Why Is Your Skin So Dry in Your 40s?
Dry skin in your 40s often comes from a weaker skin barrier, hormone shifts, or low thyroid. Targeted labs available at Quest—no referral needed.
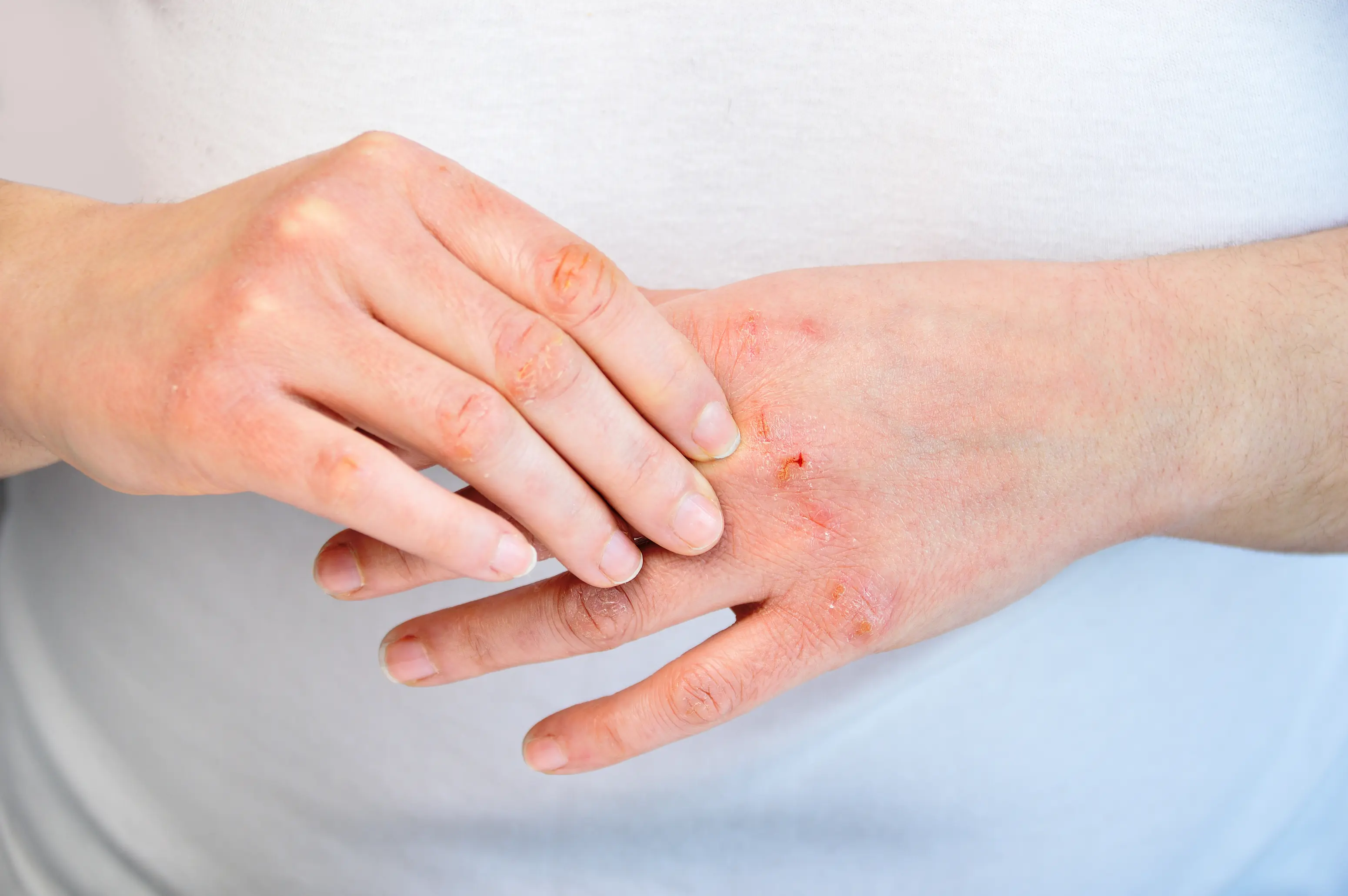
Dry skin in your 40s is usually a mix of a weaker skin barrier, lower oil production, and hormone shifts that change how well your skin holds onto water. Sometimes it is also a clue that something internal is contributing, like low thyroid or iron issues that show up as dryness plus fatigue or hair changes. A few targeted labs can help you sort out which bucket you are in so you stop guessing. In your 40s, “just moisturize more” often stops working because the problem is not only on the surface. Your skin’s outer layer is like a brick wall, and the “mortar” is made of fats called ceramides and cholesterol. When that mortar thins, water escapes faster, your skin feels tight after showering, and you can get itchy patches that look older than they are. This guide walks you through the most common reasons dryness ramps up now, what actually helps at home, and when it is worth using PocketMD to talk through your pattern or using Vitals Vault labs to check for internal drivers.
Why your skin gets drier in your 40s
Your skin barrier is leaking water
In your 40s, the outer layer of your skin often makes fewer of the fats that seal in moisture, so water evaporates faster even if you drink plenty of fluids. That is why your skin can feel tight within minutes of washing, and why fine lines can look more obvious when you are dry. The takeaway is to treat this like a barrier problem, not a hydration problem, which means using thicker, fragrance-free products that replace those fats.
Hormone shifts change oil production
During perimenopause, changing estrogen levels can reduce natural oil and slow down how quickly your skin repairs itself after irritation. You might notice dryness plus new sensitivity to products you used to tolerate, or flares that track with your cycle. If your dryness is paired with hot flashes, sleep disruption, or irregular periods, it is worth thinking “hormone transition” rather than “I suddenly forgot how to moisturize.”
Over-washing and hot showers
Hot water and foaming cleansers strip away the oils you do have, and in dry climates that can tip you into an itch-scratch cycle. It often shows up as dry shins, rough elbows, or hands that crack after frequent washing. A simple experiment helps: switch to lukewarm showers and a gentle, non-foaming cleanser for two weeks and see if the tightness after bathing improves.
Eczema (atopic dermatitis) returning
Eczema is not just a childhood thing, and in adults it can look like stubborn, itchy patches on the hands, eyelids, neck, or behind the knees. The itch can be intense at night, and scratching creates tiny breaks that let irritants in, which keeps the flare going. If you are moisturizing faithfully but still getting red, itchy plaques, treat it like inflammation and barrier damage, not “extra dry skin.”
Low thyroid slowing skin turnover
When your thyroid is underactive, your skin cells turn over more slowly and sweat and oil production can drop, which makes dryness feel deep and persistent. You might also notice constipation, feeling cold when others are fine, heavier periods, or thinning outer eyebrows. If that sounds like you, a thyroid-stimulating hormone test (TSH) is a practical next step because treating the root cause often improves your skin over a few months.
What actually helps dry skin
Moisturize like you mean it
The timing matters more than the brand. Put a thick moisturizer or ointment on within three minutes of bathing, while your skin is still slightly damp, because that traps water before it evaporates. If lotions disappear in an hour, move up to a cream with ceramides or an ointment with petrolatum, especially on shins, hands, and feet.
Use a gentle, non-foaming cleanser
If your cleanser leaves your face squeaky, it is probably taking too much oil with it. Switch to a fragrance-free, creamy cleanser and use it only where you actually need it, like armpits and groin, while letting water do the rest. This one change can reduce post-shower tightness in a week because you stop stripping the barrier every day.
Add urea for rough, scaly areas
Urea is a moisture-binding ingredient that also softens thick, rough skin, which makes it especially useful for heels, elbows, and “sandpaper” shins. Start with a 10% urea cream once daily, and back off if you feel stinging on cracked skin. If you pair it with an ointment on top at night, you often get faster smoothing without needing harsh scrubs.
Treat flares, not just dryness
When skin is red, itchy, and inflamed, plain moisturizer can feel like it is doing nothing because inflammation is driving the symptoms. Short courses of an anti-inflammatory cream prescribed by a clinician, plus consistent barrier repair, can break the itch-scratch cycle and prevent thickened patches. If you are waking up scratching or you have oozing or crusting, that is a good moment to get medical help rather than trying five more moisturizers.
Change your air, not your skin
Indoor heating can drop humidity enough that your skin loses water all night, which is why you wake up feeling tight and itchy. A bedroom humidifier aimed for about 40–50% humidity can make a noticeable difference within days, especially in winter or desert climates. Clean it regularly, because a dirty humidifier can irritate your airways and make you feel worse overall.
Useful biomarkers to discuss with your clinician
TSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreEstradiol
Estradiol in men is produced from testosterone via aromatase enzyme. In functional medicine, we recognize that men need optimal estradiol levels for bone health, cognitive function, and cardiovascular protection. However, excessive estradiol can suppress testosterone production and cause feminizing effects. The testosterone-to-estradiol ratio is crucial for male health, with optimal balance supporting vitality while preventing estrogen dominance. Balanced estradiol levels in men support bone health and cognitive…
Learn moreDhea Sulfate
DHEA-S levels reflect adrenal function and decline naturally with age. It's used to evaluate adrenal tumors, congenital adrenal hyperplasia, and androgen excess conditions like PCOS. Some consider it a marker of biological aging and stress resilience. DHEA-Sulfate (DHEA-S) is a hormone produced by the adrenal glands that serves as a precursor to sex hormones (testosterone and estrogen). It's the most abundant steroid hormone in the body.
Learn moreLab testing
Check thyroid, iron stores, and blood sugar at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a two-week “shower audit.” Keep showers under 10 minutes, use lukewarm water, and apply a thick moisturizer right after; if your tightness drops by day 7, your routine was a bigger driver than you thought.
If your hands are the worst, treat them like a job site. Use a fragrance-free ointment after every wash and wear cotton gloves under dish gloves or winter gloves so water and detergent do not keep stripping your barrier.
Patch-test new products on one forearm for three nights before putting them everywhere. If you get burning or redness in that small area, you just saved your face from a week-long flare.
For itchy legs at night, try the “double layer” method. Put a urea or ceramide cream on first, then seal it with a thin layer of petrolatum, because that reduces overnight water loss dramatically.
If you suspect eczema, take clear photos of the rash in good light when it is active. Patterns and locations help a clinician distinguish eczema from fungal rashes or contact allergy, which changes what treatment works.
Frequently Asked Questions
Is dry skin in your 40s a sign of perimenopause?
It can be, especially if dryness shows up alongside cycle changes, sleep disruption, or hot flashes. Shifting estrogen can reduce oil production and slow barrier repair, which makes your skin feel tight and more reactive. Track whether flares cluster around certain weeks of your cycle, and bring that pattern to a clinician if symptoms are escalating.
Why is my skin dry even when I drink a lot of water?
Most stubborn dryness is about your skin barrier leaking water, not your body being dehydrated. Hot showers, harsh cleansers, and lower oil production can all make the outer layer “porous,” so moisture escapes quickly. Focus on barrier repair by moisturizing within three minutes of bathing and switching to a gentle cleanser for two weeks.
What vitamin deficiency causes dry skin in adults?
Several nutrients can play a role, but low iron stores are a common, testable contributor when dryness comes with fatigue, brittle nails, or hair shedding. Ferritin is the lab that reflects iron stores, and many people feel better when ferritin is at least above about 30 ng/mL, with some aiming higher depending on symptoms. If you suspect a deficiency, test first so you supplement the right thing in the right dose.
Can hypothyroidism cause dry, itchy skin?
Yes. Low thyroid can reduce sweat and oil production and slow skin turnover, which makes dryness feel deep and persistent rather than just “a little flaky.” A TSH test is the usual starting point, and it is especially relevant if you also feel cold easily, have constipation, or notice hair thinning. If TSH is abnormal, ask about follow-up free T4 and a treatment plan rather than only changing skincare.
When should I worry about dry skin and see a doctor?
Get checked if you have widespread redness, painful cracking, oozing or crusting, or itching that wakes you up most nights, because those can signal eczema, infection, or another treatable condition. It is also worth a visit if dryness is paired with new fatigue, hair loss, or unexplained weight change, since labs like TSH, ferritin, and A1c can uncover internal drivers. Bring photos of any rash and a list of products you use so you get a faster, clearer answer.