Hair Thinning in Your 60s: What It Usually Means
Hair thinning in your 60s often comes from pattern hair loss, thyroid slowdown, or low iron stores. Targeted blood tests available—no referral needed.
Hair thinning in your 60s is most often caused by age-related pattern hair loss, a thyroid slowdown, or low iron stores that quietly limit new growth. The good news is that these look and behave differently, and a few targeted labs can help you figure out which one is driving your shedding. It’s also normal to feel thrown by it. Hair changes can feel like they happen “all at once,” but your follicles work on a months-long cycle, so today’s thinning often reflects what your body was dealing with 2–4 months ago. In your 60s, that can include menopause-related hormone shifts, new medications, illness, weight changes, or stress on top of genetics. This guide helps you spot the pattern, choose realistic next steps, and use PocketMD and VitalsVault labs as tools when you want a clearer answer than guesswork.
Why your hair thins in your 60s
Age-related pattern hair loss
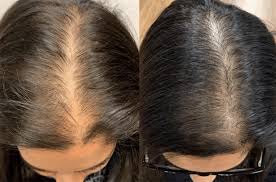
This is the most common reason, and it happens when your follicles gradually shrink and produce finer, shorter hairs over time (pattern hair loss [androgenetic alopecia]). In women, it often looks like widening part lines and less density at the crown, while men often notice recession and thinning on top. It matters because it usually won’t “bounce back” on its own, but it often responds best when you start treatment early and stick with it for months.
Thyroid slowdown affecting growth
If your thyroid is underactive, your whole hair cycle slows down, which can make hair feel dry, brittle, and thinner overall (underactive thyroid [hypothyroidism]). You might also notice constipation, feeling colder than others, puffy face, or a slower heart rate. The takeaway is simple: if thinning comes with those body-wide changes, checking a TSH blood test is one of the highest-yield steps you can take.
Low iron stores, even without anemia
Your hair follicles are fast-growing tissue, so they are sensitive when your iron “savings account” is low, even if your hemoglobin looks normal (low iron stores [low ferritin]). This often shows up as diffuse shedding, a ponytail that feels skinnier, or more hair in the shower drain. If you have a history of heavy periods earlier in life, frequent blood donation, stomach issues, or a low-meat diet, ferritin testing can explain a lot.
Vitamin D or nutrition gaps
In your 60s, it’s common to have lower vitamin D because you get less sun exposure and your skin makes it less efficiently. Low vitamin D is linked with some types of hair thinning, and it can also travel with muscle aches, low mood, or frequent infections. The practical point is not to megadose supplements blindly, but to test first and then replace to a sensible target if you’re low.
A shedding trigger 2–4 months ago
Sometimes the issue is not permanent thinning but a temporary “shedding event” where many hairs shift into the resting phase at once (stress shedding [telogen effluvium]). The trigger can be a surgery, fever, COVID, rapid weight loss, a new medication, or a major life stressor, and the timing is delayed enough that it feels mysterious. If your hair is coming out in handfuls or you can trace a clear trigger a few months back, the plan is usually to remove the trigger if possible and give regrowth time rather than chasing harsh treatments.
What actually helps hair thinning
Use topical minoxidil consistently
Minoxidil helps keep follicles in the growth phase longer, which can improve density over time, especially for pattern hair loss. The catch is that it works slowly, and you usually need 3–6 months to judge early response and closer to 9–12 months for a fuller picture. If you start, commit to a routine you can actually maintain, and expect a brief increase in shedding in the first weeks for some people because older hairs are being pushed out.
Treat thyroid issues to steady shedding
If labs show an underactive thyroid, treating it can reduce shedding and improve hair texture, although regrowth still takes months because follicles need time to cycle. What you feel day-to-day often improves before your hair does, which can be reassuring. Ask your clinician what TSH target makes sense for you, and recheck after dose changes rather than adjusting on your own.
Rebuild iron stores the right way
If ferritin is low, improving iron stores can reduce shedding and support regrowth, but it works best when you also address why you’re low in the first place. Many people tolerate iron better when they take it every other day, and taking it away from calcium can improve absorption. Recheck ferritin after a couple of months so you’re not guessing, and aim for a level that supports hair growth rather than just “barely normal.”
Protect your scalp and hair shaft
Thinning is partly about follicles, but breakage can make it look much worse, especially with gray hair that is naturally drier. Switching to gentle detangling, minimizing heat tools, and avoiding tight styles reduces mechanical loss so you keep the hair you have. If your scalp is itchy or flaky, treating dandruff can also reduce inflammation that makes shedding feel more dramatic.
See dermatology for targeted options
A dermatologist can confirm the type of hair loss with a scalp exam and sometimes a quick in-office look at the follicles, which prevents months of trial-and-error. Depending on your pattern, they may discuss prescription options such as oral minoxidil or anti-androgen approaches, or procedures like platelet-rich plasma, but the right choice depends on your health history. Go sooner if you see patchy bald spots, scalp pain, or rapid loss, because those patterns can signal treatable inflammatory causes.
Useful biomarkers to discuss with your clinician
TSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreFerritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreVitamin D, 25-Oh, Total
Total 25-hydroxyvitamin D represents the best measure of vitamin D status, combining both D2 and D3 forms. This is the storage form of vitamin D and reflects recent intake and synthesis. In functional medicine, total 25(OH)D is used to assess vitamin D sufficiency and guide supplementation. Optimal levels (40-80 ng/mL) are associated with reduced risk of cancer, cardiovascular disease, autoimmune conditions, and all-cause mortality. Vitamin D acts as a hormone affecting immune function, bone health, mood, and ce…
Learn moreLab testing
Get TSH, ferritin, and vitamin D checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a quick “pattern check” in good light: if your part is widening and the crown looks see-through but the hairline is mostly intact, that points more toward pattern hair loss than a one-time shedding event.
Take two baseline photos today (front hairline and top/crown) and repeat them monthly in the same lighting. Hair changes are slow, and photos keep you from quitting a helpful plan too early.
If you suspect stress shedding, look back 8–16 weeks for a trigger like illness, surgery, a new medication, or rapid weight loss. Naming the trigger helps you set expectations, because regrowth often starts only after the trigger is gone.
If you start minoxidil, put it next to something you already do daily, like brushing your teeth, so it becomes automatic. Consistency beats intensity with hair treatments.
When you supplement iron, ask for a ferritin recheck rather than guessing. Your goal is not “more pills,” it is getting ferritin into a hair-supportive range and then maintaining it safely.
Frequently Asked Questions
Is hair thinning in your 60s normal or a sign of illness?
It’s common, and the most frequent reason is age-related pattern hair loss, which is largely genetic. That said, thyroid problems and low ferritin (iron stores) can mimic or worsen thinning, and those are worth checking because they are treatable. If your thinning is sudden, patchy, or comes with scalp pain, book a dermatology visit because that pattern is less “normal aging.”
How can I tell if my hair loss is shedding or pattern thinning?
Shedding tends to be diffuse and noticeable in the shower or brush, and it often starts 2–4 months after a trigger like illness, surgery, or rapid weight loss. Pattern thinning is slower and shows up as a widening part or thinner crown, with hairs becoming finer over time. If you are unsure, monthly photos plus a ferritin and TSH check can help you avoid guessing.
What ferritin level is best for hair growth?
For hair regrowth, many clinicians aim for ferritin above about 50 ng/mL, because follicles seem to struggle when iron stores are low even if you are not anemic. Some people are targeted to 70–100 ng/mL depending on the full iron panel and medical history. The practical move is to test ferritin first, treat if low, and recheck in 8–12 weeks.
How long does it take for hair to grow back after thinning?
Hair follicles cycle slowly, so visible improvement usually takes months, not weeks. After stress shedding, many people see reduced shedding within 2–3 months and early regrowth by 3–6 months, while pattern hair loss treatments like minoxidil often need 6–12 months for a fair trial. Track progress with monthly photos so you can see small changes that are easy to miss day-to-day.
Should I take biotin or collagen for hair thinning in my 60s?
If you are not deficient, biotin and collagen usually don’t fix the most common drivers of thinning, such as pattern hair loss, low ferritin, or thyroid issues. Biotin deficiency is uncommon, and high-dose biotin can interfere with some lab tests, including thyroid and heart markers, which can create confusing results. If you want a supplement plan, start by checking ferritin, TSH, and vitamin D so you’re treating a real gap rather than hoping.