Swelling After Menopause: What It Means and What Helps
Swelling after menopause often comes from fluid retention, vein valve weakness, or heart/kidney strain. Targeted labs available—no referral needed.
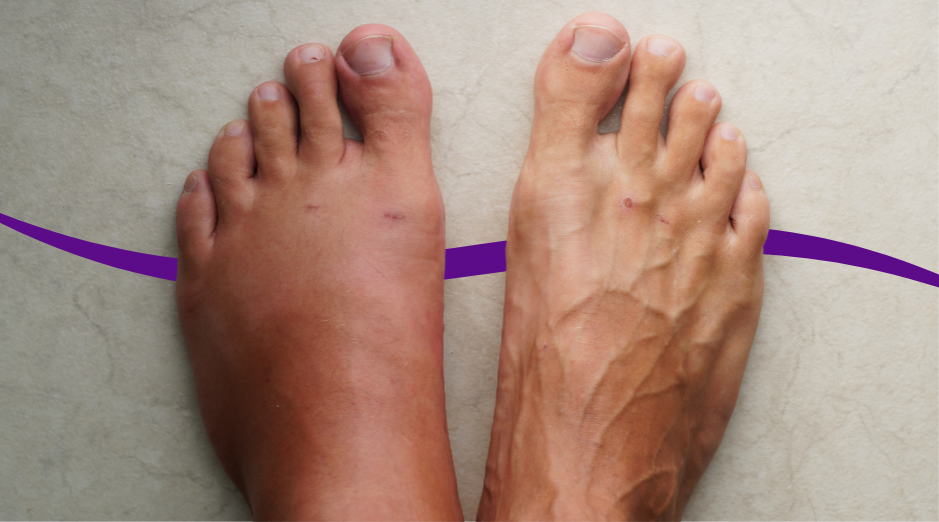
Swelling after menopause is usually your body holding onto extra fluid, your leg veins not pushing blood back up efficiently, or a signal that your heart or kidneys are under more strain than they used to be. The location matters too: ankle and lower-leg puffiness often points to veins, while swelling that comes with shortness of breath or rapid weight gain can be more urgent. A few targeted blood tests can help sort out which bucket you’re in. It’s unsettling when your shoes suddenly feel tight or your rings won’t come off, especially if you’re doing “all the right things.” After menopause, hormone shifts can change how your blood vessels behave, how your kidneys handle salt, and how easily fluid leaks into tissues. The tricky part is that swelling can be harmless and annoying, or it can be an early clue to something you should not ignore. If you want help thinking through your pattern, PocketMD can walk you through the most likely causes, and VitalsVault labs can help you check the basics without a long wait.
Why swelling can show up after menopause
Leg veins get less efficient
Over time, the one-way valves in your leg veins can weaken, so blood pools in your lower legs instead of moving smoothly back to your heart. That extra pressure pushes fluid into the surrounding tissue, which is why swelling is often worse at the end of the day and better after a night in bed. If your ankles swell more than your hands and you notice heaviness or aching after standing, ask your clinician about chronic vein issues and consider trying compression socks as a practical first step.
Fluid retention from hormone shifts
Even after periods stop, your hormones still influence how your blood vessels relax and how your kidneys handle sodium, which can nudge you toward holding onto water. This kind of swelling can feel “puffy all over,” and you might notice it fluctuates with salty meals, alcohol, or poor sleep. A useful takeaway is to test a one-week sodium experiment: keep restaurant and packaged foods low, and see whether morning puffiness and ring tightness improve.
Heart strain and fluid backup
If your heart is not pumping as strongly as it should, fluid can back up into your legs and sometimes your lungs, which makes swelling more than a cosmetic issue. You may notice swelling that climbs up the shins, new shortness of breath when walking or lying flat, or waking up at night gasping. If swelling comes with chest pressure, fainting, or sudden breathlessness, treat it as urgent and get evaluated the same day.
Kidneys leaking or retaining fluid
Your kidneys control fluid balance, and swelling can happen when they hold onto salt and water or when protein leaks into the urine, which pulls fluid out of your bloodstream and into tissues. This often shows up as persistent ankle swelling, puffy eyelids in the morning, or swelling that does not track neatly with standing and sitting. If you also notice foamy urine or your blood pressure is creeping up, kidney-focused labs and a urine check are a smart next move.
Thyroid slowdown (hypothyroidism)
A sluggish thyroid can cause a different kind of swelling that feels doughy and can involve your face, hands, and lower legs, along with fatigue, dry skin, and constipation. It is easy to blame this on “getting older,” but thyroid changes are common in midlife and treatable. If swelling is paired with low energy and feeling cold when others are fine, checking a TSH blood test is one of the highest-yield steps you can take.
What actually helps swelling go down
Use elevation with a timer
If your swelling is mostly in your ankles and calves, gravity is part of the problem, so you want to beat it on purpose. Try lying down with your legs supported above heart level for 15–20 minutes once or twice daily, especially after long standing or travel. You’re looking for a measurable change, like your sock line fading or your shoes fitting better by evening.
Try compression the right way
Compression works best when you put it on before swelling builds, which usually means first thing in the morning. A moderate strength (often 15–20 mmHg) is enough for many people, and it should feel snug but not painful or numb. If you have known artery disease or severe leg pain with walking, ask for guidance before using stronger compression.
Run a “salt reality check” week
Most sodium that drives water retention is hidden in breads, sauces, soups, deli meats, and restaurant meals, not the salt shaker. For seven days, keep meals simple and home-prepared, and aim for foods with under 300 mg sodium per serving so you can see whether swelling responds. If your swelling drops noticeably, you’ve learned something powerful about your personal threshold.
Move your calf pump on purpose
Your calf muscles act like a second heart for your legs, squeezing veins and pushing fluid upward when you walk. If you sit a lot, set a phone reminder every hour to do two minutes of brisk walking or 20 slow heel raises while holding a counter. This is especially helpful for swelling after flights, long drives, or desk days.
Match treatment to the cause
Diuretics (“water pills”) can be appropriate for heart-related fluid overload, but they are not a universal fix and they can backfire if the real issue is vein pooling or low thyroid. The best relief usually comes when you identify the driver and treat it directly, such as thyroid replacement for hypothyroidism or targeted heart therapy if strain is present. If you’re unsure which path fits your symptoms, bring a simple swelling log and your medication list to a visit so you can make a plan faster.
Useful biomarkers to discuss with your clinician
Sodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreCreatinine
Creatinine is a waste product of muscle metabolism that is filtered by the kidneys and serves as the primary marker of kidney function. In functional medicine, creatinine levels reflect not only kidney health but also muscle mass and protein metabolism. Elevated creatinine indicates reduced kidney filtration capacity, while very low levels may indicate muscle wasting or poor protein intake. Creatinine is used to calculate eGFR and helps assess long-term kidney health and detoxification capacity. Creatinine measu…
Learn moreAlbumin
Albumin is the most abundant protein in blood plasma, produced exclusively by the liver. In functional medicine, albumin serves as a marker of liver synthetic function, nutritional status, and overall health. Albumin maintains oncotic pressure (keeping fluid in blood vessels), transports hormones and nutrients, and serves as an antioxidant. Low albumin may indicate liver disease, malnutrition, chronic inflammation, or kidney disease. Since albumin has a half-life of about 20 days, it reflects longer-term nutriti…
Learn moreLab testing
Get kidney function, thyroid, and heart-strain labs checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “pitting test” once a day for a week: press your thumb into your shin for five seconds. If a dent remains, take a photo and note the time of day, because that pattern helps your clinician separate vein pooling from other causes.
Measure your ankle circumference at the same spot each evening for two weeks, using a soft tape measure. A change of even 1–2 cm can confirm that your swelling is real and fluctuating, which makes treatment experiments easier to judge.
If swelling is worse after travel, wear compression socks on the day you fly or drive and do 20 heel raises every hour. Your goal is prevention, because once fluid has leaked into tissue it takes longer to move back out.
If you wake with puffy eyelids or facial swelling, pay attention to urine clues the same day. Foamy urine or a big drop in how much you pee can be a reason to prioritize kidney testing rather than assuming it is “just salt.”
When you try a change, change only one thing for seven days. For example, keep your usual activity but cut restaurant food, because that makes it much easier to see whether sodium is your main trigger.
Frequently Asked Questions
Is swelling after menopause normal?
Mild, occasional swelling can happen after menopause because blood vessels and kidneys handle fluid a bit differently, and vein valves can weaken with age. But “common” is not the same as “ignore it,” especially if swelling is new, one-sided, or steadily worsening. If you also have shortness of breath, chest pressure, or rapid weight gain over a few days, get checked urgently.
Why are my ankles swelling but not my hands?
Ankle-only swelling often points to gravity and leg vein issues, because fluid pools in the lowest part of your body when you stand or sit. It typically worsens through the day and improves overnight. Try morning compression and a daily 15–20 minute leg-elevation session, and mention the pattern to your clinician if it persists.
When should I worry about swelling in one leg?
Swelling in one leg that comes on suddenly, especially with calf pain, warmth, or redness, can be a sign of a blood clot (deep vein thrombosis). That is not something to “watch for a week,” because clots can travel to the lungs. If this describes you, seek same-day medical evaluation.
What labs are most useful for swelling after menopause?
Three high-yield tests are a comprehensive metabolic panel (for kidney function and albumin), TSH (for thyroid slowdown), and NT-proBNP (for heart strain). These do not diagnose everything, but they quickly flag common, treatable drivers of edema. If you have puffy eyelids or foamy urine, ask about adding a urine albumin-to-creatinine ratio as well.
Can hormone therapy cause swelling after menopause?
Yes, some forms of menopausal hormone therapy can cause fluid retention, breast tenderness, or a “puffy” feeling, especially early on or with dose changes. The key clue is timing: swelling that starts soon after beginning or adjusting hormones is more suspicious for a medication effect. If that’s your pattern, talk with the prescriber about dose, route (patch vs pill), and whether another approach would suit you better.
Research and guidelines worth knowing
2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure (includes evaluation of edema and use of natriuretic peptides)
Society for Vascular Surgery and American Venous Forum guidelines on chronic venous disease management (compression and evaluation)
KDIGO 2024 Chronic Kidney Disease guideline (assessment of kidney function and albumin-related risk)