Why Your Skin Gets Dry During Fasting (and What Helps)
Dry skin during fasting often comes from dehydration, a weakened skin barrier, or thyroid and iron issues. Targeted labs at Quest—no referral needed.
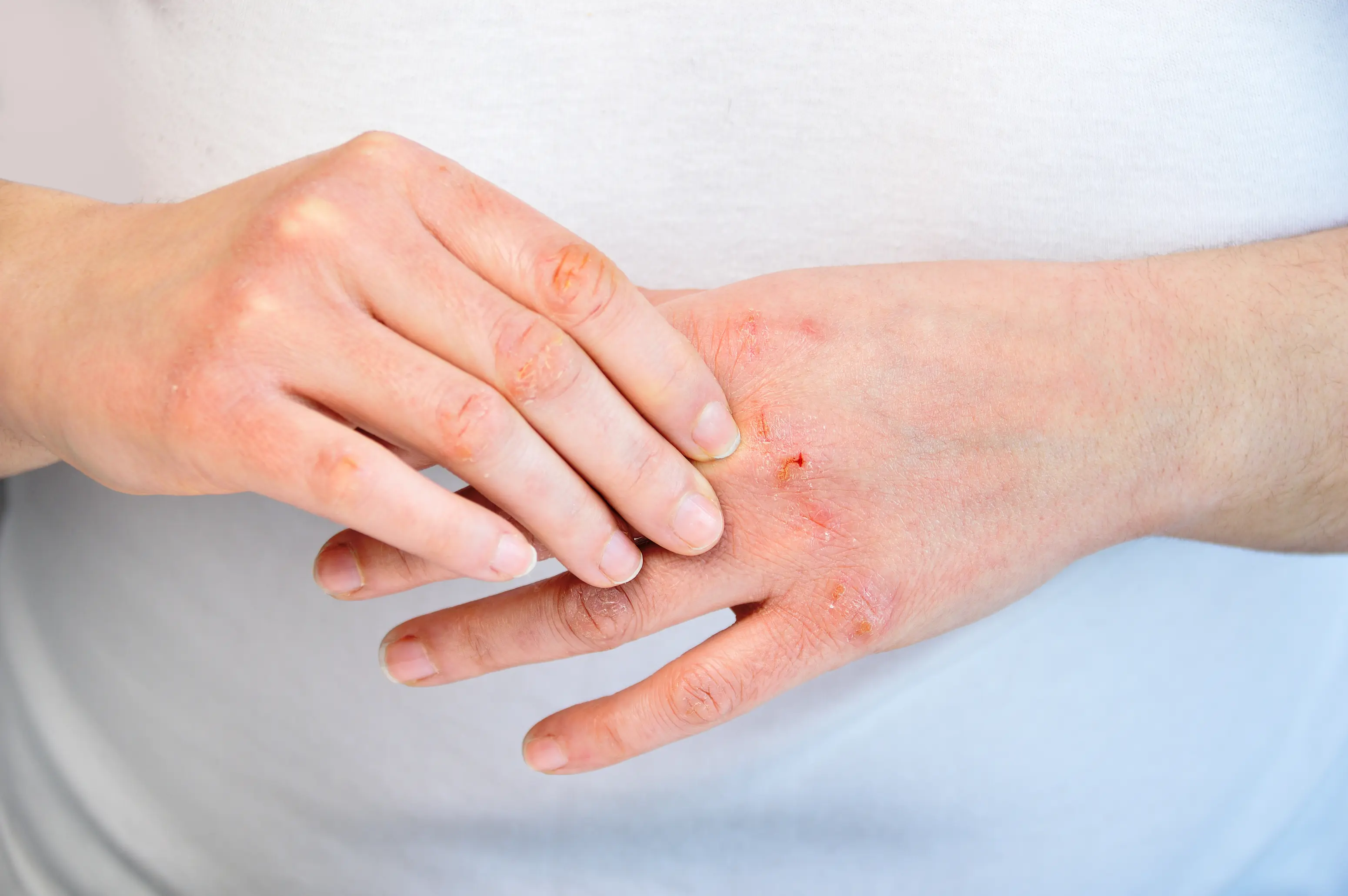
Dry skin during fasting usually happens because you are losing more water than you realize, your skin barrier is already a bit fragile, or an underlying issue like low thyroid function or low iron is making your skin less able to hold onto moisture. Fasting can also change what you eat and when, which can quietly reduce essential fats and protein your skin uses to repair itself. If it keeps happening, targeted blood tests can help you figure out which of these is driving your dryness. A lot of people expect fasting to affect energy and hunger, but skin changes can be the first clue that your body is running “tight” on fluids or building blocks. Dryness can show up as tightness after washing, flaking around the nose or mouth, or itching that feels worse at night. The good news is that most cases improve with a few specific adjustments, and if the pattern doesn’t fit, tools like PocketMD and a small set of labs through Vitals Vault can help you sort out whether this is mostly hydration, barrier care, or something internal that needs attention.
Why your skin gets dry during fasting
You’re dehydrated without noticing
When you eat less often, you often drink less often too, and you also lose some “food water” that normally comes from meals. Even mild dehydration can reduce the water content of your outer skin layer, which is why your skin can feel tight, look dull, and get fine flaking. A practical clue is darker urine or a dry mouth by late morning, so try anchoring fluids to your fasting routine instead of waiting for thirst.
Your skin barrier is already sensitive
If you have eczema-prone or easily irritated skin, fasting-related stress and dry indoor air can tip your skin barrier into a flare. A weakened barrier lets water escape faster, which is why you can moisturize and still feel itchy an hour later. Treat it like a barrier problem, not a “more lotion” problem, by using a thick, fragrance-free ointment or cream right after washing.
Electrolyte shifts make you feel “dry”
Early in fasting, your insulin drops and your kidneys release more sodium and water, which can leave you feeling a bit wrung out. That fluid shift can show up as dry lips, dry eyes, and skin that suddenly looks more crepey, especially if you also drink a lot of plain water without replacing salt. If you are otherwise healthy, adding a modest amount of sodium during longer fasts can help you feel normal again.
Low thyroid slows skin turnover
Low thyroid function (hypothyroidism) slows how quickly your skin renews itself and reduces oil production, which makes dryness stubborn and “all over,” not just on your hands. You might also notice feeling cold, constipation, or hair thinning that seems out of proportion to your fasting plan. If dryness started before fasting or persists even when you refeed, a TSH blood test is a sensible next step.
Low iron affects skin and hair
Iron deficiency can make your skin look pale and feel dry because your tissues are not getting the oxygen delivery they are used to, and your body may prioritize vital organs over skin and hair. This is especially common if fasting has reduced your overall intake, if you avoid red meat, or if you have heavy periods. Ferritin is the most useful test here because it reflects iron stores, and many people feel better when ferritin is well above the bare minimum “normal.”
What actually helps dry skin while fasting
Build a fasting hydration schedule
Instead of sipping randomly, set two or three “hydration anchors” during your fasting window, such as one large glass on waking and another mid-morning. This works because routine beats willpower, and it prevents the slow drift into dehydration that shows up as afternoon itching. If you are fasting longer than usual, check urine color as feedback and aim for pale yellow.
Use a barrier-first moisturizer routine
Moisturizer works best when it traps water, so apply it within three minutes of washing while your skin is still slightly damp. Choose a fragrance-free cream with ceramides, glycerin, or petrolatum, because those ingredients help patch the barrier and reduce water loss. If your hands crack, an ointment at night with cotton gloves can make a bigger difference than switching soaps repeatedly.
Adjust electrolytes for longer fasts
If your fasting plan includes long stretches without food, consider adding sodium in a controlled way, such as a measured electrolyte mix or a small amount of salt in water, unless you have been told to limit salt for blood pressure, heart failure, or kidney disease. The goal is not “more salt forever,” but preventing the washed-out, dry feeling that comes from sodium loss. If you get swelling, headaches that worsen, or high blood pressure readings, scale back and reassess.
Refeed with skin-building nutrients
Your skin needs protein and essential fats to repair, so a refeed that is mostly refined carbs can leave your barrier struggling even if calories are adequate. Aim for a protein-forward meal and include a source of omega-3 fats, such as salmon, sardines, chia, or walnuts, because they support the lipids that keep moisture in. If you are plant-based, make sure you are consistently hitting protein targets rather than “making it up later.”
Change the shower, not just the lotion
Hot water and long showers strip oils fast, which can make fasting-related dryness feel dramatic overnight. Keep showers warm rather than hot, limit them to about 5–10 minutes, and use a gentle cleanser only where you need it. This one change often reduces itching within a week because you stop re-injuring the barrier every day.
Useful biomarkers to discuss with your clinician
TSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreIron Binding Capacity
TIBC helps distinguish between different causes of abnormal iron levels. High TIBC indicates iron deficiency (the body increases transferrin to capture more iron), while low TIBC suggests iron overload or chronic disease. It's essential for accurate iron status assessment. Total Iron Binding Capacity (TIBC) measures the blood's capacity to bind iron with transferrin, the main iron transport protein. It indirectly reflects transferrin levels and iron status.
Learn moreFerritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreLab testing
Check TSH, ferritin, and a CMP (electrolytes and kidney markers) at Quest—starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a 7-day “tightness check” to see if dehydration is the main driver: take a photo of the same patch of skin each morning, and note urine color and how many times you refilled your bottle. Patterns show up fast when you track them simply.
If your face feels dry but also stings when you moisturize, stop actives for two weeks. That means no retinoids, no exfoliating acids, and no fragranced products, because irritated skin needs quiet to rebuild.
For fasting days, keep a small tube of petrolatum-based ointment for lips and the corners of your nose. Those areas lose water quickly, and protecting them prevents the “snowplow” cycle of licking and cracking.
If you live in a dry climate or heat your home, run a humidifier in your bedroom and aim for about 40–50% humidity. Your skin loses less water overnight, which is why morning tightness often improves first.
If dryness comes with dizziness, pounding heart, or muscle cramps during longer fasts, treat that as a signal to adjust fluids and electrolytes rather than pushing through. Your skin is often the early warning light.
Frequently Asked Questions
Is dry skin a sign you’re dehydrated while fasting?
Often, yes—especially if your skin feels tight by afternoon and you also notice darker urine or a dry mouth. Fasting can reduce both your fluid intake and the water you normally get from food, so mild dehydration sneaks up. Try scheduled fluids during the fasting window and reassess after three days.
Can intermittent fasting make eczema worse?
It can, because stress hormones and dry indoor air can weaken your skin barrier, and a weakened barrier loses water faster and itches more. The fix is usually barrier care: short warm showers, gentle cleanser, and a thick fragrance-free cream or ointment applied right after washing. If you are flaring, pause irritating actives and focus on repair for two weeks.
Why is my skin dry even though I’m drinking water?
If you drink a lot of plain water during longer fasts but you are losing sodium through your kidneys, you can still feel “dry” and washed out. That is why some people improve with a measured electrolyte approach rather than more water alone. If you have high blood pressure, kidney disease, or heart failure, check with a clinician before increasing sodium.
What vitamin deficiency causes dry skin during fasting?
Low iron is a common one during calorie restriction, and it can show up as dry skin along with brittle nails, fatigue, or hair shedding. Ferritin is the key blood test because it reflects iron stores, and symptoms are more likely when ferritin is under about 30 ng/mL. If your diet has changed with fasting, it is also worth checking whether you are consistently getting enough protein and essential fats at refeed meals.
When should I get labs for dry skin during fasting?
If dryness is new, persistent for more than 2–4 weeks, or comes with fatigue, hair thinning, constipation, or feeling unusually cold, labs can save you a lot of guesswork. A focused starting set is TSH for thyroid, ferritin for iron stores, and a CMP to look at electrolytes, kidney markers, and albumin. Bring your fasting schedule and symptoms to the conversation so results are interpreted in context.