Dry Skin in Your 20s: What It Means and What Helps
Dry skin in your 20s often comes from barrier damage, eczema, or low thyroid/iron. Get targeted labs at Quest—no referral needed.
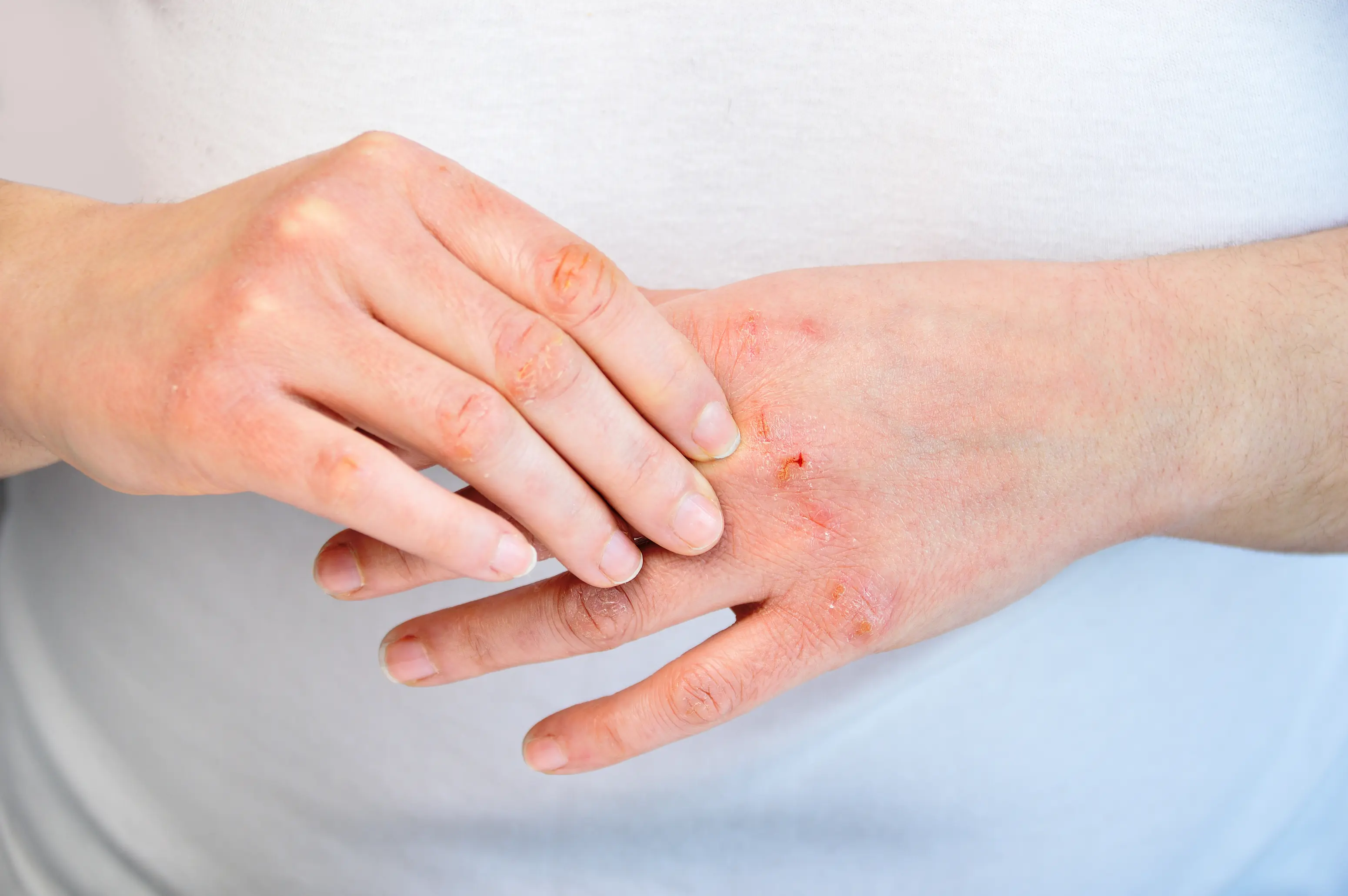
Dry skin in your 20s is usually a skin-barrier problem, not “just dehydration.” Over-washing, strong acne products, and dry air can strip the oils and fats that keep water in, and eczema can quietly drive itching and flaking even when you moisturize. Sometimes the clue is internal, like low thyroid function or low iron, and basic labs can help you figure out which bucket you’re in. It’s frustrating because you can do “all the right things” and still feel tight, itchy, or like your face is aging overnight. In your 20s, the most common pattern is that your routine is accidentally too harsh for your barrier, especially if you’re treating acne or living in a dry climate. This guide walks you through the most likely causes, what actually helps (in a practical order), and which blood tests are worth considering. If you want help matching your exact pattern to a plan, PocketMD can talk it through with you, and Vitals Vault labs can help check for common internal contributors.
Why your skin is dry in your 20s
Your skin barrier is stripped
Your outer skin layer is supposed to act like a brick wall, with skin cells as bricks and oils as mortar. Hot showers, frequent cleansing, and foaming or “deep clean” products dissolve that mortar, so water escapes and your skin feels tight within minutes of washing. The quickest clue is timing: if you feel dry right after cleansing, your routine is likely the main trigger, so start by making it gentler before you buy a new “stronger” moisturizer.
Eczema flare, even if mild
Eczema (atopic dermatitis) is a tendency toward an overreactive immune response in the skin, which weakens the barrier and drives itch. In your 20s it can look subtle, like rough patches on your hands, eyelids, or around your mouth, and you may notice stinging when you apply products that never used to bother you. If itching is a big part of your dryness, treating inflammation (not just adding moisture) is often the missing piece.
Acne treatments causing dryness
Retinoids, benzoyl peroxide, and salicylic acid are effective, but they speed up skin turnover or dissolve oil, which can outpace your barrier’s ability to rebuild. That’s why you can have acne and dry, peeling skin at the same time, especially around the nose and mouth. You don’t have to quit acne care, but you may need to reduce frequency, buffer with moisturizer, or switch formulations so your skin can tolerate it.
Dry air and indoor heating
When the air is dry, water evaporates from your skin faster, even if you’re drinking plenty of fluids. You’ll often notice it’s worse in winter, on airplanes, or in heavily air-conditioned spaces, and your lips and hands are usually the first to complain. If your dryness tracks your environment, a humidifier and “seal it in” moisturizing right after showering can make a bigger difference than changing your diet.
Internal causes like low thyroid
Low thyroid function (hypothyroidism) slows down oil production and skin cell turnover, so your skin can feel rough, cool, and persistently dry no matter what you put on it. Low iron stores can also show up as dryness alongside hair shedding or brittle nails, because your body prioritizes oxygen delivery over “nice-to-have” tissues like skin and hair. If your dryness is new, widespread, and paired with fatigue, constipation, heavier periods, or hair changes, it’s reasonable to check a few targeted labs rather than guessing.
What actually helps dry skin (without giving up your whole routine)
Switch to a gentle cleanse
Use a non-foaming, fragrance-free cleanser, and keep showers lukewarm rather than hot, because heat dissolves barrier oils faster. If your face isn’t truly dirty in the morning, rinsing with water or using cleanser only at night can be enough. Give this change a full 10–14 days, because your barrier needs time to rebuild.
Moisturize like you mean it
Apply moisturizer within two minutes of washing, while your skin is still slightly damp, because you’re trapping water before it evaporates. For stubborn dryness, choose a cream with ceramides (barrier fats) and glycerin or hyaluronic acid (water binders), and then add a thin layer of petrolatum on the driest spots at night. If a product burns on contact, that’s often a sign your barrier is irritated, so go simpler rather than “more active.”
Use actives on a schedule
If you’re using a retinoid or acne acids, start with two nights per week and increase only when your skin feels calm for a full week. On active nights, apply moisturizer first (“sandwiching”) to reduce irritation without losing all benefit. This is especially helpful around the mouth and nose, where peeling tends to concentrate.
Treat itch and inflammation early
When itching is driving scratching, your skin can’t heal, and dryness becomes a loop. Short courses of over-the-counter 1% hydrocortisone can help small flares on the body, but avoid using it on your face long-term unless a clinician guides you. If you’re getting recurrent eyelid, hand, or lip-area flares, ask about eczema care and contact allergy testing, because removing the trigger can be more effective than rotating products forever.
Fix the air, not just the cream
Aim for indoor humidity around 40–50%, because very dry air pulls moisture from your skin all day. A bedroom humidifier plus a heavier night moisturizer often improves morning tightness within a week. If you travel a lot, a small tube of petrolatum for lips and knuckles can prevent the “airplane skin” crash before it starts.
Useful biomarkers to discuss with your clinician
TSH
TSH is the master regulator of thyroid function, controlling the production of thyroid hormones T4 and T3. In functional medicine, we use narrower TSH ranges than conventional medicine to identify subclinical thyroid dysfunction early. Even mildly elevated TSH can indicate thyroid insufficiency, leading to fatigue, weight gain, depression, and metabolic dysfunction. TSH levels are influenced by stress, nutrient deficiencies, autoimmune conditions, and environmental toxins. Optimal TSH supports energy, metabolism…
Learn moreFerritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreVitamin D, 25-Oh, Total
Total 25-hydroxyvitamin D represents the best measure of vitamin D status, combining both D2 and D3 forms. This is the storage form of vitamin D and reflects recent intake and synthesis. In functional medicine, total 25(OH)D is used to assess vitamin D sufficiency and guide supplementation. Optimal levels (40-80 ng/mL) are associated with reduced risk of cancer, cardiovascular disease, autoimmune conditions, and all-cause mortality. Vitamin D acts as a hormone affecting immune function, bone health, mood, and ce…
Learn moreLab testing
Check TSH, ferritin, and vitamin D at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a two-week “barrier reset” where you stop exfoliating acids and scrubs, use a gentle cleanser only once daily, and moisturize twice daily. If your skin improves, you’ve learned your main problem is irritation, not a lack of products.
If your moisturizer pills or feels like it sits on top, try applying it to damp skin and using less than you think you need. Too much product can roll up, which makes you reapply and irritate your skin more.
Patch-test new products on the side of your neck or behind your ear for three nights in a row. If you get burning, redness, or itching there, it will almost certainly be worse on your face.
For hands that crack, keep a thick cream by every sink and apply it after every wash, then use petrolatum and cotton gloves for 30 minutes before bed. That short “occlusion window” often heals fissures faster than daytime lotions.
If your lips are constantly dry, switch to a plain petrolatum-based balm for two weeks and avoid flavored or “plumping” products. Chronic lip dryness is often irritation or contact allergy, not a hydration problem.
Frequently Asked Questions
Why is my skin so dry even when I moisturize?
If you moisturize but still feel tight or flaky, your barrier is probably being stripped faster than it can rebuild, often from hot showers, foaming cleansers, or acne actives. Moisturizer works best when you apply it to damp skin and use a barrier-repair formula with ceramides. Try a 10–14 day gentle routine reset and see if the baseline dryness improves.
Can dehydration cause dry skin in your 20s?
Mild dehydration can make skin look a little dull, but most “dry skin” is about the outer barrier leaking water, not about how much water you drank. That’s why people can drink plenty and still feel tight after washing. Focus first on gentler cleansing and sealing in moisture right after bathing.
Is dry skin a sign of hypothyroidism?
It can be, especially if the dryness is new, widespread, and comes with fatigue, constipation, feeling cold, or heavier periods. A TSH test is the usual starting point, and many clinicians interpret symptoms more carefully when TSH is above about 2.5–4.0 mIU/L depending on context. If you suspect thyroid issues, get TSH checked and bring your symptom timeline to your appointment.
What vitamin deficiency causes dry skin?
Low vitamin D can be linked to more reactive, eczema-prone skin, and low iron stores (low ferritin) can show up with dryness plus hair shedding or brittle nails. The most useful tests are 25-hydroxy vitamin D and ferritin, because they reflect body stores. If either is low, repleting and rechecking in 8–12 weeks is a practical next step.
How do I know if it’s eczema or just dry skin?
Eczema usually includes itch, recurring patches in the same areas (hands, eyelids, inner elbows, behind knees), and stinging with products that used to feel fine. Plain dry skin tends to improve steadily with gentler cleansing and consistent moisturizing, without much itch. If itch is a major feature or you’re waking up scratching, treat it like eczema and consider seeing a clinician for a targeted plan.