Dry Skin in Your 50s: What’s Going On and What Helps
Dry skin in your 50s is often from a weaker skin barrier, lower estrogen, or thyroid changes. Targeted blood tests are available—no referral needed.
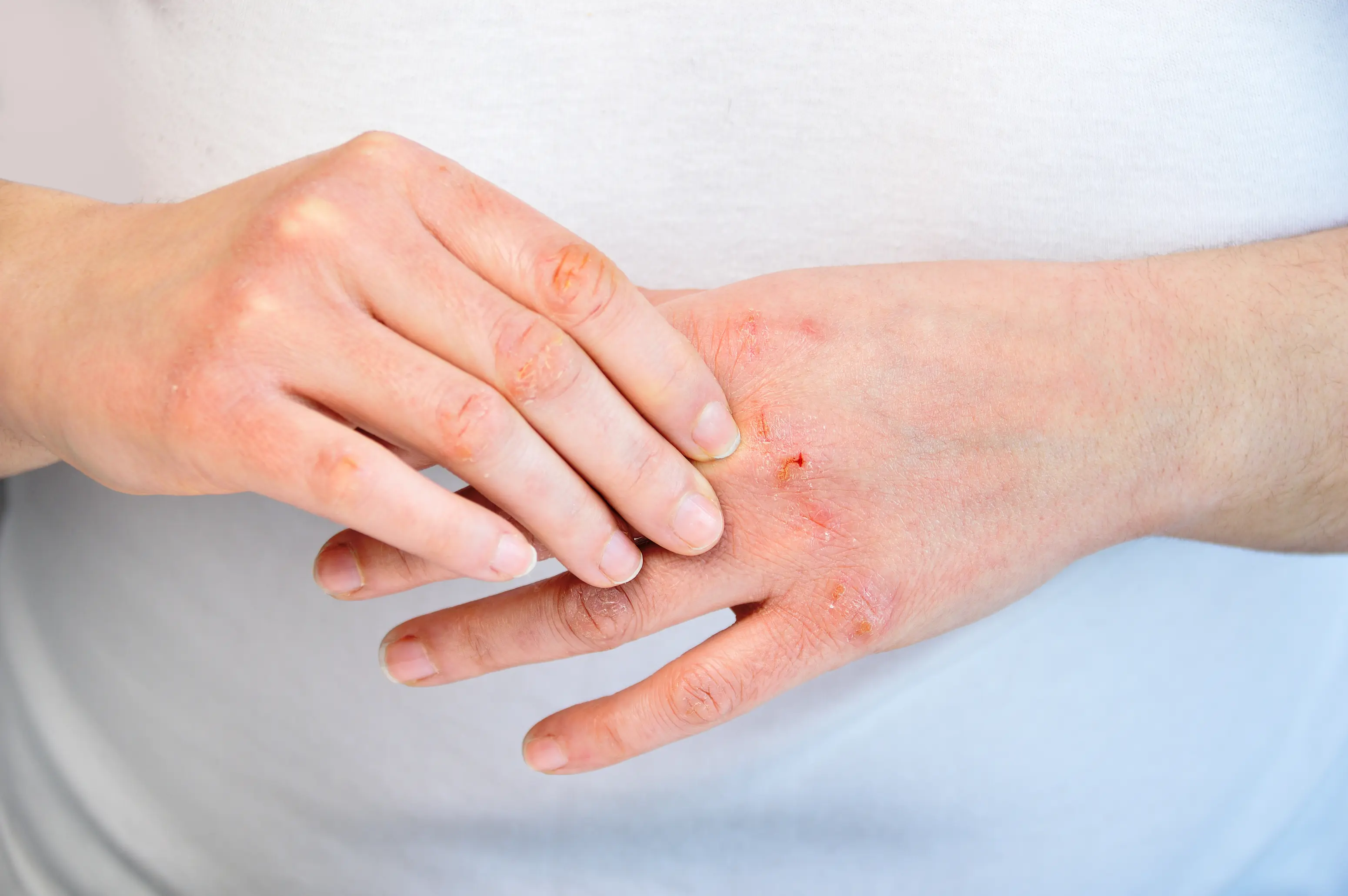
Dry skin in your 50s is usually a mix of a weaker skin barrier, hormone shifts (especially lower estrogen), and slower oil production, which means water escapes your skin faster than you can replace it. Sometimes it is also a clue that something internal is adding fuel, like an underactive thyroid or iron deficiency. A few targeted labs can help you figure out which bucket you are in so you are not guessing. This can feel unfair because you might be moisturizing more than ever and still feeling tight, flaky, or itchy by midday. In your 50s, your skin simply behaves differently, and the “fix” is often about timing, texture, and barrier repair rather than buying a stronger scented lotion. If you want help matching your exact pattern to the most likely causes, PocketMD can talk it through with you, and Vitals Vault labs can help you check the internal contributors that topical products cannot touch.
Why dry skin shows up in your 50s
Your skin barrier leaks moisture
As you get older, your outer layer of skin holds onto fewer natural fats and water-binding molecules, so moisture evaporates more easily. That is why your skin can feel tight right after you shower and then look ashy or flaky a few hours later. The takeaway is that “more lotion” is not the same as “better barrier,” so look for thick, fragrance-free products with ceramides and petrolatum and apply them while your skin is still slightly damp.
Lower estrogen dries skin out
Around menopause, lower estrogen can reduce skin thickness and oil production, and it can also change how well your skin makes collagen. You may notice dryness plus new sensitivity, crepey texture, or itching that seems out of proportion to what you see. If this started around cycle changes, hot flashes, or vaginal dryness, it is worth discussing menopause care with a clinician because the right plan can improve skin comfort along with other symptoms.
Underactive thyroid slows turnover
When your thyroid runs low, your skin cells turn over more slowly and your sweat and oil glands can become less active, which leaves you feeling rough and dry. The “so what” is that no moisturizer fully fixes thyroid-driven dryness, and you often also feel colder than others, more tired, or constipated. A simple blood test for TSH and free T4 can quickly tell you if this is part of your story.
Eczema flares more easily now
Eczema (atopic dermatitis) is basically an overreactive immune response plus a fragile barrier, and both can become more noticeable with age and dry indoor air. It often feels like itch first, especially at night, and scratching can create a cycle of thicker, darker, more inflamed patches. If you have recurrent itchy areas in the same spots, treat it like inflammation, not just dryness, and ask about short courses of prescription anti-inflammatory creams when needed.
Blood sugar changes dehydrate skin
When blood sugar runs high, your body pulls water into the urine, and you can become mildly dehydrated even if you are drinking normally. You might notice dry mouth, more frequent urination, slower healing, or itchiness along with the dryness. Checking an HbA1c can be a practical way to see whether glucose is contributing, especially if dryness arrived with weight changes or a strong family history of diabetes.
What actually helps dry skin
Moisturize within 3 minutes
Timing matters because water evaporates fast after bathing. Pat your skin dry so it is not dripping, then apply a thick cream or ointment within three minutes to “seal in” the water that is already there. If you only change one thing, change this, because it often cuts flaking within a week.
Switch to a gentle cleanser
Many body washes strip oils on purpose, which feels “squeaky clean” but leaves your barrier defenseless. Use a fragrance-free, low-foam cleanser on the areas that truly need it, and let warm water do the rest. You will usually notice less tightness after showers within a few days.
Use an ointment on problem spots
If your shins, hands, or elbows keep cracking, a lotion is often too light to keep up. At night, apply a thin layer of petrolatum-based ointment over your moisturizer on those areas, and consider cotton gloves or socks to keep it in place. This “double layer” approach is simple, cheap, and surprisingly effective for fissures.
Treat itch like inflammation
Itch is not just a nuisance; it is a signal that your skin nerves and immune system are irritated. For short bursts, an over-the-counter 1% hydrocortisone can calm mild flares, but if you need it most days or you see oozing, crusting, or spreading redness, you should get checked because you may need a stronger anti-inflammatory or treatment for infection. The goal is to break the scratch cycle before your skin thickens and stays itchy.
Fix the air, not just skin
Dry indoor air quietly pulls water out of your skin all night, which is why you can wake up feeling tight and itchy. A bedroom humidifier aimed for about 40–50% humidity often makes moisturizers work better, especially in winter or desert climates. If you try this, clean the humidifier regularly so you are not breathing in mold.
Useful biomarkers to discuss with your clinician
TSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreEstradiol
Estradiol in men is produced from testosterone via aromatase enzyme. In functional medicine, we recognize that men need optimal estradiol levels for bone health, cognitive function, and cardiovascular protection. However, excessive estradiol can suppress testosterone production and cause feminizing effects. The testosterone-to-estradiol ratio is crucial for male health, with optimal balance supporting vitality while preventing estrogen dominance. Balanced estradiol levels in men support bone health and cognitive…
Learn moreDhea Sulfate
DHEA-S levels reflect adrenal function and decline naturally with age. It's used to evaluate adrenal tumors, congenital adrenal hyperplasia, and androgen excess conditions like PCOS. Some consider it a marker of biological aging and stress resilience. DHEA-Sulfate (DHEA-S) is a hormone produced by the adrenal glands that serves as a precursor to sex hormones (testosterone and estrogen). It's the most abundant steroid hormone in the body.
Learn moreLab testing
Check TSH, free T4, ferritin, and HbA1c at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a two-week “skin audit”: take one shower a day max, keep water warm not hot, and note whether the tightness improves within 72 hours. If it does, your routine was stripping your barrier more than you realized.
If your legs look like fine white “craquelure” lines, try an ointment on shins at night for seven nights straight. That pattern is often simple barrier dryness, and it responds better to occlusion than to fancy actives.
For itchy patches, take a photo the day it starts and again three days later. If the area is expanding, oozing, or developing honey-colored crust, treat it as a possible infection and get it looked at rather than just switching moisturizers.
If hand dryness is your main issue, keep a small tube of thick cream by every sink and apply after every wash. Consistency beats intensity here, and it prevents the tiny cracks that make everything sting.
When you test a new product, try it on one forearm for three nights before putting it everywhere. If you react, you will know quickly, and you will not end up with a full-body flare from a single “miracle” ingredient.
Frequently Asked Questions
Why is my skin suddenly so dry in my 50s?
In your 50s, your skin barrier tends to hold less water and your oil production slows, so moisture escapes faster than it used to. Menopause-related estrogen decline can add dryness and sensitivity, and thyroid changes can make dryness feel stubborn. If it is new and persistent, consider checking TSH with free T4 and reviewing any new soaps, retinoids, or medications.
Is dry skin a sign of menopause?
It can be, especially if it shows up alongside hot flashes, sleep disruption, or vaginal dryness. Lower estrogen can reduce skin thickness and oil production, which makes you feel tight and itchy even with regular moisturizing. If the timing fits, bring it up at your next visit because menopause treatment options can improve skin comfort too.
What vitamin deficiency causes dry skin?
Several nutrients affect skin, but low iron stores are a common, testable contributor in adults and can show up as dry skin plus brittle nails, hair shedding, or fatigue. Ferritin is the lab marker that reflects iron reserves, and many people feel better when ferritin is at least around 50 ng/mL. If you supplement, do it with guidance because too much iron is also a problem.
What is the best moisturizer for very dry skin in your 50s?
For very dry skin, thick fragrance-free creams or ointments usually work better than lotions because they reduce water loss. Look for barrier helpers like ceramides and choose petrolatum-based ointments for cracked areas, especially at night. Apply within three minutes after bathing for the biggest payoff.
When should I worry about dry skin and see a doctor?
You should get checked if dryness comes with severe itch that disrupts sleep, painful cracks that bleed, or redness that is spreading or oozing. It is also worth a visit if you have other symptoms like unusual fatigue, constipation, feeling cold, or hair thinning, because thyroid issues can drive dryness and are easy to test with TSH and free T4. Bring photos of your worst days and a list of new products you started in the last month.