Swelling During Menopause: What It Means and What Helps
Swelling during menopause is often from fluid shifts, salt sensitivity, or vein issues, but thyroid, kidney, or heart causes matter too—targeted labs, no referral needed.
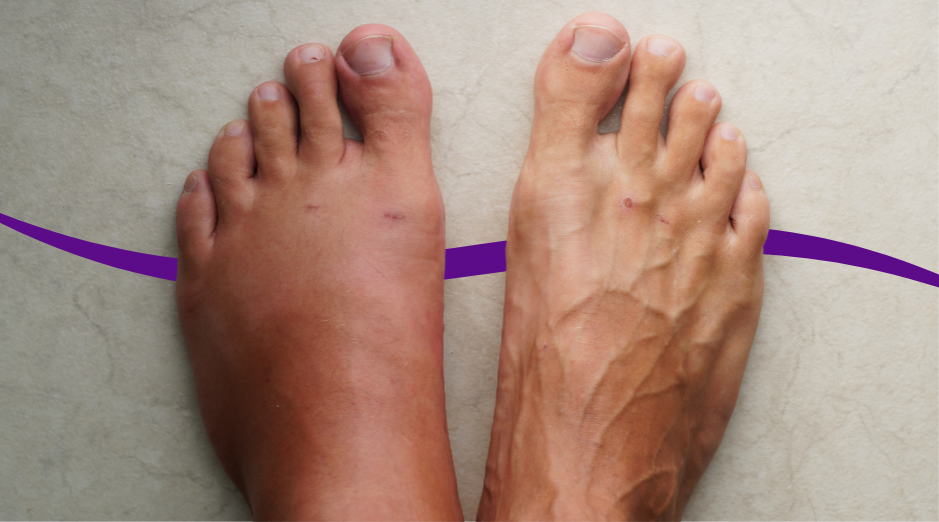
Swelling during menopause is usually your body holding onto extra fluid because estrogen is dropping, your blood vessels get “leakier,” and you become more salt-sensitive. It can also happen when leg veins stop pushing blood back up efficiently, which makes ankles and feet puff up by the end of the day. Because swelling can look the same even when the cause is different, a few targeted labs can help sort out whether this is mostly hormone-related water retention or something like thyroid, kidney, or heart strain. The frustrating part is that the swelling can be subtle at first, and then suddenly your rings feel tight or your shoes don’t fit by afternoon. Around the menopause transition, sleep disruption, stress hormones, and changes in activity can amplify fluid shifts, so you can feel “puffy” even if your weight has not changed much. This page walks you through the most common reasons, what tends to help in real life, and which tests are worth considering. If you want help matching your pattern to the most likely cause, PocketMD can talk it through with you, and Vitals Vault labs can help you check the basics without a long wait.
Why swelling shows up around menopause
Hormone shifts change fluid balance
As estrogen falls, your blood vessels tend to relax and become a bit more “leaky,” so fluid moves into tissues more easily and you notice puffiness in your hands, face, or ankles. Your kidneys can also hold onto more salt and water during this transition, which makes swelling worse after salty meals. The takeaway is that timing matters: if swelling tracks with hot flashes, sleep disruption, or cycle changes in perimenopause, hormone-driven water retention is a strong suspect.
Salt sensitivity increases with age
You can eat the same restaurant meal you always have and suddenly wake up with puffy eyelids or tight rings, because your kidneys clear sodium less efficiently over time. When sodium stays in your bloodstream, water follows it, which means you feel heavier and more swollen even if you did not “gain fat.” A practical test is a 7–10 day experiment where you cook at home and keep sodium steady; if swelling drops noticeably, salt sensitivity is likely playing a big role.
Leg veins struggle against gravity
If swelling is mostly in your ankles and calves and it gets worse as the day goes on, your leg veins may not be moving blood upward efficiently (chronic venous insufficiency). Blood pools in the lower legs, pressure rises, and fluid seeps into surrounding tissue, which can leave sock marks or a heavy, achy feeling. The clue is the pattern: it often improves overnight and flares after long sitting, long flights, or standing shifts.
Thyroid slowdown causes puffiness
An underactive thyroid can show up around midlife and it can cause generalized swelling, especially in the face and hands, along with fatigue, constipation, dry skin, or feeling cold. The swelling is not just “water weight”; thyroid hormone affects how your tissues hold onto fluid and how your kidneys handle salt. If swelling comes with those classic symptoms, checking a thyroid test is more useful than guessing based on how you feel.
Kidney, liver, or heart strain
Swelling can also be a sign that your body is not moving fluid the way it should because of kidney disease, low blood protein from liver problems, or heart failure. This kind of swelling is more concerning when it is new and rapidly worsening, when it affects both legs equally, or when you also feel short of breath, chest pressure, or you cannot lie flat comfortably. If you have those symptoms, or one leg is suddenly much more swollen and painful than the other, get urgent care rather than trying to “wait it out.”
What actually helps the swelling
Do a short sodium “reset”
For one week, aim for mostly home-prepared food and keep sodium predictable, because packaged and restaurant meals can swing wildly even when they taste normal. When you reduce big sodium spikes, your kidneys usually catch up and you often see less morning puffiness and fewer tight shoes by day 3–5. If you want a concrete target, many people do well around 1,500–2,300 mg sodium per day, but the real win is consistency.
Use compression the smart way
If your swelling is ankle-heavy and worse after standing or sitting, knee-high compression socks can reduce pooling and that end-of-day “my legs feel full” sensation. Put them on in the morning before swelling ramps up, because they work better as prevention than as rescue. If you have diabetes with numbness, severe arterial disease, or skin breakdown, ask a clinician which compression level is safe for you.
Elevate and “pump” your calves
Your calf muscles are a built-in pump for returning blood and fluid upward, but they only work when you move them. A simple routine is 2–3 minutes of heel raises or brisk walking every hour you are sitting, plus 15 minutes of legs-up-the-wall in the evening. This targets gravity-driven swelling specifically, so it is more effective than generic “exercise more” advice.
Review meds that cause swelling
Some common medications can cause fluid retention, including certain blood pressure drugs (like amlodipine), anti-inflammatories, and hormone therapies. The swelling is often symmetric and shows up after a dose change, and it can be mistaken for “menopause weight gain.” Do not stop a prescription on your own, but do ask whether an alternative or dose adjustment could reduce swelling without sacrificing control of the condition you are treating.
Treat the driver, not the puffiness
If labs or symptoms point to thyroid, kidney, or heart issues, the most effective relief comes from treating that root cause rather than chasing swelling with random supplements. For example, correcting an underactive thyroid can gradually reduce puffiness over weeks, while kidney-related swelling may require a clinician-guided plan that includes blood pressure control and sometimes a diuretic. If swelling is persistent for more than 2–3 weeks despite lifestyle changes, that is a good threshold to get evaluated.
Lab tests that help explain swelling during menopause
TSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreSodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreCreatinine
Creatinine is a waste product of muscle metabolism that is filtered by the kidneys and serves as the primary marker of kidney function. In functional medicine, creatinine levels reflect not only kidney health but also muscle mass and protein metabolism. Elevated creatinine indicates reduced kidney filtration capacity, while very low levels may indicate muscle wasting or poor protein intake. Creatinine is used to calculate eGFR and helps assess long-term kidney health and detoxification capacity. Creatinine measu…
Learn moreLab testing
Check kidney function, thyroid, and albumin at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do the “ring and shoe check” at the same times each day for two weeks, because swelling that is worse at night and better in the morning points toward gravity and veins more than hormones alone.
If your ankles swell, press a thumb over your shin for 5 seconds; if it leaves a dent that slowly fills in, that is pitting swelling, and it is a useful detail to tell a clinician because it narrows the cause.
Try a restaurant strategy instead of total avoidance: order sauces on the side and skip soups, because those two choices alone often cut a huge sodium load that drives next-day puffiness.
If you sit for work, set a timer for hourly “calf pumps”: 30 heel raises plus a 1-minute brisk walk to the bathroom and back. It sounds small, but it directly moves fluid out of your lower legs.
Take photos when swelling is at its worst (hands, ankles, face) and note your blood pressure that day, because a visual record plus a number helps your clinician take you seriously and act faster.
Frequently Asked Questions
Is swelling during menopause normal?
It can be common, especially in perimenopause, because shifting estrogen can make you more prone to water retention and salt sensitivity. “Common” does not always mean “ignore it,” though—new swelling that is rapidly worsening, one-sided, or paired with shortness of breath deserves prompt evaluation. If it has been persistent for more than 2–3 weeks, consider checking basics like a CMP, TSH, and albumin.
Why are my ankles swollen at the end of the day in menopause?
That pattern often points to gravity and leg veins rather than just hormones, because fluid pools in the lower legs after long sitting or standing. It usually improves overnight and may leave sock marks by evening. Compression socks in the morning plus hourly calf movement is a practical first step, and persistent swelling is a reason to ask about venous insufficiency.
Can menopause cause swelling in hands and fingers?
Yes. Hormone shifts can change how your kidneys handle salt and how easily fluid moves into tissues, so your rings can feel tight even without major weight gain. If hand swelling comes with numbness or tingling at night, it can also overlap with carpal tunnel symptoms, which are more common in midlife. Track timing and triggers for two weeks, and bring that pattern to a visit if it is not improving.
What tests should I ask for if I have swelling?
A good starting set is a comprehensive metabolic panel (CMP) to look at kidney and liver function, TSH to screen for an underactive thyroid, and albumin to see whether low blood protein could be contributing. These do not diagnose every cause, but they catch several important ones that can look like “menopause puffiness.” If you also have chest symptoms or breathlessness, ask specifically about heart evaluation as well.
When is swelling an emergency?
Get urgent care if one leg suddenly becomes much more swollen, painful, red, or warm, because that can signal a blood clot. Also go urgently if swelling comes with new shortness of breath, chest pressure, fainting, or you cannot lie flat without feeling breathless. If you are unsure, it is safer to be checked the same day than to assume it is just menopause.
Research worth knowing about
North American Menopause Society position statement on hormone therapy (context for menopause-related fluid symptoms and when treatment is appropriate)
AHA/ACC/HFSA guideline for the management of heart failure (how clinicians evaluate edema and shortness of breath together)
KDIGO 2024 chronic kidney disease guideline (why eGFR and albumin-related issues matter when swelling persists)