Swelling in Pregnancy: What’s Normal, What’s Not
Swelling in pregnant women usually comes from fluid shifts, vein pressure, or preeclampsia. Spot red flags and get targeted labs at Quest—no referral needed.
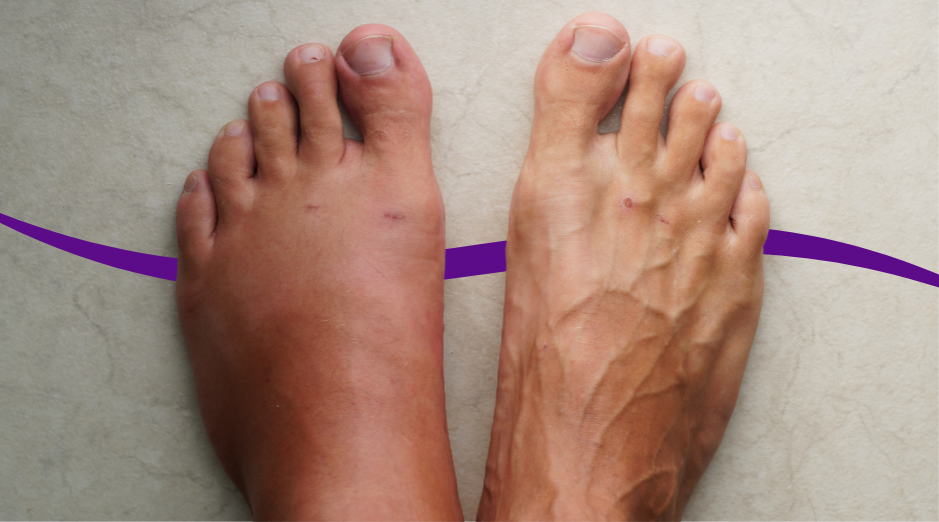
Swelling in pregnancy is usually caused by normal fluid retention, slower blood return from your legs because your uterus presses on veins, and hormonal changes that make you hold onto salt and water. But swelling can also be a warning sign when it comes on suddenly, affects your face or hands, or shows up with high blood pressure, which can point to preeclampsia. A few targeted checks and labs can help clarify which situation you’re in. Most people notice puffier ankles and feet as pregnancy progresses, especially after standing, traveling, or being out in the heat. That “end of day” swelling is common and often uncomfortable, but it is not automatically dangerous. The tricky part is that the same symptom can also show up with blood pressure problems, kidney strain, or a blood clot, which is why location, timing, and associated symptoms matter. If you want help thinking through your pattern, PocketMD can walk you through the right questions, and Vitals Vault labs can support your clinician with objective data when testing makes sense.
Why swelling happens during pregnancy
Normal fluid retention and hormones
During pregnancy, your body expands its blood and fluid volume to support the placenta and your baby, and your hormones also make you retain more salt and water. That extra fluid tends to settle in your feet and ankles by evening, which is why shoes can suddenly feel tight. If the swelling improves overnight and is worse after long standing, it often fits this normal pattern, and simple positioning changes can make a noticeable difference.
Vein pressure from your uterus
As your uterus grows, it can compress the large veins that carry blood back from your legs, so fluid leaks into nearby tissues and your calves and ankles look puffy. You might notice it more on days you sit a lot, like at a desk or in the car, because your calf muscles are not “pumping” blood upward. Taking short walking breaks and lying on your left side can reduce that pressure and help fluid move back toward your heart.
Preeclampsia (blood pressure complication)
Preeclampsia is a pregnancy-specific condition where blood vessels and the placenta don’t interact normally, which can raise your blood pressure and stress your kidneys. The swelling that worries clinicians is often sudden, involves your face or hands, or comes with headaches, vision changes, right-upper-belly pain, or shortness of breath. If you have those symptoms or your home blood pressure is at or above 140/90, call your obstetric team the same day, because early treatment lowers risk for you and your baby.
Kidney strain or protein loss
Your kidneys work harder in pregnancy, and if they are irritated by infection or underlying kidney disease, you can retain fluid or leak protein into urine. That can show up as more generalized swelling, including around your eyes in the morning, or swelling that does not improve with rest. A urine protein/creatinine ratio and a creatinine/eGFR blood test can quickly tell whether your kidneys are under unusual stress.
A blood clot in one leg
Pregnancy makes your blood more likely to clot, which is protective during delivery but increases the risk of a deep vein clot (deep vein thrombosis). This swelling is usually one-sided and comes with new pain, warmth, or redness in the calf or thigh, and it does not behave like typical “end of day” puffiness. If you suspect this, it is an urgent evaluation because treatment prevents the clot from traveling to your lungs.
What actually helps pregnancy swelling (and when to get checked)
Use gravity on purpose
If your swelling is mostly in your feet and ankles, elevating your legs above heart level for 20 minutes can move fluid back into circulation faster than simply putting your feet on a stool. Lying on your left side is especially helpful because it takes pressure off major veins in your abdomen. Make it a routine after work or after errands, and you’ll often see your ankles look more like “you” again.
Wear compression the right way
Graduated compression socks can reduce leg swelling by supporting veins and limiting fluid leakage into tissues, but they work best when you put them on first thing in the morning before swelling builds. Choose a pregnancy-safe, comfortable level (often 15–20 mmHg) unless your clinician recommends stronger. If socks leave deep grooves or your toes tingle, the fit is likely wrong and you should size up.
Move your calves every hour
Your calf muscles act like a second heart for your legs, so small movements matter. If you sit or stand for long stretches, set a timer to do 1–2 minutes of ankle pumps, calf raises, or a brisk hallway walk each hour. This is especially useful on travel days, when swelling can feel dramatic by the time you arrive.
Dial back sodium without starving yourself
You do not need a “no salt” diet, but highly processed foods can push sodium high enough that your body holds onto extra water. For one week, try swapping one salty convenience meal per day for a simpler option like yogurt with fruit, eggs and toast, or a rice-and-beans bowl you can season yourself. If your swelling noticeably improves, you’ve found a lever you can control without cutting calories you need in pregnancy.
Know the red-flag pattern
Swelling is more concerning when it is sudden, involves your face or hands, or comes with headache, vision changes, chest pain, shortness of breath, or blood pressure readings at or above 140/90. Those combinations can signal preeclampsia or a clot, and they deserve same-day medical advice even if you are not sure. If you have a home cuff, write down two readings taken five minutes apart and share the numbers, because that speeds up triage.
Useful biomarkers to discuss with your clinician
Urine Protein
Proteinuria is a key marker of kidney disease and damage. It indicates glomerular or tubular dysfunction. Persistent proteinuria is associated with progressive kidney disease, cardiovascular disease, and increased mortality. Early detection allows intervention to slow progression. Urine protein testing detects the presence of protein, primarily albumin, in urine. Normal urine contains minimal protein; elevated levels indicate kidney damage or disease.
Learn moreCreatinine
Creatinine is a waste product of muscle metabolism that is filtered by the kidneys and serves as the primary marker of kidney function. In functional medicine, creatinine levels reflect not only kidney health but also muscle mass and protein metabolism. Elevated creatinine indicates reduced kidney filtration capacity, while very low levels may indicate muscle wasting or poor protein intake. Creatinine is used to calculate eGFR and helps assess long-term kidney health and detoxification capacity. Creatinine measu…
Learn moreAlbumin
Albumin is the most abundant protein in blood plasma, produced exclusively by the liver. In functional medicine, albumin serves as a marker of liver synthetic function, nutritional status, and overall health. Albumin maintains oncotic pressure (keeping fluid in blood vessels), transports hormones and nutrients, and serves as an antioxidant. Low albumin may indicate liver disease, malnutrition, chronic inflammation, or kidney disease. Since albumin has a half-life of about 20 days, it reflects longer-term nutriti…
Learn moreLab testing
Check kidney strain and preeclampsia clues with a urine protein/creatinine ratio, creatinine/eGFR, and liver enzymes — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “pitting check” once a day: press your thumb into your shin for five seconds. If a dent stays for more than a few seconds and it’s getting worse day by day, take a photo and message your obstetric team with the timeline.
If your rings feel tight, do not wait until they are stuck. Take them off at the first sign of finger swelling and store them somewhere safe, because swollen hands can escalate quickly in hot weather or after salty meals.
On travel days, plan swelling prevention like you plan snacks: wear compression socks, drink normally, and stand up or walk every hour. If you cannot walk, do ankle circles and calf squeezes for one full minute each hour.
Try a two-day experiment to learn your pattern: one day with frequent short walks and leg elevation breaks, and one day without changing anything. If your swelling is dramatically different, that points toward vein pressure and fluid pooling rather than a systemic problem.
Keep a simple home blood pressure log for a week if swelling is new: take readings at the same time daily, seated, after five minutes of rest. Bring the numbers to your next visit, because trends matter more than one isolated reading.
Frequently Asked Questions
Is swelling in pregnancy normal?
Mild swelling in your feet and ankles, especially late in the day, is very common because pregnancy increases fluid volume and slows blood return from your legs. It is more reassuring when it improves overnight and is worse after standing or heat. If swelling is sudden, involves your face or hands, or comes with headache or vision changes, get same-day advice.
When should I worry about swelling in pregnancy?
Worry less about how puffy you look and more about the pattern: sudden swelling, one-sided leg swelling with pain, or swelling plus blood pressure at or above 140/90 needs prompt evaluation. Headache that will not quit, visual “sparkles,” right-upper-belly pain, or shortness of breath are also red flags. If you have a home cuff, take two readings five minutes apart and report the numbers.
What does swelling in the hands and face mean during pregnancy?
Hands and face swelling can still be benign, but it raises the stakes because it can be seen with preeclampsia, especially when it appears quickly. The next step is usually checking your blood pressure and looking for protein in urine, often with a urine protein/creatinine ratio. If you also have headache or vision changes, call your obstetric team the same day.
How can I reduce swollen feet during pregnancy fast?
The fastest non-medication approach is leg elevation above heart level for about 20 minutes, ideally while lying on your left side. Compression socks worn in the morning can prevent the “ballooning” effect later in the day, and short walking breaks help your calves pump fluid upward. If swelling does not improve with rest or is suddenly worse, do not just push through it—get checked.
What labs are used to check for preeclampsia?
Clinicians usually combine blood pressure readings with urine protein testing, often a urine protein/creatinine ratio, and blood tests that look at kidney and liver stress such as creatinine and liver enzymes (AST/ALT). A uPCR around 0.3 or higher is commonly treated as significant proteinuria when the clinical picture fits. If you are tracking symptoms at home, write down your blood pressure numbers and the exact day swelling changed, because that context helps interpret results.
Research and guidelines behind the advice
ACOG Practice Bulletin: Gestational Hypertension and Preeclampsia (diagnosis, thresholds, and management)
NICE guideline NG133: Hypertension in pregnancy (assessment and monitoring, including proteinuria testing)
ACOG Practice Bulletin: Thromboembolism in Pregnancy (risk, symptoms, and evaluation of suspected DVT/PE)