Swelling in Working Women: What It Means and What Helps
Swelling in working women often comes from fluid pooling after long sitting/standing, salt-related water retention, or low protein. Targeted labs—no referral needed.
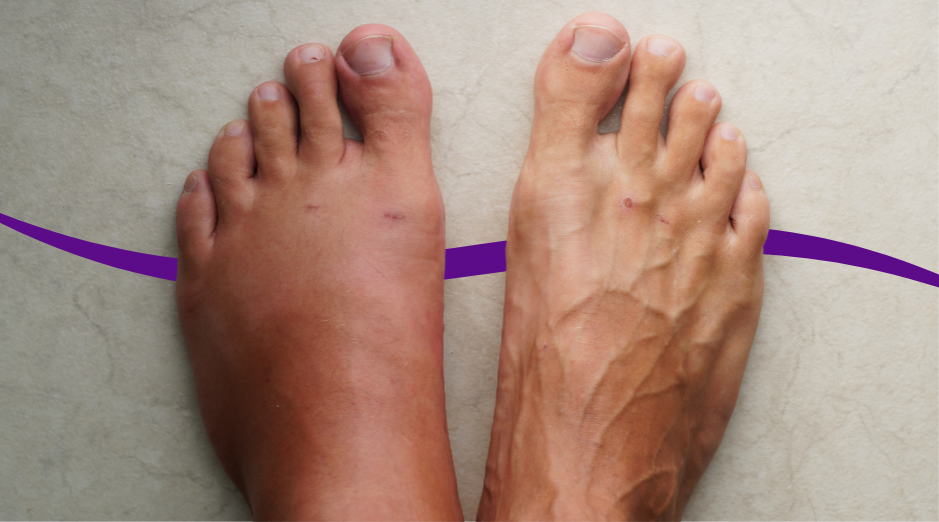
Swelling on workdays is usually your body holding onto fluid because it has been sitting or standing for hours, because you ate more sodium than you realized, or because an underlying issue like low blood protein or kidney strain is making fluid leak into tissues. The pattern and location matter, and a few targeted blood tests can help sort out what is “normal workday pooling” versus something you should treat. If your shoes feel tighter by 4 p.m. or your rings suddenly leave deep marks, you are not imagining it. Work routines can quietly stack the deck: long meetings, commuting, travel, stress hormones, and convenience food all push fluid toward your hands, ankles, and calves. Most swelling is benign and fixable, but one-sided swelling, chest symptoms, or swelling that is new and rapidly worsening deserves faster attention. PocketMD can help you triage your pattern, and Vitals Vault labs can help you check the common medical drivers without turning this into a months-long guessing game.
Why swelling shows up on workdays
Fluid pools in your lower legs
When you sit or stand for long stretches, gravity wins and fluid seeps out of tiny blood vessels into your ankles and calves. You feel it as tight shoes, sock marks, or a heavy “waterlogged” sensation by the end of the day. The key clue is timing: it is worse after work and improves overnight with your feet up.
Salt pulls water into tissues
Sodium makes your body hold onto water, and workday food is often saltier than it tastes, especially soups, sauces, deli meals, and “healthy” packaged snacks. The swelling can show up in your fingers (rings feel tight) as well as your face or ankles, and you may notice thirst or a puffy morning after takeout. A useful experiment is a 7-day “low-sodium week” where you cook simply and compare photos of your ankles at the same time each day.
Hormone shifts change fluid balance
Estrogen and progesterone influence how your kidneys handle salt and water, which is why swelling can flare in the week before your period, during perimenopause, or with certain birth control methods. It often feels like generalized puffiness rather than one specific spot, and it can come with breast tenderness or bloating. If your swelling cycles predictably, tracking it against your cycle for two months can prevent unnecessary panic and help you choose smarter timing for travel or long days on your feet.
Kidneys aren’t clearing fluid well
Your kidneys normally filter extra salt and water out of your blood, but dehydration, certain pain relievers, and early kidney disease can all reduce that “drainage.” Swelling from kidney issues is often more persistent and may be more noticeable around the eyes in the morning, not just in the ankles at night. If you have foamy urine, rising blood pressure, or swelling that does not improve with elevation, checking kidney labs is a practical next step.
Low protein in your blood (albumin)
Albumin is a protein that helps keep fluid inside your blood vessels, so when it is low, water leaks into tissues more easily. You may notice swelling that is more widespread and stubborn, sometimes with fatigue or unintentional weight changes that are really fluid shifts. Low albumin can come from liver problems, kidney protein loss, or poor intake during stressful, busy stretches, which is why a simple blood test can be surprisingly clarifying.
What actually helps swelling when you’re working
Use timed movement “flush breaks”
Set a timer for every 45–60 minutes and do two minutes of calf pumps, brisk hallway walking, or stair laps, because your calf muscles act like a second heart for your legs. This is not about burning calories; it is about pushing fluid back up toward your torso so it can be cleared. If you can only do one thing, do 20 heel raises while you wait for coffee or a file to load.
Compression that fits your day
Graduated compression socks or stockings can prevent that end-of-day ankle ballooning by supporting the veins and limiting fluid leakage. Many people do best with 15–20 mmHg for desk or retail work, while stronger compression is usually a clinician-guided choice. Put them on in the morning before swelling starts, because they work far better as prevention than as a rescue.
A sodium “swap,” not a diet
Instead of trying to eat perfectly, pick one high-sodium work habit to replace for two weeks, such as switching from deli lunch to a simple protein-and-produce meal with an unsalted dressing. You are looking for a noticeable change in ring tightness or ankle size, which tells you sodium is a major driver for you. If the swelling improves, you can keep the swap and still enjoy salty foods occasionally without feeling like you failed.
Elevate with a specific target
Elevation helps when the swelling is mostly from pooling, but it has to be high enough to matter. Aim for 15–20 minutes with your feet above heart level, like lying on the floor with calves on a couch, because “feet on an ottoman” often isn’t enough. If your swelling drops quickly with true elevation, that is reassuring and points toward a circulation-and-gravity problem rather than a kidney or protein issue.
Review meds and pain relievers
Some common medications can cause swelling, including certain blood pressure drugs, hormones, and anti-inflammatory pain relievers like ibuprofen, which can make your kidneys retain salt. The practical move is to write down everything you take, including supplements, and note when the swelling started or changed. Bring that timeline to your clinician, because adjusting a dose or switching a medication can fix the problem without adding new treatments.
Useful biomarkers to discuss with your clinician
Sodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreProtein, Total
Total protein levels reflect nutritional status, liver function (protein synthesis), and kidney function (protein retention). Abnormal levels can indicate liver disease, kidney disease, malnutrition, inflammation, or blood cancers. It provides a general overview of protein metabolism. Total protein measures the combined amount of albumin and globulins in blood. These proteins are essential for maintaining fluid balance, transporting substances, fighting infections, and blood clotting.
Learn moreAlbumin
Albumin is the most abundant protein in blood plasma, produced exclusively by the liver. In functional medicine, albumin serves as a marker of liver synthetic function, nutritional status, and overall health. Albumin maintains oncotic pressure (keeping fluid in blood vessels), transports hormones and nutrients, and serves as an antioxidant. Low albumin may indicate liver disease, malnutrition, chronic inflammation, or kidney disease. Since albumin has a half-life of about 20 days, it reflects longer-term nutriti…
Learn moreLab testing
Get kidney function, albumin, and thyroid checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a 3-day “same-shoes test”: wear the same shoes at the same time each day and note when they start to feel tight. If tightness reliably hits after long sitting or standing, you have a strong clue that pooling is the main driver.
Take two quick photos for a week: one of your ankles or hands right after waking, and one at the end of your workday. Seeing the change makes it easier to judge whether a new plan is working.
If you travel for work, put compression socks in your bag like you would a charger. Flights and long drives are swelling multipliers, and prevention is much easier than trying to “undo” it at the hotel.
When your rings feel tight, use it as a signal to do a two-minute movement break rather than forcing the ring off. If the tightness eases after walking, that points away from an emergency and toward fluid shifting.
If you need pain relief, ask your clinician whether frequent NSAID use (like ibuprofen) could be contributing to swelling for you. For some people, changing the pain plan reduces swelling within a week.
Frequently Asked Questions
Why do my ankles swell after sitting at a desk all day?
When you sit for hours, gravity pulls fluid into your lower legs and your calf muscles are not “pumping” it back up efficiently. That is why you see sock marks and feel tight shoes late in the day, but you look more normal in the morning. Try two-minute calf-pump breaks every hour for a week and compare end-of-day swelling.
When is swelling an emergency?
Get urgent care if you have swelling in one leg with pain or warmth, sudden shortness of breath, chest pain, or you are coughing up blood, because those can signal a clot or heart/lung strain. Also take new, rapidly worsening swelling seriously if you are pregnant or have known heart or kidney disease. If you are unsure, it is reasonable to call for same-day advice rather than waiting it out.
Can stress cause swelling and water retention?
Yes, stress hormones can nudge your body to retain salt and water, and stress also changes sleep and food choices in ways that amplify swelling. The pattern is often “puffier during intense weeks” rather than a single dramatic episode. If this is you, tracking swelling against sleep and sodium for two weeks usually shows which lever matters most.
What blood tests should I get for unexplained swelling?
A practical starting trio is a comprehensive metabolic panel (kidney and liver clues), albumin (your main fluid-holding protein), and TSH (thyroid signal). If albumin is low, urine testing for protein is often the next step, because protein loss through the kidneys is a common reason swelling persists. Bring your results and your swelling pattern (morning vs evening, one-sided vs both) to a clinician for interpretation.
Why do my fingers swell and my rings get tight at work?
Finger swelling is often from sodium-related water retention, heat, or long periods of stillness where fluid shifts into tissues. It can also flare around the premenstrual week because hormones change how your kidneys handle salt. Try a one-week experiment where you cut one major salty work meal and add short movement breaks, then see if ring tightness improves.
Research and guidelines worth knowing about
International Society of Lymphology consensus on peripheral lymphedema evaluation and management
KDIGO guideline for chronic kidney disease evaluation and risk stratification (eGFR and albumin considerations)
AHA/ACC/HFSA guideline for heart failure (edema as a key symptom that needs clinical assessment)
