Dry Skin During Menopause: What’s Causing It and What Helps
Dry skin during menopause is often from lower estrogen, a weaker skin barrier, and thyroid shifts. Targeted blood tests available—no referral needed.
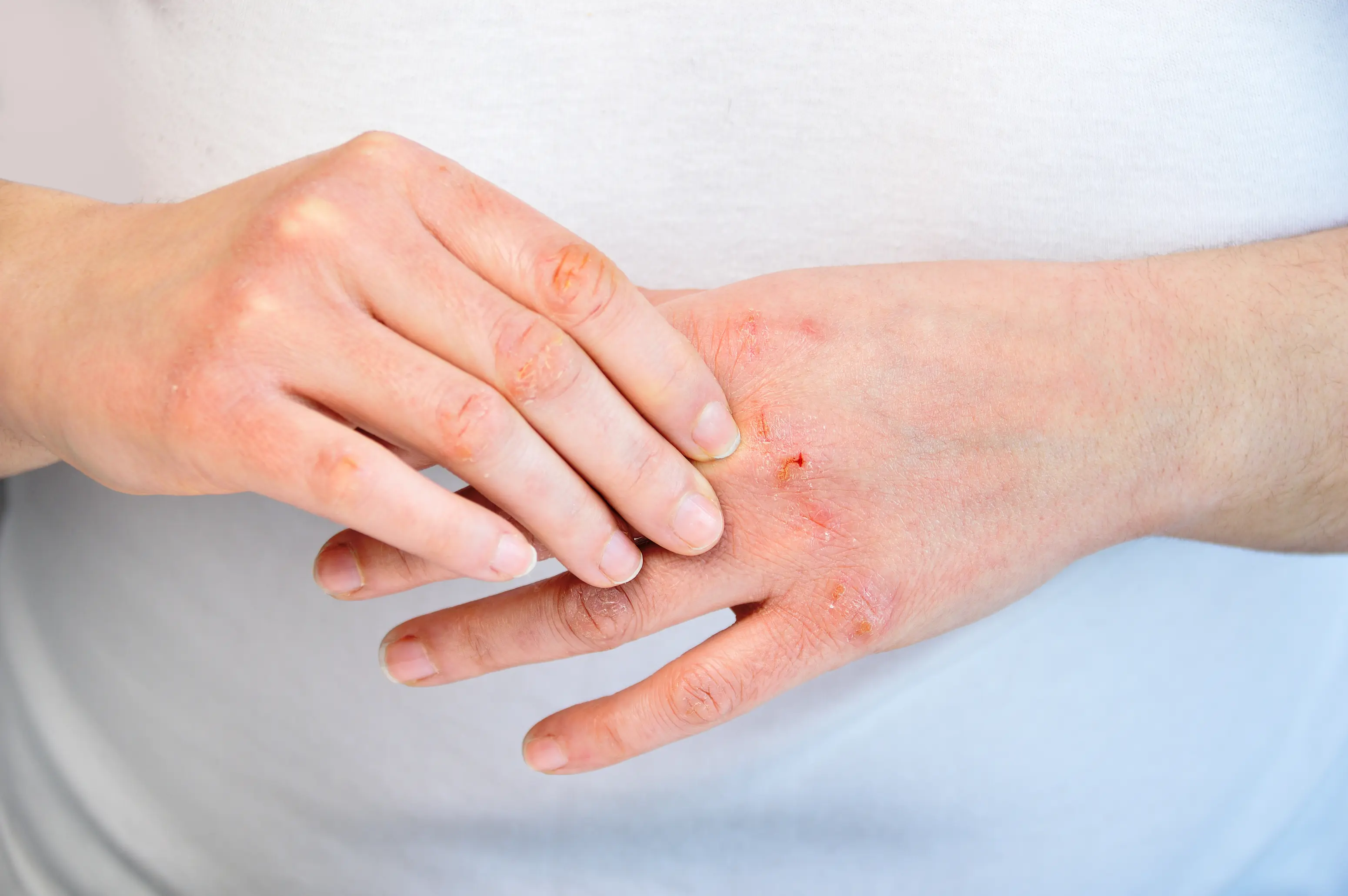
Dry skin during menopause usually happens because falling estrogen reduces your skin’s natural oils and water-holding ability, which weakens your barrier and makes irritation easier. It can also be worsened by thyroid slowdowns and by everyday “drying” exposures like hot showers, indoor heating, and harsh cleansers. A few targeted labs can help you tell whether this is mostly hormone-related skin change, a thyroid issue, or something else you can fix. This symptom is frustrating because you can do “everything right” with lotion and still feel tight, itchy, or flaky by lunchtime. Menopause changes how your skin behaves, not just how it looks, so the old routine often stops working. In the guide below, you’ll get the most common reasons dryness ramps up, what actually helps (including ingredient-level guidance), and which blood tests are worth considering. If you want help matching your pattern to the most likely cause, PocketMD can talk it through with you, and VitalsVault labs can help you confirm what’s going on.
Why your skin gets drier in menopause
Lower estrogen, less skin oil
As estrogen drops, your oil glands tend to make less sebum, which is the thin “natural moisturizer” that slows water loss. That’s why your skin can feel tight right after washing and why fine lines can suddenly look more obvious even if you’re drinking plenty of water. If your dryness started around cycle changes, hot flashes, or sleep shifts, it’s a clue that hormones are part of the story, so barrier-focused skincare usually works better than just switching to a thicker lotion.
A weaker skin barrier leaks water
Menopause can reduce the lipids and proteins that keep your outer skin layer sealed, so water escapes faster and irritants get in more easily. You might notice stinging when you apply products that never used to bother you, or patches that look “ashy” no matter how much you moisturize. The takeaway is that your goal is not only adding moisture, but also rebuilding the seal with ceramides and gentle cleansing so your moisturizer can actually stay put.
Thyroid slowdown (hypothyroidism)
An underactive thyroid slows skin cell turnover and reduces sweat and oil production, which can make your skin feel rough, thick, or persistently dry. This kind of dryness often comes with other changes, like feeling colder than everyone else, constipation, hair thinning, or puffy eyes. Because thyroid issues are common in midlife and treatable, it’s worth checking a thyroid-stimulating hormone test (TSH) if your dryness feels out of proportion or arrived with those other symptoms.
Eczema flares and new sensitivities
When your barrier is already fragile, you can tip into eczema (atopic dermatitis) more easily, even if you never had it as a kid. It often shows up as itchy patches in classic spots like the hands, eyelids, neck, or behind the knees, and scratching can start a loop that keeps the skin inflamed. If itch is a major feature, think “inflammation plus dryness,” which means you may need a short course of an anti-inflammatory plan (often a topical steroid or non-steroid prescription) in addition to daily barrier repair.
Dry air and hot water habits
Indoor heating, low humidity, and long hot showers pull water out of your skin faster than most creams can replace it. You feel it as that immediate post-shower tightness, plus flaking on shins, forearms, or around the mouth. A simple change like lowering shower temperature and adding a bedroom humidifier can make your moisturizer work twice as well, because you’re reducing the “leak” instead of only trying to refill the tank.
What actually helps dry menopausal skin
Moisturize like you’re sealing a leak
Apply a thick, fragrance-free moisturizer within three minutes of bathing, while your skin is still slightly damp, because that’s when you can trap the most water. Look for ceramides, glycerin, and petrolatum, since they rebuild barrier lipids and slow water loss rather than just feeling creamy. If your skin is very dry, using an ointment on top at night on the worst areas can be the difference between “better for an hour” and “better until morning.”
Switch to a gentle cleanser
Many foaming washes strip oils and leave you squeaky-clean, which is exactly the feeling you don’t want right now. A creamy, non-foaming cleanser or cleansing oil can remove sunscreen and makeup without wrecking your barrier, so you itch less and need less product to feel comfortable. If you’re not visibly dirty, it’s also okay to cleanse only the “sweaty zones” and rinse the rest with lukewarm water.
Use urea or lactic acid carefully
If you have rough, scaly areas on legs or arms, low-strength urea (around 10%) or lactic acid can soften the “glue” between dead skin cells so moisturizers penetrate better. The catch is that acids can sting on cracked or inflamed skin, especially around the face. Start every other night on a small area, and if you get burning that lasts more than a few minutes, pause and focus on barrier repair first.
Treat itch so you stop scratching
Itch is not just annoying; it keeps inflammation going and prevents healing. Cool compresses, a thicker ointment layer at night, and short nails help break the scratch cycle, and an over-the-counter 1% hydrocortisone can calm a small flare for a few days. If you’re getting widespread rash, oozing, or sleep-disrupting itch, that’s a good moment to ask for prescription options because you don’t have to “tough it out.”
Ask about hormone and thyroid options
If dryness is part of a bigger menopause picture, treating the transition itself can help some people, especially when symptoms cluster with hot flashes, sleep disruption, and vaginal dryness. Separately, if labs suggest thyroid slowdown, correcting it often improves skin texture over weeks to months because your skin turnover normalizes. The practical move is to bring a short symptom timeline to your clinician so you can discuss whether hormone therapy, thyroid treatment, or both make sense for you.
Useful biomarkers to discuss with your clinician
TSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreEstradiol
Estradiol in men is produced from testosterone via aromatase enzyme. In functional medicine, we recognize that men need optimal estradiol levels for bone health, cognitive function, and cardiovascular protection. However, excessive estradiol can suppress testosterone production and cause feminizing effects. The testosterone-to-estradiol ratio is crucial for male health, with optimal balance supporting vitality while preventing estrogen dominance. Balanced estradiol levels in men support bone health and cognitive…
Learn moreDhea Sulfate
DHEA-S levels reflect adrenal function and decline naturally with age. It's used to evaluate adrenal tumors, congenital adrenal hyperplasia, and androgen excess conditions like PCOS. Some consider it a marker of biological aging and stress resilience. DHEA-Sulfate (DHEA-S) is a hormone produced by the adrenal glands that serves as a precursor to sex hormones (testosterone and estrogen). It's the most abundant steroid hormone in the body.
Learn moreLab testing
Check thyroid and key nutrients linked to dry skin — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a two-week “skin log” once, not forever: note shower temperature, indoor humidity, and any new products, and rate itch and tightness from 1–10 each night. Patterns show up fast, and you’ll stop guessing.
Try the “soak and seal” method on your worst areas: dampen skin with lukewarm water for 30–60 seconds, pat until just not dripping, then apply a thick cream and a thin layer of ointment on top before bed.
If your face stings, simplify for seven days: one gentle cleanser at night, one bland moisturizer, and sunscreen in the morning. When the sting settles, add actives back one at a time so you can tell what’s irritating you.
Put a humidifier where you sleep and aim for about 40–50% humidity in winter. Your skin loses water overnight, so improving the air you breathe can noticeably reduce morning tightness.
If hand dryness is your main issue, treat it like a job hazard: use gloves for dishes and cleaning, keep a tube of thick cream by every sink, and apply after every wash so you’re not starting from zero each time.
Frequently Asked Questions
Does menopause really cause dry skin?
Yes. Falling estrogen can reduce skin oils and weaken the outer barrier, which makes water escape faster and irritation more likely. That’s why dryness can start even if you never had it before and even if you moisturize regularly. If it’s severe or comes with fatigue, hair loss, or feeling cold, consider checking TSH and free T4 to rule out thyroid slowdown.
Why is my skin so itchy at night during menopause?
At night your skin tends to lose more water, and scratching is easier when you’re tired and less distracted. If your barrier is compromised, even normal fabrics and heat under the covers can trigger itch. Try a thicker ointment layer before bed and keep the room cooler, and if itch is widespread or disrupting sleep, ask about eczema treatment rather than only switching moisturizers.
What ingredients are best for menopausal dry skin?
Ceramides help rebuild the “mortar” in your skin barrier, glycerin pulls water into the outer layer, and petrolatum slows water loss better than almost anything else. If you also have rough, scaly patches, low-strength urea (around 10%) can help, but it can sting if your skin is cracked. Choose fragrance-free products first, because fragrance is a common trigger when your skin is more reactive.
Can thyroid problems cause dry skin in midlife?
They can. Hypothyroidism often causes persistent dryness because skin turnover slows and you make less sweat and oil, and it may come with constipation, feeling cold, or puffy skin. A simple starting point is TSH, and pairing it with free T4 helps confirm whether the thyroid is truly underactive. If results are borderline, bring your symptom timeline to a clinician so the numbers are interpreted in context.
When should I worry about dry skin during menopause?
It’s worth getting checked if you have cracking that bleeds, signs of infection like increasing redness and warmth, or a new widespread rash. It’s also a good idea to investigate if dryness comes with unexplained weight change, severe fatigue, or significant hair loss, because thyroid and iron issues can overlap with menopause. Take photos of the worst areas and note what you’ve tried, because that makes your next visit much more productive.