Why Are You Swelling More in Your 40s?
Swelling in your 40s often comes from fluid retention, vein valve weakness, or kidney/heart strain. Targeted labs available at Quest—no referral needed.
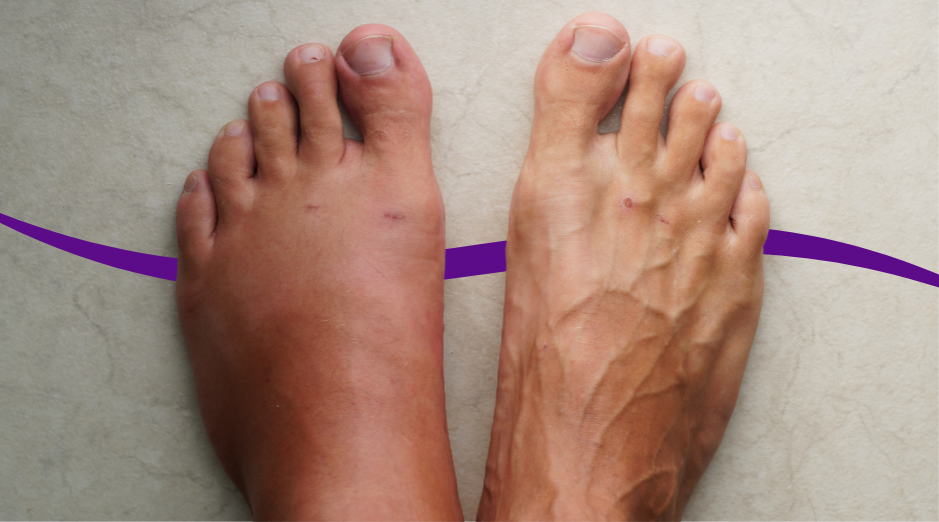
Swelling in your 40s is usually your body holding onto extra fluid, most often from leaky leg veins after long days on your feet, salt-driven water retention, or a medication side effect. Less commonly, it can be a sign that your kidneys, liver, or heart are struggling to manage fluid balance. A few targeted labs can help sort out which bucket you’re in so you’re not guessing. Swelling is frustrating because it can look dramatic while the cause is surprisingly fixable, but it can also be the first visible clue of something you shouldn’t ignore. In your 40s, work and family routines often mean more sitting, more standing, less sleep, and sometimes new meds for blood pressure, pain, or hormones, which all nudge fluid in the same direction. This guide helps you use location and timing clues, know the red flags, and choose smart next steps. If you want help matching your exact pattern to likely causes, PocketMD can talk it through with you, and Vitals Vault labs can help confirm what’s going on.
Why Are You Swelling More in Your 40s?
Leg vein valves getting weaker
If your ankles puff up by evening and look better in the morning, your leg veins may be letting blood pool instead of pushing it back up efficiently. That higher pressure in the veins pushes fluid into nearby tissue, which is why socks leave deep marks and shoes feel tight. The most useful clue is timing: swelling that worsens after standing or sitting and improves with elevation points strongly in this direction.
Salt-driven fluid retention
When you eat more sodium than your kidneys can comfortably excrete that day, your body holds onto water to keep blood sodium stable. You feel it as puffy fingers, a tighter waistband, and a “heavy” feeling in your legs, often within 24–48 hours of restaurant meals or packaged foods. A practical test is a three-day experiment: cook at home with low-sodium choices and see if morning swelling and ring tightness noticeably improve.
Medication side effects
Some common midlife meds make swelling more likely because they relax blood vessels or change kidney salt handling. A classic example is certain blood pressure drugs called calcium channel blockers, which can cause ankle swelling even when your heart is fine. If swelling started within weeks of a new prescription or dose change, bring that timeline to your clinician because a switch or adjustment often fixes it.
Low blood protein from kidney loss
Your blood proteins act like tiny sponges that help keep fluid inside your blood vessels, and when protein drops, fluid leaks into tissue more easily. One reason protein drops is kidney “leakiness” (protein in the urine), which can show up as swelling around the eyes in the morning or swelling that doesn’t fully go away overnight. If you notice foamy urine or new, persistent puffiness, it’s worth checking kidney function and urine protein rather than assuming it’s just “water weight.”
Heart strain and fluid backup
When the heart isn’t pumping effectively, fluid can back up into the legs and sometimes the lungs, which is why swelling can come with shortness of breath or needing extra pillows at night. This is not the most common cause in otherwise healthy 40-somethings, but it matters because it changes what you should do next. If you have swelling plus new breathlessness, chest pressure, or swelling that is rapidly worsening over days, get urgent medical care.
What Actually Helps Swelling Go Down
Use elevation like a tool
If your swelling is worse at the end of the day, you can often “reset” the pressure in your legs by elevating them above heart level for 15–20 minutes. You’ll know it’s working when the tight, stretched feeling eases and sock marks fade faster. Try doing this once mid-day and once in the evening for a week and compare your shoe fit and ankle shape.
Compression that fits your day
Graduated compression socks help because they physically support the veins and reduce fluid leaking into tissue while you’re upright. They work best when you put them on in the morning before swelling builds, and many people do well starting with 15–20 mmHg rather than jumping to very tight medical-grade compression. If one leg is much more swollen than the other, skip self-treating and get checked first because a clot needs a different plan.
A realistic sodium reset
Instead of trying to “eat perfect,” aim for a short, targeted reset that proves whether sodium is your driver. For three to five days, avoid restaurant meals and packaged snacks, and choose foods where you can taste the salt you add rather than the salt that’s hidden. If swelling drops quickly, you’ve found a lever you can pull before big events, travel days, or long shifts.
Move your calf pump on purpose
Your calf muscles are a built-in pump that helps push blood and fluid back up toward your heart, but they only work when you use them. If you sit a lot, set a timer for every 45–60 minutes and do one minute of brisk walking or 20 slow heel raises while holding a counter. This sounds small, but it can noticeably reduce end-of-day ankle swelling because it changes the physics in your veins.
Match the fix to the cause
If a medication is the trigger, the “solution” is often a conversation, not a supplement, because changing the drug can solve the problem without adding new side effects. If labs suggest low thyroid function, treating that can reduce puffiness over weeks as your metabolism and kidney handling of salt normalize. The goal is to stop chasing swelling and start treating the reason your body is holding fluid in the first place.
Useful biomarkers to discuss with your clinician
Protein, Total
Total protein levels reflect nutritional status, liver function (protein synthesis), and kidney function (protein retention). Abnormal levels can indicate liver disease, kidney disease, malnutrition, inflammation, or blood cancers. It provides a general overview of protein metabolism. Total protein measures the combined amount of albumin and globulins in blood. These proteins are essential for maintaining fluid balance, transporting substances, fighting infections, and blood clotting.
Learn moreSodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreCreatinine
Creatinine is a waste product of muscle metabolism that is filtered by the kidneys and serves as the primary marker of kidney function. In functional medicine, creatinine levels reflect not only kidney health but also muscle mass and protein metabolism. Elevated creatinine indicates reduced kidney filtration capacity, while very low levels may indicate muscle wasting or poor protein intake. Creatinine is used to calculate eGFR and helps assess long-term kidney health and detoxification capacity. Creatinine measu…
Learn moreLab testing
Check kidney function, protein levels, and thyroid status at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “morning vs evening” check for one week: take a photo of both ankles when you wake up and again before bed. If swelling is clearly worse at night and better in the morning, vein-related pooling is much more likely than a whole-body cause.
Press your thumb firmly into your shin for five seconds and release. If a dent lingers, that pitting pattern points to fluid in the tissue, which is different from the firmer puffiness you can get with thyroid-related swelling.
If your rings get tight, use them as a simple tracker: note the first day you can’t comfortably remove them and what changed in the prior 48 hours. This often reveals a sodium or medication pattern faster than trying to remember meals.
When you travel or have a long desk day, plan two “calf pump breaks” before you start: one at the 60–90 minute mark and one mid-way through. A minute of heel raises plus a short walk is often enough to prevent the end-of-day ballooning.
If only one leg swells, measure it instead of guessing: wrap a tape measure around both calves at the same height. A difference of about 3 cm (a little over an inch) or more, especially with pain or warmth, is a strong reason to get checked the same day.
Frequently Asked Questions
Is ankle swelling in your 40s normal?
It can be common, especially if it builds through the day and improves overnight, because that pattern often comes from leg veins struggling with gravity. It is not something you should ignore if it is new, rapidly worsening, or happening with shortness of breath. If it keeps recurring, checking creatinine/eGFR, albumin, and TSH can help rule out kidney, protein, or thyroid drivers.
Why do my fingers and rings swell in the afternoon?
Afternoon finger swelling is often fluid retention from sodium, hormonal shifts, or heat, because your body holds extra water to keep blood chemistry stable. It can also happen when you sit for long stretches and your circulation slows down. Try a three-day low-sodium reset and see if ring tightness improves, and consider checking TSH if you also feel unusually tired or cold.
When is swelling an emergency?
Get urgent care if swelling comes with new shortness of breath, chest pressure, coughing up frothy sputum, fainting, or if one leg becomes suddenly swollen and painful. Those patterns can signal heart strain, fluid in the lungs, or a blood clot. If you are unsure, err on the side of being seen the same day.
What labs should I ask for if I have swelling?
A practical starting trio is creatinine with eGFR to assess kidney filtering, albumin to see if low blood protein is letting fluid leak into tissue, and TSH to screen for an underactive thyroid. These three do not diagnose every cause, but they quickly separate “simple pooling” from systemic issues that need follow-up. Bring your swelling pattern and any medication changes to the appointment so results are interpreted in context.
Can blood pressure meds cause ankle swelling?
Yes, certain blood pressure medicines—especially calcium channel blockers—can cause ankle swelling because they widen small arteries and increase pressure in the tiny vessels where fluid can seep out. The swelling is often worse by evening and improves overnight, and it may happen even if your heart and kidneys are fine. Do not stop the medication on your own, but ask about dose changes or alternatives if the timing matches.