Swelling in Men: What It Means and What Helps
Swelling in men often comes from fluid retention, vein problems, or low blood protein from kidney/liver issues. Targeted labs available—no referral needed.
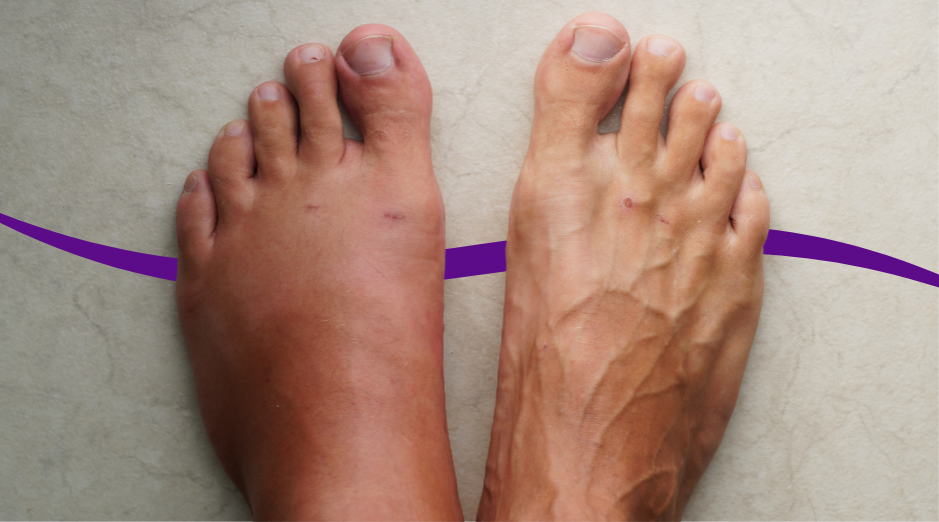
Swelling in men is usually your body holding onto extra fluid or fluid leaking into tissues, and the most common reasons are salt and medication-related water retention, vein circulation problems in the legs, or low blood protein from kidney or liver issues. Sometimes it is also a sign your heart is struggling to move blood forward, which pushes fluid into your ankles and feet. A few targeted blood tests can help sort out which pattern fits you. Swelling can look simple, but it is one of those symptoms where the location and timing matter a lot. One swollen calf after a long flight is a different problem than both ankles puffing up every evening, and facial puffiness in the morning points you in yet another direction. If you have sudden one-sided leg swelling with pain or warmth, new shortness of breath, chest pain, or you cannot lie flat without getting winded, treat that as urgent and get checked right away. If you are trying to make sense of a slower-burn situation, PocketMD can help you think through your pattern, and Vitals Vault labs can help you confirm whether your kidneys, liver, or protein levels are part of the story.
Why swelling happens in men (and what it usually means)
Leg vein pooling (venous insufficiency)
If the valves in your leg veins get leaky, blood tends to pool in your lower legs when you sit or stand, and that pressure pushes fluid into the surrounding tissue. You usually notice ankle or calf swelling that is worse at the end of the day and improves overnight. The practical clue is timing: if elevation helps within an hour and the swelling is fairly symmetrical, veins are often the main driver.
Salt, alcohol, or medication fluid retention
Your kidneys balance salt and water, so when you eat very salty food, drink more alcohol than usual, or start certain meds, your body may temporarily hold onto extra fluid. Common culprits include blood pressure medicines like amlodipine, anti-inflammatories like ibuprofen, and steroid pills, and the swelling can show up in your ankles or hands within days. If your swelling started soon after a medication change, ask your clinician or pharmacist whether that drug is known to cause edema and whether an alternative is reasonable.
Kidney leakiness causing low protein
Your blood protein, especially albumin, helps keep fluid inside your blood vessels, and your kidneys are supposed to keep that protein in your bloodstream. When the kidney filters get damaged, protein can spill into urine, your blood albumin drops, and fluid shifts into tissues, which can cause puffy eyelids in the morning and swelling in the legs later. A simple urine protein check plus blood albumin and creatinine often clarifies whether this is the direction you need to investigate.
Heart not pumping strongly enough
When your heart cannot move blood forward efficiently, pressure backs up in the veins and your kidneys interpret that as “low circulation,” so they retain salt and water. You tend to see swelling in both ankles, weight gain over days, and sometimes shortness of breath when you climb stairs or lie flat. If swelling is new for you and you also feel unusually winded, do not just “wait it out,” because early treatment can prevent a bigger flare.
A blocked vein clot (deep vein thrombosis)
A clot in a deep leg vein (deep vein thrombosis) blocks blood return, so fluid builds up quickly below the blockage and the leg can feel tight, heavy, or painful. This is usually one-sided, and the calf may be warmer or more tender than the other side, especially after travel, surgery, injury, or long periods of immobility. Because a clot can travel to the lungs, sudden one-leg swelling with pain is a “same day” evaluation problem, not a home-treatment problem.
What actually helps with swelling (based on the cause)
Use elevation the right way
If your swelling is from vein pooling, “feet on an ottoman” often is not enough because your ankles are still below your heart. Try lying down and propping your legs so your heels are above heart level for 20–30 minutes, once or twice daily, and see whether your ankle size changes measurably. If that reliably helps, it is a strong hint that circulation and gravity are major players.
Try compression, but size matters
Graduated compression socks help push fluid back toward your core, but only if they fit correctly and you can tolerate them. For mild daily ankle swelling, many men do well starting with 15–20 mmHg and moving up only if needed, and you should put them on in the morning before swelling builds. If you have severe pain, numbness, or your feet look pale or cold in compression, stop and get advice because that can signal an artery circulation issue.
Do a 7-day sodium experiment
If your swelling fluctuates with food, a short, structured trial is more informative than vague “eat less salt” advice. For one week, avoid obvious high-sodium foods like restaurant meals, deli meats, and salty snacks, and aim for roughly 1,500–2,000 mg sodium per day while tracking morning weight and ankle swelling. When swelling improves within a few days, you have a lever you can keep using even while you work on the deeper cause.
Review meds that commonly cause edema
Some medications cause swelling by widening small blood vessels, which lets fluid seep into tissues even when your heart and kidneys are fine. Calcium channel blockers, NSAIDs, testosterone or anabolic steroid use, and some diabetes drugs are frequent examples in real life. Bring a full list, including supplements, and ask a specific question: “Could any of these be causing my swelling, and what is the safest swap or dose change?”
Get evaluated for organ-related swelling
When swelling is persistent, spreading upward, or paired with fatigue, foamy urine, belly swelling, or shortness of breath, you are past the point of guessing. Blood tests, urine testing, and sometimes an ultrasound or heart evaluation can identify kidney disease, liver disease, or heart failure early, when treatment works better. If you are unsure how urgent your pattern is, use a symptom summary (including photos and daily weights) to make the visit more efficient.
Useful biomarkers to discuss with your clinician
Albumin
Albumin is the most abundant protein in blood plasma, produced exclusively by the liver. In functional medicine, albumin serves as a marker of liver synthetic function, nutritional status, and overall health. Albumin maintains oncotic pressure (keeping fluid in blood vessels), transports hormones and nutrients, and serves as an antioxidant. Low albumin may indicate liver disease, malnutrition, chronic inflammation, or kidney disease. Since albumin has a half-life of about 20 days, it reflects longer-term nutriti…
Learn moreCreatinine
Creatinine is a waste product of muscle metabolism that is filtered by the kidneys and serves as the primary marker of kidney function. In functional medicine, creatinine levels reflect not only kidney health but also muscle mass and protein metabolism. Elevated creatinine indicates reduced kidney filtration capacity, while very low levels may indicate muscle wasting or poor protein intake. Creatinine is used to calculate eGFR and helps assess long-term kidney health and detoxification capacity. Creatinine measu…
Learn moreSodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreLab testing
Get kidney function, albumin, and BNP checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “pitting” check once a day for a week: press your thumb into the swollen ankle for 5 seconds. If a dent stays for more than a few seconds, it is true fluid swelling, which is more useful information than how it looks in the mirror.
Measure, do not guess. Wrap a soft tape measure around your ankle at the same spot each evening, and write down the number along with your morning weight; a 2–3 lb (1–1.5 kg) jump over 48 hours often means fluid, not fat.
If the swelling is mostly in your legs, take two short walking breaks during long sitting days and do 20 slow calf raises each time. Your calf muscles act like a pump, and using them regularly can noticeably reduce end-of-day tightness.
If you wear compression socks, put them on before you get out of bed or right after a shower in the morning. Waiting until noon often feels like “they do nothing,” because the fluid is already in the tissue by then.
Take a phone photo of both ankles at the same time each day (same lighting, same distance). It sounds silly, but it helps you and your clinician see trends and makes it easier to notice when swelling is becoming one-sided.
Frequently Asked Questions
When is swelling in one leg an emergency?
Treat sudden one-sided leg swelling as urgent if it comes with pain, warmth, redness, or a tight calf, especially after travel, surgery, or being laid up. That pattern can be a deep vein clot (deep vein thrombosis), which can become dangerous if it moves to the lungs. If you also have chest pain or new shortness of breath, go to emergency care now.
Why are my ankles swollen at night but fine in the morning?
That day-to-night pattern often points to gravity and vein pooling, where fluid collects in your lower legs while you are upright and then redistributes when you lie down. It can also happen with salt-heavy days or medications that cause ankle edema, such as amlodipine. Try a week of consistent leg elevation and a sodium experiment, and bring your notes to your clinician if it persists.
Can testosterone cause swelling in men?
Yes. Testosterone therapy and anabolic steroids can cause water retention, and they can also raise red blood cell levels, which changes circulation and can make you feel puffy or tight in your extremities. If swelling started after starting or increasing testosterone, ask for a medication review and consider checking kidney function and a heart strain marker like BNP if you are also getting breathless.
What blood tests are best for unexplained swelling?
A practical starting trio is a comprehensive metabolic panel (kidney and liver function plus electrolytes), serum albumin (your main “fluid-holding” protein), and BNP or NT-proBNP (a heart strain marker). Abnormal albumin points you toward kidney protein loss or liver issues, while a high BNP pushes you toward a heart-focused evaluation. If your swelling is new or worsening, do not rely on labs alone—pair them with an exam and, when needed, imaging.
How do I tell if swelling is fat gain or fluid retention?
Fluid changes faster than fat, so a 2–5 lb (1–2.5 kg) weight jump over a couple of days with tighter shoes or sock marks strongly suggests fluid. Pitting swelling, where a thumb press leaves a dent, also supports fluid rather than fat. Track morning weight for a week and note whether elevation or compression changes the swelling within hours, because fat will not respond that quickly.
Research and guidelines worth knowing about
2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure (includes edema evaluation and BNP use)
KDIGO 2024 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease (protein loss and edema workup)
CHEST guideline on antithrombotic therapy for venous thromboembolism (DVT diagnosis and treatment principles)