Why Is Your Skin So Dry After Having a Baby?
Dry skin postpartum is often from hormone shifts, frequent handwashing, or thyroid changes. Targeted blood tests are available at Quest—no referral needed.
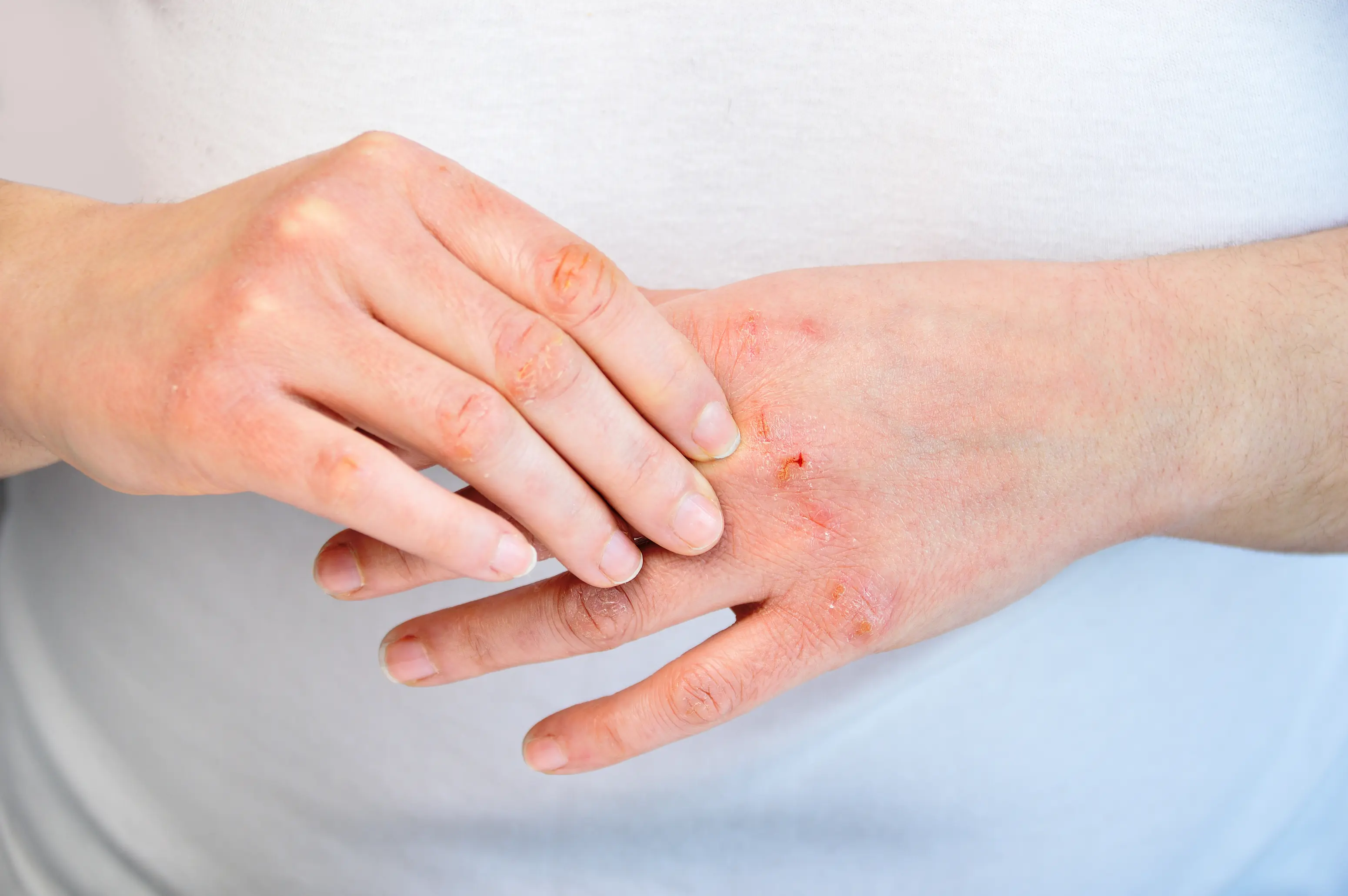
Dry skin after having a baby is usually a mix of hormone shifts, a stressed skin barrier from frequent washing, and sometimes an underactive thyroid that shows up in the months after delivery. When your barrier is leaky, water escapes faster, which is why your skin can feel tight, flaky, and itchy even when you moisturize. A few targeted labs can help you tell the difference between “new-mom skin stress” and a treatable internal cause. Postpartum life is rough on skin in very practical ways: more handwashing, more hot showers, less sleep, and often less time to apply products correctly. At the same time, your hormones are changing quickly, and that can change oil production and how reactive your skin feels. If you’re not sure what’s driving your dryness, PocketMD can help you sort through your pattern and symptoms, and Vitals Vault labs can help confirm whether thyroid or iron issues are part of the story.
Why your skin gets so dry postpartum
Hormone drop lowers skin oils
After delivery, estrogen and progesterone fall quickly, and that can reduce the natural oils that keep your skin flexible. The “so what” is that your skin can suddenly feel papery or tight, especially on your face, shins, and hands, even if you never had dry skin before. If your dryness started within the first few weeks postpartum and you also notice more sensitivity to products, think “oil and barrier shift” first and focus on barrier repair rather than stronger exfoliants.
Overwashing and sanitizer damage
Newborn care often means constant handwashing, dishwashing, and alcohol-based sanitizer, which strip the lipids that seal water into your outer skin layer. That is why your hands can crack at the knuckles or sting when you apply lotion. The quickest win is changing the routine: use lukewarm water, a fragrance-free cleanser, and apply a thick ointment within one minute of drying your hands.
Postpartum thyroid slowdown
Some women develop thyroid inflammation after pregnancy, and it can swing from “fast” to “slow” thyroid over a few months. When your thyroid is underactive, your skin turns over more slowly and makes less oil, so dryness comes with fatigue, constipation, feeling cold, or hair shedding. If your dryness is getting worse around 2–6 months postpartum, a TSH and free T4 blood test can be a very practical next step.
Eczema flare (atopic dermatitis)
Postpartum stress, sleep loss, and barrier disruption can flare eczema, even if it was mild before. This dryness usually itches more than it flakes, and it tends to show up in patches that get red, rough, or thickened from scratching. If you see that pattern, treat it like inflammation plus dryness: consistent moisturizer is necessary, but you may also need a short course of an anti-inflammatory cream from your clinician.
Low iron stores dry you out
Blood loss from delivery and months of pregnancy can leave your iron stores low, even if your hemoglobin looks “okay.” Low iron does not directly dry your skin the way cold weather does, but it can worsen fatigue and slow tissue repair, which makes cracked, irritated skin harder to bounce back from. If you also have brittle nails, more shedding hair, or shortness of breath with stairs, checking ferritin can help you decide whether iron repletion should be part of your plan.
What actually helps postpartum dry skin
Do the one-minute moisturize rule
Moisturizer works best when it traps water that is already in your skin, which is why timing matters more than brand. After a shower or handwashing, pat dry and apply a thick cream or ointment within one minute, while your skin is still slightly damp. If you only have time for one step, do this one consistently for a week and watch how much the tightness improves.
Switch to barrier-building ingredients
Look for products that replace what your barrier is missing, like ceramides, glycerin, and petrolatum, because they reduce water loss instead of just making you feel temporarily slick. If you are itchy or rough, urea at low strength can soften scale without the sting that acids sometimes cause on postpartum-sensitive skin. Patch test new products on a small area for two nights, since your skin may react differently right now.
Make hand care realistic
If your hands are the worst area, keep a tube of fragrance-free cream at every sink and a small ointment by your bed. Put ointment on at night and wear cotton gloves for 20–30 minutes, which gives your skin time to re-seal without smearing everything on the sheets. During the day, choose nitrile gloves for wet chores, because “just one quick wash” is often what keeps cracks from healing.
Treat eczema flares early
When dryness is driven by eczema, waiting it out usually backfires because scratching keeps the inflammation going. A short, targeted anti-inflammatory plan can break the cycle, and then moisturizer keeps it from returning as quickly. If you have widespread redness, oozing, or honey-colored crusting, get checked promptly because skin infections can piggyback on eczema and need different treatment.
Fix the internal driver if present
If labs show hypothyroidism or low iron stores, topical care alone often feels like pushing a boulder uphill. Thyroid treatment can gradually improve dryness over weeks, and iron repletion can support skin and hair recovery over a few months, especially when ferritin is low. Bring your results and symptoms to a clinician so your plan matches your postpartum stage and whether you are breastfeeding.
Useful biomarkers to discuss with your clinician
TSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreEstradiol
Estradiol in men is produced from testosterone via aromatase enzyme. In functional medicine, we recognize that men need optimal estradiol levels for bone health, cognitive function, and cardiovascular protection. However, excessive estradiol can suppress testosterone production and cause feminizing effects. The testosterone-to-estradiol ratio is crucial for male health, with optimal balance supporting vitality while preventing estrogen dominance. Balanced estradiol levels in men support bone health and cognitive…
Learn moreDhea Sulfate
DHEA-S levels reflect adrenal function and decline naturally with age. It's used to evaluate adrenal tumors, congenital adrenal hyperplasia, and androgen excess conditions like PCOS. Some consider it a marker of biological aging and stress resilience. DHEA-Sulfate (DHEA-S) is a hormone produced by the adrenal glands that serves as a precursor to sex hormones (testosterone and estrogen). It's the most abundant steroid hormone in the body.
Learn moreLab testing
Check TSH, free T4, ferritin, and vitamin D at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
If your hands are cracking, try “cream after every wash, ointment at night.” The cream makes daytime life workable, and the ointment does the heavy repair while you sleep.
Use lukewarm showers and keep them short for two weeks as an experiment. Hot water feels good in the moment, but it strips oils and can make the post-shower itch much worse.
If lotion stings, that is a clue your barrier is irritated, not that you need a stronger product. Switch to a bland ointment (like petrolatum) for 72 hours, then reintroduce a ceramide cream once the sting calms down.
For flaky legs, apply a urea-based cream at night and put on soft leggings or pajama pants. The fabric reduces evaporation and helps the ingredient work without needing a thick greasy layer.
Take two phone photos of the worst area in the same lighting, one today and one in seven days. Dry skin changes slowly, and seeing the difference keeps you from product-hopping before anything has a chance to work.
Frequently Asked Questions
How long does postpartum dry skin last?
For many women, the worst dryness improves over several weeks as hormones stabilize and your routine becomes less wash-heavy. If it is still worsening after 2–3 months, or it is paired with fatigue, constipation, and feeling cold, it is worth checking thyroid labs like TSH and free T4. In the meantime, the fastest improvement usually comes from consistent barrier repair, not stronger exfoliation.
Can breastfeeding make your skin drier?
Breastfeeding can keep estrogen relatively low, and lower estrogen can mean less natural skin oil and more sensitivity. That does not mean you have to stop breastfeeding, but it does mean your skin may need richer moisturizers and gentler cleansing for a while. If dryness is severe or you also have postpartum mood changes and extreme fatigue, ask your clinician whether thyroid testing makes sense.
Is postpartum dry skin a sign of thyroid problems?
It can be, especially when dryness shows up with hair shedding, constipation, a slower heart rate, feeling cold, or brain fog. Postpartum thyroiditis often appears within the first year after delivery, and a simple blood test starting with TSH (and usually free T4) can help clarify what is going on. If your symptoms started around 2–6 months postpartum, that timing is a common clue to mention.
What ingredients should you use for postpartum dry skin?
Ceramides, glycerin, and petrolatum are reliable because they reduce water loss and help rebuild the barrier. If you have rough, scaly patches, low-strength urea can soften flakes without the harshness of strong acids. If fragrance or “natural” oils make you itch, choose fragrance-free products for two weeks and see if the baseline irritation drops.
When should you worry about dry skin postpartum?
Get checked sooner if you have widespread redness with oozing, fever, or painful cracks that look infected, because skin infections can happen on top of dryness. Also follow up if dryness comes with strong fatigue, dizziness, or heavy ongoing bleeding, since low iron stores or thyroid changes may need treatment. A practical next step is to ask for TSH, ferritin, and vitamin D if your dryness is persistent and not responding to consistent barrier care.