Hair Thinning in Women: What It Usually Means and What to Do
Hair thinning in women often comes from low iron, thyroid imbalance, or hormone-related pattern loss. Targeted labs available at Quest—no referral needed.
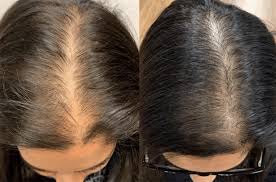
Hair thinning in women is usually caused by one of three things: a shedding shift after stress or hormones (telogen effluvium), a gradual genetic-and-hormone pattern (female pattern hair loss), or a correctable body signal like low iron or a thyroid imbalance. The fastest way to stop guessing is to match your pattern of loss with a few targeted labs, because the right fix depends on the trigger. Hair changes hit hard because they are visible and personal, and because the internet makes it sound like there is one magic shampoo you are missing. In real life, hair follicles respond slowly, so even the “right” treatment takes months to show up in the mirror. This page helps you figure out what type of thinning you likely have, what you can do today, and which blood tests are most useful. If you want help sorting your story into the most likely bucket, PocketMD can talk it through with you, and Vitals Vault labs can help confirm what your body is signaling.
Why your hair is thinning (and what that pattern means)
Female pattern hair loss
This is the slow, widening-part kind of thinning where your ponytail gradually feels smaller, even though you are not seeing dramatic clumps in the shower. Your follicles become more sensitive to normal hormone signals over time, so each hair grows in a shorter, finer cycle. If your part is widening at the crown and your hairline is mostly preserved, think “pattern” and plan for long-term treatment rather than a quick reset.
Stress or illness shedding shift
After a big stressor, your body can push more hairs into the resting phase at once, which means you shed more 2–3 months later even if the stressful event is already over. This is called stress shedding (telogen effluvium), and it often feels like handfuls of hair with washing or brushing. The key takeaway is timing: look back 8–12 weeks for triggers like high fever, surgery, a crash diet, or a major emotional hit.
Postpartum hormone drop
During pregnancy, higher estrogen keeps more hairs in the growth phase, so your hair can look thicker. After delivery, estrogen falls quickly, and those “extra” hairs shed together, usually peaking around 3–4 months postpartum. It is scary, but it is often temporary, so focus on gentle hair care and making sure iron stores and thyroid function are solid while your body recalibrates.
Low iron stores (low ferritin)
Ferritin is your stored iron, and hair follicles are surprisingly sensitive to low reserves even when your hemoglobin is still “normal.” When ferritin is low, your body prioritizes oxygen delivery and basic survival over hair growth, so your strands can become finer and shedding can ramp up. If you have heavy periods, follow a vegetarian diet, or feel unusually tired, ferritin is one of the most practical tests to check early.
Thyroid imbalance
Your thyroid hormone sets the pace for many tissues, including hair follicles, so both an underactive and overactive thyroid can cause diffuse thinning. You might also notice dry skin, constipation, anxiety, heat or cold intolerance, or changes in your cycle, which helps connect the dots. If hair thinning comes with those whole-body clues, a simple TSH test is often the quickest way to rule in or rule out a thyroid driver.
What actually helps hair thinning (without guessing)
Treat the pattern you actually have
If your thinning is gradual with a widening part, you usually need a long-game plan because the follicles are slowly miniaturizing. If it is sudden shedding after a trigger, the goal is to remove the trigger and give your follicles time to re-enter growth. Take two clear photos today in the same lighting and part, then repeat monthly, because your eyes will lie to you day to day.
Topical minoxidil, used consistently
Minoxidil helps keep follicles in the growth phase longer, which can thicken the look of hair over time, especially in female pattern hair loss. The frustrating part is that you may shed a bit more in the first 4–8 weeks as older hairs cycle out, and then improvement usually shows up around 3–6 months. If you try it, commit to daily use and track progress with monthly photos rather than week-to-week mirror checks.
Rebuild iron stores if ferritin is low
If ferritin is low, hair often will not fully rebound until your stored iron is repleted, even if you are eating “enough” iron on paper. Work with a clinician on the dose and form, because side effects like constipation are common and can derail you, and you may need to treat heavy bleeding at the same time. A practical target many dermatologists use for hair is ferritin above about 50 ng/mL, not just barely within the lab range.
Address thyroid issues, not just symptoms
If your TSH suggests hypothyroidism or hyperthyroidism, treating the thyroid problem is what gives your follicles a stable environment again. Hair regrowth is slow, so you typically judge response over months, not weeks, and you may notice baby hairs at the hairline before overall density changes. Ask for a plan to recheck TSH after any medication change so you are not stuck in the “almost treated” zone.
Be gentle with traction and heat
Tight ponytails, braids, extensions, and frequent high-heat styling can add mechanical stress to follicles that are already struggling, which makes thinning look worse and can cause breakage that mimics shedding. Switching to looser styles and lowering heat does not fix hormonal or iron-driven loss, but it removes a preventable multiplier. If your temples are thinning and you wear tight styles often, this change can pay off faster than most supplements.
Useful biomarkers to discuss with your clinician
Ferritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreTSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreEstradiol
Estradiol in men is produced from testosterone via aromatase enzyme. In functional medicine, we recognize that men need optimal estradiol levels for bone health, cognitive function, and cardiovascular protection. However, excessive estradiol can suppress testosterone production and cause feminizing effects. The testosterone-to-estradiol ratio is crucial for male health, with optimal balance supporting vitality while preventing estrogen dominance. Balanced estradiol levels in men support bone health and cognitive…
Learn moreLab testing
Check ferritin, TSH, and vitamin D at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “part check” once a month: take a photo of your middle part and crown in the same bathroom lighting, from the same distance. Hair changes are slow, and this stops you from spiraling based on one bad hair day.
If you are shedding a lot, run your fingers through dry hair for 60 seconds over a light towel and count roughly how many hairs come out. Repeat twice a week for two weeks, because trends matter more than a single count.
If you recently stopped hormonal birth control, started a new medication, or had a big diet change, write down the date. Hair shedding commonly shows up 8–12 weeks later, so that timeline clue can be more useful than any supplement label.
If you suspect low iron, pair iron-rich meals with vitamin C (like citrus or bell pepper) and avoid taking iron with coffee, tea, or calcium, because absorption drops. Small changes here can make your lab numbers move faster.
If your scalp is itchy, greasy, or flaky along with thinning, treat the scalp like skin, not just hair. Using an anti-dandruff shampoo consistently for a few weeks can reduce inflammation that makes shedding feel worse.
Frequently Asked Questions
Is hair thinning in women usually hormonal?
Sometimes, but not always. Gradual thinning with a widening part often fits female pattern hair loss, which is influenced by hormone sensitivity, while sudden shedding often follows stress, illness, postpartum changes, or low ferritin. If you are unsure, checking ferritin and TSH can quickly reveal two common, fixable drivers.
What ferritin level is too low for hair growth?
Many dermatology practices see more shedding when ferritin is below about 30 ng/mL, and regrowth is often harder when it stays below about 50 ng/mL. The lab “normal” range can be misleading because it is designed for anemia screening, not hair optimization. If your ferritin is low, ask about a repletion plan and a repeat test in 8–12 weeks.
How long does it take for hair to grow back after shedding?
Even when the trigger is gone, follicles need time to re-enter the growth phase, so you usually see improvement in shedding first and visible density later. A common timeline is 3–6 months to notice meaningful change, and up to 9–12 months for fuller recovery. Taking monthly photos is the simplest way to see progress that mirrors hide.
Does postpartum hair loss mean something is wrong?
Postpartum shedding is often a normal response to the hormone drop after pregnancy, and it typically peaks around 3–4 months after delivery. It is still worth checking ferritin and TSH if the shedding is severe, lasts beyond about 6–9 months, or comes with fatigue, palpitations, or heat/cold intolerance. If you are worried, bring the timeline to a clinician so you are not dismissed as “just postpartum.”
When should you see a doctor for hair thinning?
Get checked sooner if you have sudden patchy bald spots, scalp pain or sores, or rapid shedding that started after a new medication, because those patterns can need specific treatment. Also book a visit if thinning comes with heavy periods, new facial hair or acne, or thyroid-type symptoms, since labs like ferritin and TSH can change the plan. Bring photos and a 2–3 month timeline of major stressors, illnesses, and cycle changes to make the visit more productive.