Why Your Skin Gets So Dry in Perimenopause
Dry skin perimenopause often comes from estrogen shifts, slower skin oil production, and thyroid changes. Targeted blood tests available—no referral needed.
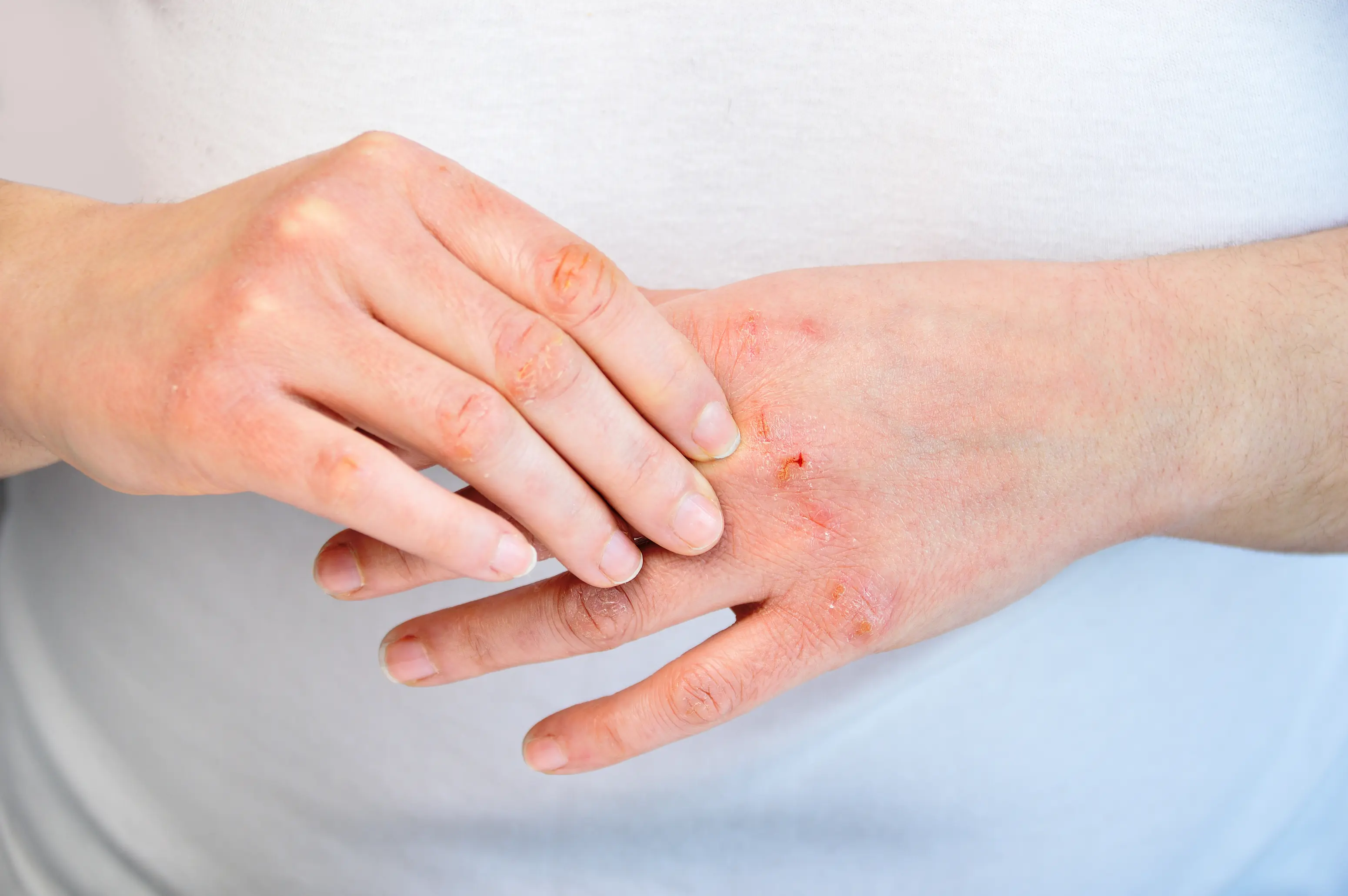
Dry skin in perimenopause usually happens because estrogen starts fluctuating and trending down, which weakens your skin barrier and reduces natural oils. Thyroid slowdowns and low iron can also make your skin feel rough, tight, and itchy even when you moisturize. A few targeted labs can help you figure out which driver fits your body. This can be surprisingly frustrating because you can do “all the right things” and still feel like your skin is drinking lotion and staying dry. Perimenopause also overlaps with life changes that dry skin out on their own, like more indoor heating, stress, and disrupted sleep. Below, you’ll see the most common causes, what actually helps (including ingredient-level guidance), and the blood tests that are worth considering. If you want help connecting your symptoms into a plan, PocketMD can talk it through with you, and Vitals Vault labs can help you check the internal contributors.
Why your skin gets so dry in perimenopause
Estrogen drops weaken your barrier
As estrogen fluctuates and gradually declines, your skin makes fewer of the lipids and “glue” that keep water sealed in. That means moisture escapes faster, so your face and body can feel tight right after washing and itchy by afternoon. If dryness showed up alongside cycle changes, new hot flashes, or sleep disruption, hormones are a very plausible driver, and barrier-focused skincare usually helps more than switching to a heavier lotion.
Less skin oil, more rough texture
Perimenopause can reduce oil production, especially on your cheeks, shins, and forearms, which makes skin feel papery and look dull. You might notice makeup clinging to dry patches or fine lines looking suddenly more obvious because dry skin reflects light differently. The takeaway is to treat dryness like an “oil-and-water” problem, which means pairing a humectant (water-binding) product with an oil or balm to lock it in.
Thyroid slowdown can mimic menopause
An underactive thyroid (hypothyroidism) can slow skin cell turnover and reduce sweat and oil, which leaves skin dry, cool, and sometimes puffy. It can look like perimenopause on the surface, but the fix is different, and you may also notice constipation, hair thinning, or feeling unusually cold. If dryness is new and persistent, a simple TSH and free T4 blood test can be a high-value check.
Eczema flares from a fragile barrier
When your barrier is weaker, irritants and allergens get in more easily, and your immune system can overreact, which can trigger eczema (atopic dermatitis) flares even if you have not had them in years. This often feels like intense itch with red, scaly patches, especially on hands, eyelids, neck, or behind knees. If itching is keeping you up or you see cracking or oozing, it is worth treating it as eczema early with fragrance-free care and a clinician visit for prescription options if needed.
Dry air and hot showers amplify it
Perimenopause can lower your margin for error, so the same winter heating or long hot shower that used to be fine now strips oils and worsens water loss. You feel it as post-shower tightness, flaky shins, and hands that crack after washing dishes. The practical move is to change the environment and the routine, because no cream can fully outwork daily barrier stripping.
What actually helps perimenopause dry skin
Moisturize like a barrier repair plan
Look for a fragrance-free moisturizer that contains ceramides, glycerin, or hyaluronic acid, because these support the barrier and hold onto water. Apply it within three minutes of bathing while your skin is still slightly damp, and then add a thin layer of petrolatum or a facial oil on top if you are still getting tightness. This “layering” approach usually beats buying a single expensive cream.
Change how you cleanse
Switch to a gentle, non-foaming cleanser on your face and a mild body wash only where you truly need it, because harsh surfactants remove the oils you are trying to keep. Keep showers warm rather than hot and aim for under 10 minutes, which reduces the amount of lipid stripping. If your skin stings when you wash, that is a sign your barrier is irritated and needs a simpler routine for a couple of weeks.
Use urea or lactic acid on body
For rough, scaly areas like shins, elbows, and heels, a lotion with urea or lactic acid can soften thickened dry skin by gently loosening the “dead skin” layer. Start a few nights per week and increase as tolerated, because overdoing acids can sting when your barrier is already fragile. If you get eczema patches, keep acids off the inflamed areas and use a plain moisturizer there instead.
Treat itch before you scratch
Itch can become a loop, because scratching damages the barrier and creates more inflammation, which makes you itch again. Short-term, a cool compress and a thick ointment can calm the nerve endings, and an over-the-counter 1% hydrocortisone can help small irritated spots for up to a week. If you are needing steroid cream repeatedly or the itch is widespread, that is a good moment to ask a clinician about eczema, allergy, or other skin conditions.
Address internal contributors you can fix
If labs show low ferritin (iron stores) or low vitamin D, correcting them can support healthier skin turnover and reduce the “everything feels dry” feeling. If thyroid testing suggests hypothyroidism, treating it often improves dryness over a few months as your skin cycle normalizes. This is where testing helps, because you do not want to guess and supplement blindly when a targeted plan would work better.
Useful biomarkers to discuss with your clinician
TSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreEstradiol
Estradiol in men is produced from testosterone via aromatase enzyme. In functional medicine, we recognize that men need optimal estradiol levels for bone health, cognitive function, and cardiovascular protection. However, excessive estradiol can suppress testosterone production and cause feminizing effects. The testosterone-to-estradiol ratio is crucial for male health, with optimal balance supporting vitality while preventing estrogen dominance. Balanced estradiol levels in men support bone health and cognitive…
Learn moreDhea Sulfate
DHEA-S levels reflect adrenal function and decline naturally with age. It's used to evaluate adrenal tumors, congenital adrenal hyperplasia, and androgen excess conditions like PCOS. Some consider it a marker of biological aging and stress resilience. DHEA-Sulfate (DHEA-S) is a hormone produced by the adrenal glands that serves as a precursor to sex hormones (testosterone and estrogen). It's the most abundant steroid hormone in the body.
Learn moreLab testing
Get TSH, free T4, ferritin, and vitamin D checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a two-week “barrier reset” where you use only a gentle cleanser, one fragrance-free moisturizer, and sunscreen on your face. If your dryness improves, you have learned that irritation from products was part of the problem.
After every hand wash, apply a pea-sized amount of thick cream and then a tiny smear of petrolatum over the knuckles. If you do this for three days straight, many painful cracks start to close.
If your legs are the worst, try applying moisturizer before you fully dry off, and then put on soft cotton leggings for 30–60 minutes. That little bit of occlusion helps the product actually stay on your skin instead of on your clothes.
Run a humidifier in your bedroom during heating season and aim for around 40–50% humidity. If you wake up less itchy and your lips are less chapped, the environment was a bigger driver than you thought.
Patch-test new actives by putting them on the same small spot near your jawline or inner forearm for three nights. If you get stinging or redness, skip it for now and focus on barrier repair first.
Frequently Asked Questions
Can perimenopause really cause dry, itchy skin?
Yes. Estrogen shifts can weaken your skin barrier and reduce natural oils, which makes water escape faster and can trigger itch. If the timing lines up with other perimenopause changes like irregular cycles or new sleep issues, hormones are a common explanation. Start with barrier repair for two weeks, and consider checking TSH and ferritin if it is persistent.
Why is my skin dry even when I moisturize?
Often you are adding water but not sealing it in, especially if your barrier is irritated from hot showers, harsh cleansers, or fragranced products. Try applying moisturizer within three minutes of bathing and topping it with a thin occlusive layer like petrolatum on the driest areas. If your skin still feels dry plus you are cold, constipated, or losing hair, ask for TSH and free T4 testing.
What is the best ingredient for perimenopause dry skin?
Ceramides help rebuild the barrier, glycerin pulls water into the outer skin, and petrolatum is one of the most effective sealants for preventing water loss. If your body skin is rough and scaly, urea (often 10–20%) can make a noticeable difference within a week. Pick one fragrance-free product you will actually use daily and give it 14 days before you judge it.
Should I get hormone tests for dry skin in perimenopause?
Hormone levels can swing day to day in perimenopause, so a single estradiol result does not always explain symptoms. If your main symptom is dryness, thyroid testing (TSH with free T4) and ferritin are often more actionable because they can reveal treatable contributors. If you also have significant hot flashes, cycle changes, or vaginal dryness, discussing hormone therapy options with a clinician can be reasonable.
When is dry skin a sign of something more serious?
If you have widespread redness, painful cracking, oozing, fever, or a rapidly spreading rash, you should get urgent medical care because infection or a severe dermatitis can develop. Dryness with unexplained weight change, marked fatigue, or feeling unusually cold can point to thyroid issues, which is worth checking with TSH and free T4. If you are unsure, take photos of the rash over 2–3 days and bring them to a clinician visit.
What research says about menopause skin
Menopause is linked to reduced skin collagen and thickness, which contributes to dryness and fragility
American Academy of Dermatology guidance on atopic dermatitis care supports fragrance-free moisturizers and barrier repair as first-line
Endocrine Society guideline on hypothyroidism supports TSH and free T4 testing when symptoms suggest thyroid dysfunction