Swelling in Your 50s: What It Means and What Helps
Swelling in your 50s often comes from fluid retention, vein valve weakness, or heart/kidney strain. Targeted labs available at Quest—no referral needed.
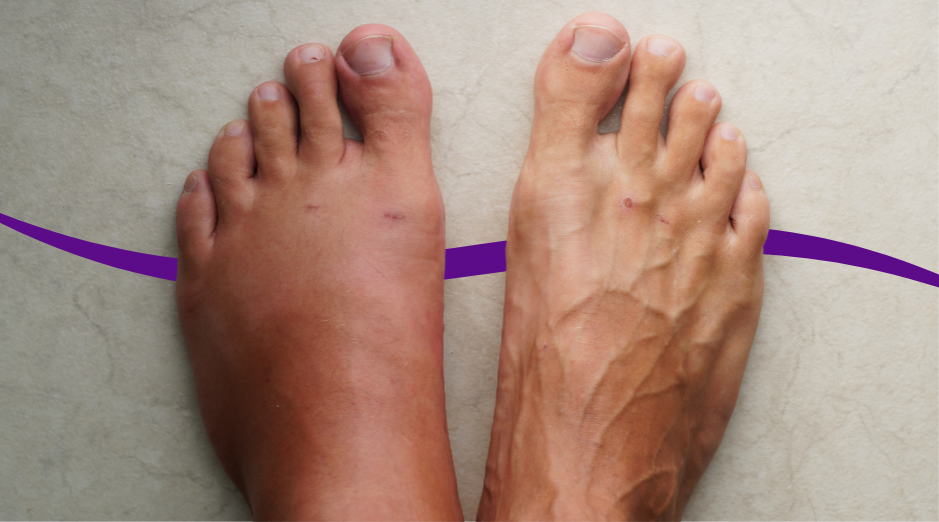
Swelling in your 50s is usually your body holding onto extra fluid because blood isn’t returning from your legs efficiently, your hormones and salt balance have shifted, or your heart or kidneys are under strain. The pattern matters: swelling in both ankles after a long day points to veins and fluid balance, while one-sided swelling or sudden swelling needs faster attention. A few targeted labs can help sort out whether this is mainly kidney-related, heart-related, or “just” fluid retention. Swelling can be annoying in a very practical way, because shoes stop fitting and rings feel tight, but it can also feel scary because you’re wondering if it’s your heart or kidneys. In your 50s, you’re also more likely to be on medications that cause swelling, and you may be navigating menopause, higher blood pressure, or less daily movement than you used to get. This guide walks you through the most common causes, what helps at home, and which tests can make the next step clearer. If you want help matching your exact pattern to the most likely causes, PocketMD can talk it through with you, and Vitals Vault labs can help you check the most relevant markers.
Why swelling shows up in your 50s
Leg veins aren’t pushing back well
Over time, the one-way valves in your leg veins can get leaky, so blood pools in your lower legs when you’re sitting or standing. That extra pressure pushes fluid out into the tissues, which is why your ankles look puffy by evening and feel better after a night in bed. A practical clue is “sock lines” and swelling that’s worse at the end of the day, so elevating your legs for 20 minutes can be a quick at-home test of whether veins are a big part of your story.
Salt, carbs, and hormones shift fluid
Your kidneys hold onto sodium, and where sodium goes, water follows, which can make your fingers and face feel puffy and your shoes feel tight. In your 50s, menopause-related hormone changes can make you more salt-sensitive, and higher-carb meals can temporarily pull water into your tissues through glycogen storage. If your swelling swings up and down within 24–48 hours, try a one-week experiment where you keep restaurant and packaged foods low and see if your morning-to-evening change shrinks.
Medication side effects cause edema
Some common meds in midlife relax blood vessels or change kidney handling of salt, which can lead to ankle swelling even when your heart and kidneys are otherwise okay. Calcium channel blockers for blood pressure are classic for this, and anti-inflammatory pain relievers can also make you retain fluid. If your swelling started within weeks of a new prescription or dose change, bring that timeline to your clinician, because a switch within the same drug class can sometimes fix the problem.
Kidneys leaking protein or under-filtering
Your kidneys normally keep protein in your bloodstream, and that protein helps hold fluid inside your blood vessels. If you’re losing protein in urine or your filtering rate drops, fluid can drift into tissues and show up as swelling in your legs or around your eyes. Swelling that’s new, persistent, and paired with foamy urine or rising blood pressure is a reason to check kidney labs sooner rather than later.
Heart strain backing up fluid
When your heart isn’t pumping forward efficiently, fluid backs up into the lungs and the veins, and gravity pulls some of it into your ankles and shins. You might notice you get winded more easily, you need extra pillows at night, or you wake up short of breath, which is a different feel than simple “puffy feet.” If swelling comes with chest pressure, new severe shortness of breath, or one leg that is suddenly much more swollen and painful than the other, treat that as urgent and get evaluated right away.
What actually helps reduce swelling
Use leg elevation strategically
Elevation works best when you do it long enough and high enough to let fluid drain, which usually means 15–30 minutes with your calves above heart level. If your swelling is mainly from vein pooling, you’ll often see a visible change after a week of doing this once mid-day and once in the evening. Pair it with ankle pumps while elevated, because muscle contractions act like a second heart for your legs.
Try compression the right way
Graduated compression socks help by squeezing fluid back toward your core, but they work best when you put them on in the morning before swelling builds. For many people, 15–20 mmHg is a comfortable starting point, and you can go higher with clinician guidance if needed. If you have numbness, severe pain, or known peripheral artery disease, get advice before using strong compression.
Run a 7-day sodium audit
Most “mystery swelling” diets are really sodium problems hiding in sauces, bread, deli meats, and restaurant meals. For one week, keep meals simple and home-prepared, and aim for roughly 1,500–2,300 mg of sodium per day unless your clinician has given you a different target. If your swelling improves quickly, you’ve learned something powerful about your personal salt sensitivity, and you can focus on the biggest sources rather than trying to be perfect.
Move your calves on purpose
If you sit a lot, your calf muscles stop doing their pumping job, and fluid collects in your lower legs. Set a timer to stand every 30–45 minutes and do 20 heel raises or a brisk two-minute walk, because that’s enough to squeeze veins and lymphatic channels. This is especially helpful if your swelling is worse on travel days or after long meetings.
Review meds and pain relievers
If you’re using anti-inflammatory pain relievers frequently for joint pain, they can quietly increase fluid retention and raise blood pressure in some people. Bring a full list of prescriptions, over-the-counter meds, and supplements to your next visit, and ask directly, “Which of these can cause swelling, and what are my alternatives?” If a blood pressure medication is the likely culprit, a clinician can often adjust the regimen without sacrificing control.
Useful biomarkers to discuss with your clinician
Urine Protein
Proteinuria is a key marker of kidney disease and damage. It indicates glomerular or tubular dysfunction. Persistent proteinuria is associated with progressive kidney disease, cardiovascular disease, and increased mortality. Early detection allows intervention to slow progression. Urine protein testing detects the presence of protein, primarily albumin, in urine. Normal urine contains minimal protein; elevated levels indicate kidney damage or disease.
Learn moreSodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreCreatinine
Creatinine is a waste product of muscle metabolism that is filtered by the kidneys and serves as the primary marker of kidney function. In functional medicine, creatinine levels reflect not only kidney health but also muscle mass and protein metabolism. Elevated creatinine indicates reduced kidney filtration capacity, while very low levels may indicate muscle wasting or poor protein intake. Creatinine is used to calculate eGFR and helps assess long-term kidney health and detoxification capacity. Creatinine measu…
Learn moreLab testing
Get kidney, heart-strain, and protein-loss labs checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “morning vs evening” check for three days: take a photo of your ankles when you wake up and again before bed. If the difference is dramatic, veins and daily fluid shifts are likely playing a big role, and compression plus calf movement usually pays off.
Press your thumb into your shin for five seconds and see what happens when you lift it. If a dent lingers (pitting swelling), fluid overload is more likely than simple joint inflammation, which helps you choose the right next step.
If you fly or drive for more than two hours, treat it like a swelling trigger: wear compression socks, stand up at least once an hour, and do ankle circles in your seat. Your future self will feel the difference that evening.
When you’re testing sodium, don’t guess—read one label per meal for a week. If a single “healthy” soup or sauce has 700–900 mg of sodium, you’ve found why your shoes suddenly feel tight the next day.
If one leg is consistently more swollen than the other, measure both calves at the same spot (for example, 10 cm below the kneecap) and write the numbers down. Bring that to your appointment, because asymmetry changes what your clinician needs to rule out.
Frequently Asked Questions
Why are my ankles swollen at night but fine in the morning?
That pattern usually means gravity and vein pooling are driving the swelling, so fluid collects while you’re upright and drains when you lie down. It’s common with chronic venous insufficiency and with long sitting or standing days. Try 15–30 minutes of leg elevation in late afternoon and see if your evening swelling shrinks within a week.
Is swelling in your 50s a sign of heart failure?
It can be, but most ankle swelling in otherwise stable people is from veins, salt sensitivity, or medications. Heart-related swelling is more concerning when it comes with shortness of breath, reduced exercise tolerance, needing extra pillows, or waking up breathless. A blood test like NT-proBNP plus an exam can help sort this out quickly.
What medications commonly cause ankle swelling?
Blood pressure medicines called calcium channel blockers are a frequent cause, and swelling can show up even if your blood pressure is well controlled. Anti-inflammatory pain relievers can also increase fluid retention in some people, especially if you use them often. If swelling started after a new medication or dose change, bring that timeline to your prescriber and ask about alternatives.
How can I tell if swelling is from my kidneys?
Kidney-related swelling is more likely if it’s persistent, more generalized, or paired with foamy urine, rising blood pressure, or swelling around the eyes. Testing helps: a CMP looks at creatinine/eGFR and albumin, and a urine albumin-to-creatinine ratio (uACR) checks for protein leakage. If uACR is over 30 mg/g, that’s a concrete reason to follow up.
When should I worry about swelling in one leg?
One-sided swelling is more concerning because it can come from a clot, an injury, or a blocked vein or lymph channel. If one leg becomes suddenly more swollen, painful, warm, or red, get urgent evaluation the same day. If it’s been gradually one-sided for weeks, measure both calves and bring the numbers to a clinician to guide the workup.
Research and guidelines worth knowing
2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure (includes edema evaluation and natriuretic peptides)
KDIGO 2024 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease (proteinuria and uACR use)
Society for Vascular Surgery/American Venous Forum guidelines on chronic venous disease and compression therapy