Why Is Your Skin So Dry at Night?
Dry skin at night often comes from low humidity, a weakened skin barrier, or eczema flares. Targeted labs are available—no referral needed.
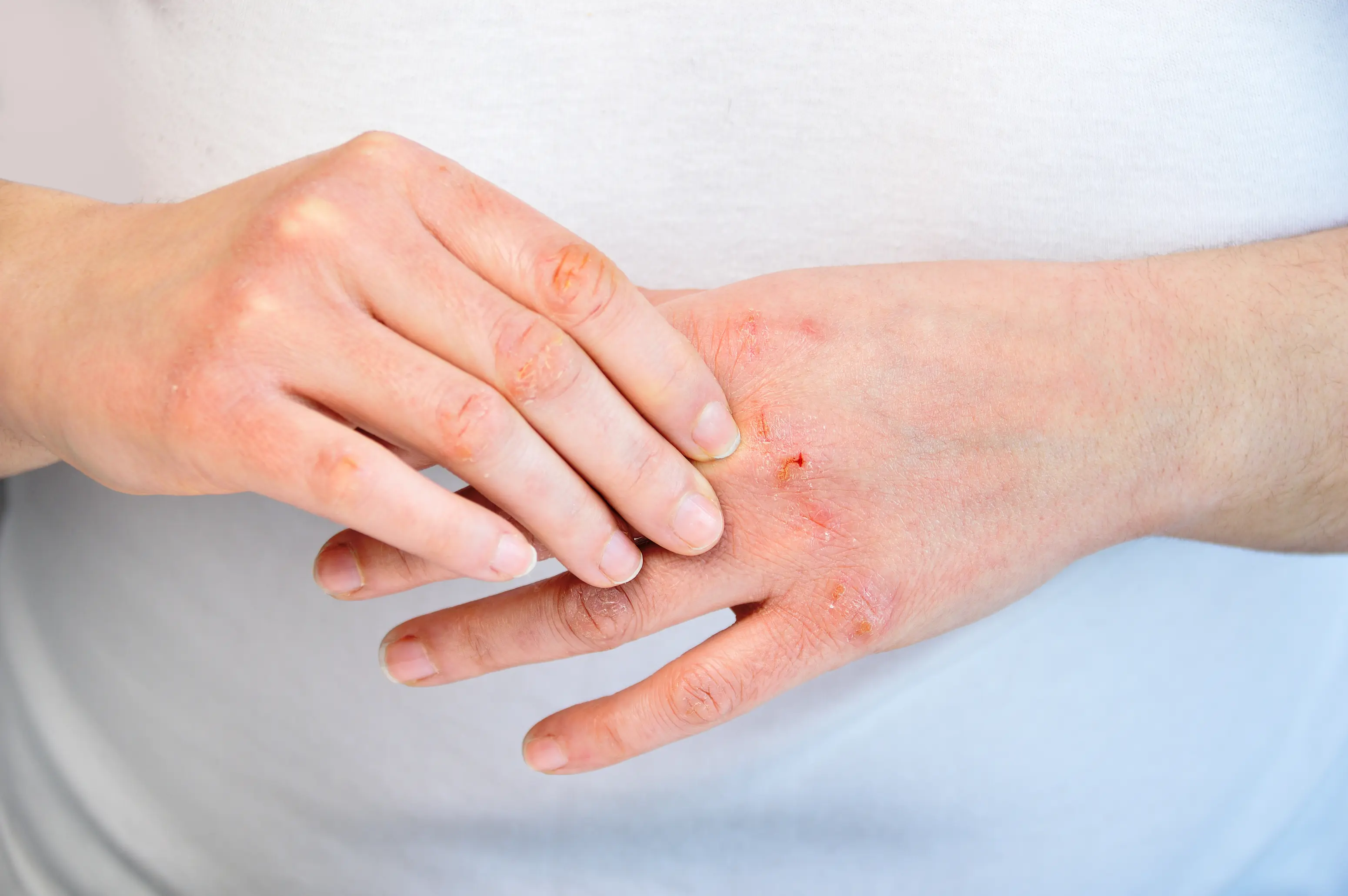
Dry skin at night usually happens because your skin loses more water in the evening, your bedroom air is dry, or your skin barrier is irritated by eczema or harsh cleansing. It can also show up when your thyroid is underactive or when iron stores are low, which can make skin feel rough and itchy. A few targeted labs can help you tell the difference between “this is my environment and routine” and “this is something internal I should treat.” Nighttime dryness is extra frustrating because it steals your sleep and turns “a little tightness” into itching that feels impossible to ignore. Your skin’s barrier is supposed to act like a brick wall, holding water in and keeping irritants out, but at night that wall can leak more easily — especially if you shower late, use strong soaps, or sleep in heated or air-conditioned air. Below, you’ll see the most common causes, what tends to help fastest, and which tests are worth considering. If you want help matching your pattern to a likely cause, PocketMD can talk it through with you, and Vitals Vault labs can help confirm what’s going on.
Why your skin gets drier at night
Dry bedroom air pulls moisture out
When the air in your room is dry, water evaporates from your skin faster, which is why you can feel fine during the day and suddenly tight and itchy after you get into bed. Heating in winter and air conditioning in summer both lower indoor humidity, and your skin notices. A simple clue is waking up with a dry nose or throat along with dry skin, which often points to the room, not your bloodstream.
Hot showers strip your skin oils
A hot shower right before bed feels relaxing, but it dissolves and rinses away the oils that help seal water into your outer skin layer. After you towel off, your skin can keep losing water for hours, so the itch ramps up as you’re trying to fall asleep. If you love nighttime showers, keep them lukewarm and short, and put moisturizer on within three minutes while your skin is still slightly damp.
Eczema flares more at night
Eczema (atopic dermatitis) is a barrier problem plus an overactive itch response, and both can feel louder at night when you’re warm under blankets and you’re not distracted. Many people also scratch in their sleep, which creates tiny breaks in the skin that burn and itch the next night. If you see red patches in the creases of your elbows or behind your knees, or if your skin feels “itchy first, rash second,” eczema becomes more likely.
Irritants on sheets and pajamas
Your skin can react to what touches it for eight straight hours, especially if your barrier is already dry. Fragranced detergents, dryer sheets, and scratchy fabrics can trigger itching that feels like “dryness,” even when you used a good lotion. A useful experiment is switching to fragrance-free laundry products and wearing soft cotton for two weeks, because contact irritation usually improves faster than true eczema.
Internal causes like thyroid or iron
An underactive thyroid (hypothyroidism) slows skin turnover and reduces oil and sweat production, so your skin can feel rough, cool, and stubbornly dry no matter how much you moisturize. Low iron stores can also show up as dry, itchy skin along with hair shedding or brittle nails, because your body prioritizes oxygen delivery over “extras” like skin and hair. If dryness is new, widespread, and paired with fatigue, constipation, heavy periods, or hair changes, it’s worth checking labs instead of only changing products.
What actually helps at night
Aim for 40–50% bedroom humidity
If your room is running at 20–30% humidity, your skin is basically being gently dehydrated all night. A cool-mist humidifier can make a noticeable difference within a few nights, especially for hands, shins, and the face. Use a cheap hygrometer to confirm you’re in the 40–50% range, and clean the humidifier regularly so you’re not breathing in mold.
Use the “soak and seal” method
The goal is to trap water in your skin, not just grease the surface. After a lukewarm shower or a 5–10 minute bath, pat dry and apply a thick moisturizer or ointment while your skin is still damp, because that’s when it can lock in the most water. If your legs are the worst, try an ointment on shins and calves at night and a lighter cream elsewhere so you don’t feel sticky.
Choose barrier-repair ingredients
Look for moisturizers with ceramides, glycerin, or urea, because they help rebuild the “mortar” between skin cells and pull water into the outer layer. If you sting when you apply products, skip acids and strong retinoids for a week and focus on bland barrier repair until the burning stops. For very itchy patches, a short course of over-the-counter 1% hydrocortisone can calm inflammation, but if you need it most nights, you should get a clinician’s plan.
Stop the itch-scratch cycle
Scratching feels like relief, but it creates micro-injuries that keep your nerves irritated and your barrier leaky, which means tomorrow night is worse. Keep nails short, consider thin cotton gloves for sleep, and use a cold pack for 5 minutes when an area is screaming, because cooling quiets itch signals fast. If itching is intense enough to keep you awake for multiple nights, that’s a good reason to ask about prescription eczema treatments.
Adjust your evening cleansing routine
If you wash your face or body at night, use a gentle, fragrance-free cleanser and avoid “squeaky clean” foaming formulas, because that squeak is often your oils being stripped. You can also try cleansing only the areas that truly need it, like armpits and groin, and rinsing the rest with water. This one change often helps people who moisturize faithfully but still wake up feeling tight.
Useful biomarkers to discuss with your clinician
Vitamin D, 25-Oh, Total
Total 25-hydroxyvitamin D represents the best measure of vitamin D status, combining both D2 and D3 forms. This is the storage form of vitamin D and reflects recent intake and synthesis. In functional medicine, total 25(OH)D is used to assess vitamin D sufficiency and guide supplementation. Optimal levels (40-80 ng/mL) are associated with reduced risk of cancer, cardiovascular disease, autoimmune conditions, and all-cause mortality. Vitamin D acts as a hormone affecting immune function, bone health, mood, and ce…
Learn moreFerritin
Ferritin is your body's iron storage protein, reflecting total iron stores in the body. In functional medicine, ferritin assessment is crucial for identifying both iron deficiency and iron overload, conditions that can significantly impact energy levels and overall health. Low ferritin is the earliest sign of iron deficiency, often occurring before anemia develops. This can cause fatigue, weakness, restless leg syndrome, and cognitive impairment. Conversely, elevated ferritin may indicate iron overload, inflamma…
Learn moreZinc
Zinc status affects immune function, growth and development, reproductive health, and cognitive function. Deficiency is common worldwide and can impair wound healing, taste perception, and immunity. Adequate zinc is essential for thyroid function, testosterone production, and skin health. Zinc is an essential trace mineral involved in over 300 enzymatic reactions in the body. It plays crucial roles in immune function, wound healing, protein synthesis, DNA synthesis, and cell division.
Learn moreLab testing
Check TSH, ferritin, and A1c at Quest — starting from $99 panel with 100+ tests, one visit. No referral needed.
Schedule online, results in a week
Clear guidance, follow-up care available
HSA/FSA Eligible
Pro Tips
Do a one-week “product fast” on the itchy areas: use only a gentle cleanser and one fragrance-free moisturizer, because too many actives at night can keep your barrier inflamed.
If your shins crack or look ashy, try an ointment (like petrolatum) just on that zone and put on loose cotton pants, because fabric friction can undo your moisturizer in minutes.
Keep a bedside “rescue kit” with moisturizer and a cold pack, so you can calm itch quickly without getting up and fully waking your brain.
If you suspect laundry irritation, rewash your sheets once with fragrance-free detergent and skip fabric softener, because residue can keep triggering itch even after you switch brands.
Take a photo of the worst spots under the same lighting for 7 nights, because patterns like redness, scaling, or small bumps help you tell dryness from eczema or contact irritation.
Frequently Asked Questions
Why is my skin only dry at night but fine during the day?
At night, your skin tends to lose more water, and your bedroom air is often drier than the daytime environment, especially with heat or AC running. You also notice itch more when you’re still and warm under blankets. Try getting bedroom humidity to about 40–50% and applying moisturizer within three minutes of washing to see if the pattern changes.
Can dehydration cause dry skin at night?
Being dehydrated can make dryness feel worse, but most nighttime dry skin is driven by a leaky skin barrier and dry air rather than “not drinking enough.” If your lips and mouth are dry too, hydration matters more, but you still usually need a barrier-focused moisturizer. If you’re urinating a lot at night or feeling unusually thirsty, consider checking a hemoglobin A1c.
Is itchy dry skin at night a sign of eczema?
It can be, especially if you have red, scaly patches, a history of allergies or asthma, or itching that comes before you can even see a rash. Eczema (atopic dermatitis) often flares at night because warmth and scratching keep the inflammation going. If you’re using moisturizer daily and still waking up itchy several nights a week, it’s reasonable to ask for an eczema treatment plan.
What moisturizer is best for dry skin at night?
For nighttime, thicker is usually better because it reduces water loss while you sleep. Look for a fragrance-free cream with ceramides and glycerin, or use an ointment on the driest areas like shins and hands. If products sting, avoid acids and retinoids for a week and focus on bland barrier repair until your skin calms down.
What labs should I check for dry skin and itching?
If dryness is new, widespread, or paired with fatigue or hair changes, checking TSH, ferritin, and hemoglobin A1c can be a practical starting point. High TSH can point to an underactive thyroid, low ferritin can suggest low iron stores, and a higher A1c can signal blood sugar issues that impair skin repair. Bring your results and your symptom timeline to a clinician, or use PocketMD to help you decide what to do next.
