Why You Might Swell During Fasting
Swelling during fasting often comes from salt shifts, low protein, or kidney/heart strain. Targeted blood tests are available at Quest—no referral needed.
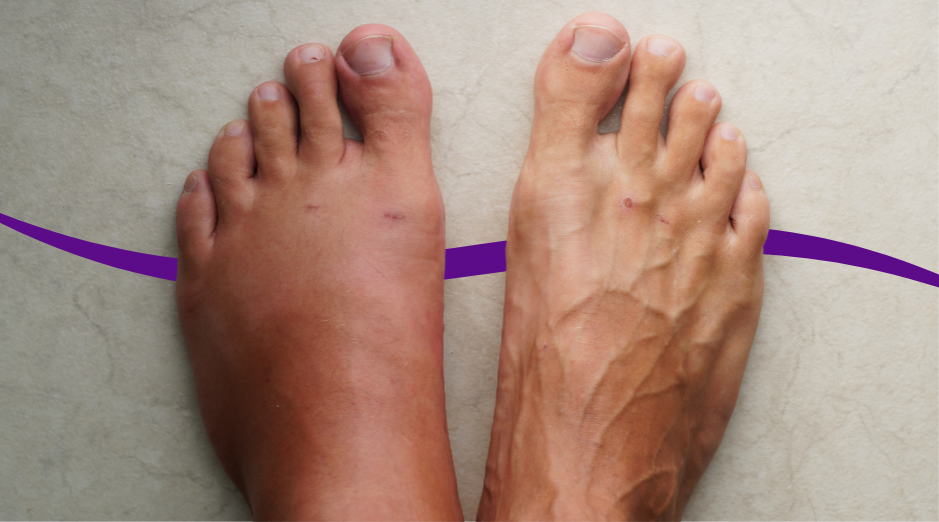
Swelling during fasting usually happens because your body is holding onto salt and water, your blood protein is lower than usual, or an underlying kidney, heart, or liver issue is being unmasked by the stress of fasting. It can show up as puffy fingers in the morning, tight shoes by afternoon, or a “full” face that does not match your calorie intake. A few targeted labs can help sort out whether this is a simple fluid shift or a sign you should stop fasting and get checked. Fasting changes hormones that control fluid balance, and it also changes what you eat and drink, which can swing your sodium and potassium intake more than you realize. That is why two people can do the same fasting schedule and have totally different results. If your swelling is one-sided, comes with chest pain, shortness of breath, new confusion, or a rapid weight jump of more than about 2–3 pounds (1–1.5 kg) in a day, treat that as urgent and get care right away. For everything else, this page will help you narrow the likely cause, try practical fixes, and use tools like PocketMD and VitalsVault labs to get clarity without guesswork.
Why you might swell during fasting
Salt and water rebound
When you fast, your insulin level drops, and your kidneys can dump salt and water at first, which can feel like you are “leaning out.” But if you then drink salty broth, eat a salty meal at refeed, or simply swing back to normal carbs, your body can pull water back into your tissues quickly. That rebound is why your rings can feel tight even though you did not overeat. The takeaway is to look at the 24 hours around the swelling, not just the fasting window, because the trigger is often the refeed sodium and carbs.
Not enough protein in refeed
Your blood needs enough protein—especially albumin—to keep fluid inside your blood vessels instead of leaking into your ankles, hands, or under-eye area. If fasting leads you to eat very small meals or mostly low-protein foods, albumin can drift low over time, and swelling becomes easier to trigger. This matters because it is not just cosmetic; low albumin can also make you feel weak and lightheaded. A practical check is whether you are consistently getting a solid protein portion at refeed, not just “something small so you don’t break the fast too hard.”
Kidneys struggling with the shift
Your kidneys are the main “fluid and salt managers,” and fasting can stress them if you get dehydrated, use NSAIDs like ibuprofen, or already have reduced kidney function. When kidneys cannot clear salt well, water follows salt, and swelling shows up in the feet and lower legs first. You might also notice foamy urine or higher blood pressure, which is your body’s way of saying fluid is staying on board. If swelling keeps recurring with fasting, kidney labs are one of the fastest ways to rule in or rule out a real problem.
Heart not moving fluid forward
If your heart is not pumping strongly enough, fluid backs up in the legs and sometimes the belly, and fasting does not “fix” that—sometimes it makes it more noticeable because you are paying closer attention to your body. Swelling from heart strain often worsens later in the day and improves overnight, and it can come with getting winded more easily than usual. This matters because the right response is not to push through longer fasts; it is to get evaluated and adjust meds or salt targets. If you have swelling plus shortness of breath when lying flat, that is a same-day problem.
Hormone and cycle water retention
If you menstruate, swelling that appears during fasting can still be driven by your cycle, because progesterone shifts and stress hormones can change how your body handles salt. Fasting itself can raise your stress hormone (cortisol), and that can make you retain water even when you are eating less. It feels unfair, because you are doing “everything right” and still look puffy. The useful move is to compare swelling to your cycle week and sleep quality, because that pattern often explains more than the fasting schedule does.
What actually helps with fasting-related swelling
Stabilize sodium across days
If your sodium intake swings wildly between fasting days and refeed days, your body will swing water with it. Try keeping sodium more consistent for a week by using the same broth or electrolyte plan each fasting day and avoiding “salt bombs” at the first meal. You are not aiming for low sodium; you are aiming for predictable sodium so your kidneys stop playing catch-up. Many people notice less puffiness within 3–5 days of consistency.
Refeed with protein first
Break your fast with a protein-forward meal, because it supports albumin over time and it also reduces the urge to overdo salty, carby foods that pull water into tissues. Think of it as giving your body building blocks before you give it a big sodium or carb load. If you are not sure what “enough” looks like, a simple target is 25–35 grams of protein in that first meal for many adults, adjusted for your size and goals. If swelling improves when you do this, it is a strong clue that your refeed pattern was part of the problem.
Hydrate on purpose, not by feel
During fasting, thirst cues can get weird, especially if you are busy or drinking a lot of coffee or tea. Instead of chugging at night, spread fluids earlier in the day and pair them with a small, steady electrolyte plan if you are doing longer fasts. This helps because dehydration can trigger your body to hold onto salt and water later, which shows up as swelling. If you wake up puffy, look at evening fluids and salty drinks, because that timing often matters more than total ounces.
Move fluid with gentle muscle work
Your calf muscles act like a pump that helps push fluid back toward your heart, so long sitting during a fast can make ankle swelling worse even if nothing is “wrong.” A 10-minute walk, a few sets of calf raises, or simply elevating your legs for 15 minutes can change how your ankles look by the end of the day. This is especially useful if your swelling is mostly below the knees and improves overnight. If movement helps quickly, it points toward circulation and positioning rather than a deeper organ issue.
Pause fasting if red flags show up
If swelling is new for you and it comes with shortness of breath, chest pressure, one-sided leg swelling, or a rapid weight jump over 2–3 pounds in a day, stop fasting and get evaluated. Fasting can mask hunger but it does not protect you from clots, heart strain, or kidney injury. The goal is not to “tough it out,” because the right fix might be medication adjustment or a different nutrition plan. If you are unsure, getting a same-week check-in is the safer move.
Useful biomarkers to discuss with your clinician
Albumin
Albumin is the most abundant protein in blood plasma, produced exclusively by the liver. In functional medicine, albumin serves as a marker of liver synthetic function, nutritional status, and overall health. Albumin maintains oncotic pressure (keeping fluid in blood vessels), transports hormones and nutrients, and serves as an antioxidant. Low albumin may indicate liver disease, malnutrition, chronic inflammation, or kidney disease. Since albumin has a half-life of about 20 days, it reflects longer-term nutriti…
Learn moreSodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreCreatinine
Creatinine is a waste product of muscle metabolism that is filtered by the kidneys and serves as the primary marker of kidney function. In functional medicine, creatinine levels reflect not only kidney health but also muscle mass and protein metabolism. Elevated creatinine indicates reduced kidney filtration capacity, while very low levels may indicate muscle wasting or poor protein intake. Creatinine is used to calculate eGFR and helps assess long-term kidney health and detoxification capacity. Creatinine measu…
Learn moreLab testing
Get kidney function, electrolytes, and albumin checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a 7-day “same-salt experiment”: keep your broth/electrolyte routine and your first meal sodium roughly the same each day, and see if swelling stops bouncing around by day 4 or 5.
Measure swelling in a way you can actually compare: take a morning photo of your hands and ankles in the same lighting, and track your weight after you pee but before you drink anything.
If your shoes get tight late in the day, try a 10-minute walk plus 2 minutes of calf raises before dinner; if that helps quickly, your swelling is more likely from pooling than from low protein.
If you use NSAIDs (like ibuprofen or naproxen), consider avoiding them during longer fasts unless a clinician told you otherwise, because they can reduce kidney blood flow and make fluid retention easier.
When you break a fast, eat slowly for 20 minutes and stop at “comfortably satisfied,” because a big fast-break meal tends to be saltier and higher carb than you planned, which is a perfect setup for next-day puffiness.
Frequently Asked Questions
Is swelling during fasting normal?
Mild puffiness can happen, especially around refeed days, because sodium and carbs change how much water your body stores. Swelling that is new, persistent, or clearly worsening is not something to brush off, because kidney, heart, and low-albumin issues can look the same at first. If you also have shortness of breath, chest pain, or one-sided leg swelling, get urgent care. Otherwise, tracking your sodium pattern and checking a CMP, albumin, and uACR can quickly clarify what is going on.
Why do my fingers swell when I’m not eating?
Your fingers often swell from fluid shifts rather than fat gain, and fasting can set up those shifts through stress hormones and big sodium changes at refeed. If you drink salty broth or break your fast with a salty meal, your body may pull water into tissues overnight, which is why rings feel tight in the morning. Try keeping sodium steadier for a week and breaking your fast with a protein-forward meal. If finger swelling comes with facial puffiness and foamy urine, ask about kidney testing such as uACR.
Can intermittent fasting make edema worse?
Yes, it can, especially if fasting leads to dehydration, higher cortisol, or a pattern of very salty refeeds. It can also make underlying heart or kidney problems more obvious because your fluid balance is being pushed around more than usual. If you already have diagnosed heart failure or kidney disease, fasting should be discussed with your clinician because medication timing and salt targets matter. A practical first step is to monitor daily weight and check kidney function and electrolytes with a CMP.
What’s the difference between water retention and real edema?
Water retention is often a short-term swing that tracks with sodium, carbs, and hormones, and it tends to come and go quickly. “Real” edema is swelling from fluid leaving the bloodstream and pooling in tissues, and it is more likely to persist, pit when you press a finger into it, or come with other symptoms like high blood pressure or shortness of breath. Labs can help separate them: low albumin, abnormal CMP kidney markers, or a high uACR point toward a medical cause. If you are unsure, check whether swelling improves overnight and whether it pits when pressed.
What labs should I get for swelling during fasting?
A good starting trio is a Comprehensive Metabolic Panel (CMP) to look at electrolytes and kidney function, albumin to assess blood protein, and a urine albumin-to-creatinine ratio (uACR) to check for kidney protein loss. For many people, an optimal uACR is under 30 mg/g, and albumin is ideally stable and comfortably above 3.5 g/dL. If any of these are abnormal, it changes what you should do next and whether fasting is a good idea right now. Bring the results to a clinician or use PocketMD to help you interpret what pattern fits your symptoms.
What research says about swelling and fasting
KDIGO guideline on chronic kidney disease evaluation, including albuminuria testing
AHA/ACC/HFSA guideline for the management of heart failure, including edema assessment and fluid management
Review of intermittent fasting and metabolic switching, including hormonal shifts that can affect fluid balance