Swelling in Women: Common Causes, Red Flags, and Lab Tests
Swelling in women often comes from fluid retention, vein valve problems, or low blood protein. Targeted labs available at Quest—no referral needed.
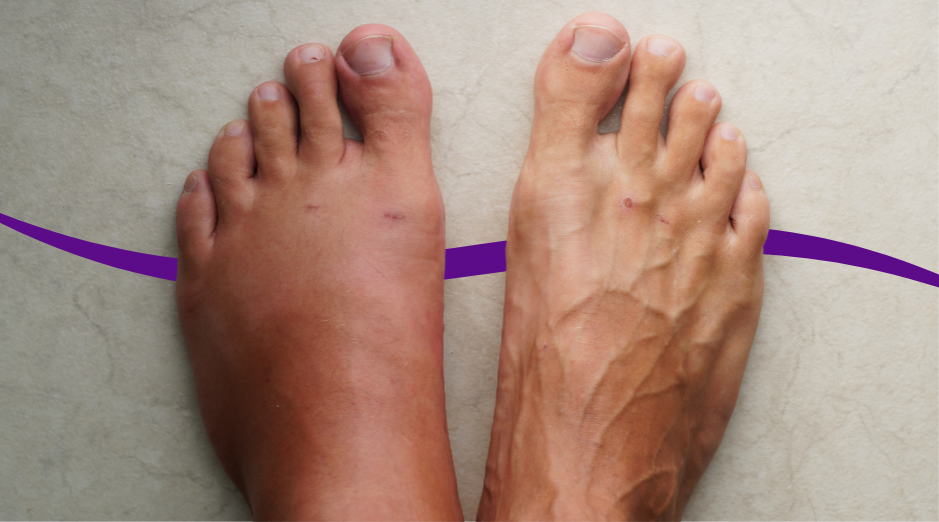
Swelling in women is usually your body holding onto extra fluid or fluid shifting into tissues, and the most common reasons are hormone-related water retention, vein circulation problems in the legs, or a “low protein” state from kidney or liver issues. It can also happen from certain medications, an injury, or heart strain, which is why the pattern and location matter. A few targeted blood tests can help sort out whether this is mainly salt-and-water retention, low albumin, or an organ-related issue. Swelling can be annoying in a very practical way because your shoes feel tight, your rings won’t come off, and your face or ankles look puffy in photos. It can also be scary because you start wondering about your heart or kidneys. Most swelling is not an emergency, but sudden one-sided leg swelling, swelling with shortness of breath, or swelling that comes with chest pain deserves urgent care. In the rest of this page, you’ll learn the most common causes, what tends to help in real life, and which labs can make the “why is this happening?” part less of a guessing game. If you want help matching your exact pattern to the most likely cause, PocketMD can walk through your symptoms with you, and Vitals Vault labs can help you confirm what your body is doing.
Why you’re getting swelling
Hormone shifts and water retention
Estrogen and progesterone changes can make your kidneys hold onto more salt and water, which pulls fluid into your tissues and shows up as puffy fingers, a bloated face, or heavier-feeling legs. This is why swelling often flares in the week before your period, during perimenopause, or with some birth control methods. If your swelling follows your cycle and improves after your period starts, tracking it for two cycles can help you confirm the pattern and avoid unnecessary panic.
Leg veins not pushing blood back
When the valves in your leg veins get leaky, blood pools lower down and fluid seeps into the surrounding tissue, especially around your ankles by the end of the day. You might notice it’s worse after standing or sitting for long stretches and better in the morning after your legs have been flat overnight. A simple clue is whether swelling improves within 30–60 minutes of elevating your legs above heart level, which points toward a circulation problem rather than a whole-body fluid issue.
Kidneys leaking protein into urine
Your blood proteins act like tiny sponges that keep fluid inside your blood vessels, and when your kidneys let protein spill into urine, that “pull” weakens and swelling becomes easier. This often shows up as puffiness around your eyes in the morning or swelling that doesn’t change much with standing. If you also notice foamy urine or your swelling is new and persistent, it’s worth checking kidney markers and urine protein sooner rather than later.
Low blood protein (albumin) state
If your albumin is low, fluid escapes from blood vessels into tissues more easily, which can cause swelling in the legs and sometimes the belly. Low albumin can happen from liver disease, poor protein intake during illness, or protein loss through the gut, and it matters because treating the swelling alone won’t fix the underlying leak. If you have swelling plus easy bruising, yellowing of the eyes, or a very poor appetite, ask for labs that include albumin and liver-related tests.
Medication side effects
Some medicines widen blood vessels or change kidney salt handling, which can make fluid collect in your feet and lower legs even if your heart and kidneys are otherwise okay. Common culprits include certain blood pressure meds like amlodipine, anti-inflammatory pain relievers like ibuprofen, and hormones like estrogen. If swelling started within weeks of a new medication or dose change, do not stop it abruptly on your own, but do ask your prescriber about alternatives or dose adjustments.
What actually helps swelling (and when to get checked)
Use elevation like a quick test
Try a structured “elevation trial” once a day for three days: lie down and prop your legs so your ankles are above your heart for 30 minutes. If the swelling noticeably softens and your shoes fit better afterward, that strongly suggests gravity and vein flow are major drivers. That information is useful because it points you toward compression, movement breaks, and vein evaluation rather than chasing random supplements.
Compression that you’ll actually wear
Graduated compression socks help push fluid back up from your ankles, but the key is getting the right strength and timing. Put them on in the morning before swelling builds, and start with a comfortable 15–20 mmHg level if you’re new to them. If you feel numbness, severe pain, or your toes turn pale or blue, stop and get fitted, because that can mean the compression is too tight or you have an artery issue.
A 7-day sodium reset
If your swelling is mostly fluid retention, sodium is often the volume knob. For one week, keep meals simple and mostly home-prepared, and aim for under about 2,000 mg of sodium per day by avoiding packaged soups, deli meats, and salty snacks. If your swelling drops and your rings fit again, you’ve learned something important about your personal sensitivity, and you can keep the benefit by targeting your highest-sodium foods rather than trying to be perfect.
Move your calf muscles on purpose
Your calf muscles act like a pump for your leg veins, and when they’re quiet for hours, fluid has an easier time settling in your ankles. Set a timer for every 45–60 minutes and do two minutes of brisk walking, stair climbing, or 20 slow calf raises while holding onto a counter. This is especially helpful if you work at a desk, travel, or notice swelling that peaks late afternoon.
Get urgent help for specific patterns
Swelling is not always benign, and a few patterns should move you from “watch and wait” to “get seen now.” Go urgently if you have sudden one-sided leg swelling with pain or warmth, swelling with new shortness of breath, or swelling plus chest pain or fainting. Those combinations can signal a blood clot or heart strain, and waiting it out is not worth the risk.
Useful biomarkers to discuss with your clinician
Albumin
Albumin is the most abundant protein in blood plasma, produced exclusively by the liver. In functional medicine, albumin serves as a marker of liver synthetic function, nutritional status, and overall health. Albumin maintains oncotic pressure (keeping fluid in blood vessels), transports hormones and nutrients, and serves as an antioxidant. Low albumin may indicate liver disease, malnutrition, chronic inflammation, or kidney disease. Since albumin has a half-life of about 20 days, it reflects longer-term nutriti…
Learn moreSodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreProtein, Total
Total protein levels reflect nutritional status, liver function (protein synthesis), and kidney function (protein retention). Abnormal levels can indicate liver disease, kidney disease, malnutrition, inflammation, or blood cancers. It provides a general overview of protein metabolism. Total protein measures the combined amount of albumin and globulins in blood. These proteins are essential for maintaining fluid balance, transporting substances, fighting infections, and blood clotting.
Learn moreLab testing
Get kidney function, albumin, and thyroid checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “finger test” once a day: press your thumb into your shin for 5 seconds. If a dent stays for more than a few seconds, that pitting swelling is more consistent with fluid buildup than with simple weight gain.
If your swelling is worst at the end of the day, take a photo of your ankles in the morning and again at night for one week. The comparison is surprisingly helpful when you talk to a clinician, and it also shows whether your changes are actually working.
When you travel or sit for long periods, treat your calves like a pump you have to turn on. Every hour, do 20 slow calf raises and then walk for two minutes, because that combination moves fluid better than fidgeting in your seat.
If you suspect cycle-related swelling, track it against day-of-cycle and sleep for two months. Many people find their swelling spikes after poor sleep or higher-carb restaurant meals in the premenstrual week, which gives you a clear target instead of vague “hormones.”
If you wear compression socks, put them on before you get out the door, not after swelling starts. Once fluid is already in the tissues, compression still helps, but it works best as prevention.
Frequently Asked Questions
Why are my ankles swollen but only at night?
Nighttime ankle swelling usually means gravity is winning during the day, which is common with standing, sitting, heat, or leg vein valve issues. If it’s much better in the morning and worse after long days, try a 30-minute leg elevation test and consider morning compression socks. If one ankle suddenly swells more than the other or it’s painful and warm, get checked urgently.
Is swelling before my period normal?
Yes, mild swelling before your period is common because hormone shifts can make your kidneys retain more salt and water. It often shows up as tighter rings, a puffy face, or heavier legs and improves after bleeding starts. If it is new, severe, or paired with shortness of breath or high blood pressure, it’s worth getting a basic workup rather than assuming it’s “just PMS.”
How do I know if swelling is from my kidneys?
Kidney-related swelling often comes with puffiness around the eyes in the morning, swelling that doesn’t change much with standing, and sometimes foamy urine. Two useful tests are a CMP for creatinine/eGFR and a urine albumin-to-creatinine ratio (uACR), because protein leakage can drive swelling even early on. If your uACR is persistently above 30 mg/g or your eGFR trends below about 60, schedule follow-up promptly.
What medications commonly cause swelling in women?
A common cause is certain blood pressure medicines like amlodipine, which can lead to ankle swelling by widening small blood vessels. Anti-inflammatory pain relievers like ibuprofen can also cause fluid retention in some people, and estrogen-containing hormones can worsen water retention. If swelling started after a new medication or dose change, ask your prescriber about alternatives instead of stopping suddenly.
When is swelling an emergency?
Treat it as urgent if you have sudden one-sided leg swelling with pain or warmth, because that can be a blood clot. Also go in urgently if swelling comes with new shortness of breath, chest pain, fainting, or coughing up pink froth, because that can signal heart or lung strain. If you’re unsure, err on the side of being seen, especially when the change is sudden.