps happening?
A focused starting set is a Comprehensive Metabolic Panel (CMP) for kidney and liver function, serum albumin to check whether low blood protein is letting fluid leak into tissues, and TSH to screen for an underactive thyroid. These tests do not diagnose every cause, but they quickly rule in or out several common, important ones. Bring your symptom timeline and photos to your visit so the results have context.
What research says about stress and swelling
Endocrine Society guideline on primary aldosteronism (a hormone that drives salt and water retention)
KDIGO 2024 guideline update for chronic kidney disease evaluation and management (edema is a key symptom to assess)
AHA/ACC/HFSA guideline for the management of heart failure (fluid retention and leg swelling are core monitoring signs)