Swelling During Your Period: What It Means and What Helps
Swelling during period is usually from hormone-driven fluid retention, higher salt sensitivity, or low iron. Targeted labs available—no referral needed.
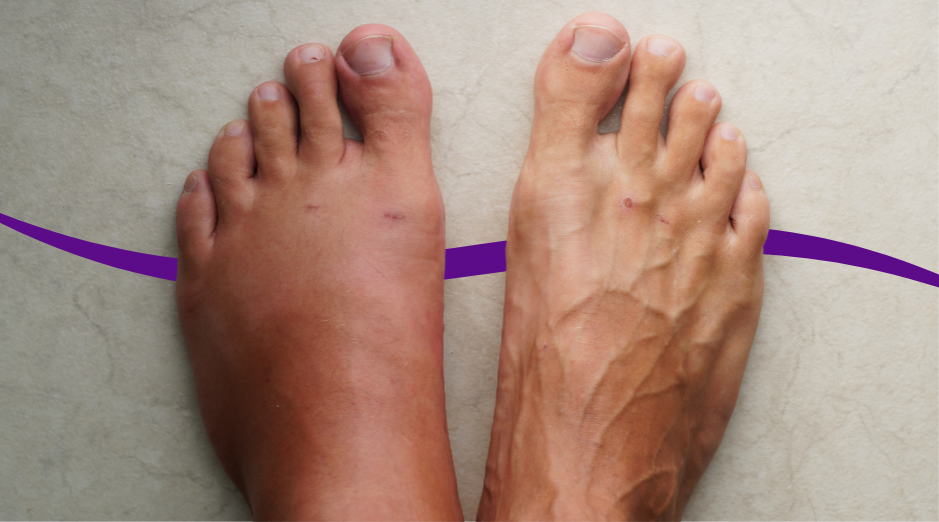
Swelling during your period is most often your hormones shifting your fluid balance, which makes you hold onto water and feel puffy in your face, hands, belly, or ankles. It can also be amplified by salt sensitivity and inflammation, and sometimes by low iron from heavy bleeding, which can make swelling feel worse because you are already tired and run down. If it is new, one-sided, severe, or you are also short of breath, labs and a quick medical check can help separate normal cycle-related water retention from kidney, thyroid, or heart problems. A little “period puffiness” is common, but it is still annoying when your rings feel tight, your shoes suddenly do not fit, or your legs look different in photos. The tricky part is that the same word—swelling—can describe harmless water retention and also true edema, which is fluid leaking into tissues. This guide helps you figure out which pattern you have, what you can try this cycle, and which blood tests are most useful. If you want help matching your exact symptoms to the right next step, PocketMD can walk you through it, and Vitals Vault labs can help you check the most relevant markers without a referral.
Why swelling happens around your period
Hormone-driven water retention
In the days before bleeding starts, progesterone and estrogen shift quickly, and your kidneys respond by holding onto more sodium and water. That extra fluid shows up as tight rings, a puffy face in the morning, or a “heavy” feeling in your legs by evening. The giveaway is timing: it tends to peak right before your period and improves within the first couple days of bleeding.
Higher salt sensitivity pre-period
Some cycles, your body reacts to the same salty meal like it is a much bigger deal, so you retain water more easily. You might notice swelling after takeout, deli foods, or restaurant meals even if you normally tolerate them fine. A practical experiment is to keep sodium steadier for three days before your expected period and see if your swelling curve changes.
Inflammation and “period aches”
The chemicals that trigger cramps and uterine shedding (prostaglandins) can also increase inflammation and make tissues feel puffy and sore. This is why swelling can come with joint stiffness, breast tenderness, or a bloated, stretched feeling in your lower belly. If your swelling is paired with pain, treating the inflammation early—rather than waiting until you feel awful—often makes a noticeable difference.
Low iron from heavy bleeding
If your periods are heavy, you can slowly run low on iron, which can leave you fatigued, short of breath with stairs, and more sensitive to normal body changes. Low iron does not directly “cause” water retention, but it can make swelling feel more dramatic because your body is under-resourced and you are less active, which lets fluid pool in your legs. If you soak through pads or tampons, pass large clots, or feel wiped out for days, it is worth checking a CBC and ferritin.
A non-period cause showing up
Sometimes swelling that you notice during your period is actually from something else that just became obvious at the same time, like an underactive thyroid, kidney strain, or a medication side effect. Red flags are swelling that is new after age 35, swelling that is much worse on one side, or swelling that comes with chest pain or shortness of breath. If any of those fit, do not wait for the next cycle to see what happens—get checked promptly.
What actually helps period swelling
Start earlier than you think
Swelling is easier to prevent than to “undo,” so begin your plan two to three days before you expect symptoms. That might mean keeping sodium consistent, going for a short walk after dinner, and prioritizing sleep so your stress hormones do not push you toward more fluid retention. If you only start once you are already puffy, you are playing catch-up.
Use movement to move fluid
When you walk, your calf muscles act like a pump that pushes fluid back toward your heart, which is why ankles often look better after a few short bouts of movement. Aim for three 10-minute walks spread through the day, especially if you sit for work. If your feet swell most, elevating your legs for 15 minutes after the last walk can help the effect “stick.”
Try magnesium glycinate at night
Magnesium can help with PMS symptoms for some people, and it may indirectly reduce swelling by improving sleep and easing cramps so you move more. Magnesium glycinate is often better tolerated than magnesium oxide, which can cause diarrhea. A common starting approach is 200–300 mg at night for the week before your period, and you stop if it upsets your stomach or makes you too sleepy.
Anti-inflammatory timing for cramps
If cramps and body aches are part of your swelling pattern, taking an anti-inflammatory medicine at the first sign of symptoms can reduce prostaglandin-driven inflammation. This is most effective when you take it with food and follow the label directions, because “more” is not safer. If you have kidney disease, ulcers, are on blood thinners, or you are pregnant, ask a clinician before using NSAIDs.
Compression for ankle and leg swelling
If your swelling is mostly in your lower legs, knee-high compression socks can reduce that heavy, stretched feeling by preventing fluid from pooling. They work best when you put them on in the morning before swelling builds. If compression makes your legs hurt, or you have numbness or skin color changes, stop and get checked.
Useful biomarkers to discuss with your clinician
Iron, Total
Serum iron measures the amount of iron circulating in your blood at the time of testing. In functional medicine, we recognize that serum iron alone provides limited information about iron status, as it fluctuates throughout the day and is affected by recent iron intake, inflammation, and diurnal variation. However, when combined with other iron studies, it helps assess iron metabolism and transport. Iron is essential for oxygen transport, energy production, DNA synthesis, and immune function. Optimal serum iron…
Learn moreFerritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreHs Crp
High-sensitivity C-reactive protein (hs-CRP) is a key marker of systemic inflammation and cardiovascular risk. In functional medicine, we recognize hs-CRP as one of the most important predictors of heart disease, stroke, and metabolic dysfunction. Levels above 1.0 mg/L indicate increased inflammation that may be driven by poor diet, chronic infections, autoimmune conditions, or metabolic syndrome. Optimal levels below 0.5 mg/L are associated with the lowest cardiovascular risk and overall inflammatory burden. hs…
Learn moreLab testing
Get CBC, TSH, and creatinine/eGFR checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a two-cycle “map” of your swelling by taking a quick morning photo of your hands and ankles and rating tightness from 0–10; patterns show up fast when you compare day -3 to day +2.
If your shoes get tight by evening, try a 10-minute walk after lunch and another after dinner for three days before your period; that calf-muscle pump often beats a single long workout.
Run a simple sodium experiment: keep restaurant food out for 72 hours before your period and cook one or two familiar meals at home; if swelling drops, you have a clear lever to pull next month.
If swelling is mostly in your belly, measure comfort instead of weight by using the same waistband or belt notch each morning; it is a more honest signal of fluid shifts than the scale.
If you suspect heavy bleeding is driving fatigue, track how often you change pads or tampons on your heaviest day; bringing that number to a visit makes it much easier to decide whether to check CBC and iron.
Frequently Asked Questions
Is swelling during your period normal?
Mild, symmetric puffiness that peaks right before your period and improves within a day or two of bleeding is usually normal hormone-related water retention. It becomes less “normal” when it is new for you, lasts most of the month, or is mainly in one leg or one hand. If you are unsure, checking TSH, a CBC, and kidney function (creatinine/eGFR) can help rule out common non-cycle causes.
Why are my hands and fingers swollen on my period?
Hormone shifts can make your kidneys hold onto sodium and water, and your hands show it quickly because the tissues are small and tight. You often notice it as rings that suddenly feel stuck or knuckles that look less defined. Try reducing salty restaurant foods for two to three days before your period and see if your ring tightness improves next cycle.
When should I worry about swelling during my period?
Get checked urgently if swelling comes with shortness of breath, chest pain, coughing up pink froth, or if one leg becomes suddenly more swollen, red, warm, and painful. Those patterns can signal heart or lung strain or a blood clot, and they are not explained by PMS. If the swelling is persistent but not urgent, ask about kidney function (creatinine/eGFR) and thyroid testing (TSH).
Can anemia from heavy periods cause swelling?
Anemia from heavy periods usually causes fatigue, dizziness, and shortness of breath more than true fluid retention, but it can make swelling feel worse because you move less and fluid pools in your legs. A CBC can show anemia, and ferritin is often the next test to confirm low iron stores. If you are soaking through protection every 1–2 hours or passing large clots, do not self-treat—get evaluated.
What’s the fastest way to reduce period swelling in your legs and feet?
The fastest non-medication combo is short, frequent walking to activate your calf pump, plus leg elevation afterward to let fluid drain. Compression socks work best if you put them on in the morning before swelling builds. If leg swelling is new, one-sided, or keeps getting worse each cycle, consider checking creatinine/eGFR and talking with a clinician.