Why Do You Get Dry Skin After Eating?
Dry skin after eating often comes from food-triggered eczema, dehydration from salty meals, or thyroid and iron issues. Targeted labs, no referral needed.
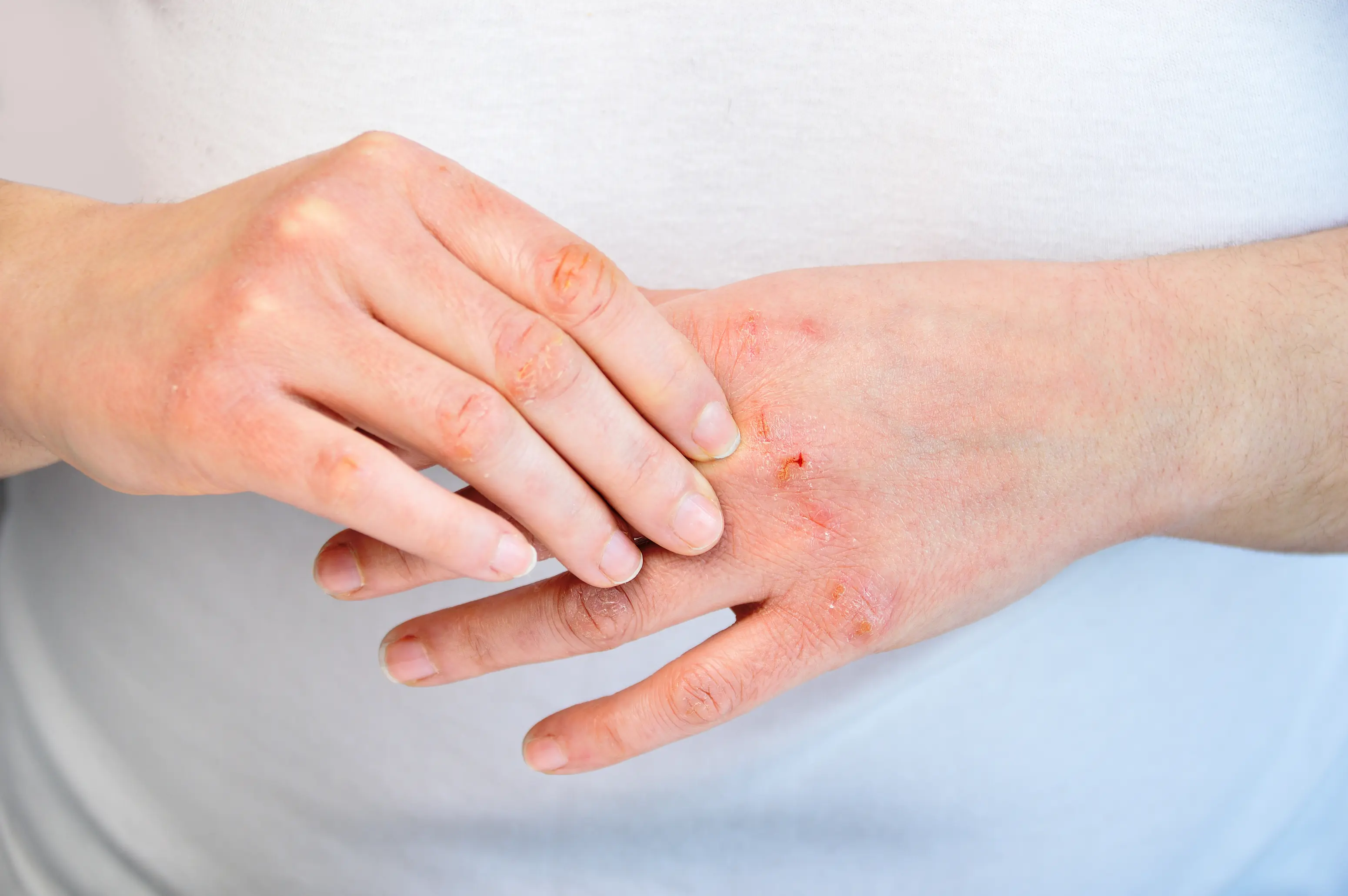
Dry skin after eating usually means one of three things is happening: a food-triggered skin flare such as eczema, a temporary dehydration effect from what you ate or drank, or an underlying issue like low thyroid or low iron that shows up more when your body shifts blood flow to digestion. The pattern matters, because dryness that starts within minutes points to a trigger, while dryness that builds over hours to days is more often a baseline skin-barrier problem. A few targeted labs can help you sort out which bucket you’re in. This symptom is frustrating because it feels “random,” especially when you’re already moisturizing. But your skin is not separate from your gut, hormones, and immune system. Meals change your blood sugar, stress hormones, fluid balance, and inflammatory signals, and your skin can be the first place you notice it. If you want help connecting your timing and triggers, PocketMD can walk through your story with you, and Vitals Vault labs can help confirm common internal contributors.
Why Do You Get Dry Skin After Eating?
Food-triggered eczema flare
If you already have sensitive skin, certain foods can nudge your immune system into an eczema flare, which makes your skin barrier leak water faster. You might notice itching first, then rough patches on your hands, eyelids, or inside elbows later that day. The most useful takeaway is timing: if dryness or itch reliably follows specific meals, a short elimination-and-rechallenge plan is often more revealing than guessing forever.
Histamine reaction after meals
Some meals are naturally high in histamine, and some people break histamine down more slowly, which can make your skin feel tight, itchy, or “prickly” soon after eating. This can look like flushing, hives, or just a sudden dry, irritated feeling around your face and neck. If symptoms start within 15–60 minutes, try simplifying one meal a day for a week and see whether leftovers, fermented foods, or alcohol are the consistent spark.
Salty meals pulling fluid away
A very salty meal can temporarily shift fluid balance, and if you are already a little under-hydrated, your skin can feel drier and less elastic afterward. This is not just about drinking more water, because your body also needs enough potassium and overall fluid across the day to keep skin cells plump. The clue is that your mouth feels dry too, and the “dry skin after eating” is strongest after takeout, soups, cured meats, or snack foods.
Blood sugar swings drying you out
Big blood sugar spikes can increase urination later and can also amplify inflammation, which tends to make skin feel more reactive. You might notice a crash a couple of hours after a carb-heavy meal along with thirst, dry lips, or itch that feels out of proportion to what you see. If this sounds like you, pairing carbs with protein and fiber at the same meal is a practical experiment that often changes the pattern within a week.
Low thyroid slowing skin turnover
An underactive thyroid [hypothyroidism] slows how quickly your skin renews itself and reduces oil and sweat production, so your baseline dryness is higher and meals can make it more noticeable. People often describe rough, flaky skin on shins and forearms, plus fatigue, constipation, or feeling cold. If dryness is persistent and not just tied to one food, checking a TSH is a straightforward way to rule this in or out.
What Actually Helps After Meals
Do a 2-week trigger timeline
Write down what you ate and when dryness starts, because “right after eating” can mean 10 minutes or 6 hours, and those are different problems. Add one extra detail that matters: whether you also had itch, flushing, or stomach symptoms. After about 10–14 days, you usually see a small set of repeat offenders, which makes your next step targeted instead of restrictive.
Build a skin-barrier routine
If your skin barrier is leaky, food triggers hit harder, so the goal is to seal in water before you chase every ingredient. Use a thick, fragrance-free moisturizer within three minutes after washing, and choose an ointment on the worst spots at night because it slows water loss better than lotion. This is especially helpful if your dryness is patchy and you can feel roughness even on “good food” days.
Try a low-histamine meal reset
If symptoms start quickly after eating and you also flush, get headaches, or feel congested, a short low-histamine trial can be informative. For five to seven days, lean on freshly cooked proteins, rice or potatoes, and simple vegetables, and avoid leftovers and fermented foods because histamine builds with storage. If your skin calms down, you can reintroduce one food at a time to find your personal threshold.
Change the meal’s salt-to-potassium balance
When salty meals are the trigger, the fix is often adjusting the meal, not just chugging water afterward. Add potassium-rich sides like beans, leafy greens, or a baked potato, and aim to spread salty foods across the week instead of stacking them in one day. If you have kidney disease or take potassium-affecting medications, check with your clinician before intentionally increasing potassium.
Treat the internal driver you find
If labs show low ferritin or thyroid issues, topical care alone usually feels like pushing a boulder uphill. Iron deficiency is often treated with iron plus a plan to find the cause, while hypothyroidism is treated with thyroid hormone under clinician guidance. Once the internal issue is corrected, many people notice their skin holds moisture better and flares become less frequent.
Useful biomarkers to discuss with your clinician
TSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreIron, Total
Serum iron measures the amount of iron circulating in your blood at the time of testing. In functional medicine, we recognize that serum iron alone provides limited information about iron status, as it fluctuates throughout the day and is affected by recent iron intake, inflammation, and diurnal variation. However, when combined with other iron studies, it helps assess iron metabolism and transport. Iron is essential for oxygen transport, energy production, DNA synthesis, and immune function. Optimal serum iron…
Learn morePotassium
Potassium is the primary intracellular electrolyte crucial for muscle function, nerve transmission, and cardiovascular health. In functional medicine, potassium deficiency is extremely common due to low fruit/vegetable intake and high sodium diets. Potassium supports healthy blood pressure, prevents kidney stones, and maintains bone health. Low potassium increases risk of hypertension, arrhythmias, and stroke. Optimal potassium levels support heart rhythm, muscle function, and cellular metabolism. Potassium is e…
Learn moreLab testing
Check TSH, ferritin, and a CBC at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Run a “single-variable lunch” for five days: eat the same simple lunch each day, then change just one thing (like adding tomatoes or leftovers) to see what reliably flips your skin from calm to dry.
If your dryness is worst on your hands after meals, try washing with lukewarm water and a gentle cleanser, then apply an ointment right away; frequent post-meal handwashing can be the hidden driver.
When you suspect histamine, prioritize freshness: cook once and freeze portions the same day, because histamine rises in the fridge even when food still tastes fine.
If salty meals are your trigger, weigh yourself before dinner and the next morning for a week; a consistent overnight jump can confirm fluid shifts, which makes meal composition a smarter target than more moisturizer.
Take phone photos of the same patch of skin in the same lighting on “good” and “bad” days; it helps you notice whether you’re dealing with true scaling and inflammation or mainly a tight, dehydrated feel.
Frequently Asked Questions
Why does my skin feel dry right after I eat?
When dryness starts within an hour, it is often a trigger effect rather than a slow skin condition. Histamine reactions, food-triggered eczema, and salty meals that shift fluid balance can all make your skin feel tight or itchy quickly. Track the exact start time and whether you also flush, get hives, or feel thirsty, because that pattern points to the most likely cause.
Can dehydration cause dry skin after a meal even if I drink water?
Yes, because hydration is not just the glass of water you drink at the table. Very salty meals can pull water into your bloodstream and then increase thirst and urination later, and alcohol can add to that effect. If your mouth is dry and your urine is darker after certain meals, try reducing salt at that meal and adding potassium-rich foods rather than only drinking more water.
Is dry skin after eating a sign of a food allergy?
It can be, but true food allergy usually causes fast symptoms like hives, swelling, wheezing, vomiting, or widespread itching. Dryness alone is more commonly eczema flaring or a histamine-type sensitivity. If you ever get lip or tongue swelling, trouble breathing, or feel faint after eating, treat that as urgent and seek emergency care.
What blood tests help explain dry skin and itching?
For meal-linked dryness where you also have fatigue, hair changes, or cold intolerance, TSH can screen for low thyroid, and ferritin plus a CBC can check for iron deficiency and anemia. Ferritin below about 30 ng/mL often supports iron deficiency, and a high TSH can fit with dry, rough skin. If your results are abnormal, bring them to a clinician so you can treat the cause and not just the symptom.
How long should I try eliminating a food to see if my skin improves?
For a suspected trigger, a focused 2-week trial is usually long enough to see a meaningful change in itch and flares, especially for eczema patterns. Keep the rest of your routine steady so you are not changing five things at once, and then reintroduce the food once to confirm it was real. If you are considering eliminating major food groups long-term, it is worth getting guidance so you do not create nutrient gaps.