Hair Thinning During Menopause: What’s Causing It and What Helps
Hair thinning during menopause often comes from lower estrogen, relative androgen effects, or thyroid/iron issues. Targeted labs available—no referral needed.
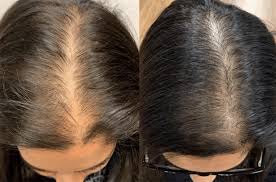
Hair thinning during menopause usually happens because estrogen drops, which shortens your hair’s growth phase and makes follicles more sensitive to androgens (the “more male-leaning” hormones). It can also be triggered or worsened by low iron stores or thyroid changes, which are both common in midlife and very treatable once you spot them. A few targeted blood tests can help you figure out which pattern fits your body so you’re not guessing. This symptom is frustrating because it’s often gradual at first, and by the time your ponytail feels smaller you’ve already lost a lot of density. The good news is that many causes are modifiable, and even when genetics plays a role you can often slow the process and regrow some thickness with the right plan. In this guide, you’ll learn the most common menopause-related reasons hair thins, what actually helps (and what tends to waste time), and which labs can clarify the story. If you want help connecting your specific pattern to next steps, PocketMD can talk it through, and Vitals Vault labs can help you confirm the “why” with real numbers.
Why your hair thins during menopause
Estrogen drops, growth phase shortens
Estrogen helps keep more of your hairs in the active growth phase, so when it falls in perimenopause and after menopause, more hairs shift into the shedding phase sooner. That can look like a widening part, less volume at the crown, or hair that just will not reach the length it used to. If your thinning started around cycle changes, hot flashes, or sleep disruption, this hormone shift is a common backdrop, and it’s worth treating the hair directly rather than waiting for it to “settle.”
Follicles become androgen-sensitive
Even if your testosterone does not rise, the balance changes when estrogen declines, and your follicles may react more strongly to androgens. This is the classic pattern of female pattern hair loss [androgenetic alopecia], which often shows up as thinning on the top of your scalp while the hairline stays mostly intact. The takeaway is that early treatment matters because follicles miniaturize over time, which means acting now can preserve density you cannot easily “make back” later.
Low iron stores (low ferritin)
Your body can have “normal” hemoglobin while your iron reserves are low, and hair follicles are one of the first places that feels the shortage. Low ferritin often shows up as diffuse shedding, brittle strands, and hair that breaks easily, especially if you also feel more tired than usual. Ask specifically for ferritin, and if it is low, work with a clinician on iron repletion and a plan to look for the reason it dropped in the first place.
Thyroid slowdown affects follicles
When your thyroid is underactive, your whole metabolism slows down, and hair growth can become sparse, dry, and more prone to shedding. This can overlap with menopause symptoms like fatigue, constipation, and feeling cold, which is why it gets missed. A simple TSH plus free T4 can quickly tell you whether thyroid function might be part of your hair story.
Stress shedding after a body shift
Big stressors, illness, rapid weight loss, surgery, or even months of poor sleep can push hairs into a synchronized shed called stress shedding [telogen effluvium]. The key clue is timing: shedding often starts about 2–3 months after the trigger, and you may notice lots of hair in the shower or on your brush rather than a specific thinning pattern. If this sounds like you, the most helpful move is to identify and correct the trigger while you protect your scalp and avoid harsh styling, because the follicles usually recover with time.
What actually helps hair thinning
Use topical minoxidil consistently
Topical minoxidil is one of the best-studied options for female pattern thinning, and it works by keeping follicles in the growth phase longer. The hard part is patience: shedding can look worse in the first 2–8 weeks, and visible improvement usually takes 3–6 months. Pick a routine you can stick to, apply it to the scalp (not the hair), and take monthly photos in the same lighting so you can see progress you might miss day to day.
Correct low ferritin on purpose
If ferritin is low, “more spinach” rarely fixes it fast enough to help your hair. Iron repletion typically means a structured supplement plan and follow-up labs, because too little does nothing and too much can cause side effects and is not safe for everyone. A practical goal many clinicians use for hair is ferritin at least around 50–70 ng/mL, but your best target depends on your symptoms and why your iron is low.
Treat thyroid issues, if present
If labs suggest hypothyroidism, treating it can reduce shedding and improve hair texture, but it is not instant because hair cycles are slow. Many people notice less shedding first, and density follows over months as new hairs grow in. The key is follow-up testing after medication changes so you are not stuck in the “almost treated” zone where symptoms linger.
Protect your scalp and strands
Menopause can make your scalp drier and more sensitive, which means inflammation and breakage can add to the appearance of thinning. Gentle handling matters: avoid tight ponytails, reduce heat styling, and ask your stylist for a cut that builds the illusion of density while you treat the root cause. If you have itching, scale, or burning, treating the scalp condition can make regrowth efforts work better.
Ask about prescription options
If your pattern looks androgen-driven, a clinician may discuss anti-androgen approaches such as spironolactone, or other prescription strategies depending on your health history. These can be especially helpful when minoxidil alone is not enough, but they require individualized risk-benefit decisions and monitoring. Bring a clear timeline, photos, and any relevant labs to that visit so the plan is based on your actual pattern, not guesswork.
Useful biomarkers to discuss with your clinician
Ferritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreTSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreEstradiol
Estradiol in men is produced from testosterone via aromatase enzyme. In functional medicine, we recognize that men need optimal estradiol levels for bone health, cognitive function, and cardiovascular protection. However, excessive estradiol can suppress testosterone production and cause feminizing effects. The testosterone-to-estradiol ratio is crucial for male health, with optimal balance supporting vitality while preventing estrogen dominance. Balanced estradiol levels in men support bone health and cognitive…
Learn moreLab testing
Check ferritin, TSH, and free T4 at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a simple “part and ponytail” baseline today: take a photo of your part from above and measure your ponytail circumference with a soft tape. Repeat monthly in the same lighting so you can tell true change from a bad hair day.
If you start minoxidil, set a 6-month expectation and track shedding weekly, not daily. Hair cycles are slow, and the early shed is often a sign follicles are switching gears rather than a sign you are “losing more.”
Treat your scalp like skin, not like hair: if you have itch, flaking, or tenderness, address that first with a clinician or dermatologist because inflammation can sabotage regrowth efforts.
If you suspect low iron, ask for ferritin specifically and recheck it after 8–12 weeks of a plan. Hair improvement usually follows the lab trend with a delay, so the repeat number keeps you from quitting too early.
Bring photos and a timeline to appointments, including when your periods changed and when shedding began. That one page of notes often saves you months of trial-and-error because it helps identify stress shedding versus pattern thinning.
Frequently Asked Questions
Does menopause cause hair thinning, or is it just aging?
Menopause can directly contribute because lower estrogen shortens the hair growth phase and can make follicles more sensitive to androgens. Aging also plays a role, but the timing around cycle changes, hot flashes, or sleep disruption often points to the menopause transition as a trigger. If you want a clearer answer, checking ferritin and thyroid labs (TSH and free T4) can identify common treatable contributors.
How do I know if it’s female pattern hair loss or stress shedding?
Female pattern hair loss usually shows up as gradual thinning on the top of your scalp with a widening part, while stress shedding tends to be sudden, diffuse, and heavy in the shower or brush. Stress shedding often starts about 2–3 months after a trigger like illness, major stress, or rapid weight loss. Taking monthly scalp photos from the same angle can make the pattern much easier to spot.
What ferritin level is too low for hair growth?
Many people with hair shedding feel better when ferritin is at least around 50–70 ng/mL, even if the lab’s “normal” range starts lower. If your ferritin is below that and you are shedding, it is a strong clue that iron stores may be limiting regrowth. Ask your clinician for an iron plan and a repeat ferritin in 8–12 weeks so you can confirm it is actually rising.
How long does it take for hair to grow back after menopause hair loss?
If the trigger is correctable, like low ferritin or hypothyroidism, you may notice less shedding in 6–12 weeks, but visible thickness usually takes 3–6 months or longer. With female pattern hair loss, the goal is often slowing progression and regaining some density, which is why consistent treatment matters. Take monthly photos so you can see changes that are too subtle week to week.
Should I get hormone tests for menopause hair thinning?
Hormone shifts are part of the story, but hormone tests do not always change the plan because levels fluctuate and “normal” does not rule out menopause-related thinning. In many cases, ferritin and thyroid tests (TSH and free T4) are more actionable because they identify common treatable drivers of shedding. If you have signs of high androgens like new facial hair or acne, bring that up because it can change what your clinician considers.
What the research says about menopause-related hair thinning
North American Menopause Society position statement on hormone therapy (context for menopause symptoms and individualized treatment decisions)
Female pattern hair loss review (pathophysiology and treatment options, including minoxidil and anti-androgen approaches)
Telogen effluvium review (timing after stressors and expected recovery pattern)