Hair Thinning With Depression: What It Usually Means
Hair thinning with depression often comes from stress shedding, thyroid imbalance, or low iron. Targeted blood tests are available—no referral needed.
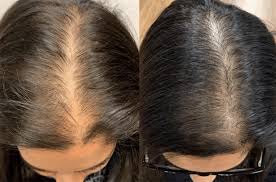
Hair thinning with depression is often a timing problem in your hair cycle: stress and low mood can push more hairs into a “resting” phase so they shed a few months later, and thyroid or iron issues can make that shedding worse. Some antidepressants can also trigger extra shedding, especially in the first months. A few targeted labs can help you figure out which of these is driving your hair changes. It’s hard because hair loss feels personal and visible, and depression already chips away at confidence. You might be staring at your part line or shower drain and wondering if this is “just stress,” genetics, or something fixable. The good news is that many common causes of diffuse thinning are reversible, but they improve on hair-timeline, not mood-timeline. If you want help sorting your pattern, triggers, and meds, PocketMD can talk it through, and Vitals Vault labs can help you check for the most common medical contributors.
Why hair thins when you’re depressed
Stress shedding (telogen effluvium)
When your body is under psychological stress, more hair follicles shift into a resting phase, and those hairs shed about 2–3 months later. That delay is why your hair can start thinning after a rough season, even if things feel “calmer” now. A useful clue is sudden, diffuse shedding all over your scalp rather than a single bald patch, and the most helpful action is to think back 8–12 weeks for triggers like a depressive episode, poor sleep, illness, or major life change.
Low iron stores, even without anemia
Your hair follicles are high-demand tissue, so when your iron reserves are low, your body quietly rations resources away from hair growth. You can have normal hemoglobin and still have low ferritin, which is the storage form of iron, and that can show up as thinning, more shedding, and hair that seems to stop growing past a certain length. If your periods are heavy, you’re postpartum, you donate blood, or you eat little red meat, ferritin testing is often the fastest way to confirm or rule this out.
Thyroid slowdown or overdrive
Your thyroid hormones act like a “metabolic volume knob” for many tissues, including your scalp, so both low and high thyroid function can cause diffuse thinning and a change in hair texture. The tricky part is that thyroid problems can also mimic or worsen depression, so it can feel like one big fog rather than two separate issues. If you also notice cold intolerance, constipation, palpitations, or unexplained weight change, checking TSH is a practical next step.
Antidepressant-related shedding
Some people notice increased shedding after starting, stopping, or changing the dose of an antidepressant, and it usually shows up as diffuse thinning rather than a specific pattern. This is often another version of hair-cycle disruption, which means it can improve once your body settles on a stable dose, but it can take months to see the change. Don’t stop your medication abruptly for your hair; instead, bring the timing to your prescriber so you can weigh options like dose adjustments or switching within the same class.
Pattern hair loss unmasked by depression
Androgen-sensitive hair thinning (pattern hair loss) can progress slowly for years, but depression can make you notice it more because you’re looking closer, and stress shedding can temporarily thin the “background” hair that was camouflaging it. This often looks like widening at the part line or thinning at the crown, and it tends to be more gradual than telogen effluvium. If you see a consistent pattern over 6–12 months, it’s worth discussing proven treatments early, because earlier intervention tends to preserve more density.
What actually helps your hair recover
Treat the trigger, then wait 3 months
Hair recovery lags behind life because follicles need time to re-enter the growth phase, so the first visible improvement often takes 8–12 weeks after the trigger is addressed. That waiting period is frustrating, but it’s also reassuring: ongoing shedding doesn’t always mean you’re still “getting worse.” Pick one main hypothesis to act on first—like stabilizing a medication change or correcting low ferritin—and track shedding weekly rather than daily.
Correct low ferritin thoughtfully
If ferritin is low, iron replacement can reduce shedding and support regrowth, but it works best when you take it consistently and you fix the reason it got low. Many people tolerate iron better when they take it every other day, and pairing it with vitamin C can improve absorption, while taking it with calcium or antacids can blunt it. Recheck ferritin after about 8–12 weeks so you know you’re moving toward a hair-friendly target rather than guessing.
Address thyroid imbalance with your clinician
If TSH suggests hypothyroidism or hyperthyroidism, treating the thyroid issue often improves both mood symptoms and hair changes, but the hair timeline is still slow. You may notice less breakage and less shedding before you see obvious thickening. Ask for a plan that includes follow-up labs after a dose change, because being slightly over- or under-treated can keep hair stuck in a shedding cycle.
Consider topical minoxidil for thinning
Topical minoxidil can help many people with pattern thinning and can also support recovery after stress shedding by nudging follicles into growth. The catch is that you may see a brief increase in shedding in the first 2–8 weeks, which is usually a sign hairs are cycling, not a sign you’re harming your scalp. If you try it, commit to at least 4–6 months before judging results, and use it consistently rather than “on and off” during bad weeks.
Make depression treatment hair-friendly
When depression is the driver, the goal is not perfection—it is steadier sleep, steadier eating, and fewer physiological stress spikes, because your follicles respond to your body’s overall stress chemistry. A small, repeatable routine helps more than a big makeover, like a protein-forward breakfast you can tolerate even on low-appetite days and a fixed wind-down time to protect sleep. If your hair loss started after a medication change, bring a simple timeline to your prescriber so you can problem-solve without sacrificing mental health stability.
Lab tests that help explain hair thinning with depression
Ferritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreTSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreIron Binding Capacity
TIBC helps distinguish between different causes of abnormal iron levels. High TIBC indicates iron deficiency (the body increases transferrin to capture more iron), while low TIBC suggests iron overload or chronic disease. It's essential for accurate iron status assessment. Total Iron Binding Capacity (TIBC) measures the blood's capacity to bind iron with transferrin, the main iron transport protein. It indirectly reflects transferrin levels and iron status.
Learn moreLab testing
Check ferritin, TSH, and vitamin D at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a two-minute “hair timeline” note in your phone: write down when shedding started, then look back 8–12 weeks for a depressive dip, medication change, illness, or postpartum shift. That timing pattern is one of the strongest clues for stress shedding.
If you want a quick at-home gauge of shedding, count hairs on your brush after one consistent routine (same wash schedule, same brush) once a week. Watching the trend is more useful than obsessing over one scary shower.
Treat your scalp gently while you’re shedding: skip tight hairstyles and aggressive heat for a month, because breakage can masquerade as “more hair loss” and make you feel worse than you need to.
If you’re postpartum, remember that shedding often peaks around 3–4 months after delivery and then improves. If it keeps worsening past 6–9 months, that is a good moment to check ferritin and TSH rather than assuming it’s still “just postpartum.”
Bring a simple one-page summary to appointments: your shedding start date, your current meds and dose changes, your period pattern, and any symptoms like cold intolerance or heavy bleeding. You’ll get a better plan faster because you’re not trying to remember everything on the spot.
Frequently Asked Questions
Can depression itself cause hair thinning?
Yes. Depression can act as a chronic stressor that shifts more follicles into a resting phase, which leads to shedding about 2–3 months later (stress shedding). It can also indirectly contribute by disrupting sleep and appetite, which makes nutrient deficits more likely. If the timing fits, focus on stabilizing mood and check ferritin and TSH to rule out common medical amplifiers.
How do I know if my hair loss is stress shedding or genetic?
Stress shedding is usually sudden and diffuse, and you often notice handfuls of hair in the shower with a start date you can roughly name. Pattern hair loss is slower and more “mapped,” such as widening at the part or thinning at the crown over many months. If you’re unsure, take monthly photos in the same lighting and part, because patterns show up clearly over 3–6 months.
Do antidepressants cause hair loss, and will it grow back?
Some people do experience increased shedding after starting or changing an antidepressant, and it is typically diffuse rather than patchy. It often improves after your body adapts or after a medication adjustment, but regrowth still takes months because follicles cycle slowly. The most practical step is to bring a start-date and dose-change timeline to your prescriber before making any changes yourself.
What ferritin level is best for hair growth?
For hair shedding, many clinicians aim for ferritin around 50–70 ng/mL or higher, even though the lab “normal” range may start much lower. Levels in the teens or 20s are commonly associated with diffuse thinning, especially if you have heavy periods or you’re postpartum. If your ferritin is low, recheck it after about 8–12 weeks of treatment to confirm it is rising.
When should I worry that hair thinning is something serious?
Get prompt medical care if you have sudden bald patches, scalp pain or scaling, signs of infection, or hair loss with new symptoms like a racing heart, fainting, or rapid unexplained weight change. Those patterns can point to conditions that need targeted treatment rather than watchful waiting. If your shedding is diffuse but persistent beyond 6 months, ask for an evaluation and consider labs like TSH, ferritin, and vitamin D to avoid missing a fixable cause.
