Hair Thinning in Your 40s: What It Usually Means
Hair thinning in your 40s is often from hormone shifts, low iron stores, or thyroid changes. Targeted blood tests are available—no referral needed.
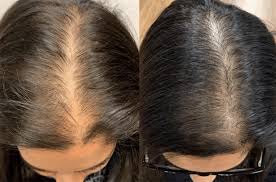
Hair thinning in your 40s is usually driven by a mix of genetics and shifting hormones, but low iron stores and thyroid changes can also quietly push more hairs into shedding. The pattern matters: gradual widening at the part points to pattern hair loss, while sudden extra shedding often points to a “reset” after stress, illness, or a medication change. A few targeted labs can help you figure out which bucket you’re in so you don’t waste months guessing. This symptom feels personal because it is. Your hair is one of the first places your body shows long-term trends in hormones, nutrition, and inflammation, and in your 40s those trends often start changing at the same time. The good news is that most causes are manageable once you name them, and you can usually see early signs you’re on the right track within 8–12 weeks. If you want help matching your pattern and timeline to the most likely causes, PocketMD can talk it through with you, and Vitals Vault labs can help confirm what’s going on under the hood.
Why hair thinning often shows up in your 40s
Pattern hair loss and sensitivity
This is the classic “genetic” kind of thinning, but the real driver is how sensitive your follicles are to androgens, especially DHT. In your 40s, that sensitivity can show up as a widening part, more scalp showing at the crown, or a gradually receding hairline. The takeaway is that earlier treatment tends to preserve more density, because once a follicle miniaturizes for years, it is harder to reverse.
Perimenopause hormone shifts
As estrogen and progesterone fluctuate in perimenopause, your growth phase can shorten and more hairs can shift into the resting phase, which means you notice more shedding and less “bounce.” You might also see texture changes, like hair feeling finer or less able to hold volume. If your periods are changing, your sleep is worse, or you’re getting new chin hairs along with scalp thinning, it’s a clue that hormones are part of the story.
Low iron stores (low ferritin)
Ferritin is your iron storage tank, and hair follicles are surprisingly sensitive to a low tank even when your hemoglobin is still “normal.” When ferritin is low, your body prioritizes essentials like oxygen delivery over “luxury” tissues like hair, so shedding can creep up and regrowth can stall. If you have heavy periods, donate blood, eat little red meat, or feel unusually winded, checking ferritin is one of the highest-yield steps.
Thyroid slowdown or overactivity
Your thyroid hormone sets the pace for many tissues, including how quickly hair cycles. When it is low, hair often becomes dry and brittle and sheds more diffusely; when it is high, you can also shed because the cycle speeds up and hairs drop sooner. If thinning comes with new fatigue, constipation, heat or cold intolerance, or eyebrow thinning, a TSH test can help you avoid treating the wrong problem.
Stress shedding (telogen effluvium)
After a big stressor—like a high fever, surgery, rapid weight loss, a new medication, or a major life event—your follicles can “pause” together and shed 2–3 months later. It feels alarming because it can come out in handfuls in the shower, but the scalp usually looks evenly thinner rather than patchy. The practical move is to look back 8–12 weeks for the trigger and focus on recovery, because the shedding often improves once your body feels safe again.
What actually helps hair thinning
Use 5% minoxidil consistently
Topical minoxidil helps keep follicles in the growth phase longer, which is why it is a first-line option for pattern thinning in both women and men. The hard part is patience: you can see a temporary increase in shedding in the first 2–8 weeks as older hairs make way for new growth. If you commit to daily use for at least 4–6 months, you give yourself a fair test of whether it is working for you.
Correct low ferritin carefully
If ferritin is low, replenishing iron can reduce shedding and support regrowth, but it works slowly because your body refills storage before it “spends” on hair. Many clinicians aim for ferritin around 50–70 ng/mL for hair goals, even if the lab’s lower limit is much lower. Ask for a plan that includes dose, timing with food, and a recheck in about 8–12 weeks so you know you’re actually moving the needle.
Treat thyroid issues, not just symptoms
If your TSH suggests hypothyroidism, the fix is not a supplement—it is getting the thyroid treated to the right level for you. For many people, hair improves when TSH is brought into a steady, mid-range zone and stays there for a few months, because follicles need time to cycle back. Bring your hair timeline to your clinician, because it helps them interpret whether the thyroid change is likely the main driver.
Make protein a daily target
Hair is built from protein, and in your 40s it is easy to drift into “light” meals that leave you under-fueled without realizing it. When your protein intake is low, your body can shift resources away from hair growth, especially if you are also dieting or exercising more. A practical target many people can act on is 25–35 grams of protein at breakfast and lunch, because spreading it out tends to work better than trying to catch up at dinner.
See a dermatologist for pattern confirmation
A scalp exam can tell the difference between pattern thinning, stress shedding, and inflammatory scalp conditions that need specific treatment. That matters because the wrong plan wastes time, and time is a real factor in hair density. If you have scalp burning, scaling, or obvious patches, prioritize an in-person evaluation sooner rather than later.
Useful biomarkers to discuss with your clinician
Ferritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreTSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreTestosterone, Total, Ms
Total testosterone is the primary male sex hormone responsible for muscle mass, bone density, libido, energy levels, and cognitive function. In functional medicine, we recognize testosterone as a key marker of vitality and aging. Low testosterone (hypogonadism) affects up to 40% of men over 45 and is linked to metabolic syndrome, cardiovascular disease, depression, and reduced quality of life. Optimal testosterone levels support healthy body composition, sexual function, motivation, and overall masculine vitalit…
Learn moreLab testing
Check ferritin, TSH, and vitamin D at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Take four photos today—front hairline, both temples, and the part under bright bathroom light—and repeat every 4 weeks. Your brain forgets what “normal” looked like, but photos make progress (or lack of it) obvious.
Do a simple 60-second part check once a week: pick the same spot, part your hair, and look for widening or more scalp show. If the part is widening slowly, think pattern thinning; if the part is stable but shedding is high, think stress shedding.
If you start minoxidil, set a calendar reminder for week 8 and week 16 so you do not quit during the “it looks worse” phase. That early shed is common and does not mean you are harming your hair.
If you suspect low iron, do not start high-dose iron blindly. Get ferritin checked first, because too much iron can be harmful, and the right dose depends on how low your stores actually are.
Treat your scalp like skin, not just “hair territory.” If you have itching, burning, or thick scale, use that as a signal to get evaluated, because inflammation can sabotage regrowth even when your labs look fine.
Frequently Asked Questions
Is hair thinning in your 40s normal or a sign of something wrong?
It is common, but it is not always “just aging.” In your 40s, pattern hair loss and perimenopause shifts are frequent, but low ferritin and thyroid changes are also fixable contributors. If thinning is new or accelerating, checking ferritin and TSH is a practical way to rule out common medical drivers.
What ferritin level is too low for hair growth?
Many people shed more when ferritin is low even if their hemoglobin is normal. For hair goals, clinicians often aim for ferritin around 50–70 ng/mL, because follicles seem to do better when iron stores are comfortably repleted. If your ferritin is below that, ask for a repletion plan and a repeat test in 8–12 weeks.
How can you tell if it’s stress shedding or pattern hair loss?
Stress shedding usually starts suddenly and peaks about 2–3 months after a trigger, and the thinning looks fairly even across your scalp. Pattern hair loss is slower and shows up as a widening part or thinning at the crown or temples. If you are unsure, a dermatologist can confirm the pattern with a scalp exam, which saves you months of trial-and-error.
Does perimenopause cause hair thinning even if your periods are still regular?
Yes. Hormones can fluctuate for years before cycles become obviously irregular, and those swings can shorten the hair growth phase so density slowly drops. If you also notice sleep changes, new facial hair, or more scalp oiliness, it strengthens the case that hormones are involved. Tracking your cycle and symptoms for 2–3 months gives your clinician much better context.
How long does it take to see regrowth after you fix the cause?
Hair moves slowly because follicles need time to cycle back into growth. With iron repletion or thyroid stabilization, many people notice less shedding in 8–12 weeks, while visible thickening often takes 4–6 months. Pick one or two measurable markers—like weekly shedding amount or monthly photos—so you can see change before you “feel” it.