Hair Thinning in Pregnancy: What It Means and What Helps
Hair thinning in pregnancy is often from iron depletion, thyroid shifts, or stress-related shedding. Targeted blood tests available—no referral needed.
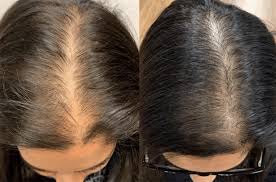
Hair thinning in pregnancy is usually caused by a shift in your hair-growth cycle, low iron stores, or thyroid changes that can show up even if you feel “mostly fine.” It can also happen when your scalp is inflamed or when you are unintentionally under-eating because nausea or heartburn makes food hard. Simple blood tests can often tell which bucket you are in, so you are not guessing. Seeing more scalp in the mirror can feel scary, especially when pregnancy is “supposed” to give you thicker hair. The truth is that pregnancy hormones help some people hold onto hair, but they do not protect everyone, and they cannot override iron depletion or thyroid problems. This page walks you through the most common reasons hair thins during pregnancy, what tends to help without risking the baby, and which labs are actually useful. If you want help matching your pattern to a likely cause, PocketMD can talk it through with you, and Vitals Vault labs can help you confirm what is going on.
Why your hair may thin during pregnancy
Iron stores get quietly depleted
During pregnancy, your blood volume expands and your baby uses iron for growth, so your iron “savings account” can drop even if your hemoglobin looks normal. When your iron stores are low, your hair follicles tend to exit the growth phase earlier, which can make your ponytail feel thinner over a couple of months. The practical takeaway is that ferritin (your stored iron) is often a better hair clue than a basic anemia screen, and it is worth checking if shedding is new or accelerating.
Thyroid shifts change hair cycling
Pregnancy can unmask thyroid underactivity or overactivity, and both can affect your hair because thyroid hormone helps set the pace of follicle growth. If your thyroid is off, hair thinning often comes with other “subtle” signs like feeling unusually cold, constipation, a racing heart, or anxiety that feels out of character. If you have a personal or family history of thyroid disease, or if hair thinning shows up alongside energy and temperature changes, a TSH test is a smart first step.
Normal hormone changes, different response
Even when pregnancy hormones are doing what they are supposed to do, your follicles can respond differently than someone else’s. Some people get the classic “pregnancy hair,” while others notice more shedding or a widening part because more hairs shift into a resting phase and then let go. This is frustrating, but it is often temporary, so taking photos of your part line every two weeks can help you see whether it is stabilizing or truly worsening.
Scalp inflammation and itching
If your scalp is flaky, itchy, or tender, the hair loss may be coming from irritation rather than hormones alone. Conditions like dandruff and scalp eczema can flare in pregnancy, and constant inflammation can make hairs break or shed sooner. The key takeaway is that treating the scalp gently and consistently can improve shedding, so do not ignore itching as “just pregnancy skin.”
Stress, illness, or under-eating
Your hair follicles are sensitive to big body stressors, including high stress, a febrile illness, surgery, or significant calorie restriction from nausea and food aversions. The shedding often shows up 6–12 weeks after the trigger, which is why it can feel like it came out of nowhere. If you have had hyperemesis, COVID, a bad flu, or rapid weight loss, anchoring the timeline can keep you from chasing the wrong cause and can guide you toward nutrition support.
What actually helps (and what to skip)
Treat low ferritin with a plan
If ferritin is low, your goal is to rebuild stores, not just “take a prenatal and hope.” Ask your clinician what iron dose fits your labs and stomach tolerance, because every-other-day dosing often causes fewer side effects while still working well. Pairing iron with vitamin C and avoiding taking it with calcium at the same time can improve absorption, which matters when you want results before delivery.
Get thyroid dosing truly pregnancy-safe
If your TSH suggests hypothyroidism, treatment is usually levothyroxine, and pregnancy has specific targets because your baby depends on thyroid hormone early on. The point is not to self-adjust, but to make sure your numbers are being followed closely enough, especially after dose changes. If you are already on thyroid medication and shedding is worsening, it is worth rechecking rather than assuming it is “just hormones.”
Use pregnancy-safe scalp care
When flaking and itching are part of the picture, improving the scalp environment can reduce breakage and shedding. Many people do well with an anti-dandruff shampoo used a few times a week and left on for several minutes before rinsing, plus a gentle conditioner on the hair lengths only. If you see patchy bald spots, thick scale, or oozing, that is a reason to ask for a dermatology evaluation because the treatment approach changes.
Reduce traction and breakage now
Pregnancy can make hair feel more fragile, so tight ponytails, braids, and extensions can turn mild thinning into obvious thinning at the hairline. Switching to loose styles, soft scrunchies, and a wide-tooth comb sounds small, but it protects the hairs you still have while the underlying cause is being addressed. If you notice thinning mainly at the temples, traction is especially worth considering.
Be cautious with “hair growth” supplements
A lot of hair supplements contain high-dose vitamin A or herbal blends that are not well studied in pregnancy, and too much vitamin A can be harmful. Biotin is popular, but it does not fix most pregnancy shedding and it can interfere with some lab tests, which can create confusion when you are trying to get answers. If you want to add anything beyond a prenatal, run the label by your OB or midwife first and prioritize targeted fixes like iron or thyroid treatment when indicated.
Useful biomarkers to discuss with your clinician
Ferritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreTSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreIron Binding Capacity
TIBC helps distinguish between different causes of abnormal iron levels. High TIBC indicates iron deficiency (the body increases transferrin to capture more iron), while low TIBC suggests iron overload or chronic disease. It's essential for accurate iron status assessment. Total Iron Binding Capacity (TIBC) measures the blood's capacity to bind iron with transferrin, the main iron transport protein. It indirectly reflects transferrin levels and iron status.
Learn moreLab testing
Check ferritin, TSH, and vitamin D at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “part photo” check-in: take a photo of your part in the same lighting once every two weeks. It is a calmer way to track change than staring daily, and it helps you notice when shedding is stabilizing.
If you are taking iron, try it away from calcium: take iron with a small vitamin C source and avoid taking it at the same time as milk, calcium supplements, or your prenatal if it contains calcium. That one timing tweak can make the same dose work better.
Treat your hair like delicate fabric for a month: skip tight styles, avoid heat tools when you can, and detangle only when your hair is damp with conditioner in. Less breakage makes true shedding easier to judge.
If nausea is limiting food, aim for “iron anchors” you can tolerate, such as fortified cereal, lentils, or meat in small portions. Even modest improvements in intake can prevent a slow slide in ferritin over the second and third trimester.
If you start biotin, pause it 48–72 hours before bloodwork unless your clinician says otherwise. It can distort some lab results, and you want your thyroid and other tests to be as interpretable as possible.
Frequently Asked Questions
Is hair thinning during pregnancy normal?
It can be normal, but it is not something you have to ignore. Pregnancy hormones can shift your hair cycle, yet low ferritin or thyroid changes can look the same in the mirror and are treatable. If thinning is new, fast, or paired with fatigue, feeling cold, or palpitations, checking ferritin and TSH is a practical next step.
When should I worry about hair loss in pregnancy?
Worry is reasonable if you see patchy bald spots, scalp pain, crusting, or rapidly widening areas of visible scalp, because that can point to inflammatory scalp disease or alopecia areata. Also flag it if you feel unwell in other ways, such as severe fatigue, shortness of breath, or a racing heart, because anemia or thyroid issues may be involved. Take a few scalp photos and bring them to your OB or dermatologist so you are not relying on memory.
What ferritin level is too low for hair growth?
Labs often mark ferritin as “normal” at low values, but hair follicles tend to struggle when ferritin is under about 30 ng/mL. Many clinicians aim for at least 30–50 ng/mL for hair support, and some people do best closer to 50–70 once treatment is underway. If your ferritin is low, ask for a specific recheck timeline, such as 6–10 weeks, so you can see if your plan is working.
Can thyroid problems cause hair thinning in pregnancy?
Yes. If your thyroid is underactive or overactive, your follicles can shift out of the growth phase, which shows up as diffuse thinning rather than a single bald patch. A TSH test is the usual starting point, and pregnancy has trimester-specific targets, so “normal” on a generic range is not always the full story. If you are already on levothyroxine, pregnancy often changes your dose needs, so rechecking matters.
What can I do right now that is safe for the baby?
Start with low-risk steps that protect hair you have and support the most common fixable causes. Use gentle, traction-free hairstyles, treat dandruff or itching consistently, and make sure your prenatal is not your only iron strategy if ferritin is low. If you want a clear plan, ask for ferritin, TSH, and vitamin D testing and then match your next step to the results.