Hair Thinning in Your 50s: What It Usually Means
Hair thinning in your 50s often comes from pattern hair loss, menopause-related hormone shifts, or low iron/thyroid issues. Targeted labs—no referral needed.
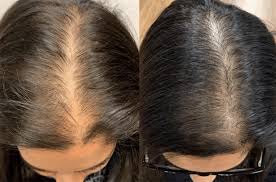
Hair thinning in your 50s is usually a mix of genetics (pattern hair loss), hormone shifts around menopause or andropause, and “silent” medical issues like low iron stores or thyroid imbalance. The tricky part is that these can overlap, so the right blood tests can help you figure out which driver is actually in the driver’s seat for you. It’s also a very normal time for hair to change. Hair follicles naturally spend less time in the growth phase as you age, and the scalp can start to show through even if you are not “going bald.” Still, it can feel personal and scary when your part widens, your ponytail shrinks, or you see more hair in the drain. This guide helps you tell common patterns apart, explains what’s happening under the surface, and lays out realistic next steps. If you want help connecting your symptoms, medications, and lab results into one story, PocketMD can walk through it with you, and Vitals Vault labs can help you test the most relevant markers without turning this into a months-long guessing game.
Why your hair thins in your 50s
Genetic pattern hair loss
This is the most common reason hair looks thinner in your 50s, even if you have always had “good hair.” The follicles slowly miniaturize, which means each hair grows in finer and shorter, so your scalp shows more easily over time. In women it often looks like a widening part or diffuse thinning on top, while in men it often starts at the temples or crown. The key takeaway is that this tends to be gradual and predictable, and earlier treatment works better than waiting until the scalp is very visible.
Menopause hormone shift
Around menopause, estrogen drops and the balance between estrogen and androgens (testosterone-like hormones) changes, even if your testosterone level is not “high.” That shift can make genetically sensitive follicles on the top of your scalp shrink faster, while facial hair can sometimes feel more stubborn. You might notice thinning that accelerates over 6–18 months rather than over a decade. If your thinning started around cycle changes, hot flashes, or sleep disruption, it is worth thinking about menopause as part of the picture.
Low iron stores (ferritin)
You can have “normal” hemoglobin and still have low iron reserves, and hair is one of the first places your body cuts back when supplies are tight. Low ferritin can shorten the growth phase, so more hairs shift into shedding at the same time and your density drops. This often feels like extra hair in the shower or brush, not just a slow change in your hairline. The practical move is to test ferritin before you start supplements, because too much iron is not harmless either.
Thyroid imbalance
Your thyroid helps set the pace for how fast cells turn over, including hair follicles, so both underactive and overactive thyroid can show up as thinning. People often describe hair that feels drier, more brittle, or harder to style, and the outer third of the eyebrows can thin too. Because thyroid symptoms can be subtle in your 50s, hair changes may be the clue that prompts testing. If you also have new fatigue, constipation, heat or cold intolerance, or unexplained weight change, bring that context to your clinician.
Stress shedding after a trigger
A big stressor can push many hairs into the “resting” phase at once, and then 2–3 months later you shed more than usual. This is called stress shedding (telogen effluvium), and it can follow surgery, a high fever, a crash diet, a new medication, or a major life event. It feels dramatic because the shedding is sudden, but the follicles are usually still alive and capable of regrowth once the trigger is addressed. The most helpful step is to think back three months and write down what changed, because the timing is often the giveaway.
What actually helps hair thinning
Use minoxidil consistently
Topical minoxidil is one of the best-studied options for pattern thinning, and it works by keeping follicles in the growth phase longer. The hard part is patience: shedding can increase in the first 4–8 weeks, and visible improvement usually takes 3–6 months. Pick a routine you can stick with, because stopping typically means you lose the gains over the next few months. If your scalp gets irritated, switching vehicle (foam vs solution) or using it once daily can make it tolerable.
Treat low ferritin on purpose
If ferritin is low, the goal is not just “take iron,” but to rebuild stores to a level that supports hair growth. Many hair specialists aim for ferritin roughly above 50–70 ng/mL for regrowth, even if the lab’s normal range starts much lower. Iron is absorbed best when you take it away from calcium and with vitamin C, and it often takes 8–12 weeks to see shedding calm down. Retesting ferritin after a few months keeps you from under-treating or overdoing it.
Fix thyroid issues, then wait
When thyroid levels are off, correcting them is the foundation, but hair does not bounce back overnight. Once your thyroid is stable, follicles still need time to cycle back into growth, so improvement often lags by 3–6 months. If you are already on thyroid medication and still thinning, it is worth checking whether your dose is actually getting you to a good range rather than just “technically normal.” Bring your TSH trend and your symptoms to the conversation, not just a single number.
Protect your hair from breakage
Not all “thinning” is from the root; sometimes the hair is snapping, which makes your ends look wispy and your volume disappear. Heat styling, tight ponytails, frequent bleaching, and aggressive brushing can all turn normal shedding into visible loss. Try a three-month experiment where you lower heat, loosen tension, and use a gentle detangling routine, because breakage can improve faster than true follicle miniaturization. If you see short broken hairs along your part line, this is especially worth addressing.
See a dermatologist for diagnosis
If your scalp is itchy, scaly, painful, or you have patchy bald spots, you may be dealing with an inflammatory or autoimmune condition rather than typical aging. A dermatologist can look with a dermatoscope, check for scarring, and sometimes do a small biopsy to avoid months of trial-and-error. This matters because scarring hair loss can become permanent if treatment is delayed. Take clear photos of your part and hairline every month so you can show the pace and pattern of change.
Useful biomarkers to discuss with your clinician
Ferritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreTSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreTestosterone, Total, Ms
Total testosterone is the primary male sex hormone responsible for muscle mass, bone density, libido, energy levels, and cognitive function. In functional medicine, we recognize testosterone as a key marker of vitality and aging. Low testosterone (hypogonadism) affects up to 40% of men over 45 and is linked to metabolic syndrome, cardiovascular disease, depression, and reduced quality of life. Optimal testosterone levels support healthy body composition, sexual function, motivation, and overall masculine vitalit…
Learn moreLab testing
Check ferritin, TSH, and vitamin D at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a “pattern check” in good light: take photos of your center part, temples, and crown once a month from the same distance. Slow pattern thinning looks different from sudden shedding, and photos stop your brain from catastrophizing on bad hair days.
Try the 60-second shed snapshot for one week: after brushing, count roughly how many hairs you see and write it down. A clear spike that started 2–3 months after an illness, surgery, or diet change points toward stress shedding rather than permanent loss.
If you color or heat-style your hair, run a three-month low-damage trial before you assume it is all “from the root.” Use the lowest heat that works, stop tight styles, and add a leave-in conditioner so breakage does not masquerade as thinning.
When you start minoxidil, set a calendar reminder for month 4 and month 6. Most people quit right before it starts to pay off, because the early shedding phase feels like proof it is failing when it is often a sign follicles are cycling.
If you supplement iron, do it with a plan: take it away from calcium, expect constipation, and recheck ferritin in about 8–12 weeks. Your goal is to rebuild stores, not to stay on iron forever without knowing where your level landed.
Frequently Asked Questions
Is hair thinning in your 50s normal or a sign of something wrong?
Some thinning is common in your 50s because follicles spend less time growing and more time resting, and genetics starts to show itself more clearly. But it can also be the first noticeable sign of low ferritin, thyroid imbalance, or stress shedding after an illness or major life event. If the change was sudden, patchy, or paired with fatigue, dry skin, or heavy shedding, lab tests like ferritin and TSH are a practical next step.
How can I tell if it’s menopause hair loss or just genetics?
Menopause often accelerates thinning on the top of the scalp because estrogen drops and follicles become more sensitive to androgens, so the change can feel faster over 6–18 months. Genetics can look similar, but it usually creeps along for years and may match family patterns. If your thinning started around cycle changes, hot flashes, or sleep disruption, menopause is likely part of the story, and a dermatologist can confirm the pattern on exam.
What ferritin level is too low for hair growth?
For hair, “normal” is not always “enough.” Many clinicians aim for ferritin above about 50–70 ng/mL when treating shedding or thinning, because regrowth can be sluggish when stores are low even without anemia. If your ferritin is below that, ask about a structured iron plan and a repeat ferritin test in 8–12 weeks to make sure you are actually repleting.
How long does it take for hair to grow back after stress shedding?
Stress shedding (telogen effluvium) usually starts about 2–3 months after the trigger, and shedding often improves over the next 3–6 months once the trigger is gone. Visible density can take longer because hair grows roughly 1 cm per month, so regrowth is slow even when follicles recover. If shedding is still heavy after 6 months, it is worth checking ferritin and TSH and considering a dermatology visit.
Does minoxidil work for women in their 50s, and is it safe?
Yes, minoxidil can help women in their 50s with pattern thinning by prolonging the growth phase of follicles, but it requires consistent use for at least 3–6 months to judge results. Early shedding in the first 4–8 weeks can happen and does not automatically mean it is making things worse. If you have scalp irritation, unwanted facial hair, or heart symptoms, talk with a clinician about adjusting the formulation or dose rather than quitting abruptly.