Swelling in Your 60s: What It Means and What Helps
Swelling in your 60s often comes from fluid pooling in leg veins, heart strain, or kidney issues. Targeted blood tests available—no referral needed.
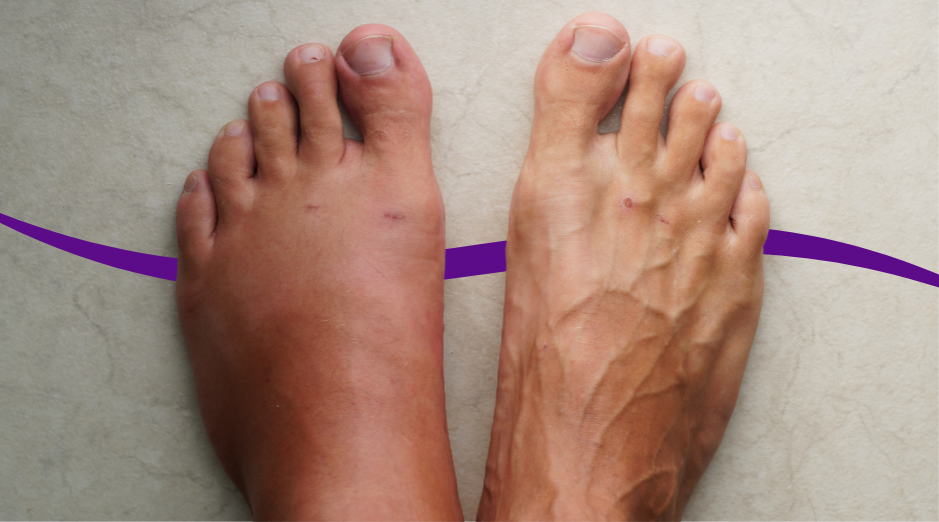
Swelling in your 60s is usually your body holding onto extra fluid or letting it pool where gravity pulls it, most often in your ankles, feet, or lower legs. Common reasons include aging veins that don’t push blood back up efficiently, heart strain that raises pressure in your leg vessels, or kidneys that are not filtering salt and water as well as they used to. A few targeted labs can help sort out which one fits your situation so you are not guessing. Swelling can be annoying in a very practical way because shoes stop fitting and rings feel tight, but it can also be your body’s early warning light. The tricky part is that “puffy” can mean several different things depending on where it is, how fast it showed up, and what else you feel with it. This guide walks you through the most common causes in your 60s, what helps at home, and which blood tests are most useful. If you want help connecting your exact pattern of swelling to the most likely cause, PocketMD can talk it through with you, and VitalsVault labs can help confirm what your body is doing.
Why swelling shows up in your 60s
Leg veins get leaky and slow
As you get older, the one-way valves in your leg veins can weaken, so blood and fluid drift downward and linger instead of moving back up toward your heart. That extra pressure pushes fluid into the tissues, which is why your ankles look puffy at the end of the day and feel better after a night in bed. A simple clue is timing: swelling that worsens with standing or sitting and improves with elevation often points to vein-related pooling.
Heart strain backs fluid up
When your heart is not pumping as strongly, pressure builds in the veins and your body holds onto salt and water to “protect” circulation, which unfortunately makes swelling worse. You might notice shoes getting tighter along with shortness of breath when walking, needing more pillows at night, or sudden weight gain over a few days. If swelling is new and you also feel breathless, that combination deserves prompt medical attention because it can signal worsening heart failure.
Kidneys hold onto salt and water
Your kidneys act like a filter and a thermostat for fluid balance, and when they are under stress they may keep more sodium and water than you need. That can show up as swelling in your legs, puffiness around your eyes in the morning, or higher blood pressure than usual. The practical takeaway is that “just drink less water” is rarely the fix; what matters more is whether your kidneys are clearing sodium and whether a medication adjustment is needed.
Low blood protein from liver or urine
Protein in your blood, especially albumin, helps keep fluid inside your blood vessels, and when it drops, fluid slips into tissues more easily. Albumin can be low if your liver is not making enough, or if your kidneys are leaking protein into urine, and either way swelling can look more generalized and stubborn. If you have swelling plus new fatigue, poor appetite, or foamy urine, ask specifically about checking albumin and kidney leakage rather than assuming it is “just aging.”
Medication-related fluid retention
Some common medications in your 60s can cause swelling by relaxing blood vessels, changing kidney salt handling, or triggering inflammation in the tissues. Calcium channel blood pressure medicines, anti-inflammatory pain relievers, steroids, and some diabetes drugs are frequent culprits, and the swelling often starts within days to weeks of a change. Bring your full medication list to your clinician and ask, “Could any of these be causing edema?” because switching within the same drug class can sometimes solve the problem.
What actually helps swelling (and when to get help)
Use elevation like a real tool
For gravity-driven swelling, “put your feet up” only works if your ankles are above the level of your heart for long enough to drain fluid. Try 20–30 minutes once or twice daily with your calves supported, and notice whether your sock marks fade afterward. If elevation does nothing at all, that is a useful clue that the cause may be more systemic, such as heart, kidney, or low albumin.
Try compression the right way
Graduated compression socks can reduce leg swelling by giving your veins a gentle squeeze so fluid does not pool as easily. They work best when you put them on in the morning before swelling builds, and they should feel snug but not painful or numb. If you have known peripheral artery disease or severe leg pain with walking, ask before using strong compression because circulation problems change the safest approach.
Do a 7-day sodium experiment
If your swelling is partly salt-driven, you can often see a difference in a week by cutting the biggest sources, which are usually packaged foods and restaurant meals rather than the salt shaker. Aim for roughly 1,500–2,000 mg sodium per day for seven days, and track morning weight and ankle tightness to see if you respond. A clear response tells you your kidneys and hormones are sensitive to sodium right now, which helps guide longer-term choices.
Review meds and timing with your clinician
If swelling started after a new prescription or a dose change, the most effective “treatment” can be adjusting that medication rather than adding more pills. Ask whether a blood pressure medicine swap is reasonable, whether an anti-inflammatory can be reduced, or whether a diuretic is appropriate for your situation. Bring a simple timeline of when swelling began and what changed around that time, because it makes the conversation much faster and more accurate.
Know the red flags for urgent care
One-sided leg swelling with pain, warmth, or redness can be a blood clot (deep vein thrombosis), especially if it came on suddenly or after travel or surgery. Swelling with chest pain, coughing blood, or sudden shortness of breath is an emergency because it can signal a clot in the lungs. New swelling plus rapidly worsening breathlessness, confusion, or fainting also deserves urgent evaluation, even if you are not sure what is causing it.
Lab tests that help explain swelling in your 60s
Albumin
Albumin is the most abundant protein in blood plasma, produced exclusively by the liver. In functional medicine, albumin serves as a marker of liver synthetic function, nutritional status, and overall health. Albumin maintains oncotic pressure (keeping fluid in blood vessels), transports hormones and nutrients, and serves as an antioxidant. Low albumin may indicate liver disease, malnutrition, chronic inflammation, or kidney disease. Since albumin has a half-life of about 20 days, it reflects longer-term nutriti…
Learn moreCreatinine
Creatinine is a waste product of muscle metabolism that is filtered by the kidneys and serves as the primary marker of kidney function. In functional medicine, creatinine levels reflect not only kidney health but also muscle mass and protein metabolism. Elevated creatinine indicates reduced kidney filtration capacity, while very low levels may indicate muscle wasting or poor protein intake. Creatinine is used to calculate eGFR and helps assess long-term kidney health and detoxification capacity. Creatinine measu…
Learn moreSodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreLab testing
Check kidney function, liver protein, and thyroid in one go — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “morning vs evening” check for three days: take a photo of your ankles when you wake up and again before bed. Swelling that builds through the day strongly suggests gravity and vein pooling, which responds best to compression and elevation.
Press your thumb into the swollen area for five seconds and then release. If a dent stays for a while, that is “pitting swelling,” which often points to fluid overload rather than inflammation, and it is worth discussing heart, kidney, and medication causes.
Weigh yourself after you pee, before breakfast, in similar clothing for a week. A gain of about 2–3 pounds in 24 hours or 5 pounds in a week can be a fluid shift, not fat, and it is a useful number to report to your clinician.
If your shoes only fit after lunch, set a phone reminder to walk for five minutes every hour you are sitting. Calf muscles act like a pump for your veins, and frequent short walks can reduce pooling more than one long walk at the end of the day.
If you are trying compression socks, start with a moderate level and focus on comfort and consistency rather than the tightest option. If your toes tingle, turn pale, or feel cold, take them off and ask for guidance because fit and circulation matter.
Frequently Asked Questions
Is ankle swelling in your 60s normal?
It is common, but “common” is not the same as “nothing.” Mild swelling that worsens after standing and improves overnight often comes from vein pooling, but new or rapidly worsening swelling can signal heart strain, kidney issues, or a medication effect. Track whether it is one-sided or both-sided and whether it improves with elevation, and bring that pattern to your clinician.
When is swelling an emergency?
Go urgently if you have sudden one-leg swelling with pain, warmth, or redness because that can be a blood clot. Swelling with chest pain, coughing blood, or sudden shortness of breath is an emergency. If you have new swelling plus rapidly worsening breathlessness or fainting, do not wait it out—get evaluated the same day.
Why is my swelling worse at night?
Gravity is usually the reason: fluid slowly pools in your lower legs while you sit or stand, so the swelling peaks by evening. That pattern often improves with 20–30 minutes of leg elevation above heart level and with compression socks put on in the morning. If swelling is worse at night and you also feel more short of breath when lying down, ask about heart-related fluid overload.
What blood tests are most useful for swelling?
A comprehensive metabolic panel (CMP) helps assess kidney function and electrolytes that affect fluid balance, while albumin helps identify low blood protein that can drive swelling. TSH screens for an underactive thyroid, which can cause a puffy look and fluid retention. If you already have heart failure symptoms, ask whether BNP or NT-proBNP testing is appropriate as well.
Can blood pressure medicine cause swelling in the feet?
Yes. Calcium channel blockers are a classic cause of ankle swelling because they widen small arteries and increase pressure in capillaries, which pushes fluid into tissues. The swelling often starts after a new prescription or dose increase and is usually worse by evening. Do not stop your medication on your own, but ask whether a dose change, a switch, or adding a balancing medication is reasonable for you.
Research and guidelines worth knowing
2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure (how clinicians evaluate and treat fluid overload)
KDIGO 2024 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease (kidney-related fluid retention and monitoring)
International Society of Lymphology consensus document on peripheral lymphedema (how chronic limb swelling is assessed and managed)