Hair Thinning Under Stress: What It Means and What Helps
Hair thinning under stress is often telogen effluvium, thyroid shifts, or low iron. Targeted blood tests are available at Quest—no referral needed.
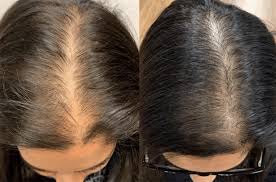
Hair thinning under stress is usually caused by a “shedding shift” called stress shedding (telogen effluvium), where more hairs than usual move into the resting phase and fall out a few months later. It can also be stress uncovering a separate issue like low iron stores, thyroid imbalance, or postpartum hormone changes. A few targeted labs can help you figure out which pattern fits your body so you’re not guessing. Seeing more hair in the shower drain can feel personal, even when it’s a common body response to a rough season. The tricky part is timing: the stressful event and the shedding often do not happen at the same time, which makes it easy to blame the wrong thing or panic that it’s “permanent.” This page helps you tell stress shedding from other common causes, gives you a realistic timeline for regrowth, and shows which blood tests are most useful. If you want help sorting your exact pattern and next steps, PocketMD can talk it through with you, and Vitals Vault labs can help confirm what’s going on.
Why your hair thins when you’re stressed
Stress shedding (telogen effluvium)
When your body goes through a shock—emotional stress, illness, surgery, intense work burnout—it can “reassign” hair follicles into a resting mode. About 2–3 months later, those resting hairs shed, which is why the timing feels confusing. The key clue is diffuse shedding all over your scalp rather than a single bald patch, and the most helpful takeaway is to look back 8–12 weeks for a trigger instead of only focusing on what happened this week.
Low iron stores, even mild
Your hair follicles are high-demand tissue, and they notice when your iron reserves are running low, even if your hemoglobin is still normal. This often shows up as more shedding plus feeling colder than usual, getting winded easily, or having heavier periods. If you suspect this, ferritin is the test that matters most, and many hair specialists aim for ferritin above about 50 ng/mL for hair support rather than just “in range.”
Thyroid imbalance affecting growth
Your thyroid hormone sets the pace for many body processes, including how long hair stays in its growth phase. When thyroid function is low, hair can become finer and shed more, and you might also notice constipation, dry skin, or feeling unusually tired. Because stress and thyroid symptoms can overlap, a simple TSH test can be a reality check before you assume it is “just stress.”
Postpartum hormone shift and sleep loss
After pregnancy, the hormone environment changes quickly, and many hairs that were “held” in the growth phase during pregnancy enter resting at the same time. The shedding typically peaks around 3–4 months postpartum, and sleep deprivation and nutritional depletion can make it feel worse. The takeaway is that postpartum shedding is usually temporary, but it is still worth checking iron stores if you had blood loss at delivery or you feel wiped out.
Pattern hair loss made obvious
Sometimes stress is not the root cause, but it makes you notice thinning that was already developing from genetics and hormones. This type often looks like widening of the part or thinning at the crown, and it tends to progress slowly rather than coming on suddenly. If your shedding is not improving after 6 months, or you see a clear pattern rather than diffuse loss, it is worth asking a clinician or dermatologist about pattern hair loss so you can start targeted treatment early.
What actually helps stress-related thinning
Give it a real timeline
Stress shedding is delayed, and regrowth is slow, so quick fixes almost always disappoint. Many people see shedding calm down within 3–6 months after the trigger resolves, and visible fullness often takes another 3–6 months because hair grows roughly 1 cm per month. Your job is to track trend lines, not day-to-day shedding, so take monthly photos in the same lighting and part line.
Fix the “hidden” deficiency first
If ferritin is low, replacing iron can be the difference between ongoing shedding and steady regrowth, but it has to be done consistently and safely. Pairing iron with vitamin C and taking it away from calcium can improve absorption, while taking it with coffee or tea can blunt it. The practical move is to recheck ferritin after about 8–12 weeks so you know you are actually refilling stores rather than guessing.
Treat thyroid issues, not symptoms
If TSH suggests hypothyroidism, treating the thyroid problem can normalize the hair cycle over time, but hair usually lags behind energy and mood improvements. It is common to need a few months after thyroid levels stabilize before hair looks better. Bring your hair timeline to your clinician, because it helps them interpret whether your dose is truly optimized or still drifting.
Use minoxidil if thinning persists
Topical minoxidil can help if stress uncovered pattern thinning, and it can also support regrowth after shedding by extending the growth phase. The catch is that you may see a temporary increase in shedding in the first 2–8 weeks, which is often a sign the follicles are cycling rather than a sign you are “losing more hair forever.” If you try it, commit to at least 4–6 months before judging results.
Reduce scalp inflammation gently
Stress can worsen dandruff and scalp irritation, and inflamed skin does not support healthy follicles. If you have itch, flakes, or scalp tenderness, using an anti-dandruff shampoo a few times a week and avoiding harsh oils or aggressive scratching can calm the environment. A calmer scalp does not fix every type of hair loss, but it removes a common “extra brake” on regrowth.
Useful biomarkers to discuss with your clinician
Ferritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreTSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreIron Binding Capacity
TIBC helps distinguish between different causes of abnormal iron levels. High TIBC indicates iron deficiency (the body increases transferrin to capture more iron), while low TIBC suggests iron overload or chronic disease. It's essential for accurate iron status assessment. Total Iron Binding Capacity (TIBC) measures the blood's capacity to bind iron with transferrin, the main iron transport protein. It indirectly reflects transferrin levels and iron status.
Learn moreLab testing
Check ferritin, TSH, and vitamin D at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a 60-second “part line check” once a month: take a photo of your part from the same angle and lighting, because your brain is terrible at noticing slow change without a reference.
If you are shedding, be extra gentle when detangling: use conditioner, start from the ends, and stop brushing once your hair is dry, because dry brushing can turn normal shed hairs into breakage that looks like more loss.
Look for the timing clue: if the shedding started 8–12 weeks after a stressful event or illness, that delay strongly points toward stress shedding rather than an immediate reaction to a new shampoo or supplement.
If you are postpartum, treat sleep like a medical intervention: even one protected 3–4 hour block most nights can reduce the stress load that keeps shedding feeling relentless.
When you start iron or minoxidil, write down the start date and commit to a checkpoint at 12 weeks, because hair responds slowly and you will otherwise quit right before it begins to pay off.
Frequently Asked Questions
How long does stress hair loss last?
With stress shedding (telogen effluvium), the shedding often begins about 2–3 months after the trigger and then gradually improves over the next 3–6 months. Visible thickening usually takes longer because hair grows about 1 cm per month, so many people need 6–12 months to feel “back to normal.” If you are still worsening after 6 months, it is worth checking ferritin and TSH and considering pattern hair loss.
Can anxiety cause hair thinning even if I’m eating fine?
Yes, because anxiety can act like a chronic stress signal that nudges more follicles into the resting phase, even when your nutrition is decent. It can also disrupt sleep, which is a big deal for hair cycling and recovery. If the timing fits and you are shedding diffusely, treat it like stress shedding and consider checking ferritin and TSH so you do not miss a fixable driver.
What blood tests should I get for hair thinning under stress?
The most useful starting trio is ferritin for iron stores, TSH for thyroid signaling, and 25-hydroxy vitamin D for a common, silent deficiency that can slow regrowth. These tests help separate “stress triggered it” from “stress revealed it,” which changes what you do next. Bring your results and your shedding timeline to a clinician if anything is abnormal or borderline.
Is stress hair loss permanent?
Stress shedding is usually temporary because the follicles are not scarred; they are just cycling differently for a while. It can feel permanent when the trigger is ongoing or when low ferritin or thyroid imbalance is also present and keeps the cycle disrupted. If you see widening of the part or crown thinning that keeps progressing, ask about pattern hair loss because that type benefits from early treatment.
When should I see a doctor for hair thinning?
Go sooner if you have sudden bald patches, scalp pain, pus, or thick scale, because those can signal conditions that need prompt treatment. You should also get evaluated if shedding is heavy for more than 3 months, if you are postpartum and feel unusually exhausted or lightheaded, or if you have symptoms of thyroid issues like constipation and cold intolerance. A simple plan is to get ferritin and TSH checked and then review the results with a clinician or PocketMD to decide the next step.