Swelling After Birth: What It Means and What Helps
Swelling in postpartum women is usually from fluid shifts, IV fluids, or low protein, but watch for preeclampsia or clots. Targeted labs—no referral needed.
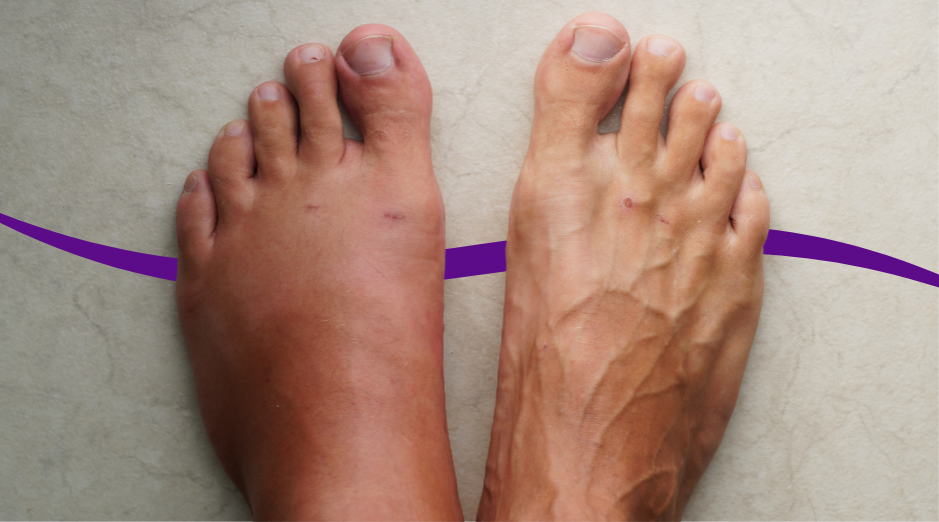
Swelling after birth is usually your body offloading extra pregnancy fluid, plus any IV fluids you received during labor, which often shows up in your feet, ankles, and hands. It can also happen when your blood protein is low or when your kidneys are under strain, and those situations tend to make swelling feel more “puffy” and persistent. Because a small number of postpartum swelling cases are tied to high blood pressure after delivery or a blood clot, targeted labs and a quick symptom check can help you sort “normal recovery” from “get checked today.” Most new moms notice swelling peak around days 2–5 after delivery and then gradually improve over 1–2 weeks, although it can linger longer after a C-section or a long labor with lots of fluids. The tricky part is that the same swollen ankles that feel like a normal postpartum nuisance can also be the first visible sign of something more serious if it comes with the wrong symptoms. This guide walks you through the most common causes, the red flags that should change your plan, and the specific blood tests that can clarify what your body is doing. If you want help matching your exact pattern of swelling to the most likely cause, PocketMD can talk it through with you, and Vitals Vault labs can help confirm what’s driving it.
Why you’re swollen after giving birth
Normal fluid shift after delivery
During pregnancy you carry extra fluid, and after birth your body has to move that fluid back into circulation so you can pee and sweat it out. While that’s happening, gravity pulls fluid into your ankles and feet, especially if you’re sitting a lot and not sleeping. If the swelling is on both sides and slowly improves day by day, it’s usually this, and gentle walking plus leg elevation tends to help.
IV fluids from labor or surgery
If you had an epidural, induction, long labor, or a C-section, you may have received a lot of IV fluid, and your tissues can hold onto it for several days. This kind of swelling often feels “tight” in your hands and face as well as your legs, and your rings and shoes suddenly don’t fit. A useful clue is timing: swelling that noticeably worsens in the first few days after delivery and then turns the corner is often IV-related.
High blood pressure after birth
Postpartum high blood pressure can show up even if your pregnancy blood pressure was fine, and it can be part of postpartum preeclampsia (a pregnancy-related blood pressure condition). Swelling alone is not enough to diagnose it, but swelling plus a new headache that won’t quit, vision changes, chest pain, or shortness of breath is a different situation. If you can, check your blood pressure today, and treat readings at or above 140/90 as a reason to call your OB or urgent care for same-day advice.
A blood clot in one leg
After delivery your blood is temporarily more likely to clot, and a clot in a deep vein (deep vein thrombosis) can cause swelling that is clearly worse on one side. It often comes with calf tenderness, warmth, or pain when you walk, and it does not improve much with elevation. If one leg is suddenly more swollen than the other, especially with pain or redness, it’s worth urgent evaluation because clots can travel to the lungs.
Low blood protein or kidney strain
Your blood protein, especially albumin, helps keep fluid inside your blood vessels, and when it’s low, fluid leaks into tissues and causes soft, pitting swelling. Kidney problems can do something similar by spilling protein into urine or by holding onto salt and water. If your swelling is persistent, more generalized (including face or hands), or paired with foamy urine or very low urine output, labs that check albumin, creatinine, and urine protein can be surprisingly clarifying.
What actually helps postpartum swelling
Elevate and compress strategically
Elevation works best when your ankles are above your heart, not just propped on an ottoman, because it gives fluid a real path back to circulation. If your swelling is mostly in your lower legs and both sides look similar, knee-high compression socks can reduce that heavy, “about to burst” feeling by the end of the day. Put them on in the morning before swelling builds, and take them off if you get numbness, worsening pain, or one-sided swelling.
Walk in short, frequent bursts
Your calf muscles act like a pump that pushes fluid back up toward your heart, and that pump is weak when you’re sitting or lying down for long stretches. A realistic goal is a 5–10 minute walk a few times a day, even if it’s just around your home, because consistency matters more than intensity. If walking makes one calf hurt or swell more, pause and get checked rather than pushing through.
Dial back sodium for one week
Salt makes your body hold onto water, and postpartum swelling is one of the few times when a short, focused sodium cut can make a noticeable difference quickly. For a week, aim to avoid the obvious high-salt foods like soups, deli meats, fast food, and salty snacks, and taste your food before salting it. You’re not trying to “detox,” you’re just making it easier for your kidneys to let go of the extra fluid.
Track blood pressure and symptoms
If you have a cuff at home, checking once in the morning and once in the evening for a few days can catch postpartum hypertension early, when it’s easier to treat. Write down the numbers along with symptoms like headache, vision changes, right-upper-belly pain, or shortness of breath, because that combination is what clinicians use to judge urgency. If you repeatedly see 140/90 or higher, call your OB office the same day even if you feel “mostly fine.”
Get labs if swelling isn’t improving
If you’re 10–14 days postpartum and swelling is not clearly trending down, or it’s spreading to your face and hands, it’s reasonable to look for a fixable driver. Kidney function (creatinine), liver enzymes, and urine protein can help separate “slow recovery” from kidney strain or postpartum preeclampsia patterns. Having objective results also makes it easier to advocate for yourself if you’re being told it’s “just normal.”
Lab tests that help explain swelling in postpartum women
Protein, Total
Total protein levels reflect nutritional status, liver function (protein synthesis), and kidney function (protein retention). Abnormal levels can indicate liver disease, kidney disease, malnutrition, inflammation, or blood cancers. It provides a general overview of protein metabolism. Total protein measures the combined amount of albumin and globulins in blood. These proteins are essential for maintaining fluid balance, transporting substances, fighting infections, and blood clotting.
Learn moreSodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreHemoglobin
Hemoglobin is the iron-containing protein in red blood cells that actually carries oxygen throughout your body. In functional medicine, hemoglobin is considered one of the most important markers of oxygen-carrying capacity and overall vitality. Low hemoglobin (anemia) significantly impacts energy levels, cognitive function, exercise tolerance, and quality of life. Even mild decreases can cause fatigue and reduced performance. Hemoglobin levels are influenced by iron status, vitamin B12, folate, protein intake, a…
Learn moreLab testing
Check kidney function, liver enzymes, and urine protein at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “one-leg check” once a day: look at both calves and ankles side by side, then press your thumb into each shin for 5 seconds. If one side is clearly more swollen, warmer, or painful, treat that as a same-day call or urgent visit rather than a wait-and-see problem.
If your shoes suddenly don’t fit, switch to supportive slides or sneakers with room and wear compression socks for the first half of the day. You’ll often prevent the late-afternoon swelling spike that makes your feet throb at bedtime.
Set a timer to elevate your legs for 15 minutes after feeds or pumping sessions. Tying elevation to something you already do makes it far more likely you’ll actually get enough “above heart level” time to notice a difference.
If you have a home blood pressure cuff, take two readings one minute apart and write down the lower number, not the higher one. Bring that log to your postpartum visit, because patterns matter more than a single scary reading.
When swelling is bothering your hands, run cool (not ice-cold) water over them for 30–60 seconds and then gently open and close your fists for a minute. It sounds simple, but it can reduce that stiff, sausage-finger feeling enough to make daily tasks easier.
Frequently Asked Questions
How long does postpartum swelling last?
For many people, swelling peaks around days 2–5 after delivery and improves over 1–2 weeks as your body sheds extra fluid. It can last longer if you had a C-section, lots of IV fluids, or limited mobility. If you’re past two weeks and it is not clearly improving, consider checking blood pressure and labs like creatinine, albumin, and urine protein.
Is swelling after a C-section normal?
Yes, swelling is common after a C-section because surgery, inflammation, and IV fluids all encourage your tissues to hold onto water for a while. You should still see a gradual downward trend over the next 1–2 weeks, even if it’s slow. If swelling is getting worse, becomes one-sided, or comes with shortness of breath or chest pain, get evaluated urgently.
When should I worry about postpartum swelling?
Worry less about mild, two-sided ankle swelling and more about swelling with warning symptoms. Call or seek same-day care if you have blood pressure readings at or above 140/90, a severe headache, vision changes, right-upper-belly pain, or sudden shortness of breath. Also get urgent evaluation if one leg is much more swollen or painful than the other, because that can signal a clot.
Can postpartum swelling be a sign of preeclampsia?
It can be, especially when swelling is paired with high blood pressure and symptoms like headache, vision changes, or nausea and upper abdominal pain. A urine protein-to-creatinine ratio and kidney and liver labs are commonly used to support the diagnosis, along with your blood pressure readings. If you suspect this, don’t wait for your routine postpartum visit—message or call your OB team today.
What labs help explain postpartum swelling?
Three useful starting tests are creatinine with eGFR (kidney filtration), albumin (blood protein that holds fluid in your bloodstream), and a urine protein-to-creatinine ratio (protein loss that can happen with postpartum preeclampsia or kidney issues). Abnormal results help explain why swelling is persistent or generalized rather than just in your feet. If you get results, bring them to your clinician so they can interpret them in the context of your delivery and blood pressure.
