
Back to Articles
Blood Work Results: When to Retest vs Follow Up
Confused by blood work results? Learn when to retest vs follow up, ideal timing by biomarker (apoB, hs-CRP, insulin), and next steps.
April 28, 2026
1 min read
Vitals Vault Team
Core Essential Wellness Panel
120+ Biomarkers & a thumbprint of your biological age
Includes the depth of physician-backed labs plus AI-reviewed storytelling so you can act on your physiology with confidence.
- 120+ doctor-curated functional medicine tests
- Personalised Action Plan + AI-reviewed clinical summary
- Upload, track, and securely share past reports
- PhenoAge score to measure your biological age
Understanding your blood work results can be daunting, especially when faced with abnormal flags. This guide provides clear, clinician-style advice on when to retest versus when to follow up, helping you interpret common biomarkers like apoB, hs-CRP, fasting insulin, and more. Whether you're managing your health proactively or navigating specific concerns, this post offers practical timelines and decision-making strategies tailored to your blood work results.
Most people don’t get stuck on getting labs, they get stuck on what to do after the portal lights up with flags.
Some abnormal blood work results are real signals that deserve timely follow-up. Others are noise caused by timing, hydration, recent exercise, a brewing virus, or even how long the tube sat before processing.
This guide gives you a practical, clinician-style way to decide when to retest vs when to follow up, plus realistic retest windows for high-impact longevity markers like apoB, Lp(a), hs-CRP, fasting insulin, HOMA-IR, HbA1c, testosterone, cortisol, ferritin, eGFR, ALT/AST, and GGT.
If you want to skip the referral loop, Vitals Vault lets you order comprehensive labs with no doctor referral needed, draw at 2,000+ Quest/Labcorp locations, and get clinician-reviewed insights with results often in 24-48 hours. You can start with a full panel at checkout or explore markers in the biomarker library.
Retest vs follow up: what’s the difference (and why it matters)?
Retesting is about confirmation. You repeat the same test (often with better prep or timing) to answer: Was that value reproducible?
Following up is about escalation. You involve a clinician and/or add tests to answer: What’s causing this and does it need treatment or further evaluation?
A useful mental model:
- Retest when you suspect a one-off influence (sleep debt, dehydration, recent hard training, acute illness, supplement timing, non-fasting draw, lab variability).
- Follow up when results show severity, symptoms, a pattern across multiple markers, or persistence over time.
Could these blood work results be urgent right now?
Educational note: labs are not a substitute for urgent evaluation.
Follow urgent instructions from the lab or your clinician if you see “critical” flags or if you have concerning symptoms (chest pain, shortness of breath, fainting, severe weakness, confusion, uncontrolled bleeding, severe abdominal pain). If you are worried, seek urgent care.
For non-critical abnormalities, the rest of this article helps you choose the next best step.
Should I retest my blood work results first? Ask these 5 questions
1) Was the draw standardized?
Many “abnormal” results are explainable by pre-analytic variables.
Common examples:
- Non-fasting can raise triglycerides, glucose, insulin, and sometimes liver enzymes.
- Dehydration can concentrate markers like albumin and BUN, and can affect creatinine.
- Hard training 24-48 hours prior can shift CK, AST/ALT, creatinine, and inflammatory signals.
- Alcohol (especially within 24-72 hours) can worsen triglycerides and liver enzymes.
- Acute illness can elevate hs-CRP, WBC, ferritin (as an acute-phase reactant), and lower performance hormones.
If the draw was “messy,” retesting is often the fastest way to de-noise.
2) Is it a single outlier or a multi-marker pattern?
A single mildly abnormal value is more likely to be variability. A cluster of related markers moving together is more likely to be physiology.
Example patterns that usually deserve follow-up, not just a casual retest:
- Insulin resistance pattern: fasting insulin high, HOMA-IR high, triglycerides high, HDL low, ALT trending up.
- Atherogenic risk pattern: apoB high (with or without LDL-C), hs-CRP elevated, Lp(a) elevated.
- Kidney filtration concern pattern: creatinine up, eGFR down, urine albumin (ACR) up, urine RBC/WBC abnormalities.
3) How far outside the reference range is it?
Borderline deviations often merit retesting. Larger deviations generally merit follow-up.
Reference ranges are population-based, not personalized. Your decision should reflect:
- Degree of abnormality
- Symptoms
- Trend history
- Companion markers
4) Do you have symptoms that match the finding?
Symptoms raise the urgency. For example:
- Fatigue plus abnormal TSH/free T4, ferritin, B12, fasting insulin, or testosterone.
- New headaches or blood pressure changes plus kidney markers.
- Frequent infections plus unusual CBC patterns.
5) Did you recently change meds, supplements, or habits?
If you started or stopped something meaningful, retesting too soon can be misleading.
Examples:
- Lipid changes after diet shifts often stabilize over 6-12 weeks.
- HbA1c reflects roughly 8-12 weeks of glycemic exposure.
- Thyroid dose changes are typically reassessed after several weeks.
A simple timeline: when to retest common biomarkers (and when to follow up instead)
The table below is a practical starting point for proactive adults. It is educational and not medical advice.
Swipe
If you want your retest to actually answer the question, standardization is everything (more on that below).
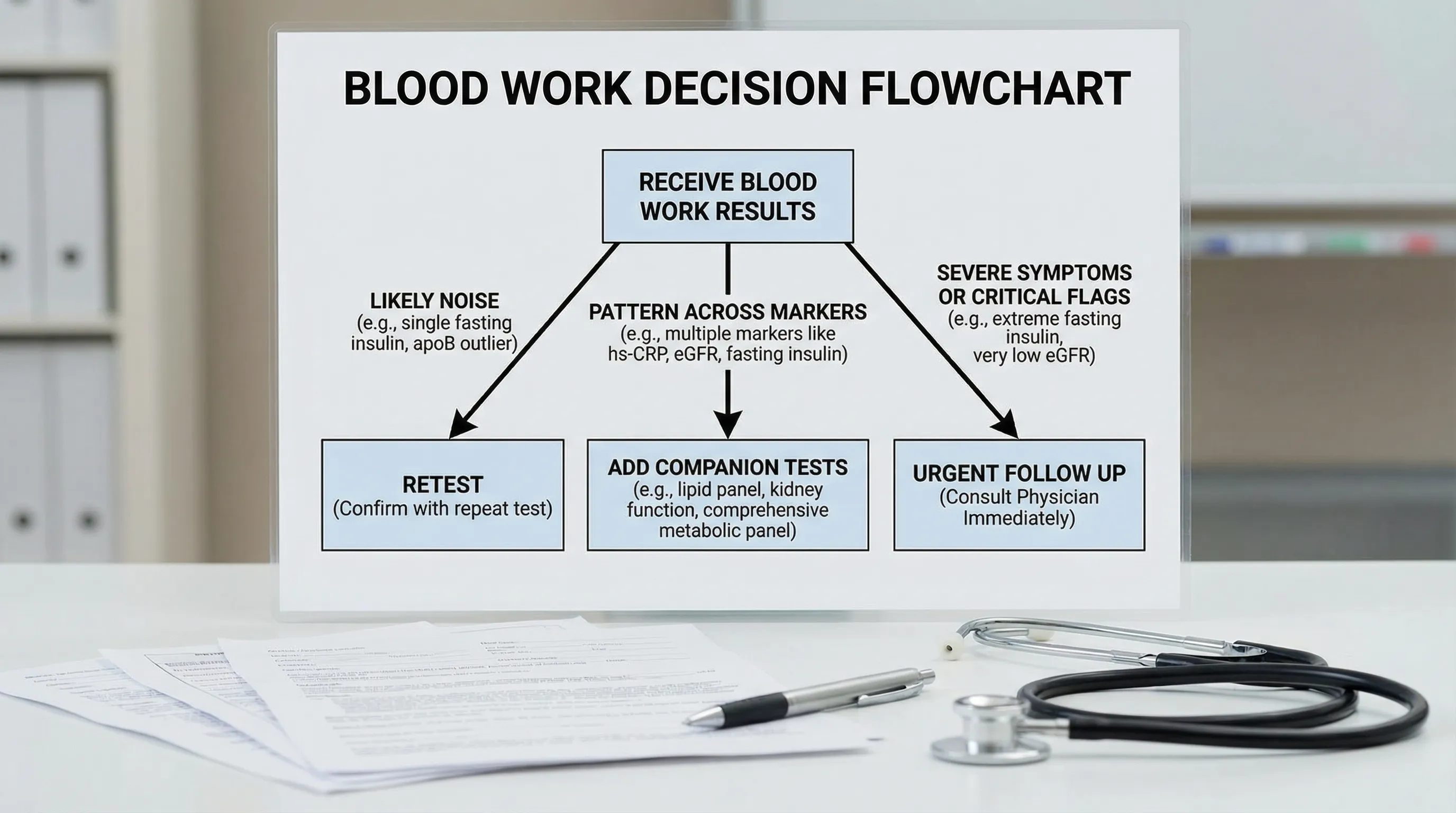
Which blood work results should I retest quickly (within 1-2 weeks)?
Retesting sooner makes sense when you suspect a reversible confounder and the goal is confirmation.
Typical examples:
- Creatinine/eGFR after dehydration, sauna use, or heavy lifting. Retest with normal hydration and no intense training for 48 hours.
- AST/ALT after hard workouts (especially eccentric lifting) or alcohol. Consider adding GGT to clarify liver-specific stress.
- hs-CRP during or right after a cold, flu, dental work, or injury. Retest after you are back to baseline.
- Mild CBC shifts (WBC, neutrophils, lymphocytes) after a recent infection. Retesting after recovery can prevent overreaction.
Which blood work results should I retest after 8-12 weeks (because biology needs time)?
Some markers change slowly or reflect longer-term exposure.
Common examples:
- HbA1c: often best reassessed around 12 weeks after consistent changes (diet, sleep, training).
- Fasting insulin and HOMA-IR: can improve sooner than A1c for some people, but 8-12 weeks is a realistic window for a clean “before vs after.”
- ApoB and triglycerides: many people see meaningful shifts after 6-12 weeks of consistent nutrition, weight change, or medication adjustments.
- Vitamin D and ferritin after supplementation changes: 8-12 weeks is a common reassessment interval.
For diabetes screening and monitoring cadence, see the American Diabetes Association Standards of Care.
When is it smarter to follow up than to retest?
Retesting can become a stall tactic when the situation calls for interpretation and next-step diagnostics.
Follow up is usually the better move when:
- You have multiple abnormal markers in the same system.
- The result is significantly abnormal, not borderline.
- You have symptoms that match the abnormality.
- The abnormality persists on a repeat test.
- You need a decision about medication, imaging, or a targeted workup.
Concrete examples:
- ApoB is elevated: rather than repeating immediately, follow up to interpret it in context (LDL-C, triglycerides, non-HDL-C, hs-CRP, blood pressure, family history), and consider adding Lp(a) if not already tested.
- Fasting glucose is normal but fasting insulin is high: that is often an early insulin resistance signal. Follow up with a structured plan and retest after 8-12 weeks, not 8-12 days.
- eGFR is down and urine protein is positive: follow up promptly, a single retest without urine context can miss risk.
What companion tests should I add instead of repeating the same panel?
One of the highest leverage moves in interpreting blood work results is adding the “missing context” marker.
Swipe
This “add context first” approach is one reason comprehensive testing beats piecemeal labs.
How do I retest blood work results correctly (so it’s not garbage-in, garbage-out)?
If you are going to retest, make the second data point comparable.
Standardize these variables as much as possible:
- Time of day: morning draws are often best for hormones like testosterone and cortisol.
- Fasting: if fasting insulin, triglycerides, or glucose are involved, keep fasting consistent (often 10-12 hours, water allowed).
- Exercise: avoid intense training 24-48 hours before testing (especially if liver enzymes, creatinine, CK, or inflammation markers are in play).
- Alcohol: avoid for 48-72 hours if triglycerides or liver markers were abnormal.
- Hydration and sodium: keep routine normal, do not “overcorrect” with extreme water loading.
- Supplements and biotin: disclose everything you take. Some supplements can interfere with certain immunoassays.
- Illness and sleep: postpone optimization-focused retests if you are acutely sick or severely sleep-deprived.
If you are tracking trends, consistency is more valuable than perfection.
Can I order follow-up labs without my doctor?
Yes, in many cases you can access repeat and add-on testing directly.
The bigger issue is not access, it is getting the right set of biomarkers with interpretation that helps you decide what to do next.
Vitals Vault is built for that exact gap:
- No doctor referral needed
- Results often in 24-48 hours
- 100-160+ biomarkers in comprehensive panels (so you are not stuck repeating partial panels)
- Clinician-reviewed insights included
- Draw options at 2,000+ Quest/Labcorp locations nationwide
If you already have results and want a clearer next step, start with a comprehensive panel at Vitals Vault checkout or find the exact markers you want to add at /biomarkers.
How does Vitals Vault compare for retesting and follow-up vs Function Health, InsideTracker, Superpower, and Mito Health?
If your goal is better decisions from your blood work results, the differences that matter are biomarker depth, turnaround, and whether follow-up is built in.
Swipe
Bottom line: if you are retesting because you want clarity (not just another PDF), you generally want the platform that combines depth + clinician review + easy repeat testing, without a waitlist.
What’s the fastest way to get “unstuck” after confusing blood work results?
If you are staring at flags and unsure whether to retest or follow up, do this:
- Identify whether the result could be explained by conditions (fasting, illness, dehydration, heavy training).
- Check whether it forms a pattern with companion markers (apoB with triglycerides and hs-CRP, fasting insulin with glucose and ALT, creatinine with urine markers).
- Decide your next step: retest to confirm (when likely noise) or follow up and expand context (when likely real).
Vitals Vault is designed for exactly that moment, comprehensive panels, rapid turnaround, and clinician-reviewed next steps.
Explore the markers you care about at Vitals Vault Biomarkers, or order a comprehensive panel now at Vitals Vault Checkout.
Educational content only. Not medical advice. If you have severe symptoms or critical lab values, seek urgent care.
Conclusion
Navigating blood work results effectively requires distinguishing between test variability and genuine health concerns. By using the outlined retest windows and follow-up criteria, you can make informed decisions that prioritize accuracy and timely care. Consider applying these guidelines to approach your next blood test results with confidence and clarity.