Swelling in Perimenopause: Causes, Relief, and Lab Tests
Swelling in perimenopause is often from fluid shifts, salt sensitivity, or thyroid changes. Targeted blood tests available at Quest—no referral needed.
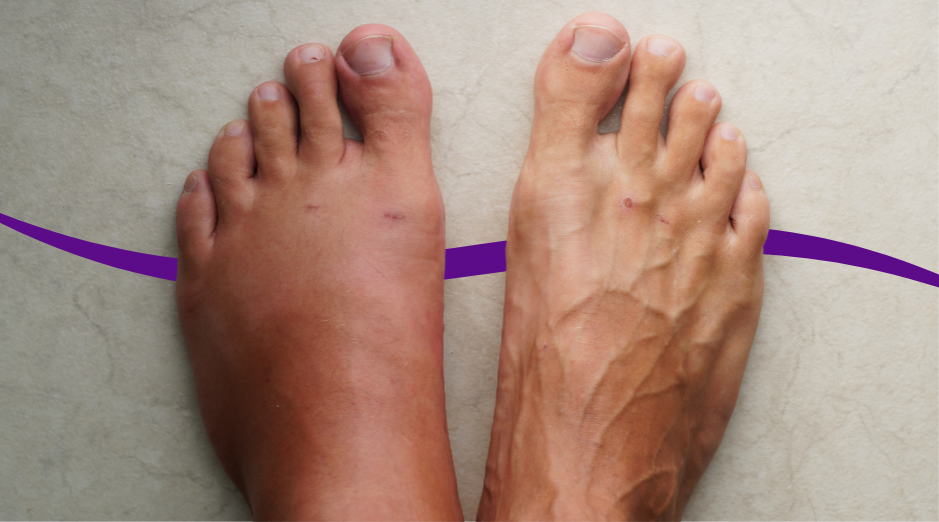
Swelling in perimenopause is usually your body holding onto extra fluid because hormones are shifting, your blood vessels are a bit “leakier” than usual, or you have a hidden driver like low thyroid. It often shows up as puffy fingers in the morning, ankle swelling by evening, or a tight, bloated feeling that comes and goes with your cycle. A few targeted labs can help sort out whether this is mostly hormone-related water retention or something you should treat as a thyroid, kidney, or protein issue. The frustrating part is that perimenopause swelling can look dramatic while still being benign, and it can also be the first sign that something else is going on. Location and timing matter: swelling that’s worse after salty meals is a different story than swelling that’s one-sided, painful, or paired with shortness of breath. This guide walks you through the most common causes, what tends to help in real life, and which tests are actually useful. If you want help matching your exact pattern to the most likely cause, PocketMD can talk it through with you, and VitalsVault labs can help you confirm what your body is doing.
Why swelling shows up in perimenopause
Hormone shifts change fluid balance
When estrogen and progesterone swing up and down, your kidneys respond by holding onto more salt and water at certain points in the month. That extra fluid tends to collect where gravity wins, which is why your ankles can look normal in the morning and puffy by evening. If your swelling tracks with cycle changes or comes with breast tenderness and “tight rings,” treating it like cyclical water retention is often the right first step.
Salt sensitivity increases with age
In perimenopause, your blood vessels and kidneys can become more reactive to sodium, so the same restaurant meal you used to tolerate can suddenly make your hands and face look puffy the next day. This is not about willpower; it is about how your body handles salt and water now. A useful clue is swelling that spikes after packaged foods or takeout and improves within 24–48 hours when you cook simply at home.
Low thyroid slows fluid clearance
An underactive thyroid (hypothyroidism) can cause a heavier, “doughy” puffiness and stubborn weight gain because your metabolism and lymph flow slow down. You might also notice dry skin, constipation, thinning hair, or feeling cold when others are comfortable. Because thyroid changes become more common in midlife, checking a TSH test is a practical way to avoid blaming everything on perimenopause.
Low blood protein causes edema
Albumin is a protein that helps keep fluid inside your blood vessels, and when it is low, fluid leaks into tissues more easily. This can show up as swelling in your legs or around your eyes, and it often feels different from “period puffiness” because it does not reliably come and go. If swelling is persistent or you notice foamy urine, an albumin test plus kidney testing can help your clinician look for protein loss or liver-related causes.
Vein issues make ankles swell
If the valves in your leg veins are not pushing blood upward efficiently, fluid pressure builds in your lower legs and your ankles swell, especially after standing or sitting for long stretches. It can come with heaviness, aching, or visible varicose veins, and it often improves when you elevate your legs. A simple check is whether swelling is clearly worse at the end of the day and better after a night in bed.
What actually helps the swelling
Do a 7-day sodium reset
For one week, aim for mostly home-prepared meals and keep packaged foods to a minimum, because that is where sodium quietly piles up. If your swelling improves noticeably by day 3–5, you have strong evidence that salt sensitivity is a major driver. After that, you can reintroduce a few “usual” foods one at a time to find your personal tipping point.
Use leg elevation strategically
If your ankles swell by evening, elevate your legs above heart level for 15–20 minutes once or twice a day, ideally after work and again before bed. This is not just comfort; it helps move fluid back into circulation so your kidneys can clear it. Pair it with a short walk afterward, because calf muscle pumping is one of the best natural “drains” for leg swelling.
Try compression on long days
Graduated compression socks can reduce ankle and lower-leg swelling when you are on your feet, traveling, or sitting for hours. The goal is steady support, not pain, so start with a moderate level and see how your legs feel after a full day. If compression helps a lot, it points toward a vein or gravity-related component rather than a whole-body fluid problem.
Review meds and supplements
Some common medications can worsen swelling, including certain blood pressure drugs, anti-inflammatories, and hormones, because they change blood vessel tone or kidney salt handling. You do not need to stop anything on your own, but it is worth asking, “Could this be contributing?” and seeing if timing matches when you started or changed a dose. Bring a photo of the swelling and a list of what you take to make that conversation quicker and more accurate.
Treat the driver, not the puffiness
If labs suggest hypothyroidism, kidney strain, or low albumin, the most effective “swelling treatment” is addressing that root cause rather than chasing water weight. That might mean thyroid replacement, adjusting blood pressure management, or evaluating protein loss in urine, depending on what shows up. If swelling is new and comes with chest pain, shortness of breath, or one-sided calf pain and warmth, treat that as urgent and get evaluated the same day.
Useful biomarkers to discuss with your clinician
TSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreAlbumin
Albumin is the most abundant protein in blood plasma, produced exclusively by the liver. In functional medicine, albumin serves as a marker of liver synthetic function, nutritional status, and overall health. Albumin maintains oncotic pressure (keeping fluid in blood vessels), transports hormones and nutrients, and serves as an antioxidant. Low albumin may indicate liver disease, malnutrition, chronic inflammation, or kidney disease. Since albumin has a half-life of about 20 days, it reflects longer-term nutriti…
Learn moreSodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreLab testing
Get kidney function, thyroid, and albumin checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “ring and sock test” for two weeks: note whether rings feel tighter in the morning and whether sock lines are deeper at night, because that pattern strongly suggests gravity plus fluid retention rather than a single swollen joint.
Take two photos of your ankles on the same spot of floor—one right after waking and one before bed—for 5–7 days. Seeing the change makes it easier to connect swelling to salt, standing time, or cycle phase.
If swelling is mostly in your legs, set a timer to stand up every 45–60 minutes and do 20 slow calf raises. It sounds small, but it mimics the “pump” your veins rely on to move fluid upward.
When you eat out, try one simple experiment: choose a meal that is grilled or steamed and ask for sauce on the side. If the next-day puffiness is dramatically less, you have identified restaurant sodium as a key trigger.
If your swelling is persistent, ask your clinician specifically about urine protein testing, because protein loss can cause edema even when you feel otherwise fine. It is an easy miss if everyone assumes it is hormonal.
Frequently Asked Questions
Is swelling a normal perimenopause symptom?
It can be, especially when it comes and goes and you notice it around certain points in your cycle. Hormone swings can make you retain salt and water, which shows up as puffy hands, a bloated feeling, or ankle swelling by evening. If swelling is new, persistent, or paired with shortness of breath or one-sided leg pain, it deserves a same-day medical check.
Why are my fingers puffy in the morning during perimenopause?
Overnight, fluid redistributes when you are lying flat, and hormone-related water retention can make that morning puffiness more obvious. It often feels like tight rings that loosen later in the day as you move around. If morning puffiness comes with fatigue, dry skin, or constipation, a TSH test can help check for hypothyroidism.
What does ankle swelling in perimenopause mean?
Ankle swelling that worsens through the day often points to gravity, vein valve strain, and salt sensitivity, which can all become more noticeable in midlife. If it improves with leg elevation or compression socks, that supports a circulation-related component. If it is sudden, one-sided, red, or painful, get evaluated urgently to rule out a clot.
Which blood tests help explain swelling and water retention?
Three practical starting tests are TSH for thyroid-driven puffiness, a comprehensive metabolic panel (CMP) for kidney and electrolyte clues, and albumin to check whether low blood protein is letting fluid leak into tissues. These tests do not diagnose everything, but they quickly separate common, fixable causes from “watch and wait.” If results are abnormal, bring them to a clinician to decide the next step.
When should I worry that swelling is heart or kidney related?
Worry more if swelling is persistent for weeks, rapidly worsening, or paired with shortness of breath when lying down, chest pressure, or a big drop in exercise tolerance. Kidney-related swelling can also show up with foamy urine or high blood pressure, and low albumin can cause more generalized puffiness. If you notice any of those patterns, get checked promptly and consider labs like a CMP and albumin to speed up the workup.
What research and guidelines say about swelling and midlife
NICE guideline: Menopause—diagnosis and management (covers symptom patterns and when to evaluate other causes)
KDIGO 2024 guideline: Chronic kidney disease evaluation and management (how kidney function and albumin relate to edema risk)
American Thyroid Association guidelines for hypothyroidism (TSH-based diagnosis and treatment targets)