Why Do You Swell More at Night?
Swelling at night is often from fluid pooling, salt-related water retention, or heart/kidney strain. Targeted blood tests available—no referral needed.
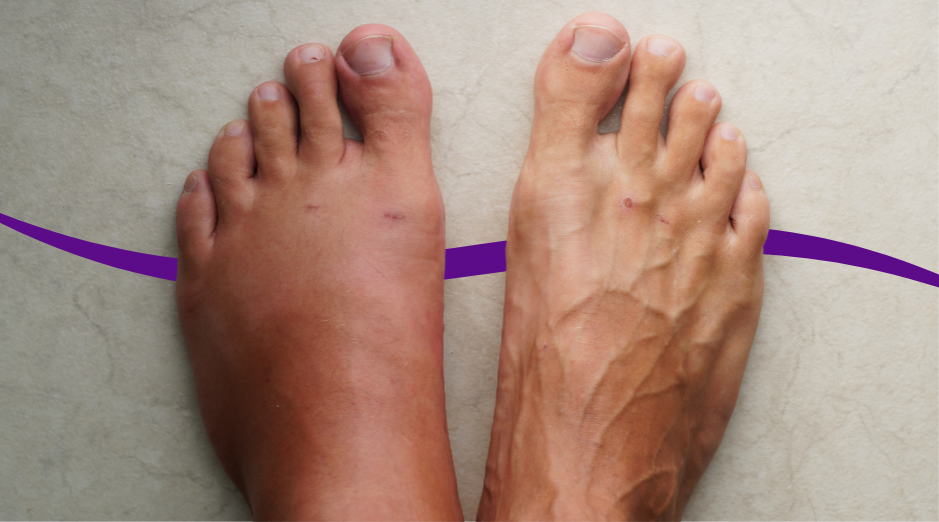
Swelling at night usually happens because fluid settles in your legs and feet after a day of gravity, or because your body is holding onto extra salt and water. Sometimes it is a clue that your heart, kidneys, veins, or lymph system are under strain, and blood tests can help sort out which one fits your situation. Nighttime swelling is frustrating because it can look dramatic even when you felt “fine” earlier, and it can make shoes, rings, and sleep uncomfortable. Most of the time it is fixable once you identify the pattern, but there are a few red flags you should not ignore, like swelling in just one leg with pain, sudden shortness of breath, or swelling that is rapidly getting worse. If you want help thinking through your specific mix of symptoms and meds, PocketMD can walk you through the most likely causes, and targeted labs through Vitals Vault can help confirm what your body is doing behind the scenes.
Why You Swell More at Night
Fluid pools in your legs
When you are upright all day, gravity pulls fluid into the tissues of your ankles and feet, especially if you sit or stand for long stretches. By evening, that “extra” fluid shows up as sock marks, tight shoes, or puffy toes. A simple clue is that the swelling improves overnight and is worse after long days, flights, or car rides.
Vein valves are getting weak
Your leg veins rely on one-way valves and calf muscles to push blood back to your heart, and when that system is leaky (chronic venous insufficiency), fluid seeps into the surrounding tissue. It often feels like heaviness or aching that builds through the day, and you might notice skin discoloration near the ankles over time. Compression socks and leg elevation help this cause more than they help “water retention” from hormones or diet.
Salt makes you retain water
After a salty meal, your body holds onto water to keep your blood chemistry stable, and that extra volume can end up in your hands, face, or lower legs by nighttime. This is why swelling can flare after restaurant food even if you did not eat more calories. If your swelling predictably follows certain foods, a two-week sodium experiment is often more informative than guessing.
Kidneys not clearing fluid well
Your kidneys control how much salt and water you keep, so when kidney function is reduced, swelling can show up in the legs and around the eyes and may not fully disappear by morning. You might also notice foamy urine, higher blood pressure, or fatigue that feels out of proportion to your day. This is one of the situations where labs matter, because early kidney issues can be silent until swelling becomes obvious.
Heart strain causing fluid backup
If the heart is not pumping effectively (heart failure), pressure builds in the veins and fluid leaks into tissues, which often shows up as ankle swelling that worsens later in the day. The “so what” is breathing: you may get short of breath when walking, need extra pillows at night, or wake up feeling air-hungry. If swelling comes with chest pain, fainting, new one-sided leg swelling, or sudden shortness of breath, treat that as urgent and get evaluated right away.
What Actually Helps Tonight
Do a 20-minute leg-elevation reset
Lie down and elevate your legs so your ankles are above the level of your heart, because that position helps fluid move back into circulation. If you do this once in late afternoon and again before bed, many people notice less tightness and fewer nighttime throbs. It works best if you keep your knees fairly straight and avoid letting your heels dig into the mattress.
Use compression the right way
Compression socks work when you put them on in the morning, before swelling builds, because they prevent fluid from leaking into tissue in the first place. For mild swelling, 15–20 mmHg is a common starting point, but if you have significant varicose veins or venous disease you may need a higher level guided by a clinician. If your feet are cold, numb, or painful in compression, stop and get checked for circulation problems.
Walk after dinner, not later
A 10–15 minute easy walk after your evening meal turns your calf muscles into a pump that pushes fluid back up your legs. Doing it earlier matters, because it gives your body time to re-balance before you lie down and notice every sensation. If you cannot walk, slow ankle circles and heel raises while seated can still help.
Run a sodium reality check
For one week, aim for roughly 1,500–2,000 mg of sodium per day and see what your swelling does, because many “healthy” packaged foods quietly push you far above that. The goal is not perfection; it is to learn whether your body is salt-sensitive. If your swelling drops noticeably within 3–5 days, you have a clear lever you can use on busy weeks or travel days.
Review meds that cause swelling
Some common medications make nighttime swelling more likely, especially certain blood pressure drugs like amlodipine, anti-inflammatories like ibuprofen, and hormones. The fix is not to stop them on your own, because there are often safer swaps or dose adjustments that keep the benefit without the puffiness. Bring a photo of the swelling and a list of meds and supplements to your next visit so the conversation is concrete.
Useful biomarkers to discuss with your clinician
Sodium
Sodium is the primary extracellular electrolyte essential for fluid balance, nerve transmission, muscle contraction, and blood pressure regulation. In functional medicine, sodium balance reflects kidney function, adrenal health, and hydration status. Low sodium (hyponatremia) can cause neurological symptoms and may indicate SIADH, adrenal insufficiency, or excessive water intake. High sodium may indicate dehydration, diabetes insipidus, or excessive salt intake. Optimal sodium levels support cellular energy prod…
Learn moreCreatinine
Creatinine is a waste product of muscle metabolism that is filtered by the kidneys and serves as the primary marker of kidney function. In functional medicine, creatinine levels reflect not only kidney health but also muscle mass and protein metabolism. Elevated creatinine indicates reduced kidney filtration capacity, while very low levels may indicate muscle wasting or poor protein intake. Creatinine is used to calculate eGFR and helps assess long-term kidney health and detoxification capacity. Creatinine measu…
Learn moreAlbumin
Albumin is the most abundant protein in blood plasma, produced exclusively by the liver. In functional medicine, albumin serves as a marker of liver synthetic function, nutritional status, and overall health. Albumin maintains oncotic pressure (keeping fluid in blood vessels), transports hormones and nutrients, and serves as an antioxidant. Low albumin may indicate liver disease, malnutrition, chronic inflammation, or kidney disease. Since albumin has a half-life of about 20 days, it reflects longer-term nutriti…
Learn moreLab testing
Get kidney function, albumin, and BNP checked at Quest—starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Take a clear photo of the swelling at the same time each evening for a week, and include a side view of your ankle bones. Patterns show up fast, and photos help a clinician take you seriously even if the swelling is gone by the appointment.
Try the “sock line test” at 6–8 pm: if you have deep indentations from socks or leggings, that is true fluid swelling, not just normal softness. Write down whether it is equal on both sides, because one-sided swelling changes the differential.
If your swelling is in your feet and ankles, measure around the narrowest part above the ankle bone with a tape measure before bed and again in the morning. A drop of 1–2 cm overnight strongly suggests gravity and vein-related pooling.
On travel days, set a timer for every 60–90 minutes to stand up and do 20 calf raises, because your calves are your “second heart” for moving fluid. This one habit can prevent the evening ballooning that makes you dread taking your shoes off.
If you are starting a new medication and swelling appears within 1–3 weeks, do not wait months hoping it will settle. Message your prescriber early, because a small change in drug choice can fix the problem without losing the benefit.
Frequently Asked Questions
Why are my feet and ankles swollen at night but normal in the morning?
That pattern usually means gravity-related fluid pooling: fluid collects in your lower legs during the day and then re-enters circulation when you lie flat overnight. It is common with long sitting or standing, and it is even more likely if your leg veins are not pushing blood up efficiently. Try leg elevation for 20 minutes before bed and see if the next morning looks different.
When is swelling at night an emergency?
Get urgent care if you have sudden shortness of breath, chest pain, coughing up pink froth, or swelling that rapidly worsens over hours. Also take one-sided leg swelling seriously if it comes with calf pain, warmth, or redness, because that can signal a blood clot. If you are unsure, err on the side of being checked the same day.
Can dehydration cause swelling at night?
It can, in a roundabout way, because when you are dehydrated your body releases hormones that tell your kidneys to conserve salt and water. If you then eat salty food or drink a lot late in the day, you can “overshoot” and feel puffy by evening. Aim for steady fluids earlier in the day and watch whether late-night swelling improves within a week.
What blood tests should I get for swelling in my legs?
A practical starting trio is a comprehensive metabolic panel (kidney function and electrolytes), albumin (a blood protein that keeps fluid in vessels), and BNP or NT-proBNP (a heart strain marker). Abnormal kidney numbers or low albumin can explain persistent edema, while a higher BNP makes heart-related fluid overload more likely. If you have results, bring them to a clinician so they can interpret them in the context of your symptoms and medications.
Does amlodipine or ibuprofen cause ankle swelling at night?
Yes, both can contribute, but through different mechanisms: amlodipine can widen small blood vessels so fluid leaks into tissue, while ibuprofen can make the kidneys hold onto salt and water. The swelling often shows up in the evening and improves overnight, which can make it easy to miss as a side effect. Do not stop prescribed meds abruptly; ask about alternatives or dose adjustments if the timing fits.
What Research and Guidelines Say
2022 AHA/ACC/HFSA guideline for the management of heart failure (includes edema evaluation and BNP use)
KDIGO 2024 chronic kidney disease guideline (fluid balance, kidney testing, and risk stratification)
Society for Vascular Surgery and American Venous Forum guideline on chronic venous disease and compression therapy