Why You’re Getting Swelling in Your 30s
Swelling in your 30s is often from fluid retention, vein issues, or kidney/thyroid shifts. Targeted blood tests available—no referral needed.
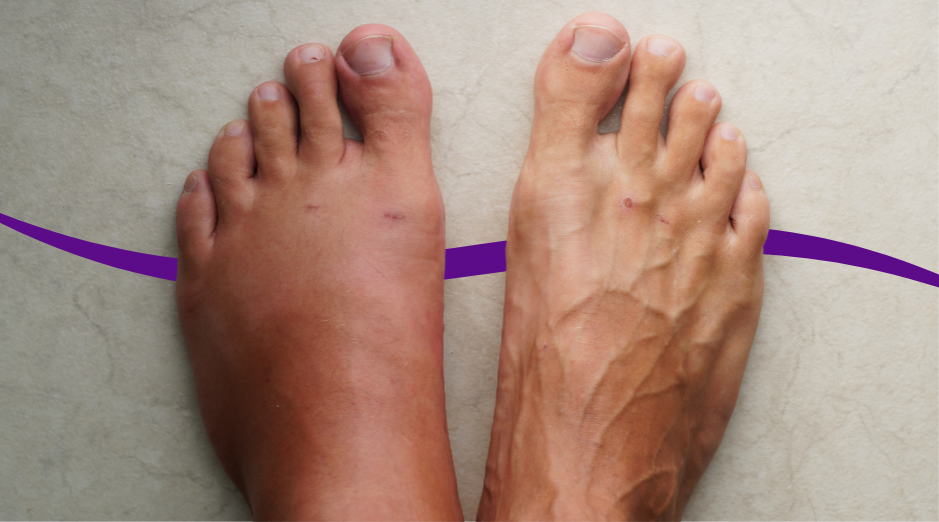
Swelling in your 30s usually means fluid is collecting in the wrong place because your veins are struggling to push blood back up, your body is holding onto salt and water, or your kidneys and proteins aren’t balancing fluid the way they should. Sometimes it is local and mechanical, like an ankle injury, and sometimes it is a whole-body signal, like low thyroid or early kidney strain. A few targeted labs can help sort out which pattern fits you. Swelling is frustrating because it changes how you look and how you move, and it can make you worry that something “big” is wrong. The good news is that most swelling in otherwise healthy 30-somethings has a clear explanation once you pay attention to where it shows up, when it’s worse, and what else is happening in your body. This guide walks you through the most common causes, what actually helps at home, and which blood tests are worth doing. If you want help matching your exact pattern to the most likely cause, PocketMD can talk it through with you, and Vitals Vault labs can help you confirm what’s going on.
Why swelling shows up in your 30s
Veins not moving fluid upward
If your swelling is mostly in your ankles or lower legs and it gets worse as the day goes on, your leg veins may be letting fluid leak out because blood is pooling instead of flowing back up efficiently. This can happen with long hours sitting or standing, pregnancy, or after weight changes, and it often leaves a sock-line dent that lingers. The takeaway is simple: if elevation helps within 30–60 minutes, the problem is often “plumbing” rather than your organs.
Salt-driven water retention
Your kidneys follow sodium, which means a salty day can pull extra water into your bloodstream and then into tissues, especially in your hands, face, and feet. You might notice rings feeling tight in the morning or shoes feeling snug by afternoon, even though nothing else seems wrong. Try a two-day experiment: keep sodium lower and eat potassium-rich foods like beans or yogurt, and see if the puffiness noticeably backs off.
Low blood protein (albumin)
Albumin is the main protein that keeps fluid inside your blood vessels, so when it is low, water slips into tissues more easily and swelling can become more “general,” including around your eyes. Low albumin can come from kidney protein loss, liver problems, or not absorbing enough nutrition, and it matters because it changes how your body handles fluids and medications. If you have swelling plus foamy urine, easy bruising, or ongoing diarrhea, albumin testing is a smart next step.
Kidney strain or protein loss
Your kidneys act like a filter, and when that filter is inflamed or damaged, you can retain salt and water or leak protein into urine, both of which lead to swelling. People often notice puffy eyelids in the morning, swelling that doesn’t improve much with elevation, or blood pressure creeping up. If swelling is new and persistent for more than a week, especially with darker urine or high blood pressure, it is worth checking kidney markers rather than guessing.
Injury or one-sided inflammation
Swelling that is clearly on one side, tied to pain, warmth, or a recent twist, is often your body’s normal inflammatory response as it sends fluid and immune cells to heal tissue. That kind of swelling usually feels tender and stiff, and it can limit range of motion in a way that “water retention” does not. The key is pattern: if one calf or one ankle is suddenly much more swollen than the other, especially with redness or shortness of breath, you should get urgent evaluation to rule out a clot.
What actually helps swelling (and how to tell if it’s working)
Do a 7-day swelling map
Take a quick photo of the same area at the same time each day, and note whether the swelling is worse in the morning or evening. This matters because morning facial puffiness points you toward kidney or protein issues, while evening ankle swelling points you toward vein pooling. Bring that pattern to a clinician or PocketMD, because it often narrows the cause faster than a vague “I’m swollen sometimes.”
Use elevation the right way
If your swelling is in your legs, “feet on the coffee table” often isn’t enough to change the pressure in your veins. Aim for 20–30 minutes with your legs above heart level, and pay attention to whether the tightness and sock-line dent improve. A clear improvement suggests vein pooling or salt-related fluid shifts, while no change makes you think harder about kidney, protein, or inflammation causes.
Try compression when it’s leg-heavy
Graduated compression socks gently squeeze your lower legs, which helps push fluid back toward your heart when you’re on your feet. They work best when you put them on in the morning before swelling builds, and they are especially useful for travel days or long desk days. If compression makes pain sharply worse or one leg is much more swollen than the other, pause and get checked rather than forcing it.
Run a sodium “reset” weekend
Pick two days where you avoid restaurant meals and packaged snacks, and cook simply so you can keep sodium lower without obsessing. If your swelling is mostly fluid retention, you often see a noticeable change in ring tightness, ankle puffiness, or morning facial swelling within 48–72 hours. That response is useful information, because it tells you your body is sensitive to sodium even if your blood pressure is normal.
Know when swelling is urgent
Swelling is not always an emergency, but a few patterns deserve fast care because they can signal a clot, heart strain, or severe infection. If you have sudden one-sided leg swelling, chest pain, new shortness of breath, or swelling plus fainting, go in urgently. If swelling is gradual but persistent and you also have high blood pressure, foamy urine, or fatigue that is out of character, schedule a prompt evaluation and consider labs.
Useful biomarkers to discuss with your clinician
Albumin
Albumin is the most abundant protein in blood plasma, produced exclusively by the liver. In functional medicine, albumin serves as a marker of liver synthetic function, nutritional status, and overall health. Albumin maintains oncotic pressure (keeping fluid in blood vessels), transports hormones and nutrients, and serves as an antioxidant. Low albumin may indicate liver disease, malnutrition, chronic inflammation, or kidney disease. Since albumin has a half-life of about 20 days, it reflects longer-term nutriti…
Learn moreSodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreCreatinine
Creatinine is a waste product of muscle metabolism that is filtered by the kidneys and serves as the primary marker of kidney function. In functional medicine, creatinine levels reflect not only kidney health but also muscle mass and protein metabolism. Elevated creatinine indicates reduced kidney filtration capacity, while very low levels may indicate muscle wasting or poor protein intake. Creatinine is used to calculate eGFR and helps assess long-term kidney health and detoxification capacity. Creatinine measu…
Learn moreLab testing
Check kidney function, thyroid, and albumin at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Press your thumb into the swollen area for five seconds and then release. If a dent stays (pitting), it usually points toward fluid in the tissues, while “no dent” puffiness can fit better with thyroid-related swelling or inflammation.
If your ankles swell by evening, measure your ankle circumference at the same spot in the morning and at night for a week. A consistent swing of even 1–2 cm is a strong clue that gravity and vein pooling are driving the problem.
On travel days, set a timer for every 45–60 minutes and do two minutes of calf pumps by rising onto your toes and slowly lowering. It sounds small, but it mechanically moves fluid out of your lower legs when you’re stuck sitting.
If your rings are tight in the morning, compare two mornings after a salty dinner versus two mornings after a lower-sodium dinner. That simple A/B test often tells you more about water retention than a scale does.
If swelling is new, take your blood pressure at home for three days, morning and evening, and write down the numbers. Swelling plus readings consistently above about 130/80 is a stronger reason to check kidney and thyroid labs promptly.
Frequently Asked Questions
Why are my ankles swollen at the end of the day in my 30s?
Evening ankle swelling usually happens because gravity pulls fluid down and your leg veins are not pushing blood back up efficiently, especially if you sit or stand for long stretches. It often improves with 20–30 minutes of legs-above-heart elevation and can respond well to morning compression socks. If one ankle is suddenly much bigger than the other or you have calf pain, get checked urgently to rule out a clot.
Is swelling a sign of kidney problems?
It can be, especially if you notice puffy eyelids in the morning, swelling that doesn’t improve much with elevation, foamy urine, or rising blood pressure. A CMP (for creatinine and eGFR) plus albumin can help show whether fluid balance and protein levels are contributing. If swelling is persistent for more than a week or keeps recurring, ask for kidney-focused testing rather than assuming it’s “just water weight.”
Can hypothyroidism cause swelling and puffiness?
Yes. Low thyroid can cause a puffy, sometimes non-pitting swelling and it often comes with fatigue, constipation, dry skin, and feeling cold. A TSH test is the usual first step, and many people feel best when TSH is roughly 0.5–2.5 mIU/L, although your clinician will interpret it in context. If your face looks puffier than usual and your energy is dragging, checking TSH is a practical move.
How do I know if my swelling is from salt?
Salt-driven swelling tends to fluctuate quickly and show up as tight rings, puffy fingers, or ankle swelling after restaurant meals or packaged foods. A simple test is a 48–72 hour “sodium reset” where you cook at home and keep meals simple; if swelling noticeably improves, sodium sensitivity is likely part of your picture. Keep that experiment going for a week and you’ll usually identify your biggest triggers.
When should I worry about swelling and go to urgent care?
Go urgently if swelling is sudden and one-sided in a leg, especially with redness, warmth, or calf pain, because that can signal a clot. Also go in if swelling comes with chest pain, new shortness of breath, or fainting. If it’s not sudden but it’s persistent and paired with high blood pressure, foamy urine, or rapid weight gain over a few days, schedule prompt evaluation and consider labs like CMP, albumin, and TSH.
Research and guidelines worth knowing about
KDIGO guideline for evaluating and managing chronic kidney disease (how clinicians interpret eGFR and albumin-related risk)
AHA/ACC/HFSA guideline for heart failure (includes how fluid overload and edema are assessed and treated)
Guidance on chronic venous disease and leg edema (why compression and elevation work when the issue is venous)