Why Your Skin Gets Dry During Your Period
Dry skin during period is often from estrogen dips, barrier water loss, or low iron/thyroid shifts. Targeted labs available—no referral needed.
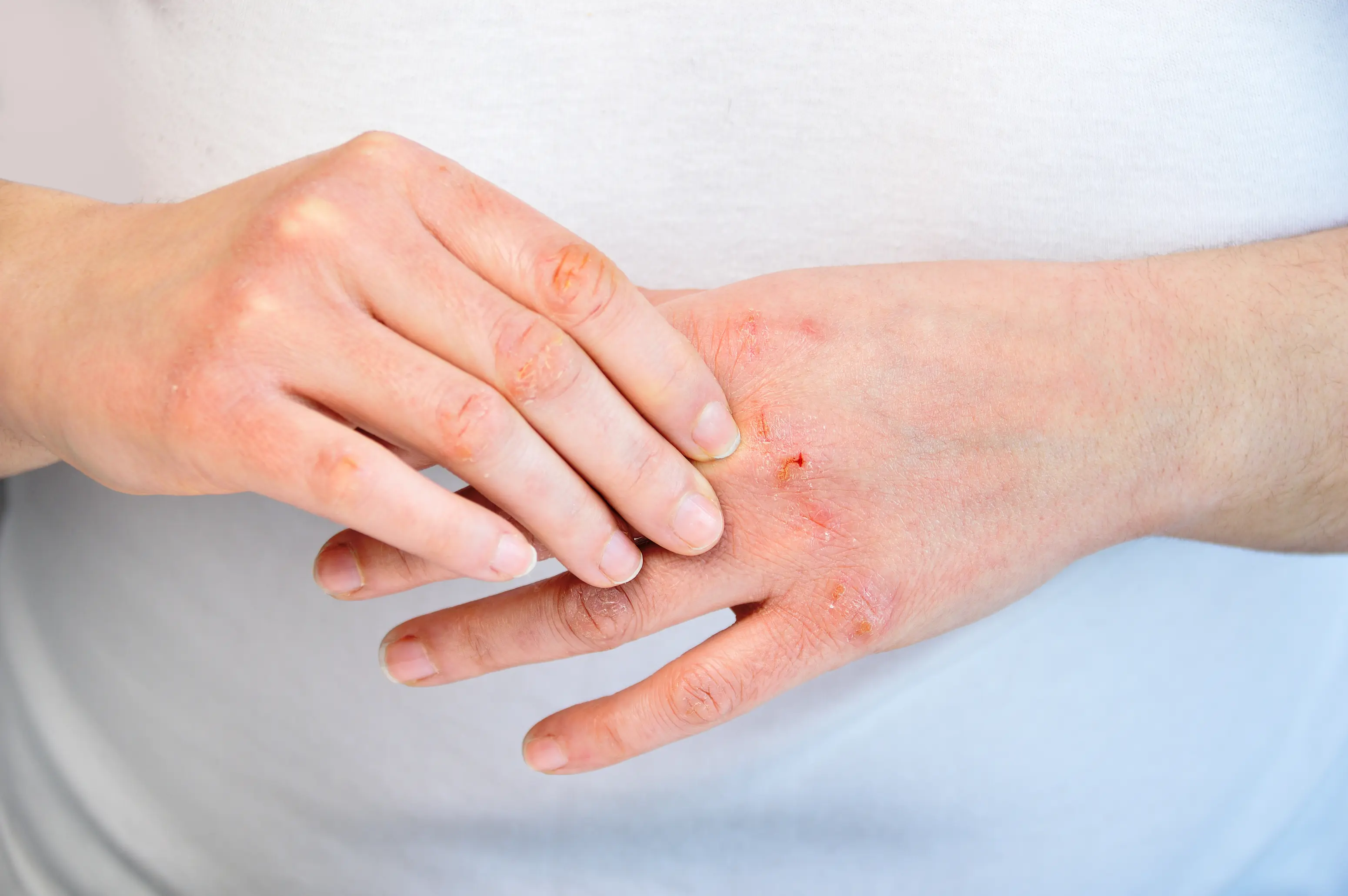
Dry skin during your period usually happens because estrogen drops, which weakens your skin barrier and lets water escape faster. It can also show up when period-week inflammation flares conditions like eczema, or when an underlying issue such as low iron stores or a sluggish thyroid makes your baseline skin drier. Simple labs can help you figure out which pattern fits you. If you feel like you are moisturizing “correctly” and your skin still looks dull, tight, or itchy right around your bleed, you are not imagining it. Hormones change how much oil your skin makes, how well it holds onto water, and how reactive it becomes to products, weather, and hot showers. This page walks you through the most common reasons, what actually helps in real life, and when it is worth using PocketMD to talk it through or ordering targeted labs through Vitals Vault to rule out fixable contributors.
Why your skin gets dry during your period
Estrogen dip weakens your barrier
In the days before and during bleeding, estrogen tends to be lower, and that can reduce the skin’s ability to hold onto water and repair itself. You feel this as tightness after washing, makeup that suddenly looks cakey, or fine lines that seem more obvious even though nothing “aged” overnight. Treat period week like barrier-repair week: use a gentle cleanser and put a moisturizer on within a few minutes of getting your face or body wet.
Less oil production, more roughness
When hormones shift, your oil glands can temporarily slow down, so your natural “seal” over the skin is thinner. That matters most on your shins, hands, and around your mouth, where skin already runs drier and cracks more easily. If you notice flaking that improves mid-cycle, it is a clue that you need a richer, more occlusive layer during your period rather than a totally new routine.
Eczema flares with cycle inflammation
If you have eczema (atopic dermatitis), period-week immune changes can make your skin more reactive and itchy, even if your products have not changed. The itch-scratch cycle can damage the barrier fast, which is why a small patch can suddenly feel like it is spreading. A practical takeaway is to treat early: use your thickest moisturizer twice daily on “hot spots,” and consider asking your clinician about a short course of anti-inflammatory cream if you get predictable monthly flares.
Hot showers strip protective oils
Cramps and fatigue can make long, hot showers feel like the only comfort, but heat and surfactants pull lipids out of your outer skin layer. You often notice dryness most after you towel off, especially on legs and arms, because the water evaporates and leaves your skin feeling papery. If you keep the shower warm instead of hot and moisturize while your skin is still slightly damp, you can get the comfort without the rebound dryness.
Low iron or thyroid makes it worse
Sometimes your cycle is just the time you notice dryness because your baseline is already on the dry side. Low iron stores (low ferritin) can be linked with brittle nails and hair shedding, and hypothyroidism (an underactive thyroid) slows skin turnover so it feels thick, rough, and stubbornly dry. If your dryness comes with heavy periods, constipation, feeling cold, or unusual fatigue, it is worth checking ferritin and TSH rather than assuming it is “just hormones.”
What actually helps (and what to skip)
Do a 7-day barrier reset
For one week around your period, simplify: a fragrance-free gentle cleanser, a ceramide-based moisturizer, and sunscreen in the morning. This works because it reduces irritation while your barrier is already more vulnerable, and it gives your skin a chance to rebuild its “mortar.” If your flaking improves during the reset, you have learned that irritation and barrier stress are a big part of your pattern.
Moisturize like a sandwich
Right after bathing, apply a humectant layer (like glycerin or hyaluronic acid) and then seal it with a thicker cream or ointment. The first layer pulls water into the outer skin, and the second layer slows evaporation, which is the step many people miss. If your skin stings when you apply products, skip acids and retinoids that week and focus on sealing and soothing.
Switch to lukewarm and shorter showers
Aim for 5–10 minutes and keep the water lukewarm, especially if you are washing your whole body. This reduces the amount of oil you strip off, which means less tightness and fewer itchy patches later in the day. If you need heat for cramps, try a heating pad on your abdomen instead of turning your shower into a sauna.
Target itchy spots, not your whole body
When one area is flaring, covering your entire body in heavy ointment can feel greasy and still not fix the problem. Instead, spot-treat the driest areas twice a day and use a lighter lotion elsewhere, which keeps you consistent. If you see cracks, bleeding, honey-colored crust, or rapidly worsening redness, get checked because infection can piggyback on broken skin.
Time exfoliation away from period week
Scrubs and strong acids can make dryness worse when your barrier is already stressed, even if they normally work for you. If you like exfoliation, move it to mid-cycle when your skin tends to tolerate more, and keep it gentle. The goal is smoothness without that “burning after moisturizer” feeling that tells you your barrier is overworked.
Lab tests that help explain dry skin during your period
Estradiol
Estradiol in men is produced from testosterone via aromatase enzyme. In functional medicine, we recognize that men need optimal estradiol levels for bone health, cognitive function, and cardiovascular protection. However, excessive estradiol can suppress testosterone production and cause feminizing effects. The testosterone-to-estradiol ratio is crucial for male health, with optimal balance supporting vitality while preventing estrogen dominance. Balanced estradiol levels in men support bone health and cognitive…
Learn moreIron, Total
Serum iron measures the amount of iron circulating in your blood at the time of testing. In functional medicine, we recognize that serum iron alone provides limited information about iron status, as it fluctuates throughout the day and is affected by recent iron intake, inflammation, and diurnal variation. However, when combined with other iron studies, it helps assess iron metabolism and transport. Iron is essential for oxygen transport, energy production, DNA synthesis, and immune function. Optimal serum iron…
Learn moreTSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreLab testing
Check ferritin, TSH, and vitamin D at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Try a “period-week kit” you only use from about 3 days before bleeding through day 3: gentle cleanser, thick ceramide cream, and a plain ointment for lips and nostrils. The predictability makes it easier to stick with it.
If your legs get scaly, apply moisturizer before you fully dry off, then put on loose cotton leggings for an hour. That little bit of occlusion often beats reapplying lotion five times a day.
When your face feels tight but looks oily, do not chase it with harsh acne washes. Use a gentle cleanser and add a light barrier cream, because dehydrated skin can overproduce oil as a rebound.
If itching wakes you up, keep a small tube of ointment by your bed and apply it the moment you notice the urge to scratch. Stopping the scratch early prevents the next-day flare more than any fancy product does.
Take two phone photos of the same area in the same lighting: one mid-cycle and one during your period. Seeing the difference helps you decide whether this is truly cycle-linked or more about weather, products, or shower habits.
Frequently Asked Questions
Is dry skin during your period normal?
Yes, it can be normal because estrogen tends to be lower around bleeding, and that can weaken your skin barrier so water escapes faster. You usually notice tightness after washing, flaking, or itch that improves later in the cycle. If it is new, severe, or comes with fatigue, heavy bleeding, or feeling cold, consider checking ferritin and TSH.
Why is my skin so dry right before my period starts?
Right before bleeding, estrogen and progesterone shift, and your skin can temporarily make less oil while also holding less water. That combination makes products feel like they “sit on top” and your skin still feels tight. A practical fix is to start your richer moisturizer and gentler cleanser 2–3 days before your period rather than waiting until you are already flaky.
Can low iron cause dry skin during your period?
Low iron stores can make your skin look dull and can travel with brittle nails, hair shedding, and fatigue, especially if your periods are heavy. Ferritin is the key test because it can be low even when hemoglobin is still normal. If ferritin is under about 30–50 ng/mL and you have symptoms, talk with a clinician about iron replacement and recheck levels.
What moisturizer ingredients work best for hormonal dry skin?
Look for a mix of water-binding ingredients like glycerin or hyaluronic acid plus barrier builders like ceramides, and then seal with something more occlusive if you are flaking. If you are itchy or eczema-prone, fragrance-free products tend to sting less during period week. Patch-test new products on a small area for 2–3 days before using them all over.
When should I worry about dry skin during my period?
Get checked sooner if you have painful cracks, spreading redness, oozing, or honey-colored crust, because broken skin can get infected. It is also worth medical attention if dryness comes with symptoms of hypothyroidism such as constipation and feeling cold, or if you have heavy periods and significant fatigue that could point to low ferritin. Bring a quick timeline of when dryness peaks in your cycle and what products you use so the visit is more productive.
What the research says
American Academy of Dermatology guidance on dry skin and eczema care (bathing, moisturizers, and triggers)
Systematic review: vitamin D supplementation for atopic dermatitis severity (mixed but clinically relevant results)
Review: estrogen and skin aging/barrier changes, explaining why low-estrogen states can feel drier