Why Does Your Hair Seem Thinner Before You Eat?
Hair thinning before eating is often from low iron, thyroid imbalance, or blood-sugar stress hormones. Targeted labs available at Quest, no referral needed.
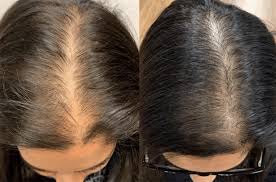
Hair thinning before eating usually comes down to your body being under-resourced or under stress when your stomach is empty, which can show up as iron-related shedding, thyroid imbalance, or blood-sugar dips that push stress hormones higher. It can also be a timing illusion, because hair and scalp look flatter and more visible when you are dehydrated or your hair is less “plumped” by oil and moisture. Simple blood tests can help you sort out which pattern fits you, instead of guessing. If you are noticing more scalp show-through in the morning, before lunch, or during fasting, you are not imagining it. Hair growth is slow, but shedding can feel sudden, and anything that nudges your body into “conserve energy” mode can shift more hairs into a resting phase. The good news is that the most common drivers are measurable and fixable, and you can often see early improvement in shedding within 6–12 weeks once the root cause is addressed. If you want help narrowing your most likely cause based on your timeline, postpartum status, diet, and symptoms, PocketMD can walk you through it, and Vitals Vault labs can help you confirm what your body is missing.
Why does your hair seem thinner before you eat?
Low iron stores (ferritin)
Iron is one of the raw materials your hair follicles use to stay in a growth phase, and your “iron savings account” is ferritin. When ferritin is low, your body quietly prioritizes essentials like oxygen delivery over hair growth, so more hairs shift into shedding a few months later. This can feel worse on an empty stomach because you are more likely to notice fatigue, lightheadedness, or cold hands at the same time, which makes the hair change feel connected to meals. A practical takeaway is to check ferritin before you start supplements, because the goal for hair is often higher than “barely normal,” and the right dose depends on your starting point.
Thyroid slowdown or overdrive
Your thyroid hormone acts like a metabolic dimmer switch for your follicles, so both low and high thyroid activity can cause diffuse thinning rather than bald patches. If your hair looks worse before eating, it can be because low thyroid function also slows digestion and lowers energy, which makes you feel especially “flat” when you have not fueled yet. Look for clues like constipation and feeling cold, or the opposite pattern of heat intolerance and a racing heart. The key move is not to self-dose thyroid meds or iodine, but to check a thyroid-stimulating hormone test and discuss results in the context of symptoms.
Blood-sugar dips and stress hormones
When you go too long without eating, your body can raise stress hormones like cortisol and adrenaline to keep your blood sugar steady. That stress signal does not directly make hair fall out in the moment, but repeated spikes can push your body toward “maintenance mode,” which is a common setup for shedding a couple of months later. You might notice this pattern if you also get shakiness, irritability, or a wired-but-tired feeling before meals. A useful takeaway is to treat this like a stability problem, not a willpower problem, and aim for fewer big gaps between meals while you investigate.
Postpartum or post-illness shedding
After pregnancy, a high fever, surgery, or a major life stress, it is common for hair to shed more than usual because many follicles synchronized into a resting phase and then “let go” together later. The timing can make it feel linked to eating because new parents and recovering bodies often have irregular meals, sleep loss, and dehydration, which make hair look flatter and scalp more visible. The most important context is that this is usually temporary, but it is emotionally loud. If shedding is still heavy beyond about 6–9 months postpartum or it is paired with symptoms like heavy periods or extreme fatigue, it is worth checking iron and thyroid because those can prolong the cycle.
Dehydration and scalp visibility
Sometimes the hair is not actually shedding more before you eat, but it looks thinner because your strands are drier, less coated with natural oils, and lying flatter against your scalp. Overnight dehydration, morning coffee, or a long stretch without fluids can make the part line look wider even if your follicle count has not changed. This matters because it can trick you into chasing the wrong cause and missing a real one. Try a simple test: take a photo of your part in the same lighting before breakfast and again after a meal plus water, and see whether the “thinning” is mostly a styling and hydration effect.
What actually helps when it’s worse on an empty stomach
Build a blood-sugar-stable breakfast
If your hair looks worse when you are hungry and you also feel shaky or anxious, start by stabilizing your mornings. A breakfast with protein plus fiber and fat tends to reduce stress-hormone spikes compared with a carb-only meal, which can help your body feel safer and more consistent day to day. You do not need perfection, but you do need repetition, because hair responds to patterns. Give this 2–3 weeks and track whether the “before eating” crash feeling improves.
Correct low ferritin thoughtfully
If ferritin is low, the fix is usually iron repletion plus finding the reason it dropped, such as heavy periods, low dietary iron, or poor absorption. Many people tolerate iron better when they take it every other day, and vitamin C can improve absorption, while calcium taken at the same time can block it. You are aiming for a ferritin level that supports hair growth, which is often around 50–100 ng/mL for many people, not just “above the lab minimum.” Recheck labs after about 8–12 weeks so you are not guessing.
Treat the thyroid, not just TSH
If thyroid tests are off, the best results come from treating the underlying thyroid condition and then giving hair time to catch up. Even when thyroid levels normalize quickly, follicles often need 2–4 months before shedding slows, and 6–12 months for visible density changes. If you are already on thyroid medication, taking it consistently on an empty stomach and separating it from iron supplements can make a real difference. Bring your symptom timeline and medication schedule to your clinician so adjustments are based on your real life, not a perfect-world routine.
Reduce fasting while shedding is active
Fasting can be a useful tool for some goals, but active shedding is a sign your body may not love the current level of stress. If you are doing intermittent fasting, try shortening the fasting window for 6–8 weeks and see whether shedding slows, especially if you are postpartum, training hard, or under-sleeping. This is not about “never fast,” but about matching your eating pattern to your recovery capacity. If you feel better within days but hair takes weeks, that is still a win because it suggests the direction is right.
Protect hair while it regrows
When shedding is high, your strands are more likely to break, which makes thinning look worse even if follicles are recovering. Gentle handling matters here, because traction and heat can turn a temporary shedding problem into a longer cosmetic one. Switch to looser styles, minimize tight ponytails, and consider a wide-tooth comb when wet hair is most fragile. If you see short broken hairs along the hairline, that is a clue to focus on breakage protection while you fix the internal driver.
Useful biomarkers to discuss with your clinician
Ferritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreTSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreGlucose
Fasting glucose is a fundamental marker of glucose metabolism and insulin function. In functional medicine, we recognize that even 'normal' glucose levels in the upper range may indicate early insulin resistance. Optimal fasting glucose reflects efficient glucose regulation and insulin sensitivity. Elevated fasting glucose suggests the body's inability to maintain normal glucose levels overnight, indicating hepatic insulin resistance or insufficient insulin production. This marker is essential for early detectio…
Learn moreLab testing
Get ferritin, TSH, and fasting insulin checked at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a 14-day “empty stomach” log: take one photo of your part in the same bathroom lighting before breakfast and rate how thin it looks from 1–10, then repeat after you have eaten and had a full glass of water. If the look changes fast, hydration and hair lay are part of the story.
If you suspect iron, do not start with a random high-dose supplement and hope. Get ferritin checked first, and if it is low, plan to recheck it in 8–12 weeks so you know whether you are actually rebuilding your iron stores.
If you are postpartum, write down your delivery date and when shedding started. Shedding that begins around 2–4 months postpartum and peaks around 4–6 months often fits a normal pattern, but persistent heavy shedding past 9 months deserves a ferritin and TSH check.
If you are fasting, try a “hair-friendly” experiment: shorten your fasting window by two hours for six weeks and keep protein consistent. Hair changes are slow, but your pre-meal shakiness and mood should improve quickly if blood-sugar stress is driving the pattern.
Separate thyroid medication from iron by at least four hours if you take both. It is an unglamorous detail, but it can be the difference between stable thyroid levels and months of unnecessary dose changes.
Frequently Asked Questions
Can hair really look thinner when you’re hungry?
Yes, it can, even if you are not shedding more in that moment. When you are dehydrated or your hair is drier and flatter, your scalp shows through more, especially along the part line. Hunger can also come with stress-hormone symptoms that make you scrutinize changes more closely. Try a same-lighting photo before eating and again after food plus water to see how much is “appearance” versus true shedding.
What ferritin level is too low for hair growth?
Many people with shedding feel better when ferritin is well above the bare minimum on the lab report. A common practical target used in hair clinics is roughly 50–100 ng/mL, depending on your history and iron overload risk. If your ferritin is below about 30 ng/mL, it is a strong clue that low iron stores could be contributing. Ask for ferritin specifically, not just hemoglobin, because you can have normal hemoglobin and still have low ferritin.
How long after fixing iron or thyroid will hair improve?
Hair follicles work on a delay, so you usually do not see immediate density changes. Shedding often starts to calm down within about 6–12 weeks after the trigger is corrected, while visible thickening commonly takes 3–6 months and can take up to a year. That timeline is frustrating, but it is also reassuring because slow improvement is still real improvement. Take monthly photos in the same lighting so you can see progress you might miss day to day.
Is intermittent fasting causing my hair loss?
Fasting does not automatically cause hair loss, but it can contribute if it leads to low overall calories, low protein, low iron intake, or frequent stress-hormone spikes from blood-sugar dips. If your shedding started after you changed your eating window, or you feel shaky and irritable before meals, it is worth loosening the fasting schedule for 6–8 weeks as a test. You can still pursue metabolic goals, but your body needs enough building blocks to keep hair in the growth phase. If you want a clearer answer, ferritin, TSH, and fasting insulin can help you see what your body is signaling.
When should I worry that hair thinning is something serious?
You should get checked sooner if hair loss is patchy, scarring, painful, or associated with a new rash, because those patterns can signal inflammatory scalp conditions that need treatment. It is also worth prompt evaluation if you have symptoms of thyroid disease such as a racing heart, fainting, or severe heat intolerance, or if you have heavy bleeding that could be driving iron depletion. Most diffuse shedding is not dangerous, but it is a meaningful clue about nutrition, hormones, or stress load. If you are unsure, start with ferritin and TSH and bring the results to a clinician or PocketMD to plan next steps.
What the research says about shedding
Serum ferritin levels and hair loss in women: low ferritin is commonly associated with diffuse shedding
American Thyroid Association guidelines for hypothyroidism: thyroid dysfunction is a recognized cause of diffuse hair loss
Telogen effluvium review: shedding often follows physiologic stress and typically resolves with time once triggers are corrected