Why Is Your Hair Thinning in Perimenopause?
Hair thinning in perimenopause often comes from estrogen shifts, thyroid changes, or low iron stores. Targeted labs can clarify it—no referral needed.
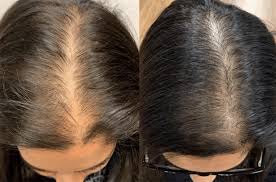
Hair thinning in perimenopause is usually a mix of shifting estrogen and progesterone, a relative rise in the effect of androgens (the “more male-leaning” hormones), and common “silent” issues like low iron stores or thyroid changes. The pattern matters: gradual widening of your part points to female-pattern thinning, while sudden shedding after stress, illness, or stopping hormones points to a shedding phase. Simple blood tests can help you figure out which driver is most likely in your case, so you are not guessing. This is one of those symptoms that feels personal because it shows up in the mirror every day, and it can hit your confidence hard. The tricky part is that perimenopause can unmask more than one cause at the same time, so you might have both a hormonal pattern and a correctable deficiency. Below, you will learn the most common reasons hair thins during this transition, what tends to help (and what is mostly hype), and which labs are worth prioritizing. If you want help matching your pattern to the most likely cause, PocketMD can talk it through with you, and Vitals Vault labs can help you confirm what your body is doing.
Why does your hair thin in perimenopause?
Female-pattern thinning gets unmasked
As estrogen support fluctuates, hair follicles that were already genetically sensitive can start producing finer, shorter hairs, especially along your part and crown. This is female-pattern hair loss [androgenetic alopecia], and it tends to be gradual rather than sudden. A useful clue is that you see more scalp through your hair, but you may not see huge clumps in the shower. If this sounds like you, think “miniaturization,” which means treatments that protect follicles early tend to work better than waiting.
A shedding phase after stress
Perimenopause often overlaps with stress, illness, weight changes, surgery, or stopping birth control, and any of those can push more hairs into a resting phase so they shed 2–3 months later. This is called a shedding episode (telogen effluvium), and it can feel dramatic because your ponytail suddenly looks thinner. The good news is that follicles are usually still healthy, which means shedding often improves over 3–6 months once the trigger is addressed. Your takeaway is to look back 8–12 weeks for a “body stressor,” not just what happened last week.
Low iron stores, even mild
You can have “normal” hemoglobin and still have low iron reserves, which your hair follicles notice because hair growth is energy-intensive. Heavy or irregular perimenopause bleeding can quietly drain iron over time, and the first sign can be more shedding and slower regrowth. Ferritin is the storage marker, and many hair specialists aim for ferritin around 50–70 ng/mL for hair support, even if the lab’s lower limit is much lower. If your periods have changed and your hair is thinning, iron stores are one of the highest-yield things to check.
Thyroid shifts change hair cycling
When your thyroid is underactive (hypothyroidism), your hair can become dry, brittle, and more likely to shed, and your eyebrows can thin at the outer edge. Thyroid issues become more common with age, and symptoms like fatigue, constipation, or feeling cold can blend into “perimenopause,” which is why it gets missed. A TSH test helps screen for this, but the “so what” is that treating thyroid imbalance can improve shedding and texture over months. If hair thinning comes with new sluggishness, it is worth testing rather than assuming it is only hormones.
Scalp inflammation or irritation
If your scalp is itchy, flaky, tender, or burning, inflammation can interfere with healthy growth and make shedding worse. Sometimes it is dandruff (seborrheic dermatitis), sometimes it is psoriasis, and sometimes it is irritation from new products or tight styles that pull on the roots. This matters because you can do everything “right” with supplements and still lose ground if your scalp is inflamed. A practical next step is to treat the scalp like skin: simplify products for two weeks and consider an anti-dandruff shampoo with ketoconazole or zinc pyrithione if flaking is part of the picture.
What actually helps with hair thinning in perimenopause
Use topical minoxidil consistently
Topical minoxidil is one of the best-studied options for female-pattern thinning because it helps follicles stay in the growth phase longer. It is common to see a temporary increase in shedding in the first 4–8 weeks, which is scary but often means older hairs are making room for new growth. Most people need 3–6 months to see early improvement and closer to 9–12 months for a clearer change. If you try it, pick a routine you can actually stick with, because stopping usually means losing the gains over time.
Correct low ferritin on purpose
If ferritin is low, treating it is not about “more supplements,” it is about a plan that you can tolerate and that actually raises stores. Many people do better with iron every other day, taken away from calcium and coffee, because absorption can be higher and stomach upset can be lower. You should also ask why iron is low, because ongoing heavy bleeding can keep draining you even if you supplement. Recheck ferritin after about 8–12 weeks so you know whether you are moving toward that hair-supportive range.
Address thyroid imbalance if present
If your TSH suggests hypothyroidism, treating the thyroid can reduce shedding and improve texture, but it is not instant because hair cycles are slow. The practical way to think about it is that you are stabilizing the “background setting” your follicles live in. If you start thyroid medication, ask your clinician when to recheck TSH, because dose tweaks are common early on. While you wait, focus on gentle hair care so you are not adding breakage on top of shedding.
Talk about hormone therapy thoughtfully
Hormone therapy can help some perimenopause symptoms, and for some people it indirectly helps hair by improving sleep, reducing stress physiology, and smoothing hormone swings. It is not a guaranteed hair-loss treatment, and certain progestins or androgenic effects can make hair worse in a subset of people. The key is personalization: your symptoms, your family history, and your risk factors matter. If hair thinning started soon after a hormone change, bring that timing to the conversation because it is often the biggest clue.
Treat the scalp like skin
If your scalp is inflamed, you will get better results when you calm it down first, because follicles do not thrive in irritated skin. For flaking and itch, a medicated shampoo used a few times per week can make a noticeable difference within a month, especially if you leave it on for several minutes before rinsing. If you have painful bumps, patchy loss, or thick scale, you may need prescription treatment, and that is worth it because scarring types of hair loss can become permanent. Take a few clear photos in good light so you can track whether the scalp is improving.
Useful biomarkers to discuss with your clinician
Ferritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreTSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreEstradiol
Estradiol in men is produced from testosterone via aromatase enzyme. In functional medicine, we recognize that men need optimal estradiol levels for bone health, cognitive function, and cardiovascular protection. However, excessive estradiol can suppress testosterone production and cause feminizing effects. The testosterone-to-estradiol ratio is crucial for male health, with optimal balance supporting vitality while preventing estrogen dominance. Balanced estradiol levels in men support bone health and cognitive…
Learn moreLab testing
Get ferritin, TSH, and vitamin D checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “pattern check” once a month: take a top-of-head photo in the same lighting and part your hair in the same place. Gradual widening of the part suggests female-pattern thinning, while a sudden overall drop in volume suggests a shedding episode.
Try the 60-second shed count for one week: on wash days, count the hairs you shed in the shower and while detangling, and write the number down. A trend matters more than a single scary day, and it helps you see whether a change is actually working.
If you start minoxidil, set a 6-month expectation up front and put it next to something you already do daily, like brushing your teeth. Consistency beats intensity with hair treatments, because follicles respond to steady signals over time.
If your periods are heavier or closer together, treat that as a hair clue, not just an inconvenience. That bleeding pattern is one of the most common ways ferritin drops in perimenopause, so it is worth checking ferritin before you spend money on hair supplements.
Protect what you have while you work on the cause: avoid tight ponytails, keep heat styling to a minimum, and use a wide-tooth comb on wet hair. Less breakage makes thinning look less dramatic and gives regrowth time to catch up.
Frequently Asked Questions
Is hair thinning a normal part of perimenopause?
It is common, but “common” does not mean you have to ignore it. Perimenopause hormone swings can unmask female-pattern thinning and can also trigger a temporary shedding phase after stress or stopping hormones. Because low ferritin and thyroid changes can mimic “hormonal hair loss,” checking ferritin and TSH is often a smart first step.
How can you tell telogen effluvium from female pattern hair loss?
Telogen effluvium usually shows up as sudden, diffuse shedding that starts about 2–3 months after a trigger, and your part may look similar while your overall volume drops. Female-pattern hair loss is more gradual and tends to widen your part or thin the crown as hairs miniaturize. If you are unsure, bring photos and a timeline to a clinician, because the treatments and expectations are different.
What ferritin level is best for hair growth?
Many hair-focused clinicians aim for ferritin around 50–70 ng/mL or higher to support regrowth, even if the lab’s “normal” range starts much lower. If your ferritin is below that, you might shed more and regrow more slowly, especially if you also have heavy periods. Ask for a ferritin test and recheck after 8–12 weeks of treatment to confirm it is rising.
Can thyroid problems cause hair thinning in perimenopause?
Yes, and it is easy to miss because symptoms like fatigue, weight changes, and sleep issues overlap with perimenopause. An underactive thyroid often causes diffuse thinning, dry texture, and slower regrowth, and TSH is the usual screening test. If your TSH is abnormal, treating the thyroid can improve hair over months, so it is worth testing rather than guessing.
How long does it take for hair to grow back after perimenopause shedding?
If it is a shedding episode, the trigger usually happens first, then shedding peaks about 2–3 months later, and improvement often starts within 3–6 months once the trigger is fixed. Visible regrowth takes longer because hair grows slowly, so a clearer “before and after” often takes 6–12 months. Track progress with monthly photos and consider checking ferritin and TSH if shedding is persistent.