Hair Thinning After Pregnancy: What It Means and What Helps
Hair thinning postpartum is usually from hormone drop, low iron stores, or thyroid shifts. See what’s normal, what to test, and get labs at Quest—no referral.
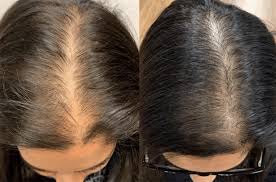
Hair thinning postpartum is most often a temporary shedding phase caused by the sudden drop in pregnancy hormones, which pushes more hairs into the “resting” stage and then out. It can also be worsened by low iron stores after delivery and by thyroid swings in the first year postpartum. A few targeted blood tests can help you figure out which of these is actually driving your shedding. If you’re seeing handfuls of hair in the shower or a widening part, it can feel alarming, especially when you’re already exhausted. The good news is that most postpartum shedding is reversible, but the timeline is slow and the “normal” range is wide. This page walks you through what’s happening in your scalp, what patterns suggest something more than typical postpartum shedding, and what you can do now. If you want help matching your symptoms to the most likely cause, PocketMD can talk it through with you, and Vitals Vault labs can help you check iron and thyroid function without a referral.
Why your hair thins after pregnancy
Hormone drop triggers extra shedding
During pregnancy, higher estrogen keeps more hairs in the growth phase, so your hair can feel thicker. After delivery, estrogen falls quickly, and many follicles shift into a resting phase and then shed a few months later, which is why the timing often surprises you. The takeaway is that shedding that starts around 2–4 months postpartum and peaks around 4–6 months is very often this temporary pattern, even if it looks dramatic.
Low iron stores after delivery
Even if your hemoglobin looks “fine,” your iron storage tank can be low, especially if you had heavy bleeding, a C-section, or close pregnancies. When iron stores are low, your body prioritizes essentials over hair growth, so regrowth can stall and shedding can feel relentless. If your shedding is paired with feeling unusually wiped out or getting short of breath on stairs, checking ferritin is a practical next step.
Postpartum thyroid swings
In the first year after birth, some people develop inflammation of the thyroid (postpartum thyroiditis), which can swing from “too fast” to “too slow.” Either direction can affect hair cycling, and the slow phase in particular can make hair feel dry, brittle, and thinner at the temples. If you also notice palpitations, heat intolerance, new anxiety, constipation, or feeling cold all the time, thyroid labs can help separate normal postpartum changes from a treatable thyroid issue.
Stress, sleep loss, and illness
Your scalp responds to big body stressors, and postpartum life is full of them: sleep fragmentation, infections, surgery recovery, and sometimes rapid weight changes. These stress signals can push more follicles into the resting phase, which means the shedding shows up later, not right when the stress happens. The useful move here is to look back 8–12 weeks for triggers like a fever, mastitis, COVID, or a major sleep collapse, because it helps you predict when shedding might ease.
Pattern hair loss unmasked postpartum
Some people already have a genetic tendency toward gradual thinning (female pattern hair loss), but pregnancy can temporarily “mask” it by holding hairs in the growth phase. After birth, when shedding happens, you may notice a wider part or thinner crown that doesn’t fully rebound. If thinning is most obvious on the top of your scalp rather than diffuse shedding everywhere, it’s worth discussing targeted treatments early, because this type responds best when you start before years pass.
What actually helps postpartum shedding
Set a realistic regrowth timeline
For typical postpartum shedding, the peak is often around months 4–6, and many people see clear improvement by 9–12 months postpartum. Regrowth can look like short “baby hairs” along your hairline, but it can take months for those hairs to add noticeable volume. If you’re past 12 months with no slowdown, or the thinning is getting steadily worse, that’s a strong signal to test iron and thyroid and consider other causes.
Treat low ferritin, not just anemia
If ferritin is low, your goal is to rebuild iron stores so follicles can stay in the growth phase. Many clinicians aim for ferritin at least around 50 ng/mL for hair concerns, and some people feel best closer to 70–100 ng/mL, even if the lab’s “normal” range starts much lower. Ask your clinician about an iron plan that fits breastfeeding and your stomach, and recheck ferritin in about 8–12 weeks to make sure it is actually rising.
Address thyroid issues promptly
If your thyroid labs show you’re hypothyroid, treating it can reduce shedding and improve energy, mood, and constipation, which often matter just as much as hair. Postpartum thyroiditis sometimes resolves on its own, but you still deserve monitoring because the low-thyroid phase can be rough and can persist. A practical approach is to repeat TSH and free T4 every 6–8 weeks while symptoms are active, so you’re not guessing based on how tired you feel.
Use gentle hair handling that protects density
When shedding is high, your hair breaks more easily, and breakage makes thinning look worse even if follicles are recovering. Switching to low-tension styles, using a wide-tooth comb when wet, and avoiding tight ponytails can preserve what you have while your cycle normalizes. If you want a simple rule, anything that causes scalp soreness by the end of the day is too much tension right now.
Consider minoxidil if thinning persists
If you’re past the typical postpartum window or your pattern looks like widening part and crown thinning, topical minoxidil can help keep follicles in the growth phase and support regrowth. It is not an instant fix, and it can cause a temporary shed in the first 2–8 weeks, which is scary but often expected. Because pregnancy and breastfeeding considerations are personal, it’s worth a quick clinician check-in before you start, especially if you’re nursing.
Useful biomarkers to discuss with your clinician
Ferritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreTSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreEstradiol
Estradiol in men is produced from testosterone via aromatase enzyme. In functional medicine, we recognize that men need optimal estradiol levels for bone health, cognitive function, and cardiovascular protection. However, excessive estradiol can suppress testosterone production and cause feminizing effects. The testosterone-to-estradiol ratio is crucial for male health, with optimal balance supporting vitality while preventing estrogen dominance. Balanced estradiol levels in men support bone health and cognitive…
Learn moreLab testing
Check ferritin, TSH, and free T4 at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Take three photos today in the same lighting: front hairline, center part, and crown. Repeat every 4 weeks, because your day-to-day shedding is noisy but photos show the trend.
If you want a quick “is this still postpartum?” check, look at timing: shedding that starts around month 3 and eases by month 9 is typical, but shedding that starts at 10–12 months postpartum deserves a ferritin and thyroid check.
When you wash your hair, use your fingertips on the scalp and let the suds run through the ends instead of scrubbing them. It sounds small, but it reduces breakage that can make thinning look worse.
If you start iron, pair it with vitamin C and keep it away from calcium by a couple of hours, because absorption matters more than the brand. Rechecking ferritin is how you know it’s working.
If your eyebrows are thinning at the outer edges or your hair feels drier and coarser than usual, put thyroid symptoms on your list even if you think you’re “just tired.” Those details help a clinician interpret TSH and free T4 correctly.
Frequently Asked Questions
When does postpartum hair loss start and stop?
Postpartum shedding often starts around 2–4 months after delivery, peaks around 4–6 months, and gradually improves by 9–12 months. You may still see short regrowth hairs for a while because hair grows slowly, about 1 cm per month. If shedding is still heavy after 12 months, consider checking ferritin and thyroid labs to look for a fixable driver.
Is postpartum hair loss normal if I’m breastfeeding?
Yes, it can be normal while breastfeeding because the main trigger is the postpartum hormone shift, not whether you nurse. Breastfeeding can indirectly affect shedding if it contributes to sleep loss or if your iron stores are low and not being rebuilt. If you feel unusually fatigued or lightheaded along with shedding, ferritin is a useful test to add.
How can I tell postpartum shedding from female pattern hair loss?
Postpartum shedding is usually diffuse, meaning you notice hair everywhere and more hair in the drain, but the overall pattern often recovers over months. Female pattern hair loss more often shows a widening part or thinning at the crown that does not bounce back fully. If your part keeps widening past 9–12 months postpartum, ask about evaluation and early treatment options.
What ferritin level is too low for hair growth?
Many people with hair shedding have ferritin below 30 ng/mL, and that level can be low enough to affect hair even if your hemoglobin is normal. For hair recovery, clinicians commonly aim for ferritin at least around 50 ng/mL, with some targeting 70–100 ng/mL depending on symptoms and tolerance. If you supplement, recheck ferritin in about 8–12 weeks so you’re not guessing.
Can postpartum thyroiditis cause hair loss, and what should I test?
Yes, postpartum thyroiditis can cause hair thinning because thyroid hormone shifts change how long hairs stay in the growth phase. Testing TSH and free T4 together is a practical starting point, especially if you also have palpitations, anxiety, constipation, feeling cold, or mood changes. If results are abnormal, repeating labs every 6–8 weeks helps track the swing and guide treatment.