Dry Skin After Menopause: What’s Going On and What Helps
Dry skin after menopause is often from lower estrogen, a weaker skin barrier, or thyroid changes. Targeted labs available at Quest—no referral needed.
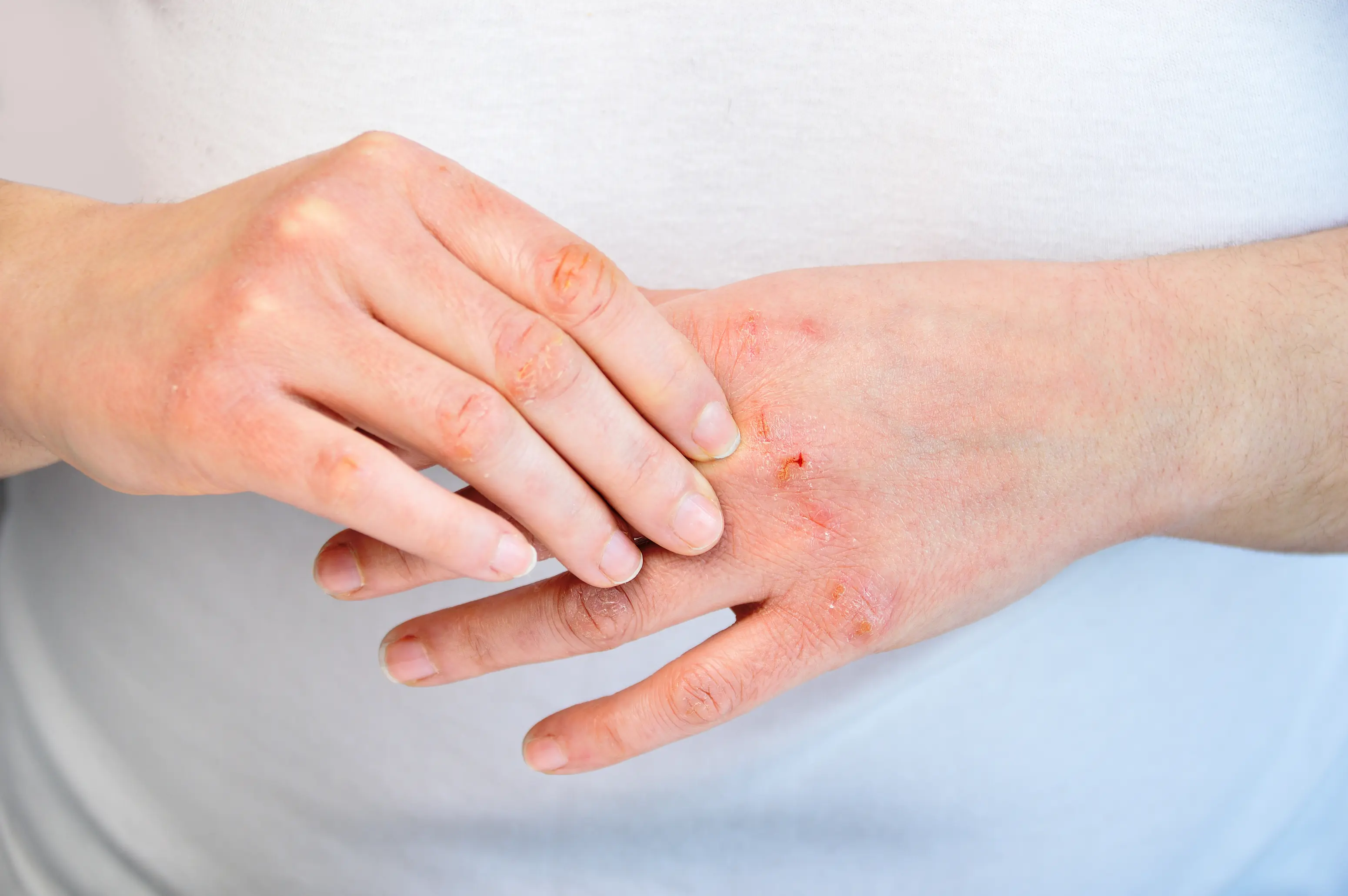
Dry skin after menopause is usually caused by lower estrogen, which slows oil production and weakens your skin’s moisture barrier, so water escapes faster. It can also be made worse by thyroid slow-down or by eczema flares that become easier to trigger as your skin thins and dries. A few targeted blood tests can help you sort out whether this is “just” barrier change or something treatable underneath. If you feel like you are doing everything right and your skin still looks dull, feels tight, or itches at night, you are not imagining it. After menopause, your skin changes from the inside out, and the same lotion that worked at 45 can suddenly feel useless at 55. This page walks you through the most common reasons, what actually helps (including ingredient-level guidance), and which labs can be worth checking. If you want help matching your pattern to the most likely cause, PocketMD can talk it through with you, and Vitals Vault labs can help confirm what your body is doing.
Why your skin gets drier after menopause
Lower estrogen weakens your barrier
After menopause, estrogen drops and your skin makes fewer of the fats and “mortar” that keep water sealed in. That means your skin loses moisture faster, so it can feel tight right after a shower and look crepey by afternoon. The most helpful takeaway is to treat this like a barrier problem, not just a “drink more water” problem, which means using a moisturizer that contains ceramides and glycerin and applying it while your skin is still slightly damp.
Less oil production on the surface
Your oil glands slow down with age and hormonal shifts, so your natural protective oil layer becomes thinner. You may notice more flaking on your shins, forearms, and around your mouth, especially in winter or in air conditioning. If your skin feels dry but not inflamed, adding a simple occlusive layer at night, like petrolatum or a dimethicone-based balm over your moisturizer, often makes a bigger difference than switching cleansers repeatedly.
Hot showers and harsh cleansers
Heat and strong surfactants strip away the lipids your skin is already struggling to replace, which can turn mild dryness into itching and cracking. It often shows up as that “squeaky clean” feeling after washing, followed by tightness and redness. Try a two-week experiment where you keep showers lukewarm, limit soap to sweaty areas, and use a fragrance-free cream cleanser, because your skin barrier can recover surprisingly fast when you stop re-injuring it.
Eczema flares become easier to trigger
Dry menopausal skin is more reactive, so you can tip into eczema (atopic dermatitis) even if you never had it before, or you can see old eczema return. This tends to itch more than it hurts, and scratching can create a cycle where the skin gets thicker, rougher, and even itchier. If you see patches that are red, scaly, or repeatedly cracking, it is worth treating the inflammation early with a clinician-guided plan rather than only layering more moisturizer.
Thyroid slow-down causing dryness
When your thyroid runs low (hypothyroidism), your skin turnover slows and sweat and oil production can drop, which makes dryness feel stubborn and “all over.” You might also notice fatigue, constipation, feeling cold, or thinning outer eyebrows, although some people have only subtle signs. The practical takeaway is that persistent dryness plus those body-wide clues is a good reason to check a thyroid test, because treating the thyroid problem can make your skin easier to manage.
What actually helps dry menopausal skin
Moisturize like a barrier repair plan
Look for a thick cream with ceramides, glycerin, and cholesterol, because those ingredients replace what your barrier is missing rather than just coating the surface. Put it on within three minutes of bathing, when your skin is still slightly damp, so you trap water in. If you only moisturize when you feel dry, you end up chasing the problem instead of preventing it.
Use a gentle cleanser, not foam
Foaming washes and “deep clean” body washes often remove too much oil, which makes postmenopausal dryness worse even if they feel refreshing. A fragrance-free cream cleanser or syndet bar (soap-free bar) cleans without leaving that tight, squeaky feeling. If your face stings after washing, that is a sign your cleanser is too aggressive for your current skin.
Add a nightly seal on rough areas
If your shins, hands, or elbows keep flaking, add an occlusive layer at night over your regular moisturizer. Petrolatum is the classic option, but dimethicone-based ointments work well if you hate the greasy feel. This is especially useful if you wake up with scratch marks, because reducing overnight water loss can cut itch significantly.
Try urea or lactic acid carefully
When dryness comes with rough texture, urea (around 5–10%) or lactic acid can soften the “glue” between dead skin cells so flakes lift off without aggressive scrubbing. You will feel the difference most on legs and feet, but these can sting on cracked or inflamed skin. Start every other night on a small area first, and if you have eczema patches, treat the inflammation before you add exfoliating acids.
Ask about hormone or eczema treatment
If your dryness started around menopause and is affecting quality of life, a clinician can discuss whether hormone therapy is appropriate for you, because estrogen influences skin thickness and hydration. If the main problem is itchy, inflamed patches, a short course of a prescription anti-inflammatory cream can break the itch-scratch cycle faster than any over-the-counter product. Bring photos and a short timeline to the visit, because pattern and onset matter as much as how dry it feels today.
Useful biomarkers to discuss with your clinician
Estradiol
Estradiol in men is produced from testosterone via aromatase enzyme. In functional medicine, we recognize that men need optimal estradiol levels for bone health, cognitive function, and cardiovascular protection. However, excessive estradiol can suppress testosterone production and cause feminizing effects. The testosterone-to-estradiol ratio is crucial for male health, with optimal balance supporting vitality while preventing estrogen dominance. Balanced estradiol levels in men support bone health and cognitive…
Learn moreTSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreDhea Sulfate
DHEA-S levels reflect adrenal function and decline naturally with age. It's used to evaluate adrenal tumors, congenital adrenal hyperplasia, and androgen excess conditions like PCOS. Some consider it a marker of biological aging and stress resilience. DHEA-Sulfate (DHEA-S) is a hormone produced by the adrenal glands that serves as a precursor to sex hormones (testosterone and estrogen). It's the most abundant steroid hormone in the body.
Learn moreLab testing
Check TSH, free T4, ferritin, and vitamin D at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a “three-minute rule” for two weeks: after every shower or hand-wash, pat dry and apply a ceramide-based cream within three minutes, because that is when you can trap the most water in your skin.
If itching wakes you up, keep a small tube of petrolatum by your bed and reapply to the itchiest spots before you scratch; reducing overnight water loss often lowers the itch signal by morning.
Switch your hand soap first if your hands are the worst area. A fragrance-free, non-foaming cleanser plus a thick cream after every wash can outperform expensive face products.
Run a humidifier in your bedroom when indoor heat is on, and aim for about 40–50% humidity. If you wake up with a tight face and dry throat, your air is probably drying your skin all night.
Stop exfoliating for ten days if your skin stings with products. When your barrier is irritated, even “gentle” acids can feel like fire, and a short reset often makes your routine work again.
Frequently Asked Questions
Can menopause really cause dry, itchy skin?
Yes. After menopause, lower estrogen reduces skin oils and weakens the moisture barrier, so your skin loses water faster and becomes more reactive, which often feels like itch. If you also see red, scaly patches, you might be dealing with eczema on top of simple dryness. A barrier-focused routine for two weeks is a good first test, and if itch persists, ask about eczema treatment.
Why is my skin so dry even when I moisturize?
If your moisturizer is mostly a light lotion, it may not replace barrier lipids or seal water in long enough to matter after menopause. Hot showers, foaming cleansers, and low indoor humidity can also undo your moisturizing within hours. Try a ceramide-and-glycerin cream applied on damp skin, then add an occlusive layer at night on the worst areas.
What vitamin deficiency causes dry skin after menopause?
Low iron stores (checked with ferritin) and low vitamin D can be associated with poorer skin and hair resilience, although they are not the only causes of dryness. Ferritin below about 30 ng/mL is a common threshold where hair and nails can suffer even if your blood count looks normal. If you suspect a deficiency, test first and then supplement based on results rather than guessing.
Could dry skin after menopause be a thyroid problem?
It can be. Hypothyroidism can cause generalized, stubborn dryness because skin turnover slows and oil and sweat production drop, and it often comes with fatigue, constipation, or feeling cold. Checking TSH and free T4 can help confirm whether your thyroid is contributing, and treating an underactive thyroid can make topical skin care work better.
When should I see a doctor for dry skin after menopause?
Go sooner if you have cracks that bleed, signs of infection like warmth and pus, or a rash that is spreading or very painful. Make an appointment if dryness and itching persist beyond about 4–6 weeks despite a barrier-focused routine, or if you have other symptoms such as fatigue, weight change, or hair loss that suggest a thyroid or iron issue. Bringing photos and a list of products you use helps your clinician pinpoint irritants quickly.