Dry Skin in Women: What It Means and What Helps
Dry skin in women often comes from barrier damage, low thyroid, or eczema flares. Targeted blood tests are available at Quest—no referral needed.
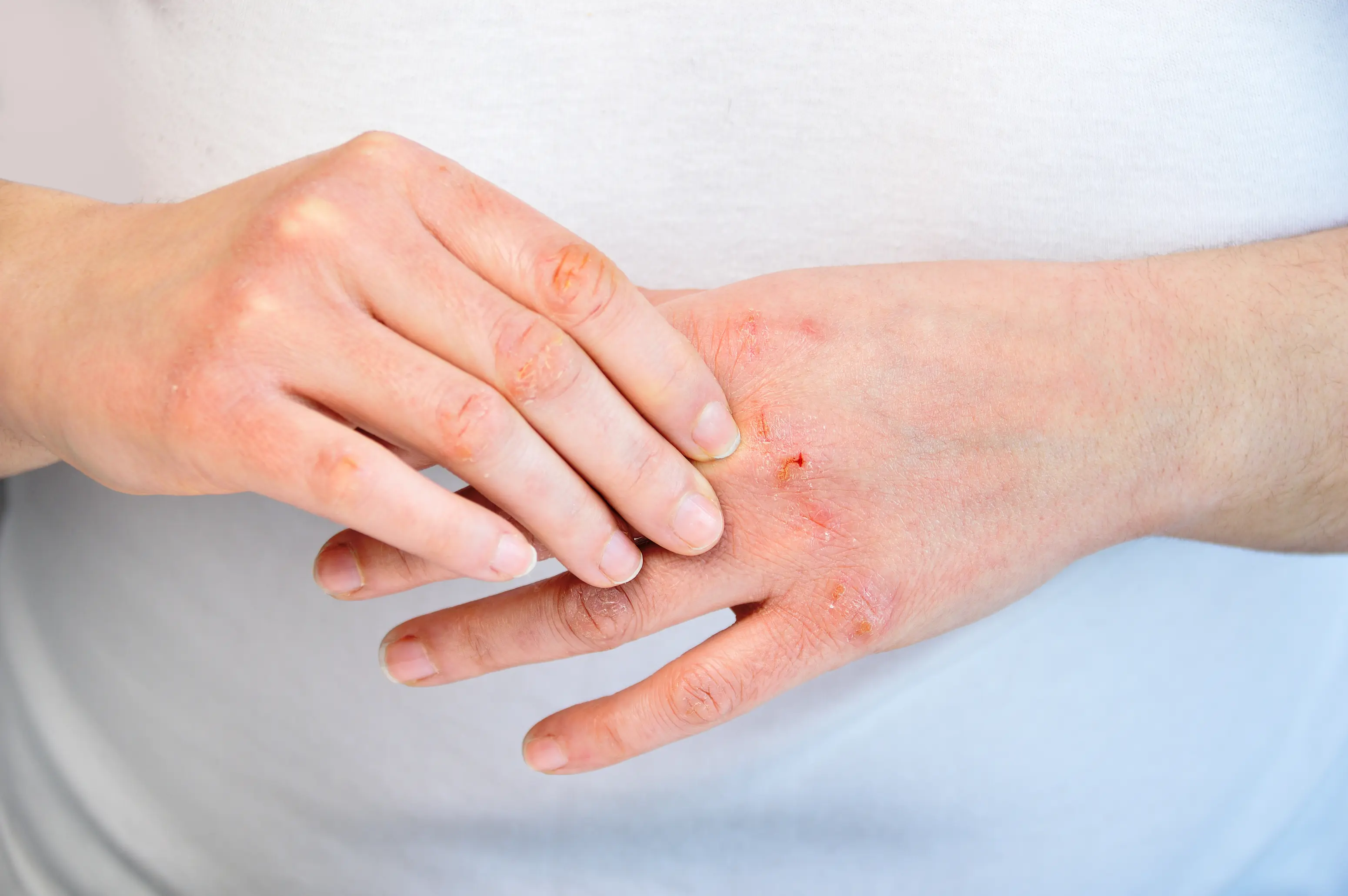
Dry skin in women is usually a skin-barrier problem, but it can also be your hormones shifting (especially around perimenopause), an eczema flare, or an underactive thyroid. The reason it “won’t moisturize away” is that water is escaping through a leaky outer layer, or your skin isn’t making enough protective oils. A few targeted labs can help you spot when it’s more than just weather and soap. Dryness can look like tightness after showering, fine flaking that shows up under makeup, or itching that gets worse at night. It is common, but it is not always simple, because the same dry feeling can come from very different causes. This page helps you connect the pattern you’re seeing to likely root causes, then gives you practical fixes that actually match the cause. If you want help narrowing it down to your situation, PocketMD can walk through your symptoms and triggers, and Vitals Vault labs can help confirm things like thyroid or iron issues when they fit the story.
Why your skin feels dry (and keeps coming back)
Your skin barrier is leaking
Your outer skin layer is supposed to hold water in and irritants out, but harsh cleansers, hot showers, and low humidity can strip the oils that seal it. When that barrier is compromised, you can moisturize and still feel tight again an hour later because water keeps evaporating. The most useful takeaway is to treat dryness like a barrier injury: reduce stripping steps first, then seal the skin while it is still slightly damp.
Eczema flare (atopic dermatitis)
Eczema is not just “extra dry skin.” It is an overreactive immune response in the skin that makes you itchy, inflamed, and more sensitive to detergents, fragrance, and stress. You may notice rough patches in typical areas like hands, eyelids, neck, or the bends of elbows and knees, and scratching can create a cycle that keeps the barrier broken. If your dryness comes with recurrent itch and redness, you usually need anti-inflammatory treatment plus barrier care, not just a richer lotion.
Perimenopause and lower estrogen
As estrogen fluctuates and trends lower, your skin makes less oil and loses some of the “plump” water-holding support in the deeper layers. That can show up as sudden dryness, more visible fine lines, and irritation from products you used to tolerate. The practical clue is timing: if dryness ramps up with new cycle changes, hot flashes, or sleep disruption, it is worth thinking “hormone transition” and adjusting skincare toward gentler cleansing and heavier sealing at night.
Underactive thyroid (hypothyroidism)
When your thyroid is underactive, your whole system slows down, including skin turnover and oil production. Dryness often comes with other hints like feeling cold, constipation, heavier periods, hair thinning, or puffy face and hands. If dry skin is new and persistent despite good topical care, a simple TSH blood test can be a high-yield way to check whether your thyroid is part of the picture.
Low iron stores or low vitamin D
Iron and vitamin D do not “moisturize” your skin directly, but low levels can show up alongside fatigue, hair shedding, brittle nails, and slower skin repair. If your skin feels fragile, irritated, and slow to recover from minor rashes, it can be a sign your body is missing building blocks. The actionable step is to connect symptoms: if dryness travels with low energy or hair changes, checking ferritin and vitamin D can prevent months of guessing.
What actually helps dry skin
Switch to a gentle, short cleanse
If your face or body feels squeaky-clean after washing, that is often a sign you stripped too much oil. Use a fragrance-free, non-foaming cleanser, keep showers lukewarm, and limit soap to the areas that truly need it. This one change can make your moisturizer work again because you stop undoing the barrier every day.
Moisturize like you’re sealing in water
Moisturizer works best when it traps water that is already on your skin. Apply it within three minutes of bathing, and consider a two-layer approach at night: a cream with ceramides, then a thin layer of petrolatum on the driest spots. If your hands are the problem, doing this after every wash for one week is a surprisingly strong “reset.”
Use urea or lactic acid for flakes
When dryness comes with rough, stubborn scale, you often need a keratolytic ingredient that loosens the “glue” holding dead skin cells. Urea (around 10%) or lactic acid (around 5–12%) can smooth texture and reduce that dusty flaking that shows under clothes or makeup. Start every other day at first, because overdoing it can sting when your barrier is already irritated.
Treat itch and inflammation early
If you are scratching, your skin cannot heal, and the dryness will keep winning. For short flares, an over-the-counter 1% hydrocortisone can calm red, itchy patches, while thick emollients reduce the urge to scratch. If you need steroid cream most days, or you have cracking, oozing, or frequent infections, that is a good moment to see a clinician for a safer long-term plan.
Match the plan to the cause
If labs point to hypothyroidism, treating the thyroid often improves dryness over weeks as your skin turnover normalizes. If ferritin is low, replenishing iron can help with hair and nail changes that often travel with dry, fragile skin. The key is patience with the right target: barrier repair can improve in days, but internal causes usually take one to three months to show on your skin.
Lab tests that help explain dry skin in women
TSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreEstradiol
Estradiol in men is produced from testosterone via aromatase enzyme. In functional medicine, we recognize that men need optimal estradiol levels for bone health, cognitive function, and cardiovascular protection. However, excessive estradiol can suppress testosterone production and cause feminizing effects. The testosterone-to-estradiol ratio is crucial for male health, with optimal balance supporting vitality while preventing estrogen dominance. Balanced estradiol levels in men support bone health and cognitive…
Learn moreVitamin D, 25-Oh, Total
Total 25-hydroxyvitamin D represents the best measure of vitamin D status, combining both D2 and D3 forms. This is the storage form of vitamin D and reflects recent intake and synthesis. In functional medicine, total 25(OH)D is used to assess vitamin D sufficiency and guide supplementation. Optimal levels (40-80 ng/mL) are associated with reduced risk of cancer, cardiovascular disease, autoimmune conditions, and all-cause mortality. Vitamin D acts as a hormone affecting immune function, bone health, mood, and ce…
Learn moreLab testing
Check TSH, ferritin, and vitamin D at Quest—starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a 7-day “barrier reset”: lukewarm showers, fragrance-free cleanser only where needed, then a ceramide cream within three minutes of drying off. If your skin improves quickly, the main problem was barrier stripping, not a mysterious internal disease.
If your face looks flaky under makeup, try applying moisturizer, waiting 10 minutes, and then using a damp makeup sponge. It sounds simple, but it reduces the visible “lift” of dry scales better than adding more foundation.
For hand dryness, keep a tube of thick ointment by every sink and use it after each wash. One week of consistency usually beats buying a new product every month.
If itching wakes you up, treat the itch before bed with a thick emollient and a cool compress for five minutes on the worst patch. Night scratching is a big reason dry skin turns into cracks and dark marks.
Take photos of the worst areas in the same lighting once a week. It helps you notice whether a change is truly working, especially when dryness fluctuates with your cycle, stress, or weather.
Frequently Asked Questions
Why is my skin so dry even when I moisturize?
Usually it is because your skin barrier is still leaking water, so the moisture you apply cannot stay put. Hot showers, foaming cleansers, and frequent exfoliation are common reasons this happens. Try a one-week reset with lukewarm bathing and a thick fragrance-free cream applied within three minutes of drying off, and see if the “tight again in an hour” feeling improves.
Can hormones cause dry skin in women?
Yes. Estrogen shifts in perimenopause and menopause can reduce skin oil production and weaken the barrier, which can make you feel dry and more sensitive to products you used to tolerate. If dryness shows up alongside cycle changes, new sleep issues, or hot flashes, treat it as a hormone-transition pattern and prioritize gentle cleansing plus heavier night sealing.
What vitamin deficiency causes dry skin?
Several nutrient issues can contribute, but low vitamin D and low iron stores (measured by ferritin) are common ones that show up with other symptoms like fatigue, hair shedding, or brittle nails. Dryness alone is not enough to diagnose a deficiency, but if you have a cluster of symptoms, testing 25-hydroxy vitamin D and ferritin can be more useful than guessing supplements. If you do supplement, recheck levels in about 8–12 weeks to confirm you actually corrected the problem.
Does hypothyroidism cause dry skin?
It can. An underactive thyroid slows skin turnover and reduces oil production, so dryness often comes with feeling cold, constipation, heavier periods, or hair thinning. A TSH blood test is the usual first step, and many people who feel symptomatic have a TSH above roughly 2.5–4.0 mIU/L even if it is only mildly elevated. If your TSH is abnormal, follow up with a clinician for interpretation and next-step testing.
When should I worry about dry skin and see a doctor?
Get checked if you have deep cracks that bleed, signs of infection like spreading redness or pus, or a rash that is rapidly worsening. It is also worth an appointment if dryness is new and persistent for more than 6–8 weeks despite a barrier-focused routine, especially if you also have fatigue, hair loss, or menstrual changes. Bringing a short timeline and photos of flares makes the visit much more productive.
Research worth knowing about
AAD guidelines for atopic dermatitis outline moisturizers, topical anti-inflammatories, and trigger management as core treatment
Cochrane review: moisturizers reduce eczema flares and can decrease the need for topical steroids in atopic dermatitis
Review of skin changes in menopause describes reduced lipids and barrier function contributing to dryness and irritation